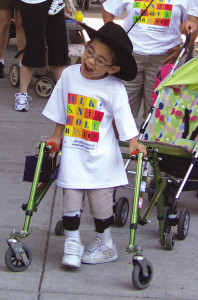
Strength training can help address weakness in children with cerebral palsy, but it can’t restore lost motor signals. Orthoses can help balance muscle activity while providing stability, but in some patients can hinder normal motion. Ultimately, the ideal synergy between the two approaches may be different for each patient.
by Cary Groner
For years, researchers and physical therapists seeking to optimize physical function and quality of life for children with cerebral palsy (CP) have debated the value of strengthening exercises. Until the early 2000s, many believed that muscle strengthening increased spasticity, but that theory has been debunked.1,2 Disagreement remains whether exercise can help compensate for the neurological deficits associated with CP, however, or if there are other benefits that should be evaluated. Additional controversy surrounds the appropriate role of orthotic treatment.
In 2004, the American Physical Therapy Association (APTA) convened a summit to investigate some of these issues, and to encourage research and the open exchange of ideas. The resulting article, published in Physical Therapy in 2007,3 noted that inadequate physical fitness affected both the function and health of children with CP, and that lack of activity may contribute to secondary conditions including fatigue and chronic pain. The association called for more research into both muscle strength and cardiorespiratory fitness, particularly as they might affect later health and QOL.
The lead author of that article, Eileen Fowler, PT, PhD, has actively pursued such research, and has published a new paper that helps clarify some of the issues.4 Fowler, a professor at UCLA / Orthopedics Hospital Center for Cerebral Palsy in Los Angeles, studied the effects of stationary cycling on muscle strength, locomotor endurance, preferred walking speed, and gross motor function (using the Gross Motor Function Measure [GMFM]) in a randomized controlled trial of 62 children with spastic diplegic cerebral palsy. She and her colleagues reported significant improvements in endurance, GMFM scores, and some measures of strength in the cycling group, but no significant differences between cycling and control groups (Fowler attributes improvements in the control group to learning or accommodation to the test environment).
“Children with spastic diplegic cerebral palsy commonly have periventricular white matter damage, which affects the tracts for voluntary motor activity,” Fowler said. “One reason we chose cycling is that children with severe damage in this area are constrained to move in patterns. If you ask them to move only their ankle, they can’t; but if you ask them to move their whole leg, they can. We felt that all of the children would be able to perform the cycling exercise program.”
Complexity
Other studies have come to different conclusions, and one reason is that CP is a multifarious and complex disease.5,6 It is caused by injuries or abnormalities of the brain that occur before birth or in infancy, and may include hypoxia, hemorrhage, infection, and head injury. It is more common in premature infants, and although it varies drastically in severity, the brain injury itself is not progressive. There are several categories of CP; patients typically have impairments of the motor system, including spasticity, low muscle strength, joint contractures, and decreased selective motor control.
The most common type, spastic CP, comprises roughly 70% of cases; it results from damage to descending motor tracts, including the corticospinal tracts (also called pyramidal tracts) and may be hemiplegic (primarily affecting one side); diplegic (mainly affecting the lower limbs); or quadriplegic (affecting all four limbs). Spastic CP typically involves loss of selective muscle control, dependence on immature patterns (e.g., short step length) during ambulation, abnormal muscle tone, an imbalance between muscle agonists and antagonists across joints, weakness, and deficient equilibrium. Less common forms of CP include extrapyramidal types including ataxic (resulting from damage to the cerebellum) and dyskinetic (resulting from damage to the basal ganglia).7
Conflicting studies
Recent research has shown that low muscle strength and deficient selective motor control, rather than spasticity, may cause the greatest deficits in motor function.8,9 This would suggest that strength training should address at least some of CP’s adverse effects, but causal relationships have been difficult to establish.
For example, a 2009 British study of medial and lateral gastrocnemius muscle strengthening showed that muscle volume increased after five and 10 weeks of training and at three-month follow up, but that there was no significant change in measured function.10 Similarly, a January study from the Netherlands concluded that 12 weeks of training improved muscle strength but did not affect mobility; that study found that the strength increases disappeared within six weeks after training ceased.11 And a 2009 meta-analysis from Australia reported—in language uncharacteristically strong for the field—that strengthening interventions are “neither effective nor worthwhile.”12
Other research suggests efficacy, however. A 2009 study in the United States found that five weeks of task-oriented strength training improved mobility function, assessed using the GMFM and the timed “up and go” test.13 Another study found that a six-week strengthening program was associated with significant improvements in trunk and lower extremity muscle strength, gait velocity, cadence, step length, energy expenditure, and distance traveled in a three-minute walk test.14 In one pilot study, researchers found that after 12 weeks of training, increases in ankle strength led to improved function, gait speed, and quality of life in children with spastic diplegia.15 And a 2007 study from the Netherlands, in contrast to the one cited earlier from that country, found that eight months of strength training improved both aerobic and anaerobic capacity, agility, and athletic competence in children and adolescents with CP, as well as improving subjects’ overall QOL.16 Moreover, a Dutch literature review from 2008, with the same lead author, concluded cautiously that “children with CP may benefit from improved exercise programs that focus on lower-extremity muscle strength, cardiovascular fitness, or a combination.”17
Selective strengthening
How to account for such disparities? Experts in the field acknowledge that the studies done so far have suffered from outcomes measures so disparate that they are hard to compare, and sometimes from a lack of methodological rigor. But even studies by highly regarded researchers can produce equivocal results.
For example, recently researchers from the National Institutes of Health studied whether strength training could diminish the crouched, internally rotated gait common to children with spastic diplegic CP. They found that although strength increased significantly in some muscle groups, kinematic and functional outcomes were inconsistent.18
The study’s lead author, Diane Damiano, PT, PhD, director of biomechanics at the NIH Clinical Center, told LER, “You need to know what muscles to strengthen, because strengthening the wrong muscles can lead to increased tightness and worse function.”
She also noted, however, that because the decline in motor function with age occurs sooner and more sharply in those with CP than in unaffected individuals, maintaining strength may help.
“Strength training and increased physical activity should be a lifestyle choice,” Damiano said. “People who have trouble moving, and therefore do not move as much as they should, need to do more than you and I to maintain the status quo. Short term programs are only a start; positive outcomes accumulate over time.”
Eileen Fowler, the UCLA researcher, acknowledged that randomized trials haven’t produced consistent results.
“There are challenges in terms of research design and statistics,” she said. “The GMFM is an important outcome measurement for children with cerebral palsy, and I think most exercise studies do show some improvement. In terms of gait, sometimes there is improvement, sometimes there isn’t. We didn’t find an improvement in gait with cycling, but did find that locomotor endurance and GMFM scores improved in the group that cycled.”
Fowler, like Damiano, believes that conclusions about efficacy should be based on broader health considerations in addition to CP-related impairments.
“If you improve your overall cardiorespiratory fitness and your muscle strength, that is important even if you don’t improve functionally,” she said. “Exercise has general health benefits, such as preventing cancer and dementia, so I disagree with statements that these approaches are not worthwhile. Exercise is important for everyone.”
Strength and orthotic management
Robert Lin, CPO, FAAOP, agrees that exercise may be helpful as long as practitioners and their patients recognize its limitations.
“Cerebral palsy is a perinatal insult to the central nervous system that affects the signal to specific muscle motor groups,” said Lin, who is chief orthotist for Hanger Orthopedic Group at Connecticut Children’s Medical Center and associate clinical instructor at the University of Connecticut. “Unfortunately, all the strength training in the world isn’t going to improve the signal.”
Lin is realistic without being a hard-liner, however.
“There’s anecdotal evidence that strength training is good for things like joint range of motion and strengthening peripheral muscles so a patient can substitute,” he said, noting that someone with hemiplegic CP and a dysfunctional anterior tibialis could train the extensor hallucis to help pick up the foot. Lin also sees promise in devices that provide electrical stimulation to the pretibial musculature to help the wearer pick up the foot.
“The problem with kids who have CP is that there’s an imbalance between agonist and antagonist muscle groups,” he explained. “When you’re walking, strength training is not necessarily going to make you more stable, because a lot of that has to do with tone and balance. It’s a complex neuromotor network that doing reps with weights may not improve.”
For Lin and others in his field, bracing is an important solution.
“When we brace kids with cerebral palsy, we are trying to biomechanically equalize the playing field. You block the overactive agonist or antagonist muscle so the weaker one can get a little more up to par,” he said
For example, in a child whose gastrocnemius muscles are much stronger than the dorsiflexors, Lin would use an ankle-foot orthosis (AFO) that blocks plantar flexion but allows free dorsiflexion.
“It stretches the gastroc and biomechanically improves the gait,” he said. “Orthotic management can be very effective in balancing the muscles. It can improve stability and suppress some tone by reducing specific movements strategically—but it doesn’t do anything relative to strength.”
Lin also draws a distinction between the potential benefits of exercise in different types of CP.
“With a patient who has spasticity, you can try to reeducate and remodel a bit,” he said. “But an athetoid patient doesn’t have any patterned movement, and walking is all pattern.”
Mark K. Taylor, CPO, FAAOP, senior prosthetist and orthotist at the University of Michigan Orthopedic and Prosthetic Center, also uses orthoses to balance CP patients’ musculature and improve gait.
“For those with an internal rotational deformity, I want to use an orthosis to help support the kids and get them out of a crouch-type gait,” he said. “That’s why range of motion is important—so we can hold that range orthotically, not let the therapy go to waste and be overpowered by tone, so they go into contracture again.”
Overbracing concerns
Eileen Fowler appreciates the role of bracing in her patients, as long as it’s done carefully.
“If someone has significant impairment in motor control, it’s important to stabilize the ankles,” she said. “Putting the foot flat on the floor provides a more stable gait pattern. But in children who have relatively good motor control, orthotic devices can get in the way. If a child is able to run and jump, and you put them in an orthosis, sometimes they have more trouble. Not every child with cerebral palsy should get braces.”
Taylor agrees.
“We never want to overbrace a child,” he said. “In my experience, a teamwork approach with physical therapists has been the key to success with these kids. We throw ideas back and forth and come up with plans for each patient. It might involve nighttime stretching or wearing a certain brace for half a day.”
Tom DiBello, CO, president of Dynamic Orthotics and Prosthetics in Houston, sees such integrated approaches as essential to effective treatment of children with CP.
“The emphasis in managing children with neuromuscular problems from an orthotic standpoint should always be improving bony alignment, but you have to be careful how you achieve it,” he said. “There’s an unfortunate tradeoff when, in the course of stabilizing a joint, you lose some of its normal motion. You never want to overly encumber these children with bracing.”
For DiBello, the optimal approach would entail maintaining good alignment through the process of strengthening.
“We’re always interested in seeing these kids become stronger,” he said.
Cary Groner is a freelance writer based in Northern California.
References
- Fowler EG, Ho TW, Nwigwe AI, Dorey FJ. The effect of quadriceps femoris muscle strengthening exercises on spasticity in children with cerebral palsy. Phys Ther 2001;81(6):1215–1223.
- Dodd KJ, Taylor NF, Graham HK. A randomized clinical trial of strength training in young people with cerebral palsy. Dev Med Child Neurol 2003;45(10):652–657.
- Fowler EG, Kolobe TH, Damiano DL, et al. Promotion of physical fitness and prevention of secondary conditions for children with cerebral palsy: section on pediatrics research summit proceedings. Phys Ther 2007;87(11):1–16.
- Fowler EG, Knutson LM, Demuth SK, et al. Pediatric endurance and limb strengthening (PEDALS) for children with cerebral palsy using stationery cycling: a randomized controlled trial. Phys Ther 2010;90(3):367–381.
- Cerebral palsy. MedlinePlus. Available at: www.nlm.nih.gov/medlineplus/print/ency/article/000716.htm
- Scholtes VA, Dallmeijer AJ, Rameckers EA, et al. Lower limb strength training in children with cerebral palsy—a randomized controlled trial protocol for functional strength training based on progressive resistance exercise principles. BMC Pediatr 2008;Oct 8:41–60.
- Lin RS, Gage JR. The neurological control system for normal gait. JPO 1990;2(1):1–11.
- Ostensjo S, Carlberg EB, Vollestad NK. Motor impairments in young children with cerebral palsy: relationship to gross motor function and everyday activities. Dev Med Child Neurol 2004;46(9):580–589.
- Ross SA, Engsberg JR. Relationships between spasticity, strength, gait, and the GMFM-66 in persons with spastic diplegia cerebral palsy. Arch Phys Med Rehabil 2007;88(9):1114–1120.
- McNee AE, Gough M, Morrissey MC, Shortland AP. Increases in muscle volume after plantarflexor strength training in children with spastic cerebral palsy. Dev Med Child Neurol 2009;51(6):429–435.
- Scholtes VA, Becher JG, Comuth A, et al. Effectiveness of functional progressive resistance exercise strength training on muscle strength and mobility in children with cerebral palsy: a randomized controlled trial. Dev Med Child Neurol 2010; Jan 28. [epub ahead of print]
- Scianni A, Butler JM, Ada L, Teixeira-Salmela LF. Muscle strengthening is not effective in children and adolescents with cerebral palsy: a systematic review. Aus J Physiother 2009;55(2):81–87.
- Salem Y, Godwin E. Effects of task-oriented training on mobility function in children with cerebral palsy. NeuroRehabilitation 2009;24(4):307–313.
- Eagleton M, Iams A, McDowell J, et al. The effects of strength training on gait in adolescents with cerebral palsy. Pediatr Phys Ther 2004;16(1):22–30.
- Engsberg JR, Ross SA, Collins DR. Increasing ankle strength to improve gait and function in children with cerebral palsy: a pilot study. Pediatr Phys Ther 2006;18(4):266–275.
- Verschuren O, Ketelaar M, Gorter JW, et al. Exercise training program in children and adolescents with cerebral palsy: a randomized controlled trial. Arch Pediatr Adolesc Med 2007;161(11):1075–1081.
- Verschuren O, Ketelaar M, Takken T, et al. Exercise programs for children with cerebral palsy: a systematic review of the literature. Am J Phys Med Rehabil 2008;87(5):404–417.
- Damiano DL, Arnold AS, Steele KM, Delp SL. Can strength training predictably improve gait kinematics? A pilot study on the effects of hip and knee extensor strengthening on lower-extremity alignment in cerebral palsy. Phys Ther 2010;90(2):269–279.