 In free-living environments, more time spent in exercise-like activities has the strongest association with blood pressure (BP), and even small changes to daily movement patterns can elicit clinically meaningful improvements.
In free-living environments, more time spent in exercise-like activities has the strongest association with blood pressure (BP), and even small changes to daily movement patterns can elicit clinically meaningful improvements.
Multinational researchers from the ProPASS Consortium (Prospective Physical Activity, Sitting and Sleep) used data from thigh-worn accelerometers and BP measurements of 14,761 free-living participants (mean age 54.2±9.6 years) to study associations between 24-hour behaviors in 6 areas (sleeping, sedentary behavior, standing, slow walking, fast walking, and combined exercise-like activities [eg, running and cycling]) and both systolic and diastolic blood pressure.
The average 24-hour composition consisted of sleeping (7.13±1.19 hours), sedentary behavior (10.7±1.9 hours), standing (3.2±1.1 hours), slow walking (1.6±0.6 hours), fast walking (1.1±0.5 hours), and exercise-like activity (16.0±16.3 minutes). More time spent exercising or sleeping, relative to other behaviors, was associated with lower BP. An additional 5 minutes of exercise-like activity was associated with estimated reductions of -0.68 mm Hg (95% CI, -0.15, -1.21) SBP and -0.54 mm Hg (95% CI, -0.19, 0.89) DBP. Clinically meaningful improvements in SBP and DBP were estimated after 20 to 27 minutes and 10 to 15 minutes of reallocation of time in other behaviors into additional exercise. Although more time spent being sedentary was adversely associated with SBP and DBP, there was minimal impact of standing or walking.
Clinical Implications:
- Small and feasible changes to habitual exercise levels are estimated to have meaningful benefits on BP, which can contribute to a reduction in prevalence of hypertension.
- Exercise-induced reductions in BP can reduce prevalence of cardiovascular outcomes by7% to 28% at the population level.
- Interventions targeting both the individual and the population (eg, public health policies) should consider the wider construct of the 24-hour day and incidental exercise embedded in daily activities.
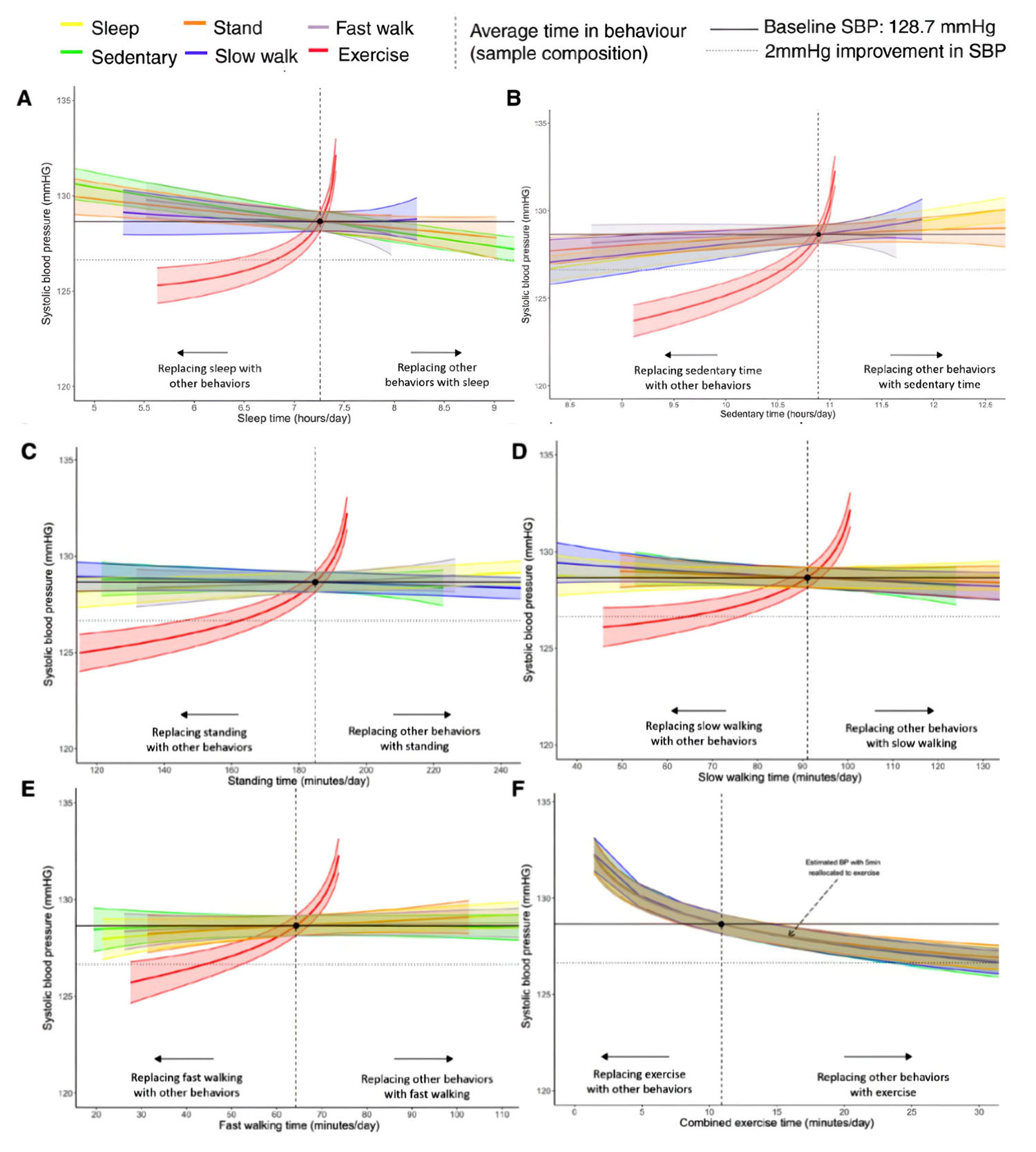
Figure 1. Estimated change in systolic blood pressure (n=14 761) based on behavioral relocation from the average composition of the population:
Sleep (A), sedentary behavior (B), standing (C), slow walking (D), fast walking (E), and combined exercise-like activities (F). Data to the left of the reference line indicate the predicted change in systolic blood pressures if a given behavior were replaced by any of the other behaviors. Data to the right of the reference line indicate the predicted change if a given behavior replaced any of the other behaviors. Model adjusted for sex (reference: female), age (reference: 54.2 years; mean-centered), and cohort (reference: The Maastricht Study). Reallocations are based on baseline systolic blood pressure (SBP; 128.7 mm Hg) expected given the average sample composition (sleep, 7.3 hours; sedentary behavior, 10.9 hours; stand, 3.1 hours; slow walk, 1.5 hours; fast walk, 1.1 hours; and combined exercise-like, 10.9 minutes per day).
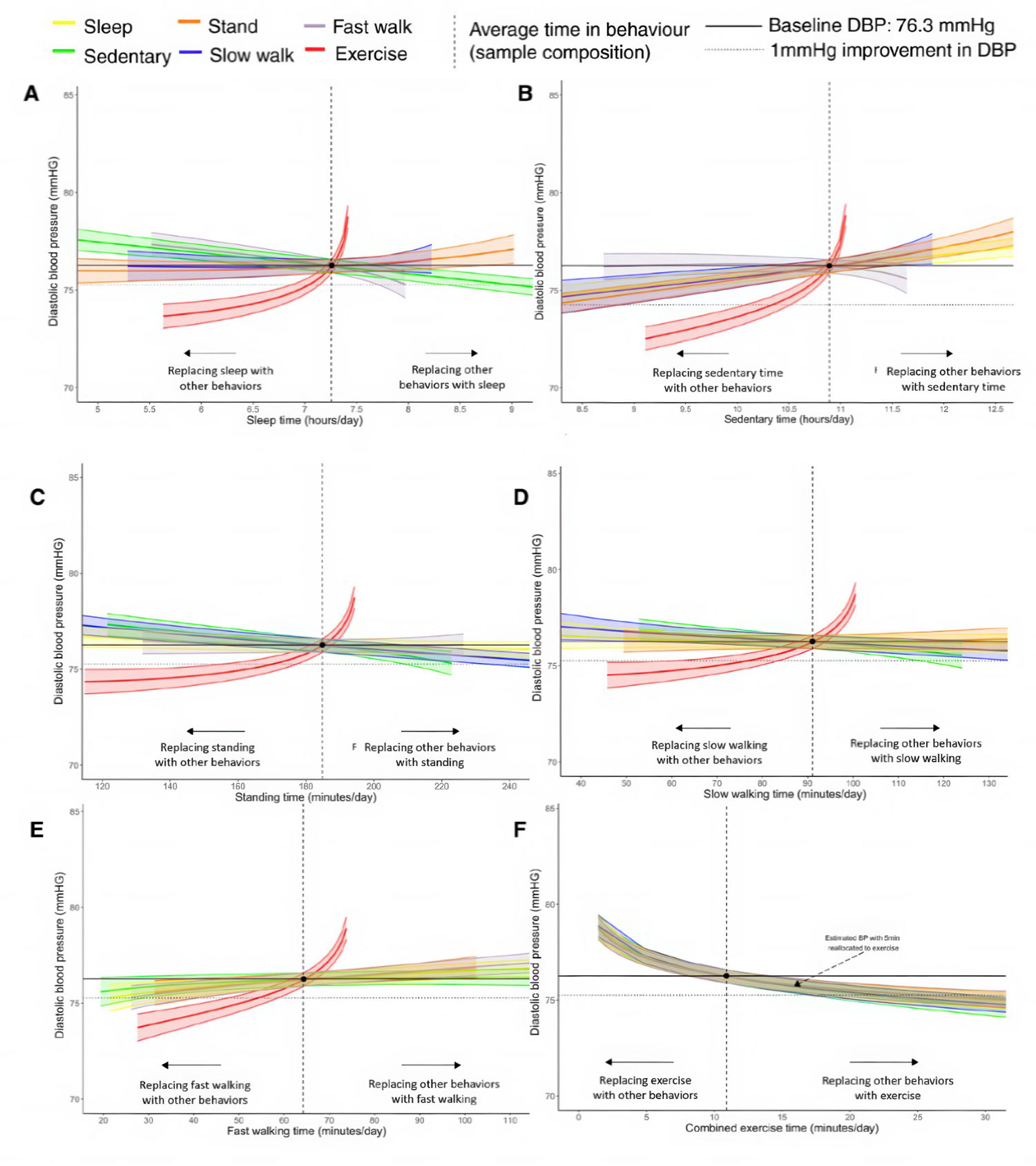
Figure 2. Theoretical change in diastolic blood pressure (n=14 761) based on behavioral relocation from the average behavior composition of the population. Sleep (A), sedentary behavior (B), standing (C), slow walking (D), fast walking (E), and combined exercise-like activity (F). Data to the left of the reference line indicate the predicted change in systolic blood pressures if a given behavior is replaced by any of the other behaviors. Data to the right of the reference line indicate the predicted change if a given behavior replaces any of the other behaviors. Model adjusted for sex (reference: female), age (reference: 54.2 years; mean-centered), and cohort (reference: The Maastricht Study). Reallocations are based on baseline diastolic blood pressure (DBP; 76.25 mm Hg) expected given the average sample composition (sleep, 7.3 hours; sedentary behavior, 10.9 hours; stand, 3.1hours; slow walk, 1.5 hours; fast walk, 1.1 hours; combined exercise-like, 10.9 minutes per day).
This article has been excerpted from: Blodgett JM, Ahmadi MN, Atkin AJ, et al for the ProPASS Collaboration. Device-measured 24-hour movement behaviors and blood pressure: A 6-part compositional individual participant data analysis in the ProPASS Consortium. Circulation. 2025;151(12):159-170. doi: 10.1161/CIRCULATIONAHA.124.069820. Epub: Nov. 6, 2024. Permission is by CC BY 4.0.







