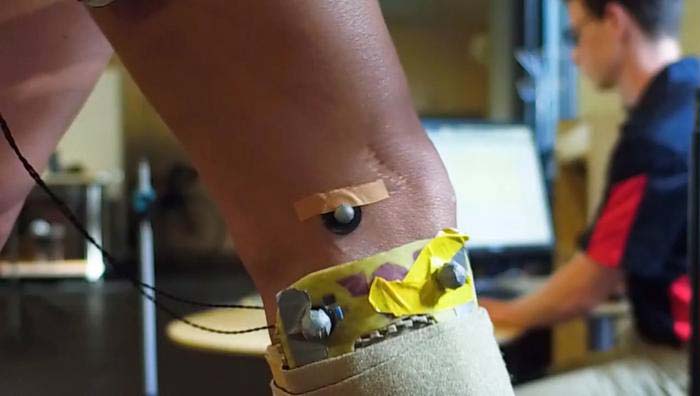
At the beginning of the study, participants received a baseline MRI and walked on a force-sensitive treadmill while motion-capture cameras recorded their walking mechanics. Image courtesy of the Utah Movement Bioengineering Lab.
Researchers from the University of Utah (U of U), Salt Lake City; New York University; and Stanford University, California, have demonstrated the potential of gait retraining to relieve arthritic knee pain without drugs or surgery. The researchers were specifically looking at patients with mild-to-moderate osteoarthritis (OA) in the medial compartment of the knee, which tends to bear more weight than the lateral compartment. This form of OA is the most common, but the ideal foot angle for reducing load in the medial side of the knee differs from person to person depending on their natural gait and how it changes when they adopt the new walking pattern.
In their first 2 visits, participants received a baseline MRI and practiced walking on a pressure-sensitive treadmill while motion-capture cameras recorded their gait mechanics. This allowed the researchers to determine whether turning the patient’s toe inward or outward would reduce load more, and whether a 5-degree or 10-degree adjustment would be ideal. This personalized analysis also screened out potential participants who could not benefit from the intervention, as none of the foot angle changes could decrease loading in their knees. Moreover, after their initial intake sessions, half of the 68 participants were assigned to a sham treatment group to control for the placebo effect. These participants were prescribed foot angles that were actually identical to their natural gait. Conversely, participants in the intervention group were prescribed the change in foot angle that maximally reduced their knee loading.
Participants from both groups returned to the lab for 6 weekly training sessions, where they received biofeedback that helped them maintain the prescribed foot angle while walking on the treadmill. After the training period, participants were encouraged to practice their new gait for at least 20 minutes a day, to the point where it became natural. Periodic check-in visits showed that participants were adhering to their prescribed foot angle within a degree on average.
After a year, all participants self-reported their experience of knee pain and had a second MRI to quantitatively assess the damage to their knee cartilage.
“The reported decrease in pain over the placebo group was somewhere between what you’d expect from an over-the-counter medication…,” Uhlrich said. “With the MRIs, we also saw slower degradation of a marker of cartilage health in the intervention group, which was quite exciting.”






