 By Cassandre Voltaire, DO
By Cassandre Voltaire, DO
Wound care is an evolving science, but if there’s one lesson I’ve learned, it’s this: healing isn’t just about using the latest product—it’s about knowing when and how to use it.
Early in my career as a family physician, I saw a number of chronic wounds stagnate despite standard treatments. Patients were frustrated. So were we. The limitations of traditional approaches were clear, but what wasn’t clear was how to bridge the gap between persistence and progress.
It wasn’t until I transitioned fully into wound care that I had my epiphany: precision matters more than intervention. The right product, applied at the right time, can turn a stalled wound into one that finally heals. Among the tools that have revolutionized wound care, cellular, acellular, and matrix-like products (CAMPs) stand out—not as a cure-all, but as a finely tuned instrument in the hands of those who understand their use.
Understanding CAMPs: Engineering the Body’s Healing Blueprint
CAMPs are not just advanced dressings. They are bioengineered scaffolds that mimic the extracellular matrix (ECM)—the skin’s natural support system. By providing a structure that promotes cellular migration, angiogenesis, and granulation tissue formation, CAMPs create an environment conducive to healing.
But the effectiveness of CAMPs doesn’t come from simply applying them. Matching the right product to the right wound at the right time is essential. This is something I learned firsthand from a patient whose case taught me the importance of timing and precision.
A Case of Precision: The Right Choice at the Right Time
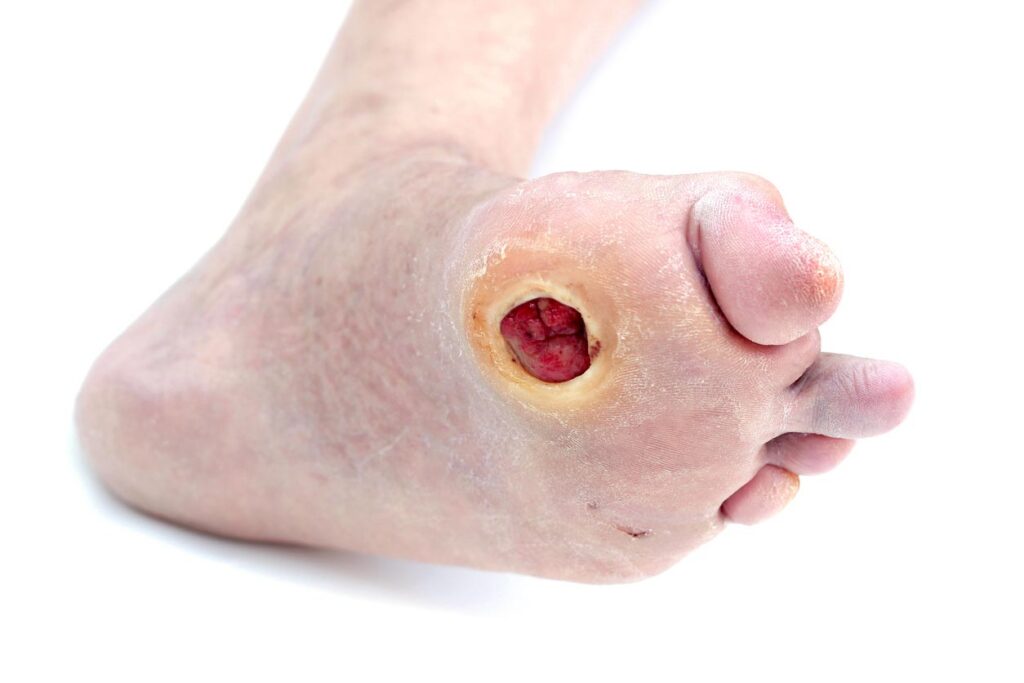
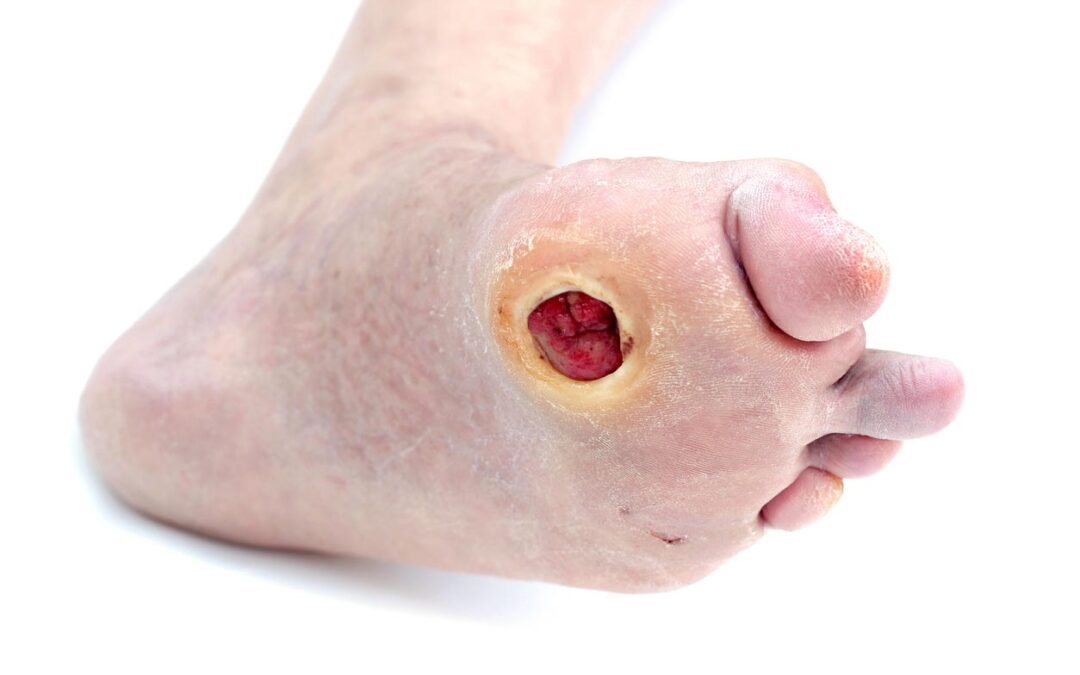
One patient with a diabetic foot ulcer stands out in my memory. His ulcer had been stagnant for months despite standard treatments like offloading, debridement, and dressings. He was understandably frustrated.
Instead of immediately reaching for an advanced product, we took a step back. We optimized his hyperglycemia and addressed vascular insufficiency, ensuring his wound was in the best possible state for healing. Once his wound was stable and free from infection, we used a bilayered bioengineered matrix product—not as a last resort, but as a deliberate, well-timed choice.
The difference was remarkable. Within 6 weeks, granulation tissue filled the base, epithelialization was progressing, and—most importantly—his hope was renewed. It was a powerful reminder that CAMPs are not a one-size-fits-all solution. Their success depends on timing, preparation, and precise application.
This case reinforced what I’ve come to believe: CAMPs work, but only when the wound is truly ready.
Choosing the Right CAMP for the Right Wound
CAMPs come in different forms, each with unique benefits:
- Human Skin Allografts – Derived from cadaveric skin, these retain growth factors that promote regeneration.
- Allogeneic Matrices – Created from human tissue, designed to support chronic wound repair.
- Composite Matrices – A blend of living cells and scaffolds, often using xenogeneic collagen to enhance healing.
- Acellular Matrices – Structural scaffolds from human, porcine, or bovine sources that provide a framework for cellular infiltration and tissue regeneration.
Choosing the right CAMP isn’t about following a strict formula. It requires understanding each product’s strengths and how they align with the wound’s needs. In my practice, I’ve seen how the right choice can make a dramatic difference in healing outcomes.
Where CAMPs Shine
From my experience, CAMPs are particularly effective for:
- Venous Leg Ulcers (VLUs) – Often combined with compression therapy for better results.
- Diabetic Foot Ulcers (DFUs) – Particularly effective when standard treatments fail.
- Complex Chronic Wounds – Including pressure ulcers, burns, and surgical wounds, where emerging evidence supports their use.
- However, despite their potential, the use of CAMPs is complicated by more than just clinical considerations.
Navigating Reimbursement and Policy Challenges
Two significant challenges often limit the use of CAMPs:
1. Reimbursement Limitations – Local Coverage Determinations (LCDs) cap the number of CAMP applications for DFUs and VLUs, which can limit access. Originally set to take effect this year, these LCD changes have now been delayed until April 13, 2025. This delay presents an opportunity to advocate for policies that better align with patient needs.
2. Documentation Demands – To justify the use of CAMPs, clinicians must provide thorough documentation, including wound history, prior treatments, and measurable outcomes.
The regulatory landscape is complex, but staying informed and advocating for fair policies is crucial for ensuring that patients have access to the best available treatments.
Lessons Learned: Precision Matters
Reflecting on my journey with CAMPS, 3 key insights stand out:
- Timing and Precision – The right product at the wrong time won’t work. Assessing the wound’s readiness is just as important as selecting the product itself.
- Advocacy Is Essential – With LCD changes on the horizon, clinicians must engage in policy discussions to ensure patient access to these innovative therapies.
- Holistic Care Comes First – Even the most advanced CAMP can’t replace vascular optimization, offloading, infection control, and comprehensive patient-centered care.
CAMPs are more than just innovative products – they represent an opportunity to heal smarter and with greater precision, ensuring patients receive the most appropriate care at the right time. When used wisely, they remind us of the ultimate goal: transforming lives, one wound at a time.
Cassandre Voltaire, DO, is a wound care physician specializing in advanced wound management and chronic wound healing. Based in Massachusetts, she combines her background in family medicine with holistic and evidence-based wound care. She is also the founder of WoundFit, dedicated to empowering healthcare providers with accessible wound care education and resources.








Desperate decision to close a very chronic back surgery wound had me provide a Pulsed Galvanic Stimulation unit to HHA wound care nurse. The flesh in the wound looked like pale porkchop meat. Less than a week of PGS use (saline soaked gauze with + & – clips attached to deliver direct current to wound), nurses called & said tissue was now bright red with increased blood flow & wound was shrinking in depth and length for first time in months. Closed wound successfully. Happy orthoped, patient, and nurse.