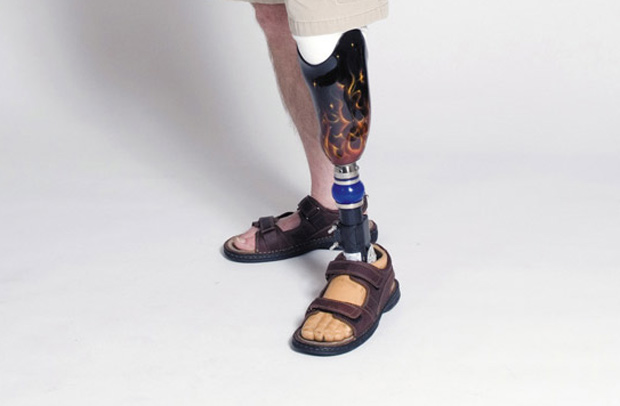
O&P devices are all-too-public indicators of an infirmity, and often limit clothing and footwear options—all of which contributes to poor self image. But a little empathy can keep self image issues from sabotaging patient compliance.
By Emily Delzell
Innovations in biomechanical technology and design combined with durable graphite and carbon fiber materials mean practitioners can offer patients more refined, lightweight, and aesthetically acceptable orthotic and prosthetic devices than ever before. Research and clinical experience, however, indicate that many patients only reluctantly accept and sometimes reject such devices.
The negative impact therapeutic devices have on self image is often the major barrier to patient satisfaction and compliance. Patients, who may already feel defined by a condition not of their choosing, often view the need for a medical device as yet another change in their identity dictated by their pathology.
Unlike many medical interventions, orthotic and prosthetic devices are observable, public indicators of a medical condition or injury. In addition, wearing these devices often requires altering or replacing clothing or footwear that would normally be chosen by the individual with items dictated by their clinical needs.
“What we wear reflects who we are or, at the very least, what we want to project of ourselves. That is why fashion is such a powerful and ever-changing industry. Practitioners who work with patients who need orthotic or prosthetic devices need to understand this to provide the best care,” said Janet Marshall, CPO, LPO, a pediatric specialist at Shriners Hospital for Children in Tampa, FL. “Today’s orthotic or prosthetic industry is constantly evolving to make products that are more effective, lighter, stronger, and cosmetically more appealing. But for every ‘best’ there is a ‘better.’”
Choice and voice
Providing optimal clinical care is a priority for practitioners, but for patients, even those with painful or disabling condition, self image often supersedes almost all other considerations.
Rheumatoid arthritis (RA) has significant effects on the feet, which are one of the first areas of the body to show visible damage from the disease. Studies of individuals with RA and their attitudes toward therapeutic footwear have found that such shoes often create negative social and emotional consequences for patients.
Although recent guidelines1 and research support the use of therapeutic footwear for reducing pain, improving mobility, and preserving function in RA, patients—particularly women—often express dissatisfaction with the intervention, said Anita Williams, PhD, FPodM, a senior lecturer at the Directorate of Prosthetics, Orthotics and Podiatry and Centre for Rehabilitation and Human Performance Research at the University of Salford, United Kingdom.
Williams, who has served as lead investigator for a series of studies examining therapeutic shoe use in people with RA and diabetes, finds that although such footwear can address patients’ clinical needs, reducing the negative impact on their self image—and subsequently improving compliance—often requires that shoes also meet some of their nonclinical needs.
“Most of the women in our studies of RA and therapeutic footwear2-4 characterize the shoes as a visible marker for disability that carries with it the stigma of being different from their peers,” she said. “Many expressed feelings of loss and sadness because they could no longer choose their own style of footwear. They feel people wonder why they’re wearing ‘ugly’ shoes and worry that others think the style is their choice.”
Many women also reported that the narrow range of footwear choices impacted clothing styles they could choose to wear, Williams noted.
“As a result, women often feel they can’t easily engage in some social activities, particularly more formal or celebratory occasions,” she said. “This contributes to their sense of social isolation, reduced self worth, dissatisfaction with their bodies, and depression—already a comorbidity of RA.
Williams’ studies and others suggest both a lack of choice and patients’ impressions that practitioners don’t understand the nature or significance of their concerns—what she termed a lack of “voice”—lead to dissatisfaction with the process, a poor self image, and lower wear rates, or “shoes in the cupboard.”
When a patient can voice opinions to practitioners about both the process and the corrective devices, he or she will feel more like an active participant and consequently experience less of a negative impact on their identity, Williams said.
“These discussions can create a sense of partnership with the practioner and increase patients’ perceptions of control in a positive way,” she said. “They feel better about the process and about themselves.”
But in Williams’ studies, practitioners could help give weight to that voice by making sure patients were actually being heard.
“Being understood—i.e., having practitioners acknowledge patients’ unique experience of their disease and listen to their concerns about the emotional consequences of the device on their self image and their lives—was one of the key aspects participants identified that would have improved their overall experience and potentially increased compliance,” she said.
Patients often fear an unpleasant experience when they fill a prescription for therapeutic shoes, said Dennis Janisse, CPed, president and CEO of National Pedorthic Services and clinical assistant professor in the department of physical medicine and rehabilitation at the Medical College of Wisconsin, both in Milwaukee.
“In a lot of people’s minds a corrective device is like a big billboard they’re carrying around that says, ‘Look at me. I’m different.’ That’s difficult enough, but unfortunately, a lot of patients don’t understand why they’re ‘forced’ to do this, they are just told they must,” Janisse said.
This lack of understanding can be exacerbated in patients with diabetic peripheral neuropathy, if their impaired sensation means that therapeutic footwear or other devices don’t have the appeal of relieving pain or discomfort.
“Compliance is often quite poor among people with diabetic neuropathy because they don’t have the feedback to know they’re suffering,” said David Levine, DPM, CPed, who has been practicing for 23 years, most recently in Frederick, MD.
One of Williams’ studies compared perceptions of therapeutic footwear in people with RA with those of individuals with diabetes.5
“There was a major difference between patients with RA and those with diabetes. Comfort was the priority for patients with RA, but the primary concern of those with diabetes was style,” she and colleagues wrote. “Not focusing on practical aspects of the footwear may in part be due to the fact that in diabetes normal foot structure is broadly maintained and more easily accommodated in retail footwear. Also, any failure in sensory function reduces a patient’s ability to sense poorly fitted shoes, and in fact, all shoes may feel relatively comfortable.”
Bryan West, DPM, who practices in Livonia, MI, recommended that practitioners spend time focusing on the patient’s state of mind as well as their physical condition.
“Practitioners need to evaluate the whole patient, body and mind. Some patients, such as those who have suffered stroke or have drop foot, are so pleased to walk normally with the assistance of an ankle-foot orthosis or other device that they simply don’t care what it looks like, or what shoe they have to wear to accommodate it,” he said. “Others may have a different personality or existing depression or social anxiety. A brace can magnify those issues so much that they quickly stop using it. Or if they do comply and use it without acknowledging or resolving its emotional impact, it can deepen their depression and have other detrimental effects on their mental health.”
Understanding a patient’s experience of their disease can help practitioners connect with the whole person, Janisse said.
“Specialization in medicine often means the focus is on a specific pathology or part of the body and the person can get lost,” he said. “We have to think about what people are going through. People with diabetes, for example, may be losing their sight or sexual function. They may have to test their blood glucose levels multiple times a day and modify their diet. We as practitioners get frustrated because we feel that what we’re offering is highly important. But it may not be the most important thing for patients, who often must make many other lifestyle concessions.”
Explaining why
Even if practitioners can’t do anything about the aesthetics of an O&P device, taking time to listen to patients’ concerns, educate them about therapeutic benefits, and learn what level of intervention they are ready to accept can improve wear rates and clinical outcomes.
Giving patients more control over the process can help build confidence and improve compliance, even if that means making some clinical compromises, Janisse said.
“For example, when I’m filling a prescription, it may call for five options. Patients may not be ready for that level of intervention. If they aren’t, I may suggest we take things in steps as long as it is not detrimental,” he said. “That could mean starting with an orthotic insert rather than a shoe. This isn’t an option for everyone, but having these kinds of discussions with patients makes them part of the process and can give them a feeling of responsibility for their clinical outcomes.”
Similar compromises may be warranted when it comes to bracing, West said.
“Prescribing a brace that is the textbook answer for a given condition does not always work in real life,” West said. “A brace that’s too heavy for an elderly patient, for example, may simply not get worn. I would rather offer a lighter alternative and have patients wear it than have a heavier device gather dust. Even if the lighter device cannot offer the same level of correction, patients still will shave a better clinical outcome because they’ll actually use the lighter device.”
Another key to improving compliance is making sure patients understand why a particular device has been prescribed and how it will positively affect their pain and function.
“Explaining why the brace is so important for the patient’s health can help,” West said. “If a patient fully understands why they need the device—the functional improvement it can provide or complications and progression it can prevent—they are much more likely to comply with its use.”
Janisse strongly agreed.
“To achieve good compliance and outcomes, patients have to understand what the device does and practitioners have to explain how it is going to enhance their life,” he said. “Practitioners need to be specific and say things like, ‘This will relieve pain or improve ambulation,’ or ‘This will heal the ulcer on your foot so you can avoid amputation in the future.’ As practitioners, we have to take the time to work with each patient and help them understand the true value of the prescribed device as well as the risks of not using it.”
Janisse noted that one of his patients, a woman with RA who initially resisted corrective shoes, ultimately embraced the intervention when the therapeutic benefits became apparent.
“She said that although the shoes made her feel less feminine, the subsequent reduction in pain and the belief that the shoes would help keep her ambulatory for years helped her overcome most of the negative impact on her emotional identity,” he said. “Helping patients identify more with the positive effects of devices can improve their self image. Instead of being the person in the orthopedic shoes, for example, they become the person who can take their grandchildren to the playground.”
Education is a crucial issue for patients with diabetes, Levine said.
“Lack of tactile sensation can allow them to believe they are not significantly damaging their feet by failing to wear prescribed footwear,” he said. “A simple visual illustration can help get this point across. I recently had a patient with very little feeling in his feet. He was bursting out of his shoes. I traced his foot and put the shoe on top of the tracing. The trouble he was having—but not feeling—became much clearer to him.”
Color and personalization: Not just for kids
Perhaps not surprisingly, one of the best ways to improve self image associated with an O&P device is to change the device’s appearance. But involving the patient in the process makes it about much more than just aesthetics.
“For children with physical challenges that require the use of orthotics or prosthetics, we need to empower them to have some control over decisions that impact their lives, even if it is a simple choice of the patterns and colors used in the devices,” Marshall said. “This decision provides the opportunity to make a statement of self-image, and gives confidence and better compliance at the same time.”
Marshall noted that at Shriners Hospital in Tampa, where she practices, a survey of pediatric patients found that those who had orthoses with patterns and colors had a more positive self image, better peer acceptance, and consequently, improved compliance compared with peers who wore white braces.
As many practitioners understand, however, the benefits of personalizing the prescribing and dispensing process—as well as the device—aren’t limited to children.
“I have a patient who expressed disgust with his prosthetic leg until he found a local artist to apply the pattern of his choice,” West said. “He chose an American flag for his prosthesis and his attitude completely changed; he became proud of it.”
Chris Gracey, MPT, CPed, who works with patients with lower extremity disorders in the rehabilitation medicine department at the National Institutes of Health (NIH), is a strong advocate of the use of personalization and color. In addition to his clinical and research activities at the NIH, he heads a small custom orthotic business, producing a line he calls “Art of the Sole.”
When dispensing or filling a prescription for therapeutic device, practitioners often stress practical aspects such as improvement in function, Gracey said, and noted, “Although aesthetic preferences may seem frivolous in comparison with a person’s medical needs, I believe the color, texture, and look of a device can have a great impact on whether a person actually wears that device. These factors can help the patient connect in a more emotionally positive way with both their pathology and the device needed to treat it.”
Gracey, who hand-colors his orthotics, also spends time learning about his patients, getting a sense of their personality.
“I recently worked with a patient who is a chef at local restaurant. Her favorite color is orange. ‘Hot’ colors have traditionally been avoided in orthotics and prosthetics because they suggest pain and inflammation. But I created a pair in a color I called “Empress Orange” with a shape that suggested lobster claws and she loved the result,” he said. “Incorporating elements of patients’ unique personality helps them better identify with their pathology. It brings out feelings of pleasure, confidence, and hope, and perhaps this is why I enjoy very high compliance and successful healing rates.”
Emily Delzell is a freelance writer based in Birmingham, AL.
References
1. National Collaborating Centre for Chronic Conditions. Rheumatoid arthritis: the management of rheumatoid arthritis in adults (Clinical guideline 79). London: National Institute for Health and Clinical Excellence (NICE); 2009.
2. Silvester RN, Williams AE, Dalbeth N, Rome K. Choosing shoes: a preliminary study into the challenges facing clinicians in assessing footwear for rheumatoid patients. J Foot Ankle Res 2010; 3:24.
3. Williams AE, Nester CJ, Ravey MI, et al. Women’s experiences of wearing therapeutic footwear in three European countries. J Foot Ankle Res 2010;3:23.
4. Williams AE, Nester CJ, Ravey MI. Rheumatoid arthritis patients’ experiences of wearing therapeutic footwear – a qualitative investigation. BMC Musculoskelet Disord 2007;8:104.
5. Williams AE, Nester CJ. Patient perceptions of stock footwear design features. Prosthet Orthot Int 2006;30(1):61-71.