By Cristina Bayón, Marleen van Hoorn, Antonio Barrientos, Eduardo Rocon, Joyce P. Trost, and Edwin H. F. van Asseldonk
Ankle-foot orthoses are extensively used as a primary management method to assist ambulation of children with cerebral palsy (CP). However, certain barriers hinder their prescription as well as their use as a mobility device in all kinds of daily-life activities.
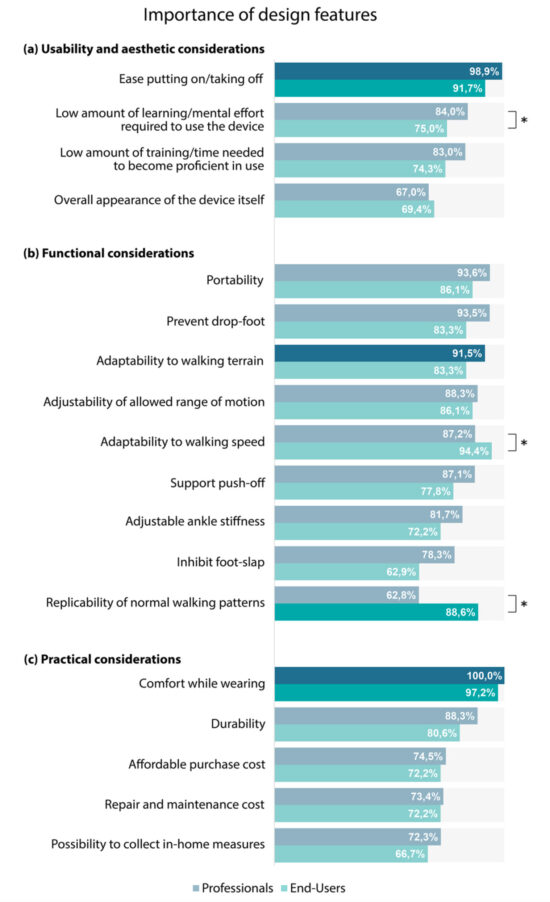
Percentage of respondents who ranked the design features as 4–important or 5–very important. Significant differences between GP and GU reported by the Mann–Whitney U tests are marked with (*). The darker bars represent those features that were selected as the top priority by the respondents within each category (a–c)
Improving the walking ability of patients with CP is a primary goal to allow for a more active and independent lifestyle. Due to the role of the ankle joint in gait and the greater muscle dysfunction of distal lower-extremity muscles in CP, ankle-foot orthoses (AFOs) are the foremost used type of assistive devices. Technological advances over the last decades have resulted in the development of AFO designs for CP, which are typically prescribed depending on the pathological gait pattern and the functional capacities (level of the Gross Motor Function Classification System, GMFCS) of the child. However, certain barriers hinder their prescription as well as their use as a mobility device in daily-life activities. This exploratory research attempts to further understand the existing limitations of current AFOs to promote a better personalization of new design solutions.
Methods
Stakeholders’ (healthcare professionals in CP and end-users with CP) perspectives on AFO technology were collected by 2 online surveys. Respondents evaluated the limitations of current assistive solutions and assessment methods, provided their expectations for a new AFO design, and analyzed the importance of different design features and metrics to enrich the gait performance of these patients in daily life.
Results
The survey respondents comprised 94 professionals who specialize in CP (GP) and 36 end-users with CP (GU). The most highly rated design features by both stakeholder groups were comfort and ease of donning and doffing the AFO. In general, professionals preferred new features to enrich the independence of the patient by improving gait at functional levels. End-users also considered their social acceptance and participation. (See Table 1.) Healthcare professionals reported a lack of confidence concerning decision making about AFO prescription. To some degree, this may be due to the reported inconsistent understanding of the type of assistance required for each pathological gait. Thus, they indicated that more information about patients’ day-to-day walking performance would be beneficial to assess patients’ capabilities.
Discussion
The most valuable feature identified by both groups was the “comfort while wearing” the AFO, ie, avoiding skin pressure, friction, or abrasions. The second most valuable design feature highlighted by both groups was the “ease of putting on and taking off” the device. Stakeholders also proposed a change to have a more breathable and softer AFO material and a better fit to the child’s foot. The rated importance for these cost features did not override the comfort and usability of the device.
Regarding “replicability of normal walking patterns,” 62.8% of GP vs 88.6% of GU considered this feature to be “important” or “very important.” While professionals preferred to provide the child with higher autonomy by making the AFO “adaptable to different walking terrains,” end-users preferred having a “more normal walking pattern.”
Concerning the classification that professionals made of the type of AFO with respect to the level of the GMFCS: (1) patients classified as GMFCS I normally have the ability to walk, so minimal additional assistance of any type is needed; (2) patients classified within levels GMFCS IV and V can barely walk, so they do not benefit that much from AFOs; and (3) patients classified within GMFCS I+ to III can benefit the most from the extra support provided by dynamic AFOs. In these cases, the prevention of drop foot is more important for less severely affected gait patterns (GMFCS I+ and II), while push-off support becomes more important as gait patterns get more severely affected (GMFCS II+ and III).
This convoluted connection between the level of the GMFCS, the patient’s pathological gait and the type of assistance needed makes it hard to prescribe the most suitable AFO for a specific patient.
Implications for future devices
Existing traditional (passive) solutions present an inherent function as mobility devices; however, from the survey responses, the AFOs are not adaptable to a specific patient’s needs, nor do they enhance their existing capabilities. Although there have been promising advances, especially with adjustable dynamic AFOs, they still lack the necessary evidence to demonstrate the adaptability to different scenarios and the achievement of lasting improvements and long-term effects in general gait quality.
For new AFO designs, the benefits of robotic technology (eg, tailoring the assistance provided) should be considered. Users’ expectations to adopt a new solution are positive. However, the survey respondents indicated it is key to address the current problems of powered devices, including comfort, weight, bulkiness, safety, operability, and user-friendliness. To satisfy the requirements of both healthcare professionals and end-users, there should be a trade-off between the improvement of functional levels, the provision of higher autonomy, and the social acceptance while using the device.
Finally, the incorporation of sensors within the design of new AFOs might be an option to provide metrics and assess the user’s gait in daily life to inform clinical decision making.
Conclusion
This exploratory study provides insights into the weighted desires of children with CP, their families, and professionals in the field toward the use and design of AFOs. The stakeholders’ needs and criteria reported here may serve as insights for the design of future assistive devices and for the follow-up monitoring of these patients.
This article has been excerpted from “Perspectives on Ankle-Foot Technology for Improving Gait Performance of Children with Cerebral Palsy in Daily-Life: Requirements, Needs and Wishes,” J NeuroEngineering Rehabil 20, 44 (2023). https://doi.org/10.1186/s12984-023-01162-3. Editing has occurred, including the renumbering or removal of tables, and references have been removed for brevity. Use is per CC BY.