Some studies support the effectiveness of physical therapy for reducing pain and improving function in patients with hip osteoarthritis, but evidence on the topic is limited and contradictory—suggesting that perhaps PT is most effective in a specific subgroup of patients.
By Alexis A. Wright, PT, PhD, DPT, and Garrett S. Naze, PT, DPT
Osteoarthritis, or degenerative joint disease, is the most common form of arthritis, and remains one of the chronic diseases of aging for which there is little effective treatment.1,2 OA accounts for more mobility-related disability in the elderly than any other disease, and ranks as one of the leading sources of disability in people from the U.S. as measured by disability adjusted life years (DALYs) and years lived with disability (YLDs).1,3
The natural history of hip OA is imperfectly understood; while it was once considered a naturally progressive disease, it has become increasingly clear that the disease does not necessarily follow this course.4 Some patients with hip OA experience little change in pain or function over extended periods, while others note a rapid downhill course in which the patient is disabled within a few years of disease onset.4
Regardless of symptoms, those with confirmed radiographic hip OA at are a higher risk of total hip replacement (THR), and the risk increases as minimal joint space decreases. Encouragingly, 11 to 28 years after receiving a diagnosis of radiographic hip OA more than four of five patients will not have undergone THR for hip OA.5
The optimal time for joint replacement surgery is unknown. In one study in patients undergoing THR, the duration of disease prior to surgery was 8.5 years.6 However, most studies report a wide range times, from <1 year to >15 years of reported pain prior to THR. Surgery is typically performed secondary to a patient report’s of pain, and is not necessarily based on their radiographic findings as these two factors do not always correlate.

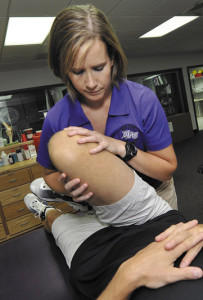
Figure 1. The Distract Manic mobilization technique is simply defined as "hip distraction manipulation."
Given that hip OA is a major cause of pain and disability in older adults, international guidelines have identified nonpharmacological treatment as one of the top 10 recommendations for management of hip OA.2,5,7,8 These guidelines include physical therapy as well as patient education, exercise, and appliances (stick or cane). Physical therapy is often considered the treatment of choice, and has been shown to reduce arthritis-associated disability.9,10
Prevalence
According to research, the prevalence of hip OA is 5% to 10% of the general adult population.11 In individuals >55 years, radiographic prevalence of hip OA increases to an estimated 68%.12 Prevalence continues to rise in proportion with age until 80 years, at which time the numbers begin to plateau.11 Differences in prevalence also have been reported between genders, with men having higher prevalence before 50 years; after this age, women demonstrate a higher prevalence. Research has also found racial differences, with Asian, African, and East Indian populations demonstrating a very low prevalence compared with higher rates noted in whites.13,14
Risk factors
The literature has defined multiple risk factors for hip OA, including genetic factors (genetic predisposition), constitutional factors (aging, gender, and greater bone mineral density), and biomechanical factors (joint laxity, muscle weakness, joint malalignment, joint injury, and occupational/recreational usage, such as regular heavy lifting over prolonged periods as well certain high-intensity, direct-impact activities, e.g., U.S. football and hockey).1,15 Other potential risk factors include weight-bearing sports; occupations requiring prolonged standing, lifting, or moving heavy objects; significant musculoskeletal injuries; and vitamin D deficiency.2,16,17
Studies have also found a link between hip dysplasia and developmental disorders, such as Legg-Calvé-Perthes disease, congenital hip dislocation, and slipped capital femoral epiphysis, and the development of hip OA.13 Along with age, hip developmental disorders and previous hip joint injury show the strongest evidence correlating to development of hip OA.15
Clinical presentation
Pain, stiffness, and reduced movement or function characterize the clinical presentation of hip OA.18,19 Of these, joint pain is the primary reason people seek medical intervention. Typically, this pain is described as a deep, aching, poorly localized discomfort, which has been present for a number of years.4 Early in the disease process the pain is reported as gradual in onset and episodic, but over time the pain is reported as gradual in onset and episodic, but over time becomes more constant, with unanticipated episodes of sharp pain with movement.2 Progression of OA is also associated with morning stiffness, pain at rest or at night, decreased active joint movement, lower limb weakness, slower gait, reduced aerobic capacity, and decreased mobility.2,4,20,21 These impairments lead to functional limitations in walking, stair climbing, entering and exiting vehicles, cycling, donning shoes, and participation in social activities.21
The level of disability related to hip OA symptoms is strongly correlated with psychological well-being and the ability to cope with pain.22 Painful hip OA can also cause psychological distress, depression, and sleep disorders and can potentially produce neuropathic elements including local nerve root irritation or radiculopathy; all these factors can have implications for patient management.1 Patients often view arthritis as a normal process of aging and therefore expect their mobility to decline with age. This, along with activity avoidance due to pain, often leads to further functional decline.23,24
Clinical examination
A decrease in the freedom of active movement is often the first sign of hip OA.4 Internal rotation and flexion are usually the first two motions to be restricted, followed by hip external rotation.25 Restriction (<40th percentile) of internal rotation has been identified as most diagnostic of hip OA in terms of single plane movements, with a reported odds ratio of 3.6 (95%CI: 1.6, 8 ) for mild to moderate OA and 46.8 (95%CI: 5.2, 420) for severe OA, while restriction in all three planes was associated with a sensitivity of 33% for mild to moderate OA and 54% for severe OA and specificities of 93% and 88%, respectively.
Functionally, range of motion losses in hip extension and external rotation have been most closely associated with disability.26 Also useful in clinical assessment is the FABER (flexion abduction external rotation) test, or Patrick’s test of the hip. This test combines the movements of flexion, abduction, and external rotation, and is designed to provoke the patient’s chief complaint of hip pain.13,27 Another provocative test is the scour test, which combines hip flexion and adduction until resistance is detected. Hip flexion is then maintained while the clinician moves the hip into two arcs of abduction. If no pain is reported, the examiner applies long-axis compression through the femur to further identify joint involvement.13
Impairments in muscle strength are also found in patients with hip OA, particularly in the hip abductor muscle groups. This may create an apparent Trendelenberg gait pattern in the later stages of hip OA.13 It is important to assess the lumbar extensors and hip adductors given the proximity of the lumbar spine to the hip joint as well as interdependence of these two areas in lumbopelvic stabilization.21 Finally, performance measures, such as the timed up-and-go test, the six-minute walk test, and the 10-meter walk test, have been found to be better predictors of physical function than pain levels in hip OA, and therefore should be an included in clinical assessment.19
Treatment
Pain relief and preservation of function remain the primary treatment objectives for patients with hip OA. Clinicians should manage these patients on an individual basis and modify treatment based on response.18 The recommended hierarchy of management should consist of nonpharmacological treatments, then drugs, and, if necessary, surgery.15 Too often this first step—nonpharmacological treatment—is forgotten, or not emphasized sufficiently; this to patients’ detriment, given that manual therapy and exercise therapy have demonstrated improvements in pain and function.18 Furthermore, clinicians should avoid surgery when patients’ symptoms can be managed by other treatment modalities. 18
A variety of nonpharmacological interventions have been described for the treatment of hip OA, and some evidence supports the benefits of physical therapy. Exercise and physical activity can be targeted at the affected joint and also at improving general mobility, function, well-being, and self-efficacy.15 Exercise therapy for OA consists of range of movement/flexibility exercises, muscle-strengthening exercises, and aerobic conditioning/endurance exercises. Often, practitioners prescribe all three forms of exercise for patients with hip OA, and some evidence suggests exercise reduces pain in people with this condition.28
McNair et al29 suggested there is insufficient evidence to support the use of land-based exercise therapy as a treatment for decreasing pain, improving function, or enhancing quality of life in patients with hip OA. The authors noted there is limited evidence regarding the efficacy of exercise therapy, and most is based on findings of a few well-designed studies focused solely on hip OA. They also suggested a need for further research to investigate the efficacy of exercise therapy for reducing pain and improving joint function and quality of life.29 A recent Cochrane systematic review30 supported these findings, suggesting that, in people with hip OA, land-based exercise therapy may reduce pain slightly but may not improve physical function.
A meta-analysis by Hernandez-Molina9 reported on the effectiveness of range of motion and strengthening exercises (including hydrotherapy) in patients with hip OA, extracting data on patients with hip OA from trials that combined findings from patients with both hip and knee OA.9 These authors found hip strengthening exercises reduced pain and improved function.9, 31
Pisters et al31 further suggested that while positive post-treatment effects of exercise therapy on pain and physical function in patients with hip or knee OA are not sustained in the long term, these effects can be maintained with additional booster sessions following cessation of the initial treatment.
The patient and the health professional should agree on the goals of prescribed exercise. A minimum of six weeks treatment is advised to ensure that patients experience some benefits of treatment and undergo behavioral changes.21 It is important to encourage the continuation of exercise both during and after treatment.15, 21

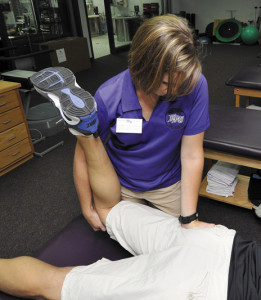
Figure 4. The PA Figure 4 technique is defined as "posterior to anterior hip mobilization in figure 4 positioning."
There is some evidence that manual therapy in patients with mild hip OA produces short-term increases in hip joint range of motion, as well as improvements in function and pain.10,13,32,33 These therapies use manual force to improve mobility of restricted joints, connective tissue, or skeletal muscles, and are directed at influencing joint function and pain. One study reported that, compared with exercise therapy, manual therapy produced general improvements, better hip function, and reduced pain in some patients with mild hip OA.10 Given these results, manual therapy is suggested to provide short-term pain relief and improve hip mobility and function in patients with mild hip OA; however, the grade of recommendation remains moderate given that currently only a single high-quality randomized controlled trial10 supports the recommendation.
Limited and conflicting evidence in support of physical therapy intervention in patients with hip OA may suggest physical therapy intervention is most effective in a subgroup of patients with hip OA. Early study results have identified patient variables associated with a favorable response to physical therapy, including selected combinations of unilateral hip pain, age ≤58 years, pain ≥6/10 on the numeric pain rating scale, walking time ≤25.9 seconds on the 40-m self-paced walk test, and duration of symptoms ≤1 year. These factors were associated with decreased pain and increased function following physical therapy.34 These findings suggest patients presenting with the above characteristics should be considered strong candidates for early referral to physical therapy to delay or avoid more aggressive interventions, such as total joint replacement surgery.
Alexis A. Wright, PT, PhD, DPT, is an assistant professor in the Department of Physical Therapy at High Point University School of Health Sciences in High Point, NC. Garrett S. Naze, PT, DPT, is a physical therapist in the Department of Physical Therapy at the University of Illinois Medical Center at Chicago.
References
1. Felson DT. Developments in the clinical understanding of osteoarthritis. Arthritis Res Ther 2009;11(1):203.
2. Lane NE. Osteoarthritis of the hip. N Engl J Med 2007;357(14):1413-1421.
3. Michaud CM, McKenna MT, Begg SJ, et al. The burden of disease and injury in the United States 1996. Popul Health Metr 2006;4:11.
4. Buckwalter JA, Martin JA. Osteoarthritis. Adv Drug Deliv Rev 2006;58(2):150-167.
5. Franklin J, Ingvarsson T, Englund M, et al. Natural history of radiographic hip osteoarthritis: a retrospective cohort study with 11-28 years of followup. Arthritis Care Res 2011;63(5):689-695.
6. Bachmeier CJ, March LM, Cross MJ, et al. A comparison of outcomes in osteoarthritis patients undergoing total hip and knee replacement surgery. Osteoarthritis Cartilage 2001;9(2):137-146.
7. Lawrence RC, Helmick CG, Arnett FC, et al. Estimates of the prevalence of arthritis and selected musculoskeletal disorders in the United States. Arthritis Rheum 1998;41(5):778-799.
8. Zhang W, Doherty M, Arden N, et al. EULAR evidence based recommendations for the management of hip osteoarthritis: report of task force of the EULAR Standing Committee for International Clinical Studies Including Therapeutics (ESCISIT). Ann Rheum Dis 2005;64(5):669-681.
9. Hernández-Molina G, Reichenback S, Zhang B, et al. Effect of therapeutic exercise for hip osteoarthritis pain: results of a meta-analysis. Arthritis Rheum 2008;59(9):1221-1228.
10. Hoeksma HL, Dekker J, Ronday HK, et al. Comparison of manual therapy and exercise therapy in osteoarthritis of the hip: a randomized clinical trial. Arthritis Rheum 2004;51(5):722-729.
11. Dagenais S, Garbedian S, Wai EK. Systematic review of the prevalence of radiographic primary hip osteoarthritis. Clin Orthop Relat Res 2009;467(3):623-637.
12. Elders MJ. The increasing impact of arthritis on public health. J Rheumatol Suppl 2000;60:6-8.
13. Cibulka MT, White DM, Woehrle J, et al. Hip pain and mobility deficits – hip osteoarthritis: Clinical practice guidelines linked to the international classification of functioning, disability, and health from the Orthopaedic section of the American Physical Therapy Association. J Orthop Sports Phys Ther 2009;39(4):A1-A25.
14. D’Ambrosia RD. Epidemiology of osteoarthritis. Orthopedics 2005;28(2 suppl):S201-S205.
15. National Institute for Health and Clinical Excellence. Osteoarthritis: national clinical guideline for care and management in adults. www.nice.org.uk/CG059. Published February 2008. Accessed August 26, 2011.
16. Das SK, Farooqi A. Osteoarthritis. Best Pract Res Clin Rheumatol 2008;22(4):657-675.
17. Juhakoski R, Heliövaara M, Impivaara O, et al. Risk factors for the development of hip osteoarthritis: a population-based prospective study. Rheumatology 2009;48(1):83-87.
18. Hunter DJ, Felson DT. Osteoarthritis. BMJ 2006;332(7542):639-642.
19. Juhakoski R, Tenhonen S, Anttonen T, et al. Factors affecting self-reported pain and physical function in patients with hip osteoarthritis. Arch Phys Med Rehabil 2008;89(6):1066-1073.
20. Arnold CM, Faulkner RA. Does falls-efficacy predict balance performance in older adults with hip osteoarthritis. J Gerontol Nurs 2009;35(1):45-52.
21. Vogels EM, Hendriks HJ, Van Baar ME, et al; The Royal Dutch Society for Physical Therapy (KNGF). KNGF-guidelines for physical therapy in patients with osteoarthritis of the hip or knee. https://www.cebp.nl/media/m11.pdf. Published 2003. Acessed August 26, 2011.
22. van Baar ME, Dekker J, Lemmens JA, et al. Pain and disability in patients with osteoarthritis of hip or knee: the relationship with articular, kinesiological, and psychological characteristics. J Rheumatol 1998;25(1):125-133.
23. Appelt C, Burant CJ, Siminoff LA, et al. Arthritis-specific health beliefs related to aging among older male patients with knee and/or hip osteoarthritis. J Gerontol A Biol Sci Med Sci 2007;62(2):184-190.
24. Goodwin JS, Black SA, Satish S. Aging versus disease: the opinions of older black, Hispanic, and non-Hispanic white Americans about the causes and treatment of common medical conditions. J Am Geriatr Soc 1999;47(8):973-979.
25. Cibulka MT, Threlkeld J. The early clinical diagnosis of osteoarthritis of the hip. J Orthop Sports Phys Ther 2004;34(8):461-467.
26. Steultjens MP, Dekker J, van Baar ME, et al. Range of joint motion and disability in patients with osteoarthritis of the knee or hip. Rheumatology 2000;39(9):955-961.
27. Martin RL, Sekiya JK. The interrater reliability of 4 clinical tests used to assess individuals with musculoskeletal hip pain. J Orthop Sports Phys Ther 2008;38(2):71-77.
28. Fransen M, McConnell S, Bell M. Exercise for osteoarthritis of the hip or knee. Cochrane Database Syst Rev 2001(3):CD004286.
29. McNair PJ, Simmonds MA, Boocock MG, Larmer PJ. Exercise therapy for the management of osteoarthritis of the hip joint: a systematic review. Arthritis Res Ther 2009;11(3):R98.
30. Fransen M, McConnell S, Hernandez-Molina G, Reichenback S. Exercise for osteoarthritis of the hip. Cochrane Database Syst Rev 2009(3): CD007912.
31. Pisters MF, Veenhof C, van Meeteren NL, et al. Long-term effectiveness of exercise therapy in patients with osteoarthritis of the hip or knee: a systematic review. Arthritis Rheum 2007;57(7):1245-1253.
32. MacDonald CW, Whitman JM, Cleland JA, et al. Clinical outcomes following manual physical therapy and exercise for hip osteoarthritis: a case series. J Orthop Sports Phys Ther 2006;36(8):588-599.
33. Brantingham JW, Globe G, Pollard H, et al. Manipulative therapy for lower extremity conditions: expansion of literature review. J Manipulative Physiol Ther 2009;32(1):53-71.
34. Wright AA, Cook CE, Flynn TW, et al. Predictors of response to physical therapy intervention in patients with primary hip osteoarthritis. Phys Ther 2011;91(4):510-524.









It is interesting that physical therapy can improve general mobility for patients with hip OA. My wife has had pain in her hip for the past three years and she has weak hip muscles as well. We may consider reaching out to a professional for recommendations.