 Not all patients with diabetes and not all ulcerated limbs are amenable to salvage. When salvage is not an option, amputation can help improve patient function, but a number of factors should be considered when deciding how much of the foot—if any—should be retained.
Not all patients with diabetes and not all ulcerated limbs are amenable to salvage. When salvage is not an option, amputation can help improve patient function, but a number of factors should be considered when deciding how much of the foot—if any—should be retained.
By Cary Groner
Diabetes patients and their physicians sometimes face life-altering decisions in the face of recurrent foot infections. The first choice is whether to continue efforts at limb salvage or to amputate; then, if they choose amputation, they must determine at what level to perform it.
A number of options are available, depending on the depth and severity of the infection: toe, metatarsal ray, transmetatarsal, Lisfranc (a tarsometatarsal disarticulation), Chopart (disarticulation through the talonavicular and calcaneocuboid joints), and more proximal partial-foot amputations including the Pirogoff and Boyd (in which some of the calcaneus may be preserved), and the Syme, in which the residual limb ends at the distal base of the tibia.1 More proximal amputations include transtibial below-knee and transfemoral above-knee approaches.
Different amputation levels offer different advantages and disadvantages, but the decision ultimately depends on individual clinical judgment and patient preference. The wound must heal, both to save the patient’s life and to prevent subsequent, higher amputations. Factors to be considered, then, include the patient’s vascular status, the presence and anatomical level of osteomyelitis, and, intraoperatively, the amount of bleeding in skin flaps.2 Some evidence suggests that sedentary patients may do better with limb salvage, whereas more active people may have better functional outcomes with early major amputation.3 But again, it depends on the patient and the type of activity.
“Deciding who needs an amputation and who doesn’t depends on a lot of factors,” said David Armstrong, DPM, MD, PhD, professor of surgery and director of the Southern Arizona Limb Salvage Alliance (SALSA) at the University of Arizona College of Medicine in Tucson.
For example, Armstrong cited the case of a patient who was recently admitted to the hospital with a high white blood cell count, fever and chills, a wound that probed to bone, and possible osteomyelitis. The man previously had a transmetatarsal amputation.

Figure 1. Examples of amputations at different levels. A. Partial second toe amputation. B. First ray resection. C. Fifth ray resection. D. Chopart hindfoot amputation. E. Syme amputation. (Photos courtesy of Michael Pinzur, MD.)
“He’s a relatively young man in his forties, and we’ve been working with him a long time,” Armstrong said. “He has bone involvement throughout his residual forefoot and midfoot, and the best surgery may be a below-knee amputation, so we can get him into a prosthetic and he can live his life. If he were my brother, that’s what I would recommend.”
Nevertheless, the patient has previously favored attempts at limb preservation, and Armstrong wasn’t sure which decision he (the patient) would make this time.
Terrible costs
Such decisions have critical implications. The incidence of vascular amputation at or near the transmetatarsal level is eight times higher in diabetes patients than in those without diabetes, and one in four amputees ends up with contralateral amputations or reamputation.4 Researchers at Kaiser Permanente Medical Center in Oakland, CA, reported that of 90 patients who underwent transmetatarsal amputation, 88 had postsurgical complications.5 Another study, from the San Antonio VA Hospital in Texas, delineated the terrible costs associated with the vascular disease that may lead to major lower-extremity amputations. Of 113 amputation patients (75% of whom had diabetes), only 65% were still alive at 10-month follow up, and 17% of those discharged with an intact contralateral limb later had that limb amputated.6 Another Texas study reported that cumulative reamputation rates in 277 diabetes patients reached 60.7% at five years.7
Researchers have bolstered the case for performing the most distal amputation possible in most cases, however, and clinicians generally agree with this recommendation. For example, a Swedish study published last year examined the outcomes of amputations through or distal to the ankle joint in diabetes patients and reported that 79% healed in surviving patients.8 A paper published in Diabetes Care in 2001 found that those with toe or midfoot amputations did not have significantly higher impairment scores than those in a control group, whereas those with transmetatarsal amputations did.9 Patients without underlying ischemia are significantly more likely to heal after transmetatarsal amputation.10
Amputations at any level have repercussions that may increase the risk of later, more proximal amputations, however—particularly if the initial amputation is made too distally in a misguided effort to save more of the foot than is feasible.11 Regional increases in plantar pressures due to biomechanical compensation after partial foot amputation elevate the risk of further tissue damage.12 One study reported that great toe amputation contributed to the development of deformities of the second and third toes and new ulcer formation in patients with diabetes.13
Of course, one reason for such findings is that amputation dramatically alters gait; loss of the metatarsophalangeal joints, for example, has a profound effect.14 Diabetes patients with transmetatarsal amputations can’t generate as much plantar flexor power at the ankle, so they rely more on “pulling” the leg forward using the hip flexors.15 Generally, the loss of the forefoot lever arm leads to a substantially reduced plantar weightbearing surface, loss of pronation and supination during gait, and an absence of active push off.16
Deciding when to cut
Clinicians still occasionally disagree about both principle and practice, but as David Armstrong’s example makes clear, the patient’s wishes sometimes trump clinical experience.
“One of the biggest factors is the patient’s willingness and ability to go through what is required to salvage this limb,” agreed Jeffrey Johnson, MD, associate professor of orthopedic surgery and chief of the Foot and Ankle Service at Barnes-Jewish Hospital at Washington University Medical Center in St. Louis, MO. “Many times it requires multiple procedures over many months, and at the end it’s hard to guarantee that they’ll be better than if we do an amputation. In some cases most of us would probably feel that a patient will function better with a well-done below-knee amputation.”
John Steinberg, DPM, an associate professor in the Department of Plastic Surgery at the Georgetown University School of Medicine in Washington, DC, concurred.
“We may wrongly assume that they’ve given their buy-in for seventeen procedures and lots of reconstruction, when really they would have rather just saved the pain and anguish,” he said.
When Steinberg spoke with LER, in fact, he had just seen a patient who begged him for an amputation; she’d had seven procedures from another physician who had worked hard to save her foot, but had left her in such pain that she couldn’t put it on the ground.
“Just because you can save anatomy,” Steinberg said, “that doesn’t mean it’s always a good idea.”
Michael Pinzur, MD, professor of orthopedic surgery and rehabilitation at Loyola University Medical Center in Maywood, IL, recently published a paper outlining a four-step approach to such decisions.17 First, will limb salvage outperform an amputation and prosthetic limb? Second, what is a realistic endpoint for either salvage or amputation? Third, what are the costs of limb salvage to the patient, not just financially but in terms of suffering and lost time? Fourth, what are the risks associated with treatment?
“Does it make sense to spend three to five months constructing a limb they can walk on when they have such bad vascular disease that they may be dead in a year or two?” Pinzur asked. “Should they spend half of their remaining life in rehab?”
Dane Wukich, MD, an associate professor of orthopedic surgery at the University of Pittsburgh School of Medicine, said several criteria help him decide when to abandon attempts at limb salvage. If an uncontrollable infection is putting the patient’s life at risk, if the patient has a deformity that’s not reconstructible, or if the surgeon can’t restore good circulation, then it’s time to amputate.
Choosing levels
Similarly, certain factors affect the decision about amputation level, according to Wukich. First is the patient’s level of function.
“If someone hopes to walk, you want to preserve as much of the lower extremity as you can,” he said. “A partial foot amputation is better than a below-knee amputation, which is better than an above-knee amputation. But if the foot infection is so bad that you can’t go through healthy tissue, you have to go above the ankle. Then, if the leg is involved, you go to the level of the knee or above. The basic principle is to remove all the infected tissue, and get to where you have good circulation.”
For Steinberg, similar considerations apply.
“First, what level will be functional for the patient?” he asked. “Do they want to be able to walk on it or just transfer their weight?”
Other issues that affect decisions about the type and extent of surgery include the patient’s overall health and ability to withstand anesthesia, the level at which there is adequate blood flow, the potential for successful rehabilitation, and the desired activity level afterward.
Some of these factors force decisions that may seem counterintuitive from the common perspective that distal is better, Steinberg said.
“We’ll be considering a foot amputation, but if it’s a young patient who wants to be a triathlete, they may be better off with a below-knee amputation, because they’ll never have the same function as with the propulsive gait offered by the new advanced prostheses.”
The general principle, according to Wukich, is: How far distal can you amputate and maintain function?
“If you’re going to take the toe off, that’s better than going higher,” he said. “If you can do a transmetatarsal, that’s good. Some hindfoot amputations, such as the Chopart, don’t do as well because of soft-tissue imbalance. Some people like a Syme because the patient can walk around at night without putting on a prosthesis. The key is to get to the healthiest tissue you can, but an active young person may do better with a well-done below-knee than a hindfoot amputation such as a Chopart.”
Jeffrey Johnson voiced similar concerns.
“Unless patients are really compliant with bracing, offloading, and careful washing of the foot, they don’t do as well with some amputations,” he said. “In those with peripheral neuropathy, I usually go from a transmetatarsal to a transtibial amputation. A Lisfranc eliminates some very important muscle attachments, so you have to compensate for that by reattaching the peroneal muscles; but that’s possible only if you have no infection on the lateral side of the foot. Even with a heel cord lengthening, the Lisfranc often results in equinus contracture.”
Johnson noted that a Chopart procedure results in even more muscles being detached—the posterior and anterior tibialis as well as the peroneals.
“That requires a fair amount of soft-tissue balancing as well, and bracing, and the ulcer recurrence rate is significant,” he said. “I think a person with a well-done below-knee amputation and a modern prosthetic device will usually function better than a braced Chopart-level amputee.”
Considerations
Michael Pinzur concurred.
“These are big operations, and anesthesias are poisons, so the more procedures you do, the more risks you take,” he said. “If you can do a higher-level amputation with a high chance of success, you don’t spend so much of the patient’s remaining life doing medical treatment.”
Pinzur recently had an experience similar to that reported by John Steinberg.
“The patient is a golfer with diabetic vascular disease who’d had one below-knee amputation,” Pinzur said. “He was having trouble with the other leg, and he came to me and said, ‘I spent a year futzing around with the first leg, so do the amputation and get me back on the golf course, because that’s what I want to do.’ Now, if you look at the vascular surgery literature, where they measure success based on graft patency and limb salvage, he is a failure. But if we’d salvaged the limb, and he had ischemic pain walking twenty steps, would that have been a success? We fit him with a prosthesis and got him back on the golf course. Is that a failure?”
Pinzur has written that when performing an amputation, the surgeon should strive to create three things: optimal residual limb length without bony prominences, reasonable function in the joint proximal to the amputation level to enhance prosthetic function, and a durable soft-tissue envelope.18 When deciding the level at which to amputate, he considers several factors.19
“You have to look at the limb and see what’s alive and what’s dead—what’s warm, what has hair growth, what tissue has normal consistency,” he told LER. “You measure blood flow to establish the threshold of adequate arterial blood to heal the wound. You have to check the patient’s nutritional status, because if they’re malnourished, their tissues won’t heal, so if someone’s albumin is below three, we don’t do amputations in the foot and ankle.”
Although some clinicians dislike Syme amputations, Pinzur defends this approach.20
“They don’t like them because they don’t know how to do them,” he said. “You have to do it technically correctly, and people don’t.”
In 2003, Pinzur and several colleagues published a paper in the Journal of Bone and Joint Surgery reporting results in 97 diabetes patients who underwent the procedure; 85% achieved wound healing (the paper also described the correct surgical procedure.)21
The paper concluded that, compared to a population of transtibial amputees who served as historical controls, patients managed with a Syme ankle disarticulation appeared to remain able to walk better and survive longer.
Great expectations
Pinzur, like other clinicians interviewed for this article, acknowledged that his patients’ expectations play an important role in determining amputation level.
“Yesterday I saw an Afghanistan veteran who is a high-AK amputee, and she is a triathlete,” he said. “Those are the people who need high-tech prostheses. But how many diabetic patients who receive amputations are going to run a marathon? They just need to walk across the room. You can fit a Syme’s amputee with a high-tech prosthesis, and even though it isn’t the greatest cosmetically, he’ll be much more functional than with a below-knee amputation. In fact, a Syme’s amputee with a low-tech prosthesis is going to be more functional than a below-knee amputee with a high-tech one, because of the difference in energy costs.”20,22
Pinzur also argued that the usual practice of doing the most distal possible below-knee amputation may be misguided because it fails to allow for the design characteristics of prostheses.
“The optimal fit for a BK amputee is with the leg flexed seven to ten degrees, but if you do the amputation right above the ankle and flex the knee ten degrees, you have to make a socket that will accommodate that leg sticking out the back,” he said. “Otherwise, you have to straighten out the knee, and the patient doesn’t function as well. I want to do a below-knee amputation at a level that will optimize prosthetic fit.”
John Angelico, CP, OTR, who works with Pinzur on many of his patients, is a managing partner at Scheck & Siress, the largest independent prosthetic foot facility in Chicago. Angelico said that BK amputees with longer residual limbs can be accommodated in prostheses and that there can be benefits to this approach in terms of energy cost, but that some object to the cosmetic repercussions.
“It’s more difficult for people who are concerned about the appearance of the prosthesis to make that look good,” he said.
Angelico agrees with Pinzur about the benefits of Syme amputations, and not just because of the lower energy costs associated with a longer limb.
“I’m a true believer in disarticulations, because the patients have a better ability to take weight on the bottom of the amputation,” he explained. He also supported the position that there are quality prostheses available for active Syme amputees.
“There are products for these patients, including carbon graphite dynamic-response feet,” he said. “People in the prosthetics industry don’t use them that often—but there are competitively active Syme’s amputees.”
Team amputee

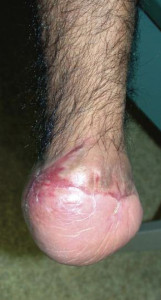
Figure 2. A construction worker in his mid-40s presented with life-threatening sepsis related to diabetic foot wounds. Because it was this patient's first such problem, limb salvage was performed. (Photos courtesy of the Southern Arizona Limb Salvage Alliance (SALSA).)
Foot care teams have been shown to reduce the incidence of major amputations by more than half, from 16 to 6.8 per 100,000, according to Swedish researchers. Moreover, the fraction of amputations with a final level at or below the ankle more than doubled, from 0.23 to 0.49, over eight years and then stabilized.23
Once an amputation is being considered by a patient, other amputees may play an important role in the patient’s decision-making process, according to several clinicians.
“It becomes a functional decision for the patient, so we try to connect them with others who’ve had proximal amputations,” said John Steinberg. “Members of our amputee support group play a big role by talking to them about what to expect and different types of recovery based on amputation level. Patients say that if they’d known how well they’d do with their prosthetic leg, they would have had an amputation years ago.”

Figure 3. A deputy sheriff in his mid-40s presented with life-threatening sepsis related to diabetic foot wounds. Unlike the construction worker described in Figure 2, this patient had a long history of such problems as well as foot deformities secondary to Charcot neuroarthropathy, and worked at a desk job. Those factors contributed to the decision to perform a below-knee amputation. (Photos courtesy of the Southern Arizona Limb Salvage Alliance (SALSA).)
“Amputees have a camaraderie, because no one else really knows what it’s like to go through this,” added Jeffrey Johnson.
He pointed out that prosthetists may play a key role, as well.
“They can see what a prosthesis looks like, talk to the prosthetist about what they’ll be able to do, and ask questions about anything—how they’ll shower, or swim, for example. The patients think these things are huge hurdles, so it can relieve their anxiety to find out that they don’t have to be,” Johnson said.
Johnson said that recent social forces have changed patients’ acceptance of amputation, as well.
“As more and more veterans are coming back from the Iraq and Afghanistan wars with amputations due to IEDs [improvised explosive devices], the media is picking up that these kids can still do a lot, play golf or basketball. So people are more aware of what amputation means, and it’s less of a stigma,” he said.
Back to the future
The decision to amputate—and where to do the procedure—always comes back to the patient’s wishes and vision of the future.
“When I was just starting out in practice, I always thought my job was to heal every wound on every body,” said David Armstrong. “I have to remind myself that our goal is to get people back to living their lives in the best manner, as soon as possible. Most of the time, that means healing the patient as distally as possible, but not always. Some people do better with an amputation [than limb salvage], and it’s not a precise formula. We can quantify it to some degree, but after all the quantification comes the qualitative interaction with the patient, which includes their beliefs and philosophy as well as those the clinician. It’s complicated.”
As an example, Armstrong and his colleague, Magdiel Trinidad-Hernandez, MD, assistant professor of vascular and endovascular surgery at the University of Arizona College of Medicine, recently reported what they call “A Tale of Two Soles.”24
Two male patients, both in their mid-40s, came in with life-threatening sepsis related to diabetic foot wounds (figures 2 and 3). For Armstrong’s patient, a construction worker, it was the first time this had happened. For Trinidad-Hernandez’s patient, a deputy sheriff with a desk job, it was another in a long history of such problems, and Charcot neuroarthropathy had already destroyed the architecture of his foot.
Though the men’s cases were similar, because of such factors their treatment took different paths. Armstrong salvaged his patient’s limb, whereas Trinidad performed a below-knee amputation on his patient. The disparate decisions made it possible for both men to return to work.
“My patient was all set up to have this problem again,” Trinidad-Hernandez said. “He’d been dealing with this chronic wound for years, which made him a better candidate for amputation, so he could move on with his life.”
“As you mature in your practice, you see these things as part of a spectrum, and view it through the prism of your experience,” said Armstrong. “I have a clinic full of patients for whom I believe distal treatment is better, but I will always offer them the option to get healed immediately.”
When Armstrong was still a resident, one of his early mentors, Irv Kanat, MD, once asked him, “How do you treat people?” Armstrong replied that he’d treat them the way he himself wanted to be treated.
“Wrong!” said Kanat. “You treat them the way they want to be treated.”
“At first, I thought he was just being obstinate,” Armstrong said. “But boy, do I understand it now.”
Cary Groner is a freelance writer in the San Francisco Bay Area.
1. Levy L, Hetherington V, Bakotic B, eds. Principles and practice of podiatric medicine. 2nd ed. Brooklandville, MD: Data Trace; 2006.
2. Davis BL, Kuznicki J, Praveen SS, Sferra JJ. Lower-extremity amputations in patients with diabetes: pre-and post-surgical decisions related to successful rehabilitation. Diabetes Metab Res Rev 2004;20(Suppl 1):S45-S50.
3. Attinger CE, Brown BJ. Amputation and ambulation and diabetic patients: function is the goal. Diabetes Metab Res Rev 2012;28(Suppl 1):S93-S96.
4. Johannesson A, Larsson GU, Ramstrand N, et al. Incidence of lower-limb amputation and the diabetic and nondiabetic general population: a 10-year population-based cohort study of initial unilateral and contralateral amputations and reamputations. Diabetes Care 2009;32(2):275-280.
5. Pollard J, Hamilton GA, Rush SM, Ford LA. Mortality and morbidity after transmetatarsal amputation: retrospective review of 101 cases. J Foot Ankle Surg 2006;45(2):91-97.
6. Toursarkissian B, Shireman PK, Harrison A, et al. Major lower-extremity amputation: contemporary experience in a single Veterans Affairs institution. Am Surg 2002;68(7):606-610.
7. Izumi Y, Satterfield K, Lee S, Harkless LB. Risk of reamputation in diabetic patients stratified by limb and level of amputation: a 10-year observation. Diabetes Care 2006;29(3):566-570.
8. Svensson H, Apelqvist J, Larsson J, et al. Minor amputation in patients with diabetes mellitus and severe foot ulcers achieves good outcomes. J Wound Care 2011;20(6):261-262.
9. Peters EJ, Childs MR, Wunderlich RP, et al. Functional status of persons with diabetes-related lower-extremity amputations. Diabetes Care 2001;24(10):1799-1804.
10. Hosch J, Quiroga C, Bosma J, et al. Outcomes of transmetatarsal amputations in patients with diabetes mellitus. J Foot Ankle Surg 1997;36(6):430-434.
11. Skoutas D, Papanas N, Georgiadis GS, et al. Risk factors for ipsilateral reamputation in patients with diabetic foot lesions. Int J Low Extrem Wounds 2009;8(2):69-74.
12. Armstrong DG, Lavery LA. Plantar pressures are higher in diabetic patients following partial foot amputation. Ostomy Wound Manage 1998;44(3):30-32.
13. Quebedeaux TL, Lavery LA, Lavery DC. The development of foot deformities and ulcers after great toe amputation in diabetes. Diabetes Care 1996;19(2):165-167.
14. Marks RM, Long JT, Exten EL. Gait abnormality following amputation in diabetic patients. Foot Ankle Clin 2010;15(3):501-507.
15. Mueller MJ, Salsich GB, Bastian AJ. Differences in the gait characteristics of people with diabetes and transmetatarsal amputation compared with age-matched controls. Gait Posture 1998;7(3):200-206.
16. Michael J. Partial foot and similar amputations: focus on hindfoot and midfoot amputations. O&P Business News 2003; accessed online at: http://www.oandpbusinessnews.com/view.aspx?rid=57810[3/14/2012
17. Pinzur MS. Outcomes-oriented amputation surgery. Plast Reconstr Surg 2011;127(Suppl 1):241S-247S.
18. Pinzur MS, Gottschalk FA, Pinto MA, et al. Controversies in lower-extremity amputation. J Bone Joint Surg Am 2007;89(5):1118-1127.
19. Pinzur MS. Amputation level selection in the diabetic foot. Clin Orthop Relat Res 1993;(296):68-70.
20. Pinzur MS. Syme’s ankle disarticulation. Foot Ankle Clin 2010;15(3):487-494.
21. Pinzur MS, Stuck RM, Sage R, et al. Syme ankle disarticulation in patients with diabetes. J Bone Joint Surg Am 2003;85(9):1667-1672.
22. Pinzur MS, Gold J, Schwartz D, Gross N. Energy demands for walking in dysvascular amputees as related to the level of amputation. Orthopedics 1992;15(9):1033-1037.
23. Larsson J, Eneroth M, Apelqvist J, Stenstrom A. Sustained reduction in major amputations in diabetic patients: 628 amputations in 461 patients in a defined population over a 20-year period. Acta Orthop 2008;79(5):665-673.
24. Trinidad-Hernandez M. “When is a BK-A A-OK?” Presented at the Diabetic Foot Global Conference 2012, Los Angeles, March 2012.








