 Varus thrust is a characteristic of dynamic alignment that has been shown to be predictive of medial tibiofemoral structural progression. Treatments aimed at minimizing varus thrust may reduce structural progression and symptoms related to knee osteoarthritis.
Varus thrust is a characteristic of dynamic alignment that has been shown to be predictive of medial tibiofemoral structural progression. Treatments aimed at minimizing varus thrust may reduce structural progression and symptoms related to knee osteoarthritis.
By Grace Hsiao-Wei Lo, MD, MSc
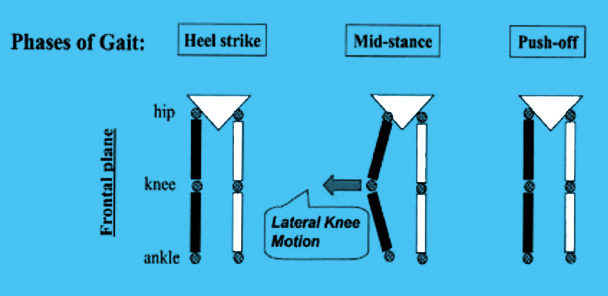
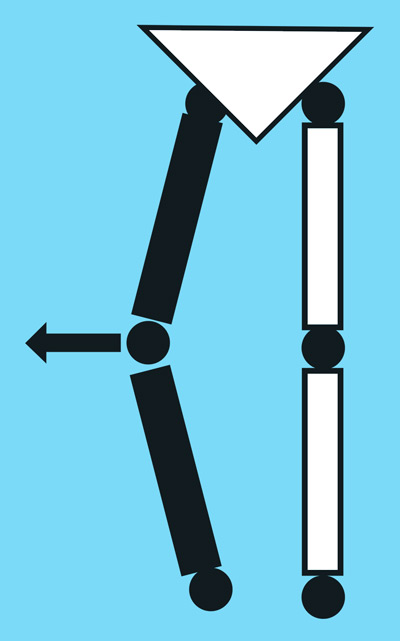
Varus thrust is the visualized dynamic bowing out of the knee laterally while the limb is weightbearing (stance) during ambulation, with the return to a less varus alignment during nonweightbearing (swing).1 Varus thrust can be defined dichotomously as being present or absent1-3 and, therefore, a trained individual can measure it in the clinic without need for a sophisticated gait laboratory. If there is an interest in quantifying the measurement, varus thrust can be assessed in a gait lab, where it is defined as the difference in the hip-knee-ankle angle between heel strike and the first varus peak.4
Varus thrust and loading
Biomechanical alignment influences the distribution of body-weight forces between the medial and lateral tibiofemoral compartments in the knee.5,6 Load distribution in individuals with varus malalignment is weighted toward the medial compartment; in those with valgus malalignment this distribution is weighted toward the lateral compartment. Varus thrust occurs during the stance phase of ambulation, when the knee sustains forces three to five times that of a person’s body weight.7 Varus thrust is the presence of dynamic worsening of varus alignment during stance phase and, therefore, is presumably associated with a high amount of medial compartment loading. This conclusion is supported by the finding that varus thrust is associated with greater external adduction moment, a reflection of dynamic medial compartment loading within a knee.8,9 The external adduction moment is a measurement of the torque (tendency of a force to rotate an object about an axis) that adducts the knee during the stance phase of gait, which can only be measured in sophisticated gait laboratories.

Drawings representing the stance phase of gait for the right leg. The lateral knee mo- tion represents varus thrust, the abrupt first apprearance of varus alignment (bowleggedness), or the abrupt worsening of existing varus alignment in the weightbearing limb, with return to less varus alignment after push-off. (Reprinted with permission from reference 1.)
Chang et al demonstrated that varus thrust and the external adduction moment are related when they found knees with a visible varus thrust had a higher external adduction moment compared with knees without varus thrust (3.63 + .66% body weight x height vs 2.6 + .81% body weight x height).1 They postulated that a visible varus thrust may represent a knee ineffectively counteracting the external adduction moment and resulting in an unstable joint.
Determinants of varus thrust
Chang et al also conducted a study of individuals with or at risk for knee osteoarthritis (OA) and identified risk factors for varus thrust, including male gender, white race (vs African American), and greater knee extensor strength.3
Chang et al posited that the greater prevalence of varus thrust seen in whites may provide an explanation for their higher prevalence of medial compartment knee OA.10 Though it has been observed by both Chang et al and Lo et al that men are at least twice as likely to have varus thrust compared with women, most studies do not show a greater prevalence of medial tibiofemoral compartment knee OA among male participants.1,2 One possible explanation for this is that there may be an unmeasured risk factor for medial compartment OA in women without varus thrust. An alternate explanation is that, in men, varus thrust alone is not sufficient to cause medial compartment OA. Men with varus thrust may require additional risk factors to be at increased risk for medial compartment knee OA.
Dynamic varus thrust is related to static varus alignment. Lo et al2 and Chang et al1 similarly found that, in populations with known symptomatic radiographic knee OA (defined as having at least one osteophyte in the knee on plain radiography and symptoms in the same knee), 80% of those with varus thrust had static varus malalignment. This is not surprising since varus thrust is the dynamic worsening of varus alignment in the stance phase of walking. However, among those without evidence of varus thrust, 33% had static varus alignment.2 Dynamic varus thrust and static varus alignment, while similar, do not represent the exact same construct.
Varus thrust is probably related to gait speed. The external adduction moment is related to gait speed, in that those who walk faster have a greater external adduction moment.11,12 Because the external adduction moment and varus thrust are associated, it is also likely that those who walk faster will be more likely to have varus thrust.
Medial cartilage damage
Chang et al evaluated the relationship between varus thrust and articular cartilage damage in knee OA.1 They studied a cohort of patients with known radiographic knee OA (n = 222), excluding those knees with advanced medial compartment knee OA. The cohort included 401 knees: 169 (42%) had varus static alignment, 199 (50%) had valgus alignment, and 33 (8%) had neutral alignment. Of the entire group, 67 (17%) had varus thrust at baseline. In total, 76 knees (19%) showed evidence of medial tibiofemoral OA progression over an 18-month period. Of the 334 knees without varus thrust, 49 (15%) had medial OA progression, while 27 of 67 (40%) of those with varus thrust had medial OA progression. The presence of varus thrust conferred an odds ratio of 3.96 (95% confidence interval [CI]: 2.11- 7.42) for medial knee OA progression. Thus, varus thrust is a potent risk factor for medial OA progression.
When adjusting for baseline static alignment, an established risk factor for medial OA progression,5 the odds ratio for varus thrust substantially decreased to 1.76 (95% CI .87-3.56) confirming that much of the effect of varus thrust in the development of medial OA progression is mediated by the presence of varus static alignment. A potential explanation for these findings is that Chang’s previously mentioned theory may be correct. A visible varus thrust occurs in a knee that ineffectively counteracts the knee adduction moment, resulting in an unstable knee exposed to high medial compartment loading, which then leads to medial OA progression.1 Kuroyanagi et al demonstrated similar findings in people with medial compartment knee OA, where increasing Kellgren-Lawrence grade (a radiographic measure of OA severity) was associated with increasing amount of varus thrust and a higher external adduction moment.4
Associations with knee pain
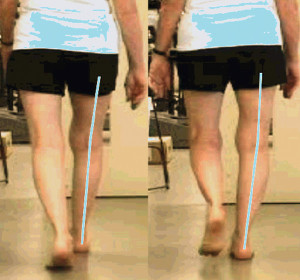
Visual representation of the observed varus thrust from two sequential video frames (initial contact on the left, early stance on the right.) Note the lateral displacement of the right knee during early stance as evidenced by increased tibial varus and interknee displacement. (Reprinted with permission from reference 11.)
Lo et al recently reported that varus thrust is associated with knee pain.2 In this 2012 study of patients with known symptomatic radiographic knee OA, those with varus thrust had a significantly higher total WOMAC (Western Ontario and McMaster Universities Arthritis Index) pain score than those without varus thrust (6.3 vs 3.9, p = .007). However, after adjustment for age, sex, height, weight, and walking speed, the difference was no longer significant (5.7 vs 4.2, p = .09).
Lessening of the association between varus thrust and knee pain with this adjustment is not surprising given that external adduction moments are associated with walking speed;11 therefore, adjusting for walking speed may have amounted to adjusting for a risk factor of varus thrust. For example, if a person were to have pain (outcome) due to the presence of varus thrust (predictor) that developed because he or she used a faster gait speed (risk factor for varus thrust), walking slower may reduce the varus thrust and therefore reduce pain (Figure 3).
This proposed conceptual framework is consistent with findings reported in a study by Thorp et al that included participants with varying degrees of medial tibiofemoral knee OA.13 They found those with greater knee OA severity had a slower gait speeds than those without knee OA. Consider, for example, a man who developed medial compartment knee OA due to repeated exposure to varus thrust. Once knee OA has developed, that knee will be more painful than when OA was not present, as it is well-established that those who have greater radiographic knee OA severity have more knee pain.14 Because the presence of varus thrust is a source of their knee pain, the man will walk with a slower gait to reduce his knee pain. Therefore, he will walk slower to reduce his exposure to varus thrust, the very risk factor that predisposed him to developing medial knee OA in the first place.
In the study by Lo et al, pain on walking and standing upright were the types of pain associated most strongly with varus thrust, such that individuals with varus thrust had a greater than four times proportional odds for pain with these two activities compared to those without varus thrust. There was a possible small association of pain with static varus alignment, but the point estimates were much smaller than those for varus thrust. The unadjusted total WOMAC pain scores in those with varus alignment compared with those without were 5 and 4.2, respectively (p = .36).
These findings support the possibility that varus thrust may be a source of knee pain in those with knee OA. Confirmation of this hypothesis would require a randomized controlled trial of an effective treatment for varus thrust in people with both varus thrust and symptomatic medial tibiofemoral knee OA. Ideally, we would find those who received effective treatment of varus thrust would also have resolution or at least reduction of their knee pain.
Clinical utility of varus thrust
Measuring varus thrust, in time, may become an important clinical tool. It is simple to assess in a clinical setting and is associated with pain and structural progression of medial tibiofemoral knee OA. In addition, clinicians can draw on a number of potential treatments that specifically target this finding. For example, a study by Ogata et al demonstrated that use of a lateral wedge insole reduces varus thrust.15
Researchers have also shown that lateral wedged insoles reduce peak knee adduction moment.16 Although this could have provided a rationale for use of a lateral wedge in the treatment of symptomatic knee OA, three randomized controlled trials of this intervention did not confirm its efficacy for reducing pain or structural progression in knee OA.17-19 A limitation to these findings is that participants were not screened for the presence of varus thrust, though they were screened for medial tibiofemoral knee OA, which should have selected out those who had increased medial compartment loading.
Although questions remain regarding treatment of knee OA with a lateral wedge insole, other interventions may be more effective for reducing varus thrust and potentially reducing structural progression and pain in patients with knee OA. Gait retraining, such as a toe-out gait or a medial thrust gait (knee medialization during the stance phase), have in cross-sectional studies been associated with lower external adduction moments,20,21 and may be effective treatments for varus thrust. It is unclear, however, how well people will accept gait retraining as an intervention. Another potential intervention is encouraging slower gait speeds, which could potentially improve symptoms and structural progression in knee OA.11,12 Not everyone who slows their gait has the same degree of reduction in their external adduction moment, however.23 Further investigation is needed to identify whether those with varus thrust are more or less likely to have reduction of the external adduction moment with a slower gait speed.
It has also been shown that those who walk barefoot or with a cane also have a lower external adduction moment.24 There is no definitive evidence that use of these interventions treats varus thrust, pain, or progression of medial knee OA, and, from a practical perspective, it may be difficult to convince people to walk barefooted or carry a cane on a regular basis when their knee pain is not severe.
Conceptually, medial compartment unloader knee bracing in a population with known varus thrust may be effective in reducing varus thrust.22 High tibial osteotomies could also potentially reduce varus thrust,25 but this may be too invasive a procedure to be widely accepted, particularly in those with mild knee OA. Systematic evaluation of treatments that reduce varus thrust in randomized controlled trials of populations preselected for the presence of varus thrust are needed.
Conclusions
Varus thrust is a measurement of dynamic alignment that potentially represents knee instability resulting from ineffective counteracting of an increased knee adduction moment, a measurement of medial compartment loading. Dynamic varus thrust is highly associated with varus static alignment, but it does represent a different construct. Factors associated with varus thrust include male gender, white race and, probably, faster gait speeds. Varus thrust has been shown to be predictive of medial tibiofemoral structural progression and is associated with symptoms in knee OA.
Treatments aimed at minimizing varus thrust hold the promise of reducing structural progression and symptoms related to knee OA. Randomized controlled trials of effective treatments of varus thrust in knee OA are warranted.
Grace Hsiao-Wei Lo, MD, MSc, is a practicing rheumatologist and an osteoarthritis clinical researcher at the Michael E. DeBakey VA Medical Center and Baylor College of Medicine in Houston, TX.
Disclosure: This work was supported in part by the Houston VA HSR&D Center of Excellence (HFP90-020). Dr. Grace Lo is currently funded on a mentored award by NIH/NIAMS (grant 1K23AR062127).
1. Chang A, Hayes K, Dunlop D, et al. Thrust during ambulation and the progression of knee osteoarthritis. Arthritis Rheum 2004;50(12):3897-9303.
2. Lo GH, Harvey WF, McAlindon TE. Associations of varus thrust and alignment with pain in knee osteoarthritis. Arthritis Rheum 2012;64(7):2252-2259.
3. Chang A, Hochberg M, Song J, et al. Frequency of varus and valgus thrust and factors associated with thrust presence in persons with or at higher risk for knee osteoarthritis. Arthritis Rheum 2010;62(5):1403-1411.
4. Kuroyanagi Y, Nagura T, Kiriyama Y, et al. A quantitative assessment of varus thrust in patients with medial knee osteoarthritis. Knee 2012;19(2):130-134.
5. Sharma L, Song J, Felson DT, et al. The role of knee alignment in disease progression and functional decline in knee osteoarthritis. JAMA 2001;286(2):188-195.
6. Wada M, Maezawa Y, Baba H, et al. Relationships among bone mineral densities, static alignment and dynamic load in patients with medial compartment knee osteoarthritis. Rheumatology 2001;40(5):499-505.
7. Hoshino A, Wallace WA. Impact-absorbing properties of the human knee. J Bone Joint Surg Br 1987;69(5):807-811.
8. Hurwitz DE, Ryals AB, Case JP, et al. The knee adduction moment during gait in subjects with knee osteoarthritis is more closely correlated with static alignment than radiographic disease severity, toe out angle and pain. J Orthop Res 2002;20(1):101-107.
9. Hurwitz DE, Sumner DR, Andriacchi TP, Sugar DA. Dynamic knee loads during gait predict proximal tibial bone distribution. J Biomech 1998;31(5):423-430.
10. Chang A, Hochberg M, Song J, et al. Frequency of varus and valgus thrust and factors associated with thrust presence in persons with or at higher risk of developing knee osteoarthritis. Arthritis Rheum 2010;62(5):1403-1411.
11. Robbins SM, Maly MR. The effect of gait speed on the knee adduction moment depends on waveform summary measures. Gait Posture 2009;30(4):543-546.
12. Hunt MA, Bennell KL. Predicting dynamic knee joint load with clinical measures in people with medial knee osteoarthritis. Knee 2011;18(4):231-234.
13. Thorp LE, Sumner DR, Block JA, et al. Knee joint loading differs in individuals with mild compared with moderate medial knee osteoarthritis. Arthritis Rheum 2006;54(12):3842-3849.
14. Neogi T, Felson D, Niu J, et al. Association between radiographic features of knee osteoarthritis and pain: results from two cohort studies. BMJ 2009;339:b2844.
15. Ogata K, Yasunaga M, Nomiyama H. The effect of wedged insoles on the thrust of osteoarthritic knees. Int Orthop 1997;21(5):308-312.
16. Shelburne KB, Torry MR, Steadman JR, Pandy MG. Effects of foot orthoses and valgus bracing on the knee adduction moment and medial joint load during gait. Clin Biomech 2008;23(6):814-821.
17. Pham T, Maillefert JF, Hudry C, et al. Laterally elevated wedged insoles in the treatment of medial knee osteoarthritis. A two-year prospective randomized controlled study. Osteoarthritis Cartilage 2004;12(1):46-55.
18. Baker K, Goggins J, Xie H, et al. A randomized crossover trial of a wedged insole for treatment of knee osteoarthritis. Arthritis Rheum 2007;56(4):1198-203.
19. Bennell KL, Bowles KA, Payne C, et al. Lateral wedge insoles for medial knee osteoarthritis: 12 month randomised controlled trial. BMJ 2011;342:d2912.
20. Chang A, Hurwitz D, Dunlop D, et al. The relationship between toe-out angle during gait and progression of medial tibiofemoral osteoarthritis. Ann Rheum Dis 2007;66(10):1271-1275.
21. Fregly BJ, D’Lima DD, Colwell CW Jr. Effective gait patterns for offloading the medial compartment of the knee. J Orthop Res 2009;27(8):1016-1021.
22. Hunt MA, Schache AG, Hinman RS, Crossley KM. Varus thrust in medial knee osteoarthritis: quantification and effects of different gait-related interventions using a single case study. Arthritis Care Res 2011;63(2):293-297.
23. Mündermann A, Dyrby CO, Hurwitz DE, et al. Potential strategies to reduce medial compartment loading in patients with knee osteoarthritis of varying severity: reduced walking speed. Arthritis Rheum 2004;50(4):1172-1178.
24. Kemp G, Crossley KM, Wrigley TV, et al. Reducing joint loading in medial knee osteoarthritis: shoes and canes. Arthritis Rheum 2008;59(5):609-614.
25. Prodromos CC, Andriacchi TP, Galante JO. A relationship between gait and clinical changes following high tibial osteotomy. J Bone Joint Surg Am 1985;67(8):1188-1194.