Effective early interventions can delay or even eliminate the need for surgery in patients with medial compartment knee osteoarthritis. From weight loss to exercise to lever arms, evidence suggests that offloading the joint is key.

istock 6364123
By Monica R. Maly, PT, PhD
Knee osteoarthritis (OA) is the leading cause of chronic disability among older adults.1 Though knee OA does not manifest with overt neurological or systemic signs, knee OA limits participation in physical activity by challenging a person’s ability to complete occupational and social responsibilities, even during the earliest disease stages.2
The gold standard treatment, surgery, addresses only late stage knee OA. Prior to that stage, intervention has focused on symptomatic relief with pharmaceuticals.3 However, many older patients prefer to avoid adding to the number of pharmaceuticals they have already been prescribed,4 and many of these drugs have serious side effects such as gastrointestinal bleeding.5
From a biomechanical perspective, pharmaceuticals actually accentuate the mechanical pathology that promotes OA,6,7 raising questions about the long-term impact of these drugs. During the years prior to surgery, we are missing opportunities to conservatively manage both the pain and mechanical pathology of knee OA.
Mechanical pathology
Knee OA is characterized by progressive degradation of articular cartilage and the surrounding joint tissues, including muscle, bone and ligament. Edema and degradation of the molecular structure of articular cartilage reduces the capacity for this tissue to dissipate loading or provide frictionless movement. These changes are accompanied by subchondral bone sclerosis, ligamentous laxity and poor muscle function, which perpetuate the disease. Risk factors include older age, female sex, obesity, muscle weakness and past injury.8 The trigger for these pathological changes is thought to be mechanical loading, which damages tissues at a rate faster than the body can repair.
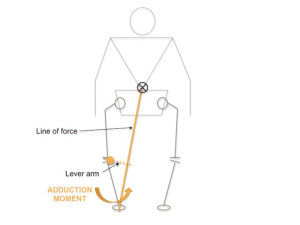
Osteoarthritic changes can occur in any of the medial, lateral or patellofemoral compartments of the knee. The focus of this article will be medial compartment knee OA, which results from abnormal loading patterns that are biased toward excessive medial loading. The knee adduction moment (or torque) represents this distribution of loading across the medial and lateral compartments of the knee surfaces. This measurement is highly reliable9 and valid.10-12 An excessive adduction moment reflects a large torque tending to rotate the tibia into a varus or bowlegged position on the femur (Figure 1). Tracking the adduction moment throughout one stride (from heel strike on one foot to the subsequent heel strike on the same foot) results in a graph denoting the magnitude of this moment at different times during gait (Figure 2).
Four elements determine the magnitude of the adduction moment during stride:
The overall mass (body “weight”) loads the knee during activity. As the foot contacts the ground during stride, laboratory measurement of the equal and opposite reaction force from the ground allows us to evaluate the impact of mass on knee loading.
If we identify the line of force of this mass during weight-bearing, we note that the knee is aligned lateral to that line of force (Figure 3). The distance between the knee and this line of force is the lever arm for the adduction moment. The longer the lever arm, the greater the adduction moment rotating the tibia into varus. The hallmark of knee OA is varus, which further lengthens the lever arm. Hence we enter a vicious cycle of greater varus, longer lever arm, greater medial loading, and greater medial degradation.
Inertial properties are relevant to the adduction moment only during motion. Because little leg motion occurs during stance, when this moment has its greatest magnitude, inertia likely has a minimal impact on knee OA. The mass of the leg and foot, the distribution of this mass (e.g., is one end of the segment heavier than another?) and the resistance of this mass to acceleration are reflected in inertial properties.13 Two methods alter inertial properties. Placing a 50-lb plaster cast on the leg will increase mass and resistance to acceleration. Alternatively, we may alter acceleration of the leg to change inertia.
Muscle activity can control the distribution of knee loads across the medial and lateral compartments. Weakness, through atrophy or an inability to fully activate muscle, minimizes the ability to dynamically stabilize the knee. Cartilage loss results in ligamentous laxity, which can only be stabilized by sagittal knee muscles, particularly quadriceps.
Identifying potential methods for correcting elements of the adduction moment provides a systematic approach to developing intervention strategies. These include reducing mass, shortening the lever arm, minimizing inertia, and strengthening muscle.
Reducing mass
Obesity increases the risk for knee OA.14 The impact of obesity on knee OA is likely multi-factorial. Recent research explores the possibility of a common pathway of chronic inflammation produced by adiopose cells that leads to both cardiovascular and joint disease.15 Obesity increases the load on the knee, leading to greater demands on the articular cartilage, muscle and ligaments.
Even small amounts of weight loss can dramatically change mechanical knee loading. In a diet and exercise trial of 142 sedentary older adults with symptomatic and radiographic knee OA, each weight loss unit was associated with a four-unit reduction in compressive knee forces and substantial reductions in the adduction moment.16
Thus, not only did the overall compressive load on the knee reduce with weight loss, the bias toward medial loading was also reduced. Loss of only 11.2 lbs reduced the risk for symptomatic knee OA by more than 50% in overweight women with a recent diagnosis of radiographic knee OA.17 Thus weight loss is effective in reducing the mechanical loads that promote knee OA and risk for this disease. However, data supporting weight loss are not as compelling for those with advanced knee OA with varus malalignment.14 It is imperative that at-risk people engage in weight loss before or during the very early stages of knee OA.
Unfortunately, fewer than half of those with knee OA engage in weight loss programs.3 Many are not counseled for weight loss by a healthcare professional or are unable to adhere to exercise and diet long term.3 Both aerobic (e.g., walking, swimming) and strengthening (e.g., quadriceps) exercises are strongly recommended for people with knee OA.18 However, exercise programs must be carefully tailored to ensure that increases in loading exposures do not exacerbate clinical signs and symptoms. Weight loss, even in those who are mildly overweight, should become a mainstay approach very early in the disease process.
Shortening the lever arm
Surgical realignment corrects varus to reduce the lever arm for the knee adduction moment. However, surgery is invasive, expensive and typically implemented in late stage disease. Are conservative strategies available to reduce the lever arm of the adduction moment earlier in the course of knee OA? Conservative interventions proposed to manipulate this lever arm include movement strategies and devices.
Movement strategies involve body segment motions that shorten the lever arm for the knee adduction moment. One strategy is a trunk lean in the direction of the affected knee during a step (Figure 4a). This action moves the body’s center of mass over the knee. In doing so, the lever arm for the adduction moment is shortened and the medial compartment load lessened.19,20 A second strategy is to outwardly rotate the foot during stance. This outward rotation shifts the application point for ground reaction forces (called the center of pressure) laterally to shorten the adduction moment lever arm (Figure 4b).21 However, the impact of these strategies on other joints, such as the lumbar spine and the hip, remains unstudied. As a result, these strategies are not recommended.
Moderate evidence supports “unloading” braces for people with knee OA. These braces are marketed to unload the medial knee compartment through improved stability, correction of varus (sometimes overcorrection to 5° valgus) and a strap that transfers load laterally. While these braces relieve pain and improve quality of life,22-25 conflicting evidence exists regarding the mechanical effect.26 Some studies report a decrease in the adduction moment during stride with use of the brace;24,27 while other studies found no effect.23 Recent work suggests that the mechanisms may not be unloading, but rather alterations in muscle activation patterns around the knee.28
It is possible that a custom fit brace is required to create even modest reductions in the adduction moment.29 A note of caution is warranted, where the fitting must be snug to produce a mechanical or muscle effect. Proper fitting may compromise circulation in some patients. A 2.5 year follow-up study reported a deep vein thrombosis and two incidents of significant knee swelling secondary to unloading brace use.30 Due to these safety concerns, brace use is only recommended with caution in patients with risk factors for deep vein thrombosis, which include obesity.
Orthotic wedging
Foot orthoses with lateral heel wedges are proposed to shorten the lever arm of the adduction moment. Again, reasonable evidence shows that foot orthoses with a lateral wedge reduce pain and improve reports of physical function among people with knee OA.31-34 Wedges of reasonable height for clinical use (5° angle or ¼ inch) are not as effective as those with excessive angles.35,36 The effect of this intervention at the knee remains unclear. Theoretically these insoles may correct femoral-tibial angle or shift the center of pressure at the foot laterally to reduce the lever arm for the adduction moment. However, evidence supporting either effect is conflicting.33-35,37-39 Among the studies showing a significant reduction in the adduction moment, the magnitude appears minimal (6% to 8%), especially when considering the potential for creating undesirable effects at the foot.40 As a result, this approach has not been recommended.41
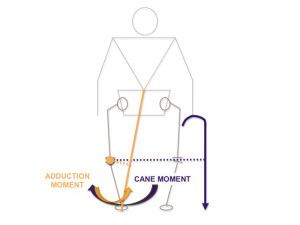
A cane is likely the most effective and safest strategy to reduce the lever arm of the adduction moment. With a cane in the hand opposite the affected knee, two mechanisms reduce the adduction moment. First, pushing down on the cane reduces the body’s ground reaction force. Second, a ground reaction force from the cane introduces a new moment that opposes the adduction moment (Figure 5). Cane use reduced the maximum knee adduction moment by 10% in a group with knee OA.42 It is imperative that the cane is placed contralateral to the affected knee; ipsilateral placement increases the adduction moment.43 Using hiking poles bilaterally during walking, hiking and exercise builds on these principles. Pole use likely has the advantage of offloading some power generation from the lower to upper extremity. Medial knee joint contact forces were reduced by 27% using poles.44 For those whose need for pain relief outweighs potential self-consciousness, canes or poles are likely excellent strategies to manage loads in people with knee OA, at any disease stage. Cane use is strongly recommended.18
Minimizing inertia
Slowed gait speed has been suggested for people with knee OA.45 Slowing gait reduces accelerations of the lower limb and as a result, reduces the magnitude of the adduction moment. Our data, however, show that while the maximum adduction moment is somewhat reduced with large declines in gait speed, the length of stance time and therefore the duration of medial loading are extended. This lengthening of the adduction moment appears to outweigh the benefit of lower magnitude.46 Thus, instruction to slow gait speed is not recommended.
Strengthening muscle
Muscle strengthening is strongly recommended for people with knee OA,18 particularly early in the disease process. Knee extensor muscle weakness increases the risk for radiographic knee OA.47 Those with weak quadriceps and hamstrings experience 21% higher knee loading rates than those with strong knees,48 resulting in greater potential for cartilage damage. Strengthening reduces medial joint loads. An eight-week strengthening program aimed at improving lower extremity strength and neuromuscular control (using closed kinetic chain, proprioceptive and pulley exercises) reduced the peak knee adduction moment by 14% during a single-leg rise from a stool among people with early knee OA.49 Strengthening the quadriceps and hamstrings muscles reduced pain by 23% in 108 older adults with knee pain.50 These pain reductions are comparable to pharmaceuticals – however, using a method that also improves mechanics.
It is critical for clinicians to note, however, that the effectiveness of strengthening is compromised in knees malaligned by 5° or more.51 Excessive varus concentrates contact forces from exercise on the medial compartment. Thus, early intervention cannot be overstated. Compliance is also important, since the beneficial effects of strengthening decline if exercise is ceased.52 People with knee OA likely require individualized programs, where proper dosing requires attention to symptoms, alignment and repetition. Referral to a physical therapist or similarly qualified practitioner is highly recommended18 to ensure that the exercise type, intensity, duration and repetition are carefully monitored and adjusted to avoid exacerbating symptoms.53
Biomechanical research has made significant contributions to the pre-surgical strategies for primary and secondary prevention of knee OA. Although cane use and other methods of shortening the lever arm for the adduction moment can be recommended at any point in the course of knee OA, healthcare providers must implement weight loss and strengthening early enough in the OA disease process to effectively manage symptoms and minimize mechanical pathology.
Monica R. Maly, PhD, PT, is an assistant professor of rehabilitation science at McMaster University in Hamilton, Ontario, Canada and an affiliate investigator at the Arthritis Community Research and Evaluation Unit in Toronto, Ontario, Canada.
Acknowledgments: Natural Sciences and Engineering Research Council of Canada
References
1. Guccione AA, Felson DT, Anderson JJ, et al. The effects of specific medical conditions on the functional limitations of elders in the Framingham Study. Am J Public Health 1994;84(3):351-358.
2. Maly MR, Cott CA. Being careful: A grounded theory of emergent chronic knee problems. Arthritis Rheum 2009;61(7):937-943.
3. Ganz DA, Chang JT, Roth CP, et al. Quality of osteoarthritis care for community-dwelling older adults. Arthritis Rheum 2006;55(2):241-247.
4. Tallon D, Chard J, Dieppe P. Relation between agendas of the research community and the research consumer. Lancet 2000;355(9220):2037-2040.
5. Zhang W, Moskowitz RW, Nuki G, et al. OARSI recommendations for the management of hip and knee osteoarthritis, part 1: Critical appraisal of existing treatment guidelines and systematic review of current research evidence. Osteoarthritis Cartilage 2007;15(9):981-1000.
6. Schnitzer TJ, Popovich JM, Andersson GB, Andriacchi TP. Effect of piroxicam on gait in patients with osteoarthritis of the knee. Arthritis Rheum 1993;36(9):1207-1213.
7. Henriksen M, Simonsen EB, Alkjaer T, et al. Increased joint loads during walking — a consequence of pain relief in knee osteoarthritis. Knee 2006;13(6):445-450.
8. Felson D. Epidemiology of osteoarthritis. In: Brandt KD, Doherty M, Lohmander SL, eds. Osteoarthritis. Oxford: Oxford University Press; 1998.
9. Birmingham TB, Hunt MA, Jones IC, et al. Test-retest reliability of the peak knee adduction moment during walking in patients with medial compartment knee osteoarthritis. Arthritis Rheum 2007;57(6):1012-1017.
10. Koo S, Gold GE, Andriacchi TP. Considerations in measuring cartilage thickness using MRI: factors influencing reproducibility and accuracy. Osteoarthritis Cartilage 2005;13(9):782-789.
11. Zhao D, Banks SA, Mitchell KH, et al. Correlation between the knee adduction torque and medial contact force for a variety of gait patterns. J Orthop Res 2007;25(6):789-797.
12. Hurwitz DE, Sumner DR, Andriacchi TP, Sugar DA. Dynamic knee loads during gait predict proximal tibial bone distribution. J Biomech 1998;31(5):423-430.
13. Winter D. Biomechanics and Motor Control of Human Movement. 2nd ed. New York: Wiley-Interscience Publication; 1990.
14. Niu J, Zhang YQ, Torner J, et al. Is obesity a risk factor for progressive radiographic knee osteoarthritis? Arthritis Rheum 2009;61(3):329-335.
15. Messier SP. Obesity and osteoarthritis: disease genesis and nonpharmacologic weight management. Rheum Dis Clin North Am. 2008;34(3):713-729.
16. Messier SP, Gutekunst DJ, Davis C, DeVita P. Weight loss reduces knee-joint loads in overweight and obese older adults with knee osteoarthritis. Arthritis Rheum 2005;52(7):2026-2032.
17. Felson DT, Zhang Y, Anthony JM, et al. Weight loss reduces the risk for symptomatic knee osteoarthritis in women. The Framingham Study. Ann Intern Med 1992;116(7):535-539.
18. Zhang W, Moskowitz RW, Nuki G, et al. OARSI recommendations for the management of hip and knee osteoarthritis, part II: OARSI evidence-based, expert consensus guidelines. Osteoarthritis Cartilage 2008;16(2):137-162.
19. Hunt MA, Birmingham TB, Bryant D, et al. Lateral trunk lean explains variation in dynamic knee joint load in patients with medial compartment knee osteoarthritis. Osteoarthritis Cartilage 2008;16(5):591-599.
20. Mundermann A, Asay JL, Mundermann L, Andriacchi TP. Implications of increased medio-lateral trunk sway for ambulatory mechanics. J Biomech 2008;41(1):165-170.
21. Rutherford DJ, Hubley-Kozey CL, Deluzio KJ, et al. Foot progression angle and the knee adduction moment: a cross-sectional investigation in knee osteoarthritis. Osteoarthritis Cartilage 2008;16(8):883-889.
22. Kirkley A, Webster-Bogaert S, Litchfield R, et al. The effect of bracing on varus gonarthrosis. J Bone Joint Surg Am 1999;81(4):539-548.
23. Hewett TE, Noyes FR, Barber-Westin SD, Heckmann TP. Decrease in knee joint pain and increase in function in patients with medial compartment arthrosis: a prospective analysis of valgus bracing. Orthopedics 1998;21(2):131-138.
24. Lindenfeld TN, Hewett TE, Andriacchi TP. Joint loading with valgus bracing in patients with varus gonarthrosis. Clin Orthop Relat Res 1997;(344):290-297.
25. Brouwer RW, van Raaij TM, Verhaar JA, et al. Brace treatment for osteoarthritis of the knee: a prospective randomized multi-centre trial. Osteoarthritis Cartilage 2006;14(8):777-783.
26. Beaudreuil J, Bendaya S, Faucher M, et al. Clinical practice guidelines for rest orthosis, knee sleeves and unloading knee braces in knee osteoarthritis. Joint Bone Spine 2009 May 19 [epub ahead of print].
27. Pollo FE, Otis JC, Backus SE, et al. Reduction of medial compartment loads with valgus bracing of the osteoarthritic knee. Am J Sports Med 2002;30(3):414-421.
28. Ramsey DK, Briem K, Axe MJ, Snyder-Mackler L. A mechanical theory for the effectiveness of bracing for medial compartment osteoarthritis of the knee. J Bone Joint Surg Am 2007;89(11):2398-2407.
29. Draganich L, Reider B, Rimington T, et al. The effectiveness of self-adjustable custom and off-the-shelf bracing in the treatment of varus gonarthrosis. J Bone Joint Surg Am 2006;88(12):2645-2652.
30. Giori NJ. Load-shifting brace treatment for osteoarthritis of the knee: a minimum 2 1/2 year follow-up study. J Rehabil Res Dev 2004;41(2):187-194.
31. Keating EM, Faris PM, Ritter MA, Kane J. Use of lateral heel and sole wedges in the treatment of medial osteoarthritis of the knee. Orthop Rev 1993;22(8):921-924.
32. Sasaki T, Yasuda K. Clinical evaluation of the treatment of osteoarthritic knees using a newly designed wedged insole. Clin Orthop Relat Res 1987;(221):181-187.
33. Butler RJ, Marchesi S, Royer T, Davis IS. The effect of a subject-specific amount of lateral wedge on knee mechanics in patients with medial knee osteoarthritis. J Orthop Res 2007;25(9):1121-1127.
34. Kakihana W, Akai M, Nakazawa K, et al. Inconsistent knee varus moment reduction caused by a lateral wedge in knee osteoarthritis. Am J Phys Med Rehabil 2007;86(6):446-454.
35. Kerrigan DC, Lelas JL, Goggins J, et al. Effectiveness of a lateral-wedge insole on knee varus torque in patients with knee osteoarthritis. Arch Phys Med Rehabil 2002;83(7):889-893.
36. Baker K, Goggins J, Xie H, et al. A randomized crossover trial of a wedged insole for treatment of knee osteoarthritis. Arthritis Rheum 2007;56(4):1198-1203.
37. Maly MR, Culham EG, Costigan PA. Static and dynamic biomechanics of foot orthoses in people with medial compartment knee osteoarthritis. Clin Biomech 2002;17(8):603-610.
38. Crenshaw SJ, Pollo FE, Calton EF. Effects of lateral-wedged insoles on kinetics at the knee. Clin Orthop Relat Res 2000;(375):185-192.
39. Barrios JA, Crenshaw JR, Royer TD, Davis IS. Walking shoes and laterally wedged orthoses in the clinical management of medial tibiofemoral osteoarthritis: a one-year prospective controlled trial. Knee 2009;16(2):136-142.
40. Butler RJ, Barrios JA, Royer TD, Davis IS. Effect of laterally wedged foot orthoses on rearfoot and hip mechanics in patients with medial knee osteoarthritis. Prosth Orth Int 2009;33(2):107-116.
41. Reilly KA, Barker KL, Shamley D. A systematic review of lateral wedge orthotics — how useful are they in the management of medial compartment osteoarthritis? Knee. 2006;13(3):177-183.
42. Kemp G, Crossley KM, Wrigley TV, et al. Reducing joint loading in medial knee osteoarthritis: Shoes and canes. Arthritis Rheum 2008;59(5):609-614.
43. Chan GN, Smith AW, Kirtley C, Tsang WW. Changes in knee moments with contralateral versus ipsilateral cane usage in females with knee osteoarthritis. Clin Biomech 2005;20(4):396-404.
44. Fregly BJ, D’Lima DD, Colwell CW Jr. Effective gait patterns for offloading the medial compartment of the knee. J Orthop Res 2009 Jan 15 [epub ahead of print].
45. Mundermann A, Dyrby CO, Andriacchi TP. Secondary gait changes in patients with medial compartment knee osteoarthritis: increased load at the ankle, knee and hip during walking. Arthritis Rheum 2005;52(9):2835-2844.
46. Robbins S, Maly M. The effect of gait speed on the knee adduction moment depends on waveform summary measures. Gait Posture [submitted].
47. Slemenda C, Heilman DK, Brandt KD, et al. Reduced quadriceps strength relative to body weight: a risk factor for knee osteoarthritis in women? Arthritis Rheum 1998;41(11):1951-1959.
48. Mikesky AE, Meyer A, Thompson KL. Relationship between quadriceps strength and rate of loading during gait in women. J Orthop Res 2000;18(2):171-175.
49. Thorstensson CA, Henriksson M, von Porat A, et al. The effect of eight weeks of exercise on knee adduction moment in early knee osteoarthritis — a pilot study. Osteoarthritis Cartilage 2007;15(10):1163-1170.
50. O’Reilly SC, Muir KR, Doherty M. Effectiveness of home exercise on pain and disability from osteoarthritis of the knee: a randomised controlled trial. Ann Rheum Dis 1999;58(1):15-19.
51. Sharma L, Dunlop DD, Cahue S, et al. Quadriceps strength and osteoarthritis progression in malaligned and lax knees. Ann Internal Med 2003;138(8):613-619.
52. van Baar ME, Dekker J, Oostendorp RA, et al. Effectiveness of exercise in patients with osteoarthritis of hip or knee: nine months’ follow up. Ann Rheum Dis 2001;60(12):1123-1130.
53. Bennell KL, Hunt MA, Wrigley TV, et al. Role of muscle in the genesis and management of knee osteoarthritis. Rheum Dis Clin North Am. 2008;34(3):731-754.
FIGURE CAPTIONS
Figure 1: The knee adduction moment, or torque, tends to rotate the tibia in a varus or bowlegged position on the femur. The adduction moment describes a tendency for the tibia to rotate in the frontal plane, where the axis of rotation is located inside the knee joint. This measure is calculated from the forces exerted by the ground onto the body (from a force plate) and the accelerations of the lower extremity (from motion capture cameras) during walking. Calculations to determine the magnitude of the adduction moment are complex and account for ankle and foot segments (an “inverse dynamics approach” described by D. Winter13). However, a simplistic calculation of adduction moment is the product of the lever arm and the vertical ground reaction force equal and opposite to body mass.
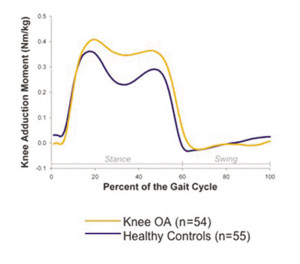
Figure 2: The magnitude of the adduction moment varies throughout different points of the stride. Stride for one leg is characterized by a stance phase, beginning at heel strike denoted by 0% and ending with the transition into swing phase at 60%. The adduction moment is most important during stance phase, when the foot is transferring body weight onto the ground. The mean adduction moment for a healthy group of older adults (blue) and a knee OA group (orange) are presented over the period of one stride. Compared to the healthy older adults, the knee OA group demonstrates an elevated knee adduction moment throughout stance phase. [Maly unpublished findings]
Figure 3: The line of force for body mass extends from the point of application of forces beneath the foot (called the center of pressure) and the center of mass for the body. The distance between this line and the center of the knee joint is the lever arm for the knee adduction moment. The lever arm must be drawn perpendicular to the line of force for the body. The longer this lever arm is, the larger the adduction moment will be, tending to rotate the tibia into varus on the femur. Many conservative treatment strategies aim to shorten the lever arm.
Figure 4: Movement strategies proposed to shorten the lever arm for the adduction moment. A) Trunk lean toward the same side as the affected knee shifts the center of mass for the body ipsilaterally. This shift of the center of mass shortens the lever arm for the adduction moment. B) Outward rotation of the foot shifts the center of pressure underneath the foot laterally. This shift of the center of pressure shortens the lever arm for the adduction moment.
Figure 5: Contralateral cane use is believed to introduce a new moment, in the opposite direction from the adduction moment. The lever arm for the cane is long. As a result, the cane moment can be very large even if little force is placed on the cane.











Hi,
It was a very useful article for me. Thanky you very much.
Verena Metzler
Motion Lab
St. Gallen
Switzerland
Thank you! This was a very useful article for me, both personally and at my job.
Hello!
Would you be so kind to clue me in about the author of “the knee adduction moment theory”. There are some discrepancies with the rules dealing with force vectors. I’d like to get to know some lowdown on what lies in the core of the theory.
Thank you in advance
Sincerely, Dr Vladimir Petrunko
And some more about the figures of the article. Firstly, “Line of force” can’t exist because force is a vector quantity and MUST have a direction. Secondly, there is no axis of rotation marked in the figures. In this case it is difficult to say about the moment of force of the knee or anything else. By the way, in the OARSI Primer in the subchapter dealing with Non pharmacological approach to the knee OA (osteoarthritis) there is another version of force vectors. Anyway that figure is not MORE clear than the figures in your article. Many researchers mention this knee adduction moment but their illustrations are open to doubts.
Dr. Vladimir Petrunko