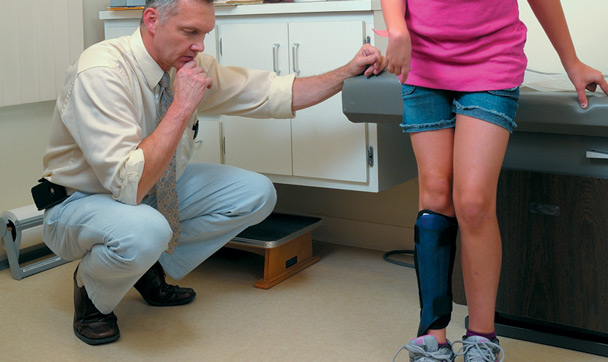
Photos by Vincent Giordano/Trinacria Photography (www.trinacriaphotography.com), courtesy of Clinical Prosthetics & Orthotics.
A recent paper suggests that a checklist system can help practitioners educate caregivers about orthotic device use in children with CP, which could improve compliance. But experts differ as to whether such checklists make sense in the complex world of O&P devices.
By Larry Hand
A serious grocery shopper never leaves home without a list of items to check off as a shopping cart fills up. Could lower extremity practitioners improve compliance and outcomes in children with cerebral palsy (CP) by providing similar checklists for caregivers regarding the use of ankle foot orthoses (AFOs)?
Such a practice could be very beneficial, some say. But others think the heterogeneity of orthotic designs and caregiver environments make it difficult to boil the care down to a list that would be simple enough for caregivers, who have their hands full already, to utilize.
The concept has proven highly successful in operating rooms. The World Health Organization launched an initiative in 2008 urging operating room personnel to use a simple one-page checklist before surgery. That list, developed in conjunction with Harvard surgeon Atul Gawande, MD, lists simple steps to take in the OR before inducing anesthesia, before skin incision, and before patients leave from surgery. A follow-up study published a year later in the New England Journal of Medicine involved eight hospitals in six WHO regions and showed that inpatient deaths fell by more than 40% following implementation of the checklist.
“Checklists are always a good idea,” said Tom DiBello, CO, of Dynamic Orthotics and Prosthetics in Houston. “The proper application of an orthosis is a big deal. If you don’t have the device appropriately applied, it’s not going to function correctly.”
 An article in the May/June issue of Orthopaedic Nursing offered a simple protocol that nurses could offer caregivers regarding the use of lower extremity orthoses in children with spastic quadriplegic CP. The protocol lists 13 items, from “Describe the purpose” to “Describe skin care” to “Wear the orthoses as prescribed,” and has signature lines for a nurse, patient, and caregiver.
An article in the May/June issue of Orthopaedic Nursing offered a simple protocol that nurses could offer caregivers regarding the use of lower extremity orthoses in children with spastic quadriplegic CP. The protocol lists 13 items, from “Describe the purpose” to “Describe skin care” to “Wear the orthoses as prescribed,” and has signature lines for a nurse, patient, and caregiver.
“Critical to the care of a child wearing orthoses is teaching family and significant others orthoses management,” wrote author Kathleen Cervasio, PhD, EdD, CCRN, RN, ACNS-BC, professor of nursing at Long Island University in Brooklyn, NY.
Spasticity is the most common impairment in children with CP, and about 85% of patients are required to wear orthotic devices to help reduce muscle tone and avoid orthopedic complications when standing, according to an article by Swedish researchers published in the July 2007 issue of the European Journal of Paediatric Neurology.
Cervasio said she wrote the article because nurses have not been offered such training before.
“I really wanted to make it very simple so that everybody could follow it,” Cervasio said in an interview. “I geared it to nursing because I am a nurse, but it can be checked off by anyone.”
Her article was based on a literature review from orthotists, physicians, and physical therapists.
“Increasingly, nursing needs to collaborate with other disciplines to share knowledge bases in clinical care,” she wrote in her summary.
She said in August that since publication of the article, she’s had numerous comments from hospital and home care professionals, with many organizations adopting the protocol as a procedure for caring for patients with orthotic devices. She said that the protocol had been added as a competency to school of nursing skills check-off lists, as well as to content in syllabi for nursing students.
Although orthotists typically comprise the first line of practitioners for educating patients and caregivers, DiBello said the interest of Cervasio and other nursing professionals is noteworthy.
“As an industry we need to educate these folks more effectively, possibly through their education or continuing education courses,” DiBello said. “There’s no reason we couldn’t include these specialized nurses [in the continuum of care].”
A familiar concept
 The concept of a checklist may not be new to some lower extremity specialists working with CP patients, though they may know it by a different name.
The concept of a checklist may not be new to some lower extremity specialists working with CP patients, though they may know it by a different name.
“I think most practitioners actually do follow a very similar checklist to what she presented,” commented Brigid Driscoll, CO, PT, at Children’s Memorial Hospital in Chicago. “The article is a nursing paper, and it appears to be addressing orthotic management for children with more significant involvement that require home care nursing, but the checklist is still appropriate across children with cerebral palsy. We also use a very similar checklist. We call it the ‘wear and care’ guideline, which has almost the exact outline that she uses. She really hit the nail on the head as to what we need to teach patients and family members.”
Carey Jinright, CO, of Precision Medical Solutions in Montgomery, AL, suggested Cervasio’s recommendations should be a wake-up call for orthotists.
“As an orthotist I felt that her recommendations were spot on,” Jinright said, “but many times she pointed out that these concepts are not taught in nursing school or covered in textbooks on nursing. The reason these concepts are not taught in nursing school is because they fall under the orthotist’s scope of practice. We need to make sure that the patient and caregiver are fully aware of their braces, and they should educate the nurses about the use and function of their particular brace at their follow-up appointment.”
Driscoll said checklists could be helpful in at least 50% of her practice in orthotics and physical therapy.
“They can help ensure that the practitioner covers all topics when they’re fitting a device for the child,” she said. “And for the family, checklists are useful just to make sure they know how to use the device at home, they know the purpose of it, and they know the overall care procedures.”
Skin care should be emphasized, she added.
“The biggest risk of using an orthotic device is pressure sores or skin irritation problems,” Driscoll said. “[Cervasio] does a really nice job outlining that.”
Many of the points in the paper are part of routine orthotic checkout procedure, DiBello said.
“The thing that’s missing is any kind of a closed loop,” he said. “In [Cervasio’s] process the caregiver has to go through this checklist and then sign off on it. We do have our patients sign that they have received advice, and included in that advice have been written and oral instructions, but it’s probably unlikely in most orthotic practices that clinicians present a document that a patient has to sign off on that is similar to the one in this article.”
He said a checklist could be useful in a “very high” percentage of his practice, which consists of prescribing custom devices for complicated orthotic problems.
At least one physical therapist is skeptical about the feasibility of the checklist concept.
“I doubt if a checklist would be used,” said Sue Murr, DPT, PCS, manager of neuroscience programs and the cerebral palsy program at Gillette Children’s Specialty Healthcare Hospital in St. Paul, MN. “Families have too many things to do and are too busy to use one. They’re lucky if they get the socks on without wrinkles and get the straps on. To use a checklist, I just don’t think it is practical.”
Checklist challenges

The checklist devised for nurses to educate caregivers of children with CP. Reprinted with permission from: Cervasio K. Lower extremity orthoses in children with spastic quadriplegic cerebral palsy. Orthop Nurs 2011;30(3):155-159.
For a checklist to work for patients wearing orthotic devices, it would have to be written specifically for each type of device, practitioners say, and a multidisciplinary approach is always necessary for follow-up care.
A checklist that accounts for a patient’s ability to function with a device may help in situations in which a child is transitioning from one device to another, Driscoll said.
“When you fit an orthotic device on a child, your goal is to improve their overall function. Sometimes, when initially transitioning to a new device, function can actually be compromised,” she said. “This often means having a physical therapist work on strengthening, postural control, and gait training to help the child become more proficient in using the new orthosis. For example, some kids may originally use an AFO, which is going to provide more support, transition to an SMO [supra-malleolar orthosis], and then again work with a physical therapist to achieve the strength they require in addition to any other alignment or postural factors that would allow them to effectively utilize the new orthotic device.”
But orthotic device wear is complicated, other practitioners point out. A checklist would have to be tailored to the condition and the patient, Jinright explained. He cited some examples of characteristics to assess, including:
- The presence of a scissoring gait;
- Range of motion, spasticity, tone, and synergistic patterns in gait for each lower extremity joint;
- Crouch gait, as well as transverse plane motion from the pelvis to the hindfoot;
- Extension of the trunk and other compensation patterns used to maintain upright posture, if any;
- Motion at the sternum during the gait cycle;
- Symmetry of the shoulders in stance as well as during walking; and
- Field of vision and the ability to maintain an adequate field of vision.
All braces have a break-in period during which wear time gradually increases, and during which patients need to check for pressure sores after a few hours of wear time. But, Jinright noted, that is where the similarities between devices end and where more detailed explanation may be necessary.
“Every brace functions in a different way based on its nomenclature,” he said. “In the case of AFOs, if a brace allows motion, the patient should have this explained to them, not be left to find out about this motion during their initial function in the brace! If a brace is going to immobilize an extremity that has been flaccid, again, the patient should have this explained and demonstrated to them prior to functioning in the brace.”
When it comes to the limitations of orthotic device wear, honesty really can be the best policy.
“I have found that in my clinic if I will go ahead and point out the negatives to the patient and the caregiver, it decreases stress and anxiety,” he said. “If I say, muscle soreness is common in the first few days of use, or tell them to watch for redness with a new brace, this seems to thwart their anxiety when they do feel soreness or pressure. Many times as clinicians it seems that we want to point out all of the good points and benefits of a brace and downplay the break-in period that all braces require.”
Jinright said his clinic uses checklists in probably 60% of administrative work but only about 5% of clinical work, and only for patients with diabetes who require therapeutic shoes.
Jinright outlined some specific steps practitioners can take to help children and their caregivers understand how orthoses work and how to wear them correctly:
- Explain—in lay terms—the functionality of the brace and the reason for the specific design;
- Show pictures or actual appliances to all parties involved;
- Talk to the patient and caregiver during the initial evaluation;
- Have the patient and caregiver show, not just explain, how they apply and remove a brace; and
- For custom-fabricated devices, make sure all parties are fully informed and on board before fabrication.
The checklist bandwagon
In addition to the WHO’s safe surgery checklist, the organization also has deployed influenza checklists and a trauma care checklist. And its surgical checklist continues to be evaluated by various disciplines around the world. For instance, a group of head and neck surgeons in Finland concluded in a paper published in the June issue of Clinical Otolaryngology that the checklist fits well into their working process. One author wrote in the April-June issue of Critical Care Nursing Quarterly that hospitals need to “manage a culture that embraces checklists.”
Checklists are also being used effectively in other areas of bone and joint care. The Journal of Orthopaedic Surgery and Research e-published an article on April 18 that tried to answer the question: “Can the surgical checklist reduce the risk of wrong site surgery in orthopaedics?” The researchers analyzed data from the U.K.’s National Patient Safety Agency database between January 1 and December 31, 2008, and concluded that use of a checklist could have prevented 28 of 133 patient safety incidents.
This makes sense to Jinright, who has been a surgical representative for four major companies.
“We always perform a ‘timeout’ in the OR prior to a case starting,” Jinright said. “This is the time that we check off what procedure is being performed on what extremity, and everyone who is in the room. We discuss what appliance will be used and the start time of the case. All of these concepts are a checklist approach. The same protocol happens before each case.”
The simplicity of this concept, however, may limit its applicability to O&P, he said.
“In the O&P field, I believe a checklist would be difficult to follow,” Jinright said. “I feel that there are so many variables that need to be addressed for different conditions that you would need 40 different checklists to treat a day’s worth of patients.”
Larry Hand is a writer based in Massachusetts.