 When calluses or ulcers develop on the distal aspect of the lesser toes, offloading pressure from the distal end of the digit is essential for healing to occur. Research suggests that toe crest pads offer an inexpensive but effective means of offloading and healing these distal wounds.
When calluses or ulcers develop on the distal aspect of the lesser toes, offloading pressure from the distal end of the digit is essential for healing to occur. Research suggests that toe crest pads offer an inexpensive but effective means of offloading and healing these distal wounds.
By Monica Melo, DNP, RN, ACNS-BC, CWOCN, CFCN
Treatment of distal toe calluses and ulcerations can be particularly challenging. The presence of multiple comorbidities, combined with toe deformity and the minimal amount of bone-covering tissue at the distal toe, can lead to the need for invasive treatments to achieve healing. These treatments can include revascularization through angioplasty, stenting, bypass, or a combination of procedures. Surgical correction of toe deformities can also be attempted to reduce pressure on the distal end of the affected digit(s). Toe amputation is another treatment option. Unfortunately, amputation of the digit can often precipitate the need for a more proximal amputation if the original surgical incision fails to heal.
The most common cause of preventable amputations in the neuropathic diabetic population is repetitive painless trauma leading to ulceration.1 Lesser-toe deformities—including hammertoes, claw-toes, and mallet-toes—are common findings in patients with peripheral neuropathy, with or without associated diabetes mellitus.2,3 Coughlin2 noted these deformities also can occur with any inflammatory arthropathies, such as gout or arthritis; repetitive trauma, such as ill-fitting shoes; or neuromuscular diseases, including lumbar disc disease or polio. Toe deformities that are initially flexible become rigid over time. This rigidity leads to increased pressures and skin shear over the distal digits and bony prominences. McGuire4 has written that joint stiffness caused by rigid deformities decreases the digit’s ability to absorb excess pressure.
Lesser-toe deformities can be precursors to the development of callus or ulceration on the distal aspect of the affected digits. Cavanaugh and Bus5 noted that claw-toe deformities are one of the most common causes of ulceration in neuropathic patients. Peripheral vascular disease also contributes to the risk of ulcer formation, and is present in 90% of patients with diabetes who undergo major amputations.6
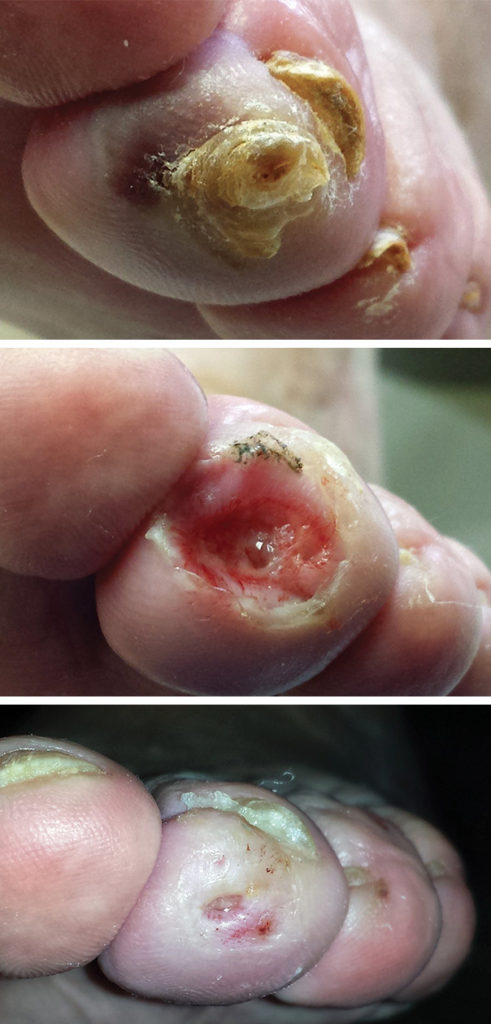
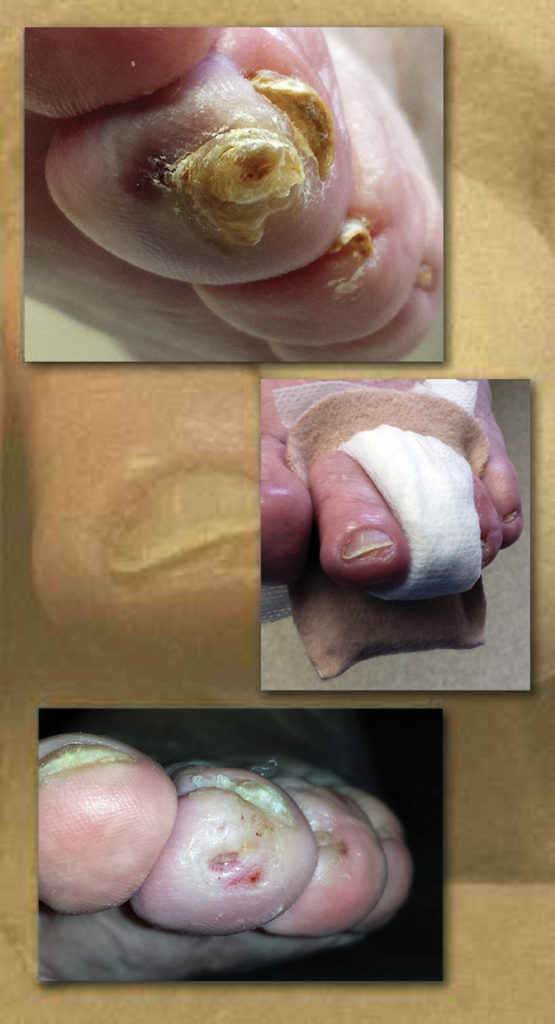
Figure 1. Photos show an example of hemorrhagic callus with underlying ulcer (top), the same digit after debridement of the callus (center), and after 12 days of crest pad use (bottom). Reprinted with permission from reference 17.
Chronic repetitive stress on the distal end of the toe, especially in neuropathic patients, leads to callus formation. A callus is an area of thickened hyperkeratotic skin cells that are compacted by pressure or friction.7 If the pressure continues, hemorrhage within the callus layers will become evident. Boulton8 described this presentation as a preulcerative lesion that needs aggressive management to avoid ulcer development. Simple callus removal through debridement may reduce pressures up to 30%, but, without intervention to relieve the pressure, the callus will return and can lead to limb-threatening problems.4,5
Treatment
When treating any wound, the principles of wound management, as outlined by Doughty,9 should be used to guide decision making. First, the underlying cause of the wound needs to be determined. Reduction or elimination of causative factors is one of the basic tenets of wound care.9,10 Secondly, systemic support should be provided. This includes adequate nutrition and fluids, appropriate oxygenation, and control of systemic variables such as blood glucose levels. Finally, appropriate topical therapy should be applied.
The first goal of topical therapy is to remove necrotic tissue. This can occur through sharp debridement or the use of dressings, such as enzymatic debriding agents. Of note, stable eschars in patients with arterial insufficiency should not be debrided until circulation has been optimized. Neuropathic ulcers should be routinely debrided of devitalized tissue and surrounding callus at one- to four-week intervals.11
The second goal of topical therapy is the identification and elimination of infection. During wound assessment, a positive probe-to-bone test has a high positive predictive value for osteomyelitis.11,12 The chosen topical therapy has to fill any dead space in the wound to decrease the likelihood of abscess formation.
Another goal of topical therapy is selecting a dressing that will absorb exudate, protecting the periwound area, while maintaining a moist wound surface. Finally, the chosen therapy should provide thermal insulation and protect the healing wound.
Rothman’s model of causation13 describes two types of causes for the occurrence of a given disease or problem. Sufficient causes invariably produce a particular effect. Component causes work together to produce a given effect. Blocking the causal role of one component will therefore block the effect.13
Distal toe callus most often occurs with a triad of component causes—neuropathy, pressure, and deformity. Per the Rothman model of causation,13 removing pressure will prevent the development of callus. This aligns with the principle of wound management addressing identification and elimination of the underlying wound cause(s).
Reducing distal toe pressure can be accomplished through surgical intervention, often involving flexor tenotomy.14 Schade15 noted that flexor tenotomy can be employed as a treatment for current ulceration as well as for the prevention of future callus formation. Surgical repair options for fixed deformities include decompression of the affected joints, along with tendon repairs.2 Boffeli, Abben, and Hyllengren14 describe performing in-office distal toe Symes amputations to excise distal lesser toe ulcers; this procedure removes the distal phalanx rather than the entire foot as is done with a conventional Symes amputation.
In-office distal toe Symes amputation offloads the tip of the toe, prevents ulcer recurrence, removes infected bone, and is most effective in treating affected digits that have rigid deformities, excessive length, and associated nail pathology.14 Unfortunately, many patients are at high risk for complications related to any surgical intervention, and require more conservative approaches.
Offloading the distal toe also can be accomplished through the use of a crest pad. Crest pads are commercially available in several styles. The first is constructed entirely of silicone, and is held in place by a silicone ring around a toe. A second style is a foam crest pad, which is secured with an adjustable elastic band that wraps around a toe. Caution must be used to avoid producing an ischemic toe or a pressure ulcer from the band. Patients with neuropathy are particularly at risk.
Huppin16 has described adding a crest pad directly to an orthotic insert; a temporary crest pad of adhesive felt is used to assess comfort prior to making it a permanent addition to the insert. Incorporating the crest pad into the insert assures that it is always being utilized; however, the patient has to be using both the prescribed shoes and inserts. Moving the insert with the molded crest pad into another pair of shoes could result in pressure over the dorsal aspect of the toes if the toe box is not of sufficient depth.
A crest pad made of rolled gauze covered in moleskin offers an alternative approach that minimizes the risks associated with tight bands or rings in at-risk patients. This design allows the affected toes to slide through an opening in the moleskin and rest on top of the rolled gauze pad. Over the course of several days, the pad will mold to the plantar surface to accommodate any deformities more comfortably.
This author and colleagues conducted a pre–post intervention retrospective chart review of the use of moleskin and gauze crest pads.17 The purpose of the study was to examine the use of crest pads in the treatment of toe callus, hemorrhagic callus, and ulceration in individuals with lesser toe deformities. All crest pads were made by the primary researcher at the time of the patient’s visit. A retrospective chart review was performed for patients seen between August 1, 2011 and December 31, 2014 who were treated with a gauze and moleskin crest pad. Callus and ulcer characteristics were compared pre- and postintervention.
Twenty-eight patients were identified as receiving a crest pad as part of their treatment, which consisted of nail or callus debridement or both as part of routine foot care. Of these, three patients were treated with a crest pad as a preventive measure and were thus excluded. Two were excluded based on the lack of a follow-up visit, and one patient was excluded due to early identification of osteomyelitis. The total sample size for the study was 22 patients, evenly divided between men and women. Two patients were aged between 50 and 59 years, five were aged between 60 and 69 years, eight were aged between 70 and 79 years, and seven were 80 years or older.17
Patients were divided into callus, hemorrhagic callus, and ulcer groups. At up to four follow-up visits, patients were recorded as either improved/resolved or unchanged/worsened. New crest pads were made for each patient at follow-up visits. The first callus follow-up group (at a mean of 45 days) had 20 resolved/improved patients and one unchanged/worsened patient, which represented a statistically significant improvement from baseline (p < .001).17 The second callus follow-up group (at a mean of 97.4 days) had 13 patients in the resolved/improved group and one in the unchanged/worsened group; this also represented a statistically significant improvement from baseline (p = .0002).17 The 21 patients in the third follow-up group (at a mean of 112 days) and the 11 patients in the fourth follow-up group (at a mean of 236 days) were all deemed resolved/improved. Patients returned for follow-up to receive routine nail care even after healing of the ulcer or resolution of the callus. This allowed us to document the maintenance of healed ulceration or lack of callus.17
Patients reported the moleskin crest pads were comfortable, especially after several days of use, which allowed the pads to mold to the shape of the toes. There were no reported adverse effects from the use of the pads, such as transfer ulcers or skin reactions. No patients developed dorsal toe ulcers, as the crest pad fits into the space under the toes. Discussion of proper footwear is standard during routine foot care visits, including an emphasis on a roomy toe box in shoes.
Discussion
Treatment of lesser toe callus and ulceration consists of eliminating infection, debriding callus, and offloading pressure. Patients with osteomyelitis will often require amputation of at least the distal end of the affected digit. Optimization of arterial circulation with angioplasty, stenting, or bypass may be required for healing for some patients. Offloading pressure from the distal end of the digit is essential in all cases if healing is to occur. This can be accomplished through the use of offloading devices such as crest pads.
While our study17 did not address prevention of callus or ulceration through the use of crest pads, it is worth noting that, in those patients having multiple follow-ups for foot care, none developed a recurrent ulcer on the distal toes once the crest pad was applied.
Commercially available silicone crest pads may be a good offloading option for patients, providing that patients are educated in proper use of the device. Crest pads can also be incorporated into an orthotic insert. Moleskin and rolled gauze crest pads may also be a good alternative, and can be custom-made by providers during foot care visits. A video demonstrating how to make a moleskin crest pad can be viewed at http://youtu.be/AMguRDlbd98.
Monica Melo, DNP, RN, ACNS-BC, CWOCN, CFCN, is a clinical nurse specialist at LVPG Vascular Surgery in Allentown, PA, treating patients with vascular wounds and performing preventive foot and nail care services.
- King LB. Impact of a preventive program on amputation rates in the diabetic population. J Wound Ostomy Continence Nurs 2008 35(5):479-482.
- Coughlin MJ. Lesser toe abnormalities. J Bone Joint Surg Am 2002;84(8):1446-1469.
- Shuman CJ, Beiser IH, Thompson J. Biomechanical impact on the etiology and treatment of neuropathic ulcerations. In: Sidawy AN, ed. Diabetic Foot: Lower Extremity Arterial Disease And Limb Salvage. Philadelphia, PA: Lippincott Williams & Wilkins; 2006: 19-27.
- McGuire J. Transitioning from open wound to final footwear: Offloading the diabetic foot. Podiatry Today 2012;25(9).
- Cavanagh PR, Bus SA. Off-loading the diabetic foot for ulcer prevention and healing. J Vasc Surg 2010;52(3 Suppl):37S-43S.
- Alavi A, Sibbald RG, Mayer D, et al. Diabetic foot ulcers: Part I. Pathophysiology and prevention. J Am Acad Derm 2014;70(1):1-20.
- Beuscher TL. Foot and nail care. In: Bryant RA, Nix DP, eds. Acute and Chronic Wounds: Current Management Concepts. 3rd ed. St. Louis, MO: Mosby/Elsevier; 2007: 337-360.
- Boulton AJM. Pressure and the diabetic foot: Clinical science and offloading techniques. Am J Surg 2004;187(5A):17S-24S.
- Doughty DB. Principles of wound healing and wound management. In: Bryant RA, ed. Acute and Chronic Wounds. St. Louis, MO: Mosby; 1992:31-68.
- Rolstad BS, Ovington LG. Principles of wound management. In: Bryant RA, Nix DP, eds. Acute and Chronic Wounds: Current management concepts. 3rd ed. St. Louis, MO: Mosby/Elsevier; 2007: 391-426.
- Hingorani A, LaMuraglia GM, Henke P, et al. The management of diabetic foot: A clinical practice guideline by the Society of Vascular Surgery in collaboration with the American Podiatric Medical Association and the Society for Vascular Medicine. J Vasc Surg 2016;63(Suppl 2):3S-21S.
- Morales Lozano R, Beneit Montesinos JV, Gonzalez Fernandez ML, et al. Validating the probe-to-bone test and other tests for diagnosing chronic osteomyelitis in the diabetic foot. Diabetes Care 2010;33(10)2140-2145.
- Rothman KJ. Causes. Am J Epidemiol 1976;104(6):587-592.
- Boffeli TJ, Abben KW, Hyllengren SB. In-office distal Symes lesser toe amputation: A safe, reliable, and cost-effective treatment of diabetes-related tip of toe ulcers complicated by osteomyelitis. J Foot Ankle Surg 2014;53(6):720-726.
- Schade V. Percutaneous flexor tenotomy: A viable alternative for distal digital ulceration? Podiatry Today 2015;28(5).
- Huppin L. Adding a crest pad to custom orthoses. Podiatry Today website. http://www.podiatrytoday.com/blogged/adding-crest-pad-custom-orthoses/. Published June 4, 2014. Accessed June 1, 2016.
- Melo M, Bernecker T, McCullough J, et al. A pilot study investigating the use of crest pads for treatment of toe callus and ulceration. J Vasc Nurs 2015;33(4):157-163.










Customized footwear, custom accommodative inserts, and rigid rocker soles. Are a great conservative treatment…. There are also custom silicone putty….toe crests/digital orthorics.
Properly fitted & fitting shoes are a good first effort as well. Most patients with toe deformities have a toe box that is too narrow & too short. The glass slipper fitting in Cinderella is a great example. Getting the patient to understand is a major issue. If they listen and acquire new shoes changes for the better will soon occur.
Very good & informative article.
A toe crest pad can be used for conservative therapy. Can be very effective.
I wrote my dissertation on how to prevent these from happening. In aviation if you put weight in the front the plane nose dives. It’s the same with feet. Forward weight, forward pressure. That dressing protects the skin but does not shift the weight/ pressure. That is done by securing the heel into the heel of the shoe (tongue pad/shoe lacing). This technique prevents slippage and grippage. That toe is gripping the shoe (hard). Postural stability and balance are a problem in our society, and most people are sliding in their shoes. Just look at the toe prints on the inserts.
A percutaneous flexor tenotony solves the problem as long as there is enough circulation to heal.
Thank you Miss Monica for this incredible work.
So, can you give me access to this vidéo :
http://youtu.be/AMguRDlbd98 (how to make a moleskin Crest pad).
My mail: ko***************@***il.com
Thanks