Night splinting for plantar fasciitis gets the lion’s share of attention, but lower extremity practitioners are also seeing positive results with night use of orthoses for conditions ranging from cerebral palsy to AIDS.
By Larry Hand
Although a limited collection of published studies has yielded mixed results regarding the nighttime use of splints or other orthotic devices for various conditions, practitioners say they get positive results and use night splinting or bracing regularly to ease pain and to help children achieve normal lower extremity development.
Practitioners also say the effects of the splinting or bracing outweigh the inconveniences of donning and wearing the devices.
“Orthotic devices worn at night can be very effective, especially in children who are still growing,” said Brigid Driscoll, CO, PT, senior physical therapist and senior orthotist at Children’s Memorial Hospital in Chicago. “By keeping their muscles in a lengthened position while they are sleeping, you are allowing their muscles to grow at an equal rate to the bone within the joint. Therefore you are correcting or avoiding contractures at a joint.”
Conditions for which night orthoses are often used include plantar fasciitis, cerebral palsy, myelomeningocele, and muscular dystrophy.
In patients with plantar fasciitis, night splinting can help to alleviate pain by lengthening the plantar fascia, which also reduces inflammation.
In patients with cerebral palsy, when spasticity and weakness are present, night orthoses are used to maintain muscles in a lengthened position to avoid contractures. If contractures have already developed, night orthoses can help a child to regain the necessary functional range of motion.
In patients with myelomeningocele, antagonist muscles that typically stabilize a joint are often not equally innervated. Due to the strength imbalance at a specific joint it is not uncommon for contractures to develop. Night splints can be used to improve range of motion and align joints for functional use, most often for weight bearing, or to prevent contractures from developing. Because the extremities are more static while sleeping than awake, and because patients with myelomeningocele often have compromised sensation, close monitoring of skin integrity is essential, Driscoll said.
Night splints are also sometimes used in patients with muscular dystrophy, in whom progressive muscle weakness leads to contracture, particularly when patients have degenerated to the point where they stop walking. However, scientific evidence to support night orthosis utilization in this population is limited, Driscoll said.
“Night orthotic management is not well researched, and often night splinting for contractures is reactionary rather than preventive,” she said.
The literature
Although not a lot of research has been published lately on night splinting, a Dutch study published in the March-April issue of Research in Developmental Disabilities found that use of night orthoses did not have a significant negative effect on sleep quality in children with CP. In the November 2002 issue of Orthopedics, researchers from Ohio reported that use of an ankle dorsiflexion splint at night by patients with recalcitrant plantar fasciitis patients improved pain and sleep symptoms. Similarly, a December 1996 Foot & Ankle International study from Johns Hopkins Hospital in Baltimore found that a combination of night splint and shoe modification improved plantar fasciitis symptoms at 16 months. And in a June 2010 study in the Journal of Physiotherapy (formerly the Australian Journal of Physiotherapy), Australian researchers found that night use of removable casts significantly improved ankle dorsiflexion range of motion in Charcot-Marie-Tooth patients after four weeks compared to a group that received no intervention, although there were no between-group differences at eight weeks.
Not all of the results have been positive, however. In the July 2010 issue of the British Journal of Sports Medicine, Dutch investigators found that adding night splinting to an exercise program for patients with Achilles tendinopathy did not significantly affect functional outcome one year later. A prospective randomized study by Texas researchers, published in the November 1999 issue of Clinical Orthopaedics and Related Research, found that adding night splints to a treatment protocol of oral antianflammatory drugs, stretching, and shoe recommendations did not significantly improve plantar fasciitis outcomes. And six weeks of night splint use did not significantly increase ankle range of motion or strength in a study of CMT patients published in the September 2006 issue of AJP.
Out of the box
Practitioners in Houston demonstrated recently how stepping outside the box of normal guidelines for treating painful peripheral neuropathy achieved improvements in pain management and sleep quality for HIV/AIDS patients. Almost all HIV patients report painful foot and calf cramps and pain at night that interferes with quality and amount of sleep, said Roberto Sandoval, PT, of the Thomas Street Health Center in Houston.
Sandoval and colleagues published their initial findings in a pilot study in the November 2010 issue of the Journal of the International Association of Physicians in AIDS Care. And in an ongoing follow-up study, patients continue to show improvements, Sandoval said. The research is dissertation work for his PhD.
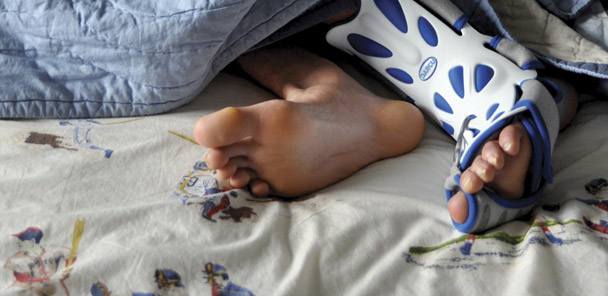
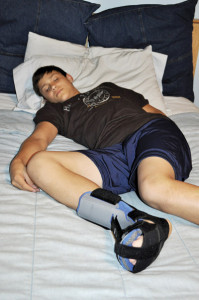
Sandoval and colleagues recruited 22 patients to either use bilateral one-piece injection molded walkabout splints fitted with rocker bottoms for ambulation over a three-week period or to participate in a seated placebo upper extremity exercise program. The device was a lightweight open heel walkabout splint for the foot and limb up to the calf that blocked a plantar flexion moment by positioning the plantar flexor muscles (e.g., soleus, gastrocnemius) in a neutral position at the ankle.
After the three weeks, plus a one-week washout period, they switched protocols for all participants. Both protocols were associated with decreased Neuropathic Pain Scale (NPS) and Pittsburgh Sleep Quality Index (PSQI) mean scores, but the participants in the exercise arm showed significantly smaller reductions in scores for both pain and sleep.
“When you look at a lot of neuropathy interventions, the main focus has been on pharmacological management,” Sandoval said. “However, some of the medications are topical applications, so there seems to be a topical or peripheral aspect to managing pain.”
Neuropathy involves an imbalance of excitatory and inhibitory inputs, he added.
“More specifically, we’re dealing with glutamate and GABA [gamma-amino butyric acid] neurotransmitters, with GABA being inhibitory in nature compared to glutamate. That’s clearly out of balance when people have neuropathy and neuropathy-related damage, because of the damage to the nerves and impact on the CNS [central nervous system]. That led me to look into peripheral means of increasing and optimizing the inhibitory stimuli on some of my patients,” Sandoval said.
First, he conducted an informal focus group session in which patients revealed that cramping and allodynia often made it difficult to sleep at night.
“At first, it was complete trial and error,” Sandoval said. “I wanted to see if a physical block would stop any of those cramps that my clients were complaining about. A muscle cramp is more than just a full contracture of a muscle, so if you can stop it midway, at least it won’t get to the point that it’s going to contract and start developing some lactic acid buildup and cause a lot of pain.”
Case studies suggested that night splinting seemed to work, so he launched the formal trial. He likened the technique, primarily the physical block to contracture and secondarily the inhibiting quality of the splint’s full contact, to comforting a crying baby.
“The first thing you do is try to cradle the baby, because as you cradle that baby, the full contact of the skin is going to provide an inhibitory input through the CNS,” Sandoval said.
In his first study, he said he could attribute about 40% of the pain reduction to use of the splints, and the numbers are ranging between 40% and 70% in his ongoing follow-up study.
“That leads me to conclude that the effect size is large in magnitude. The larger the magnitude, the shorter the application time before you start seeing results. Clients who have been experiencing a lot of pain, if they wear the splints as instructed, you notice some pain reduction at the plantar aspect of the foot within a couple of days, and cramps pretty much disappear within a week or two,” Sandoval said.
He believes his results may be applicable to neuropathic patients outside the HIV population. In patients with diabetic peripheral neuropathy, for instance, once glucose is brought under control, mechanical interventions such as splints can be used to control secondary symptoms, he said.
“At the core, in neuropathy, once the nerve damage is done, the reverberating loop and imbalance in glutamate and GABA seems to be consistent across all disease processes,” Sandoval said.
Differences by diagnosis
Clinical utilization of night splinting or bracing depends on the condition being treated, said Robert Lin, CPO, chief orthotist for Hanger Orthopedic Group at Children’s Medical Center in Hartford, CT.
In adults or children with plantar fasciitis, for example, night splints can be particularly effective for treating the pain that occurs with a patient’s first steps out of bed in the morning; sleeping with the feet in plantar flexion often causes the plantar fascia to tighten during the night.
“I won’t treat plantar fasciitis personally with foot orthotics unless the patients are agreeable to wearing a night brace,” he said. “[Otherwise] it just becomes a nightmare. They keep coming back and saying the arch supports aren’t doing anything. Every morning, they’re reinjuring the plantar fascia. If they’re agreeable to wearing some type of night positioning device, then they wear the arch supports [in the daytime] to complement the treatment; it’s really part of the treatment plan.”
He said instead of a splint he often uses a pressure relief AFO, or any device that keeps the ankle at 90°.
For children with cerebral palsy (CP), traumatic brain injury, or other CNS disorders, he uses night splinting to maintain range of motion in patients with neuromuscular imbalance.
“We use it very religiously in pediatrics. The muscles grow by stretching, and research shows that maximum amount of growth hormone emittance is during the middle of the night,” he said, referring to a study published in the November-December 2004 issue of the Journal of Pediatric Orthopaedics. “Your growth occurs at the end of the bone and the soft tissue doesn’t catch up. There’s a muscle imbalance. So it’s sort of the perfect storm for a contracture developing, particularly in the heel cords. During the periods of growth we will very aggressively brace at night.”
For that application he would use a no-load passive stretch that keeps the ankles as close to 90° as possible, so the children don’t sleep with their feet in maximum plantar flexion.
Part of a plan
Night splinting is usually one element of an overall treatment plan, said John Brinkmann, CPO, LPO, of Rockford Orthopedic Associates in Rockford, IL.
“Orthotists need to be aware of the other treatments that are in place for the specific problem, and orthotic recommendations need to take into consideration the complications associated with each disease process or condition,” he said. “A patient with tone, for instance, will be managed differently than severe burn patients or otherwise healthy individuals with plantar fasciitis. And splinting for CP patients will need to take into account physical therapy goals and the design of orthoses used for ambulation.”
He said he usually cuts out the heel of custom AFOs/KAFOs when he supplies orthoses for nighttime use.
“This reduces the risk of heel ulceration due to pressure or maceration of the skin due to excessive perspiration,” he said. “However, this design makes the device less stable and durable for weightbearing and ambulation. Conflicting functional goals for daytime and nighttime orthoses often require that different orthoses be provided for each scenario.”
The compliance issue
 Of course, as with many other treatments, compliance with night use of orthoses can be a challenge. However, practitioners agree that good education, coaching, and follow-up can improve compliance, even among children. Being specific when describing the device being supplied, how to fit it, and any expected benefits goes a long way.
Of course, as with many other treatments, compliance with night use of orthoses can be a challenge. However, practitioners agree that good education, coaching, and follow-up can improve compliance, even among children. Being specific when describing the device being supplied, how to fit it, and any expected benefits goes a long way.
“Sometimes we’ll have the parents don the brace while a child is asleep,” Lin said. “It goes on the outside of the pajamas and is a fairly generic fit. Just make sure the Velcro strap is loose before starting because the tearing sound could wake a child up.”
Other times, he added, the parent can brace one foot at a time instead of bilateral application. He considers device wear for at least half the hours of sleep—four to six hours—to be good compliance. Driscoll agrees, citing a study in the February 1988 issue of Developmental Medicine and Child Neurology.
Night orthoses may require an adjustment period, Sandoval said.
“Because we deal with people with HIV, the clients tend to be very compliant with most recommendations. In my experience, I’ve noticed it takes about a week or a week and a half to get used to using the splints at night. There is always a period of adjustment where the client needs to try it out to see this is something he can live with.”
An important part of making that adjustment, Driscoll said, is being careful not to do too much too soon.
“One of the most common mistakes in making an orthosis, for night or day, is putting the joint in too much range of motion and creating a painful stretch within the device,” she said. “The orthotic device should be set at the R1 measurement. This is defined as the place where a muscle stops when passively moving through its joint range. This is considered the full length of the muscle, and it is a position that will allow a patient to rest comfortably within the device.”
If a device has adjustable joints, patients who attempt to make adjustments on their own may set the joint in too much range of motion, causing an excessive stretch and pain and discomfort.
“Off-the-shelf night orthoses have the potential to cause problems merely due to the fact that they are not a custom fit, and the device may not properly align with anatomical landmarks,” Driscoll said.
Because they are not typically worn while weightbearing, night orthoses can be made out of more comfortable materials, like polyethelene, which can improve patient tolerance and compliance, Driscoll said. Padding and liners can sometimes make devices hot and less tolerable, she added.
Practitioners should also be aware that patients and caretakers tend to over-report wear times, Brinkmann said.
“I’ve given patients a printed calendar for recording actual wear times each day or night, and asked them to bring that with them at each follow up appointment. I record the patient’s reported compliance and my own observations as part of every follow-up encounter,” he said.
Practitioners should proactively schedule follow-up appointments rather than wait for patients to call if they are having a problem, Brinkmann added.
“These appointments not only give the orthotist an opportunity to make necessary adjustments, but may actually improve compliance by providing a sentinel effect,” he said.
In summary
Lin sees night use of orthoses as a benign, passive treatment method that is likely being underutilized.
“I’m surprised when I learn that this isn’t universal across the board,” he said. “Every child that’s had some type of invasive procedure like a percutaneous heel cord lengthening, very often they’ll just go into day braces but not sleep in anything, and I think that’s a huge disservice. They’re just going to recontract right away, and they’ll have to go back in for the casting, or the Botox [botulinum toxin], or surgery.”
Perhaps best of all, nighttime devices can be effective in young patients who may not even realize they’re wearing a device.
“They’re sound asleep anyway,” Lin noted. “It’s a very effective adjunct to the aggressive day therapy.”
Larry Hand is a writer based in Massachusetts.












I am interested in references that substantiate the effectiveness of night bracing of any diagnosis mentioned. When sleeping the body heals and grows, but where is a double blind study showing that the tendons and ligaments will lengthen with night orthoses better than with an appropriate and compliant stretching program mentored and monitored by a Physical Therapist? Are there any studies showing muscle activity while sleeping that would have the stronger muscles groups create the potential for increased contractures or are the muscles inactive and not contributory during sleep?
I have not tried night splinting yet, but wish to do so. It seems to me that by maintaining good alignment overnight any physical therapy undertaken during the day starts from a better baseline. But of course I am not a professional and my ideas have not been peer-reviewed by medics. With all due respect I just have 50 years of symptoms of FSHD behind me.