
iStockphoto.com #1195684094
Communication, education, and empathy—combined with a solid knowledge base of the disease—are key components of successful management of these damaging, even life-threatening, lesions.
By Angela Kelley, PA-C
Diabetic foot ulcers (DFUs) can be concerning to patients and providers for multiple reasons. From the patient’s perspective, DFUs can be uncomfortable, even painful, and a source of embarrassment from a cosmetic perspective; depending on the patient’s level of health literacy, there can be a lack of understanding of the entire disease process of diabetes mellitus (DM), making recurrence of DFUs a significant possibility.
A patient’s comfort level, or level of trust in the provider, can also affect communication regarding DFUs. Patients might have larger health concerns and not fully understand the sequelae of DFUs, or any of the potential risks of developing them. As providers, not only do we assess patients for the most obvious concerns about pain, we must also demonstrate a high index of suspicion for the risk of cellulitis, osteomyelitis, sepsis, amputation, and more, leading us to a prognosis for the overall stability of DM.1
Bridging the gap between patient and provider concerns during a 15-minute office visit is often difficult, as regards providing empathy and efficiency. Communication and patient education are therefore highly important aspects of diagnosing and treating DM, in an effort to prevent its significant complications. Often, patients are unaware that a lesion is present until the provider identifies it for them as many patients with DM have complete or partial loss of sensation. Seeking a way to not embarrass the patient in pointing out these lesions, while educating them and letting them know that we are there for them, is an important component of care as well.
Required: Extensive Knowledge of the Disease
Periodic Evaluation of the Patient With Diabetes4
- Perform an annual comprehensive foot exam, looking for the risk factors that could lead to ulceration and amputation:
- skin inspection
- evaluation for foot deformities
- vascular assessment of pulses in feet and legs
- neurological assessment, using 10-g monofilament and at least 1 of the following:
- temperature
- vibration
- pinprick
- Perform a foot exam at every visit for patients who have loss of sensation, prior amputation, or prior ulceration
- Elicit any history of amputation, ulceration, angioplasty, Charcot foot, retinopathy, smoking, or renal disease
- Elicit current symptoms of neuropathy (numbness, burning, pain) or peripheral arterial disease (claudication, leg fatigue)
- Refer for determination of the ankle-brachial index when a patient presents with claudication or when pedal pulses are absent or decreased
- Involve other disciplines in a case of Charcot foot, prior ulceration, or prior amputation
- Involve footcare specialists when a patient presents with a notable abnormality, such as peripheral artery disease, loss of sensation in the lower extremities, or structural deformity, or is a smoker
- Educate patients with diabetes on preventive foot self-care
- Recommend specialized footwear in patients with diabetes who have a severe case of neuropathy or foot deformity or who have had an amputation
Diabetes mellitus is a chronic condition that has the potential to affect many body systems—endocrine, cardiovascular, integumentary, neurological, ophthalmologic, genitourinary, musculoskeletal.1 When DM is the underlying cause of a foot ulcer, the risk of morbidity and mortality is significantly increased.2 Communication with patients first encompasses a deeper understanding of DFUs so that we can educate them about the signs, symptoms, disease process, treatment, and prevention of these concerning wounds, as well as their prevalence, mortality data, and cost burden.
The cause of a DFU can be multifactorial: Poor glycemic control, peripheral vascular disease, and neuropathy are all risk factors for these concerning lower extremity wounds—a result of reduced host defenses, reduced blood flow to the feet, decreased sensation of temperature and pain, and fissures in the skin from decreased autonomic supply, which can lead to a greater risk of introduction of organisms into open wounds.2 According to a report by Armstrong and colleagues,3 the annual incidence of DFU, the most commonly recognized complication of DM, is 6.0% of Medicare patients with DM.
Complications of a diabetic foot, such as amputation, and the monetary cost of those complications, are also proving to be a burden. Mortality after DM-related amputation is > 70% at the 5-year mark for all diabetic patients; the risk of death for a patient with a DFU at 10 years is twice as high as it is for a diabetic patient who does not have a foot ulcer.3 In the United States, the cost burden for patients with a DFU is as much as one-third the overall cost of the care of DM—as high as $176 billion annually.3
The range of clinical presentations of a DFU is wide; communicating the potential signs and symptoms is therefore of high importance in patient education. Patients with DM should be advised to monitor for loss of sensation; dermatologic changes, including trauma; and signs and symptoms of inflammation, including swelling, warmth, erythema, purulent secretion, tenderness, and induration.2 Patients should also report delayed healing and any hair loss, claudication, or leg fatigue.1 Foot self-exam and awareness of temperature change in the lower extremities should be taught to patients.1 According to Standards of Medical Care in Diabetes 2019, providers should examine patients as described in “Periodic evaluation of the patient with diabetes.”4
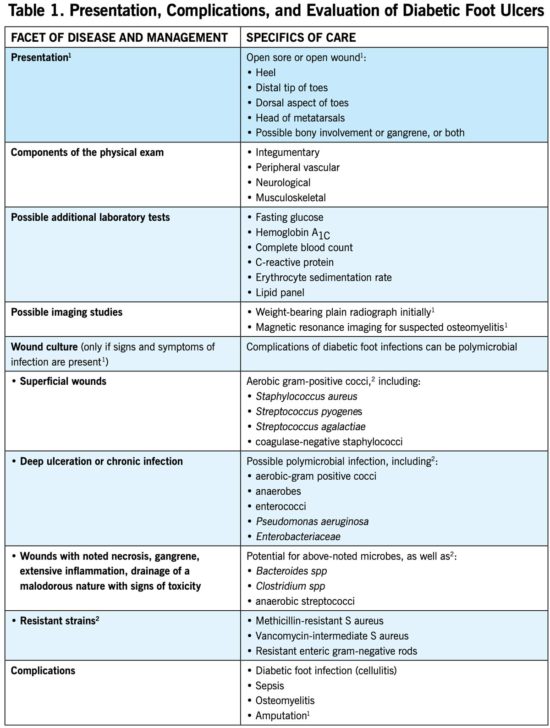
The risk of DFU is, as mentioned, associated with poor glycemic control, peripheral vascular disease, and neuropathy; however, the provider should also assess the duration of the patient’s diagnosis and search for signs of foot trauma or other orthopedic abnormalities that might result in areas of elevated pressure in the foot.1 These problems can lead to severe complications, which presses the issue of proper communication. Presentation and complications of DFUs, the physical exam, and potential tests are provided in Table 1.
 Treatment + Communication = Optimal Management
Treatment + Communication = Optimal Management
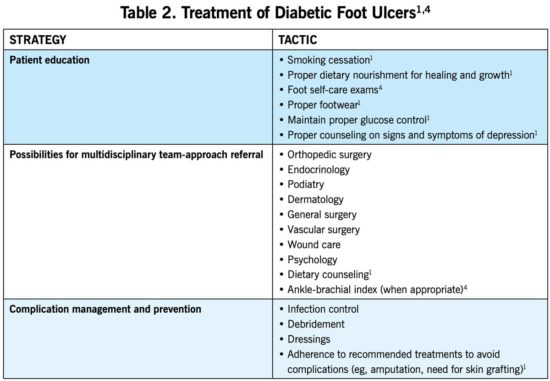
Treatment of DFUs can also be multifactorial. Table 2 outlines approaches to treatment based on severity of ulceration. Educating patients about smoking cessation, proper footwear and footcare, proper diet, and the value of a multidisciplinary approach to management is imperative. Communicating with patients about adherence to recommended treatment regimens is also a focal point because preventing severe complications is crucial.
Although we want to give patients the best education about their disease and DFUs, we are limited by barriers to communication. Communication between patients and clinicians is linked to outcomes, adherence, and satisfaction. If a clinician is unable to recognize and adapt for sociocultural differences between themselves and their patients, quality of care can be affected.
A survey5 of patients performed to assess communication found that 19% had at least 1 of the following concerns with their provider:
- difficulty understanding the provider
- the impression that the provider doesn’t listen to them
- feeling that they can’t ask the provider questions during office visits.
If providers were to take a patient-centered view on communication, they would find that patients want to be respected, to have open communication about their illness through education, to receive such education in a time-appropriate manner, and to feel that their provider is able to alleviate their fears while treating their physical discomfort. Providers would also find that patients want to know that their provider is able to coordinate care, involve their family, and help with transition and continuity of care from one location to another without significant interruption or inaccessibility of services.6
There are many strategies to improve communication between patients and providers (Table 3). Having an extensive knowledge base of the subject matter, as discussed above, and participating in continuing learning are important steps in developing trust and rapport with patients. Being courteous, professional, punctual, and supportive are desirable traits in a provider; so are showing empathy, minimizing distractions, and knowing the limits of one’s ability—that is, when it’s time to refer to other specialties.
Once a provider has established an open path to communication with a diabetic patient, the education process should be multifaceted. The provider should strive to give advice based on clinical evidence, question patients to determine the depth of their medical knowledge, assist patients in informed decision-making, order appropriate and cost-effective treatments and tests if necessary, and perform motivational interviewing to elicit appropriate behavioral changes.7 These aspects of education should be performed by using the interpersonal and professional skills mentioned above. Sending information to the patient’s portal in the electronic health record—for further self-education and to present topics for discussion in detail at later visits—can also be helpful.
 Maintaining Care After the Clinic Visit
Maintaining Care After the Clinic Visit
Follow-up care is a key part of communication. It has been determined that, once patients leave the clinic, they forget 40% to 80% of instructions related to their treatment regimen.8 Findings show that, not only are patients interested in more frequent communication from their provider, they also are more likely to be proactive in their health regimen if they have more education about their disease.8 It has been noted that, in the United States, < 2% of patients who have DM participate in, to a full extent, one of American Diabetes Association’s recommended care regimens.8 If we are able to communicate more frequently and more effectively, we are likely to improve adherence, which can have a positive impact on the care of the DM population.8
Methods of communication outside the clinic include the electronic health records, patient portals, texting, emails, and smartphone apps, reminders, and alerts. As reported in Standards of Medical Care in Diabetes 2019, all patients who have DM should participate in self-management education, with special attention to receiving education on 4 occasions4:
- at the time of diagnosis
- annually after diagnosis
- any time a disease-complicating factor arises
- during transition of care.
In addition to using technology, an individual or group setting is acceptable for continued patient education.4
Self-monitoring of the blood glucose level4 and self-efficacy management have been discussed in the literature as methods for patient adherence to treatment plans, including diabetic foot care.9 There are several methods of self-management, including the Diabetes Management Self-Efficacy Scale (DMSES) and patient-reported outcome measures (PROMs), such as10:
- Foot Self-Care Behavior Scale (FCBS)
- Foot Health Status Questionnaire (FHSQ)
- Diabetic Foot Ulcer Scale-Short Form
- Foot and Ankle Ability Measures (FAAM).
These tools provide a standardized method for gathering information from patients regarding their well-being and functional status.10
 Diabetic foot syndrome—comprising infection or ulcer, tissue abnormalities due to peripheral vascular disease, and neuropathy—occurs in 25% of patients with DM; 15% of patients are at risk of a DFU.10 More education is therefore pertinent to the prevention and management of the sequelae of DM. Technological advances, such as telemedicine, have been shown to be a cost-effective monitoring system for detecting DFUs early.11 Other means of monitoring, such as ankle-brachial index pressures, Doppler sonography, and magnetic resonance imaging can be beneficial—but also can be intrusive, be costly, and put the patient at risk of noncompliance because they can require repeated office visits.11 There is potential for additional monitoring for early detection of DFUs in continuing research on TempStat™ and sensor-equipped insoles, as well as a smartphone app with telemedicine support, in which photo documentation and an interactive diary can be transferred to a provider, via server, for interpretation.11
Diabetic foot syndrome—comprising infection or ulcer, tissue abnormalities due to peripheral vascular disease, and neuropathy—occurs in 25% of patients with DM; 15% of patients are at risk of a DFU.10 More education is therefore pertinent to the prevention and management of the sequelae of DM. Technological advances, such as telemedicine, have been shown to be a cost-effective monitoring system for detecting DFUs early.11 Other means of monitoring, such as ankle-brachial index pressures, Doppler sonography, and magnetic resonance imaging can be beneficial—but also can be intrusive, be costly, and put the patient at risk of noncompliance because they can require repeated office visits.11 There is potential for additional monitoring for early detection of DFUs in continuing research on TempStat™ and sensor-equipped insoles, as well as a smartphone app with telemedicine support, in which photo documentation and an interactive diary can be transferred to a provider, via server, for interpretation.11
For patients who have already suffered from DFUs, it is imperative that we provide follow-up care routinely to monitor for recurrence. Education regarding better control of DM is critical, including footwear and footcare, routine follow-up with podiatry, nail care, monitoring pulses in the posterior tibial and dorsalis pedis arteries, monofilament testing, and being able to recognize signs of nonhealing wounds, discolorations, and deformities.12
Put the Patient at the Center of Your Care
Improving our communications skills to reflect a more patient-centered style allows us to assess barriers to healthcare, health-education literacy, and patient preferences in DM. In turn, being better communicators will guide us in our approach to providing improved outcomes in patients with DM.4
Angela Kelley, PA-C, is Assistant Professor, Physician Assistant Program at Gannon University in Ruskin, Florida, and a Regional Director Health Coach with Optavia (www.angela.optavia.com).
- Jackson LT, Lang E, Ehrlich A, eds. Diabetic foot ulcer. DynaMed website. www.dynamed.com/condition/diabetic-foot-ulcer. Updated November 30, 2018. Accessed February 4, 2020.
- Weintrob AC, Sexton DJ. Clinical manifestations, diagnosis, and management of diabetic infections of the lower extremities. In: Calderwood SB, Sullivan M. UpToDate. www.uptodate.com/contents/clinical-manifestations-diagnosis-and-management-of-diabetic-infections-of-the-lower-extremities. Updated October 3, 2018. Accessed February 4, 2020.
- Armstrong DG, Boulton AJM, Bus SA. Diabetic foot ulcers and their recurrence. N Engl J Med. 2017; 376(24):2367-2375.
- American Diabetes Association. Standards of Medical Care in Diabetes 2019—abridged for primary care providers. Clin Diabetes. 2019 January; 37(1):11-34.
- Betancourt JR, Green AR, Carrillo JE. Cross-cultural care and communication. In: Aronson MD, Givens J. UpToDate. www.uptodate.com/contents/cross-cultural-care-and-communication. Updated March 26, 2018. Accessed February 4, 2020.
- Delbanco T, Gerteis M. A patient-centered view of the clinician-patient relationship. In: Aronson MD, Givens J. UpToDate. www.uptodate.com/contents/a-patient-centered-view-of-the-clinician-patient-relationship. Updated February 13, 2018. Accessed February 4, 2020.
- Shorey JM, Spollen JJ. Approach to the patient. In: Aronson MD, Givens J. UpToDate. www.uptodate.com/contents/approach-to-the-patient. Updated October 16, 2019. Accessed February 3, 2020.
- Khurana L, et al. Mechanisms for improving diabetes patient–provider communication through optimal use of e-clinical technologies. Patient Prefer Adherence. 2019;13:981-992.
- Amer FA, Mohamed MS, Elbur AI, Abdelaziz SI, Elrayah ZA. Influence of self-efficacy management on adherence to self-care activities and treatment outcome among diabetes mellitus type 2. Pharm Pract (Granada). 2018;16(4):1274.
- Ortega-Avila, AB, Cervera-Garvi P, Ramos-Petersen L, Chicharro-Luna E, Gijon-Nogueron G. Patient-reported outcome measures for patients with diabetes mellitus associated with foot and ankle pathologies: a systematic review. J Clin Med. 2019;8(2):146.
- Ming A, Walter I, Alhajjar A, Leuckert M, Mertens PR. Study protocol for a randomized controlled trial to test for preventive effects of diabetic foot ulceration by telemedicine that includes sensor-equipped insoles combined with photo documentation. Trials. 20129;20(1):5212.
- DeGeorge BR, van Zuuren EJ, Ehrlich A, eds. Treatment of chronic wounds. DynaMed Web site. www.dynamed.com/management/treatment-of-chronic-wounds-18. Updated November 30, 2018. Accessed February 4, 2020.









Great topic! At Rosalind Franklin University’s Center for Lower Extremity Ambulatory Research (CLEAR), we have a number of research projects tied to the concept of addressing the patients’ needs and not simply the needs of a diabetic foot ulcer. This article seems well aligned with clinically achieving this goal.
I just shared the article with members of the American Diabetes Association’s Foot Care Interest Group.