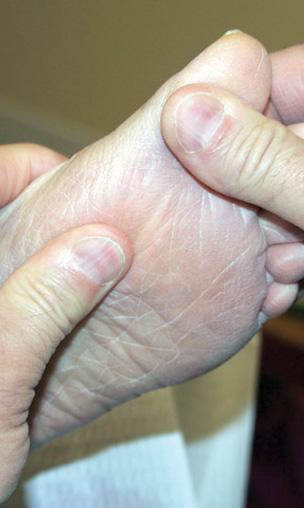
 A simple, quick clinical test can help identify functional hallux limitus, a condition that is currently underdiagnosed and, consequently, undertreated. Once identified, functional hallux limitus can be effectively managed with orthotic devices.
A simple, quick clinical test can help identify functional hallux limitus, a condition that is currently underdiagnosed and, consequently, undertreated. Once identified, functional hallux limitus can be effectively managed with orthotic devices.
By James G. Clough, DPM
Functional hallux limitus is a separate distinct diagnosis from structural hallux limitus. Functional hallux limitus (FnHL) is characterized by a lack of motion of the first metatarsophalangeal (MTP) joint during gait only.1 The first MTP joint will demonstrate normal motion during an open kinetic chain examination. Radiographs will sometimes show a small amount of dorsal spurring of the joint, however, the joint does not demonstrate pervasive degenerative joint disease (Fig. 1).
Structural hallux limitus (SHL) is characterized by structural adaptations of the first MTP joint that prevent normal motion from occurring (Fig. 2). These changes can be severe, with very limited dorsiflexion mobility, (hallux rigidus) or minor, ( hallux limitus) resulting in small changes in dorsiflexion of the first MTP joint. When first MTPJ motion is disrupted enough to prevent stabilization of the foot structure during maximal hallux dorsiflexion, through the effect of the windlass mechanism, then normal foot stabilization during propulsion is disrupted, and becomes clinically significant. In SHL, motion will be disrupted during both open- and closed-kinetic chain activities. Often, there is crepitation with joint mobilization and pain associated with any movement of the first MTP joint.
Functional hallux limitus has been identified in 53 of 86 asymptomatic feet by Payne et al.2 Even though the condition itself may be asymptomatic, the clinical manifestations of this condition can in my experience also be associated with many common pathologies related to the foot, including heel pain, lesser metatarsal pain, mortons neuromas, achilles tendon pain, and retrocalcaneal enthesitis, as well as posterior tibial tendon dysfunction and postural alignment abnormalities of the lower extremity and lumbar spine. My unpublished research to date indicates that the incidence of this disorder is much higher in the symptomatic population.
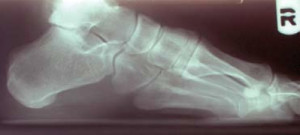
Figure 1. Radiograph of functional hallux limitus. Note the lack of joint destruction in this joint with functional limitation of motion.
It remains, however, an infrequently recognized condition, and therefore one that often goes unaddressed. This is unfortunate, as orthotic outcomes for a variety of foot disorders will be compromised if treatment does not address an underlying functional hallux limitus, when present. Most foot and postural abnormalities have a basis in poor function of the windlass mechanism and stabilization of the foot structure through the taut plantar fascia. If this stabilizing effect is not present, it is hypothesized that a variety of foot disorders may result as normal foot function cannot be achieved without proper function of the plantar fascia.3,4 We do know that addressing the proper function of the foot has a high level of predictability for addressing mechanically induced foot pain in general, and this remains the goal of footbed and shoe modifications and has been the focus of orthotic intervention for years.
Identifying functional hallux limitus

Figure 2. Radiographs of structural hallux limitus. Note the significant spurring of the joint preventing mobolization and the pervasive destructive changes in the joint.
Identification of FnHL by observing gait patterns and via pedobarographic analysis, which has been described anecdotally, requires either a very trained eye or expensive equipment and time consuming testing that is rarely able to be performed in the clinical setting. These challenges likely contribute to the underdiagnosis of FnHL.
A FnHL test has been previously described by Dananberg,5 but never published in a peer reviewed journal. He observed a stiffening of big toe joint motion when holding the STJ in neutral position and applying a loading force to the first ray to the point of maximal dorsal displacement.. When hallux dorsiflexion at the MTPJ is attempted, there is a stiffening or locking of motion of the first MTPJ, when approximately equal force is appplied to the hallux as is applied to the first metatarsal head. Payne has reviewed this test and correlated it with visual gait analysis and has noted a sensitivity of 0.72, meaning that 72 % of feet with a pronated midtarsal joint also had a positive test for functional hallux limitus.2 A specificity of 0.66 was noted as 66% of feet with normal midtarsal joint motion had a negative test result. Payne felt this to be a reliable test for the diagnosis of abnormal foot function. This test was performed on asymptomatic individuals. My own clinical experience shows that this test is positive in a much larger percentage of symptomatic patients.
Modifying the test
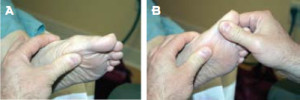
Figure 3. Positive functional hallux limitus test. A: A load is applied to the first metatarsal head to simulate ground reaction force. B: As dorsiflexion of the toe is attempted, there is a jamming at the first metatarsophalangeal joint.
I have made a small modification to the functional hallux limitus test and have found that the modified version is easy to incorporate into a foot assessment as part of the evaluation of clients with foot pain and pathology. As part of a regular protocol of biomechanical evaluation, it becomes a useful tool when recommending appropriate conservative and surgical care.
The foot is held in dorsiflexion with the foot maximally pronated but not in subtalar neutral position, based on evidence that this is not the foot’s position during midstance.6 Studies also suggest that an orthotic device has little effect on this position.7-15
An axial load, simulating ground reaction force load, is applied under the first metatarsal head. This is done with the thumb of the hand medial to the first metatarsal. When performing this test on the left foot, this would be the left thumb (Fig. 3a). This load is relatively firm, considering the body weight going through the foot during stance. If the force is inadequate, the FnHL test will be difficult to interpret. The force should be adequate to cause the medial column to be displaced in its maximally elevated position, as would normally occur during loading of the foot in midstance. We are strictly testing the mobility of the first MTP joint at this time; this is not a dynamic assessment.
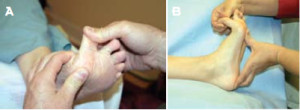
Figure 4. Negative functional hallux limitus test. A: Plantarflexion of the first metatarsal. B: Stability of the arch is achieved through the windlass mechanism once dorsiflexion of the first MTP joint is achieved.
The thumb of the opposite hand (the right thumb, when testing the left foot) then attempts dorsiflexion of the toe. (Fig. 3b) When dorsiflexion of the toe is attempted in a foot with functional hallux limitus, there will be a distinct lack of plantar flexion of the first metatarsal head into the left thumb and a perceived ‘jamming’ of first MTP joint motion. The patient as well as the clinician will be able to readily perceive this ‘jamming’ or ‘locking’ of joint motion. This occurs as the axis of the first MTP joint actually changes, becoming more dorsal and resulting in altered joint movement.16,17
In a foot without FnHL, the first metatarsal head readily plantarflexes into the thumb that is under the first metatarsal head, and first MTP joint range of motion is unrestricted. (Fig. 4a) Stability of the foot is achieved because of the windlass mechanism (Fig. 4b).
The difference in the character of the movement of the first MTPJ in these two situations is quite remarkable, and with a little practice, this test literally takes a few seconds to perform.
To confirm the diagnosis, examine the wear pattern of the patient’s shoe insole and the callus pattern of the foot. With FnHL the first metatarsal will not be able to plantarflex into the floor, increasing the load on the hallux. The typical wear pattern, therefore, will be under the hallux, second and third metatarsals and occasionally the fifth metatarsal head. There is usually a distinct lack of weight bearing under the first metatarsal head.18 (Fig. 5a) The callus pattern will also correspond to the insole wear patterns, although calluses are not consistently present (Fig. 5b).
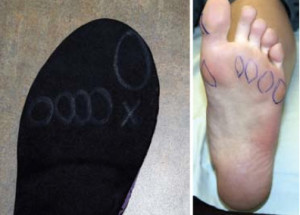
Figure 5A: Typical insole wear pattern with FnHL. Note the lack of weight bearing under the first metarsal head. B: Typical callus pattern seen with functional hallux limitus.
Shoe wear patterns are variable and tend to depend on the compensatory gait strategies that are employed, which have been described previously.5 Suffice it to say, at least for the purposes of this article, that the shoe wear patterns are so variable as to be poor predictors of FnHL. Abnormal gait patterns are epidemic in this patient population, however, and need to be addressed as part of a successful treatment protocol.
Hyperextension of the interphalangeal joint of the hallux may also be present, along with bunions, dorsal spurring on the first metatarsal head, hammertoes, lesser metatarsal pain and heel pain, along with all the supra-structural complaints typically seen by the over pronator. Cuboid syndrome is common in these patients, as a failure to engage the windlass mechanism does not allow the foot to stabilize into propulsion.19
How to fix functional hallux limitus:
Once you have made the diagnosis of FnHL, you will want to address this with your orthotic prescription.
Since this is an essential derangement of motion of the first MTP joint, conservative treatment is often successful and can be easily demonstrated in the foot assessment that will be described, and surgical treatment is rarely indicated. This is in contrast to structural hallux limitus (SHL), which often does require surgical treatment to restore painfree range of motion.21
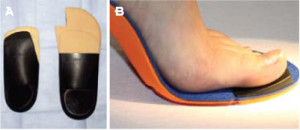
Figure 6. Orthotic options for FnHL. A: First ray cutout and a reverse Morton’s extension. B. Cluffy wedge under the hallux.
FnHL is usually a misalignment of the first MTP joint where the first metatarsal is dorsally displaced, prohibiting the normal excursion of the proximal phalanx around the first metatarsal head. Dorsiflexion of the first MTP joint involves a rolling motion for the first 34º, at which point plantar flexion of the first metatarsal is necessary for further dorsiflexion to occur.16 The rolling motion of the joint is often not restricted; rather the plantar flexion of the first metatarsal is restricted to allow further dorsiflexion to occur. This can readily be appreciated in the functional hallux limitus test.
Overcoming this problem with orthotic management will involve one of two different philosophies. The first is to put a cutout of some type under the first metatarsal head.22 This essentially creates a depression for the first metatarsal to fall into, theoretically enhancing first metatarsal plantar flexion. This is the correction offered in a reverse Morton’s extension, kinetic wedge or first ray cutout (Fig. 6a). The second philosophy applies a slight preload to the hallux in dorsiflexion and, by supporting the hallux in this position before the first metatarsal bears weight, allows any functional limitation of motion to be overcome (Fig. 6b).
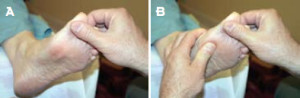
Figure 7. Pre-loading the hallux slightly (A) in a patient with FnHL will faciliate dorsiflexion when pressure is applied to the first metatarsal (B).
The rationale for the first ray cutout is not too hard to grasp. Allowing the first metatarsal to fall into the hole created in the insole will have the benefit of offloading the first metatarsal, essentially shifting the weight to the lateral metatarsals as the foot goes into propulsion. This type of accommodation also has the advantage of being easily applied to the insole. One of the potential problems with this approach, however, involves whether this will delay re-supination of the foot in propulsion. The first metatarsal must move below the level of the second metatarsal and bear weight, in order to initiate rearfoot supination and external leg rotation.23 If this is delayed as postulated with these modifications, the sequelae of this type of modification (which could involve excessive internal rotation of the lower limb in propulsion, resulting in decreased knee and hip extension, and postural problems in the lower back) certainly need to be considered.
Another potential problem with these modifications is that the medial arm of the supportive tripod of the foot is moved laterally, essentially allowing the foot to pronate further and later in midstance. This is one of the reasons that Brooks shoes pulled the kinetic wedge from its shoes in the 1980s.(personal comunication with Ray Fredericksen) Injuries were noted to be more frequent and the modification was discontinued after only a short time on the market.
Preloading the hallux
In order to understand the concept of preloading the hallux, we need to go back to the functional hallux limitus test. Remember that in a foot with FnHL, when the first metatarsal head is loaded, the first metatarsal will not plantarflex and hallux dorsiflexion will be restricted.
Overcoming this restriction is done in the following manner: Apply a slight dorsal displacement to the hallux before loading the first metatarsal head (Fig. 7a), then attempt dorsiflexion of the hallux and you will readily appreciate that dorsiflexion is now no longer restricted (Fig. 7b). The toe can be brought into full extension and the full stabilizing effects of the windlass mechanism can be appreciated.
With a little practice, this test can be performed in a matter of a few seconds. The patient will note a definite and noticeable difference in the range of motion of the joint and will be quite surprised to feel the dramatic change. This can be performed at the same time as the functional hallux limitus test.
Elevating the hallux slightly allows the first metatarsal to bear weight as dorsiflexion occurs and therefore allows appropriate and physiological off weighting of the lesser metatarsals. As the first metatarsal bears more weight, re-supination of the rearfoot can occur in a normal fashion.20,24 Fredericksen noted in his article that heel pressures were decreased in midstance and that there was a faster progression of the foot into propulsion. Forefoot pressures showed a tendency towards first metatarsal weight bearing and less weight on metatarsals 2, 3 and 4, and a medialization of the trajectory of force through the first ray.
Elevating the hallux does have one disadvantage, which is that it cannot be used in shoes with limited toe box height, such as dress shoes and some ladies’ flats. Otherwise, elevating the hallux is well tolerated and has the advantage of being easily applied to sandals and open-toed shoes that are not capable of supporting conventional orthotic insoles.
FnHL is a common problem causing pronation of the foot at point in the gait cycle when the foot should be quite stable, and could potentially be responsible for a host of problems. These include hallux rigidus, bunion deformity, metatarsal overload, plantar fasciitis, achillodynia, as well as all the problems typically seen with over pronators.
Identification and treatment of this disorder is simple and should be part of the protocol of all individuals addressing mechanical pathology of the human foot.
James Clough, DPM is an ABPS board certified podiatrist at the Foot and Ankle Clinic of Montana. He is the inventor of the Cluffy Wedge.
References
1. Dananberg HJ. Gait style as an etiology to chronic postural pain. Part 1. Functional hallux limitus. J Am Podiatr Med Assoc 1993;83(8):433-441.
2. Payne C, Chuter V, Miller K. Sensitivity and specificity of the functional hallux limitus test to predict foot function. J Am Podiatr Med Assoc 2002;92(5):269-271.
3. Hicks JH. The mechanics of the foot. II. The plantar aponeurosis and the arch. J Anat 1954;88(1):25-30.
4. Bojsen-Moller F. Calcaneocuboid joint and stability of the longitudinal arch of the foot at high and low gear push off. J Anat 1979;129(Pt 1):165-176.
5. Dananberg HJ. Sagittal plane biomechanics. In: Subotnick SI, ed. Sports Medicine of the Lower Extremity. New York: Churchill Livingstone;1999:137-156.
6. Mcpoil T, Cornwall MW. Relationship between neutral subtalar joint position and pattern of rearfoot motion during walking. Foot Ankle Int 1994;15(3):141-145.
7. Novick A, Kelley DL, Birke JA, GillisW. Frontal plane moment changes about the rearfoot with orthotic intervention. Physical Ther 1992;72:S78.
8. Nawoczenski DA, Cook TM, Saltzman CL. The effect of foot orthotics on three-dimensional kinematics of the leg and rearfoot during running. J Orthop Sports Phys Ther 1995;21(6):317-327.
9. McCulloch MU, Brunt D, Van der Linden D. The effect of foot orthotics and gait velocity on lower limb kinematics and temporal events of stance. J Orthop Sports Phys Ther 1993;17(1):2-10.
10. Stacoff A, Reinschmidt C, Nigg BM, et al. Effects of foot orthoses on skeletal motion during running. Clin Biomech 2000;15(1):54-64.
11. Nigg BM, Stergiou P, Cole G, et al. Effect of shoe inserts on kinematics, center of pressure and leg joint moments during running. Med Sci Sports Exerc 2003;35(2):314-319.
12. Genova JM, Gross MT. Effect of foot orthotics on calcaneal eversion during standing and treadmill walking for subjects with abnormal pronation. J Orthop Sports Phys Ther 2000;30(11):664-675.
13. Mundermann A, Nigg BM, Humble RN, Stefanyshyn DJ. Foot orthotics affect lower extremity kinematics and kinetics during running. Clin Biomech 2003;18(3):254-262.
14. Eng J, Pierrynowski MR. The effect of soft foot orthotics on three-dimensional lower-limb kinematics during walking and running. Phys Ther 1994;74(9):836-844.
15. Stacoff A, Reinschmidt C, Nigg BM, et al. Effects of foot orthoses on skeletal motion during running. Clin Biomech 2000;15(1):54-64.
16. Hetherington VJ, Carnett J, Patterson BA. Motion of the first metatarsophalangeal joint. J Foot Surg 1989;28(1):13-19.
17. Shereff MJ, Bejjani FJ, Kummer FJ. Kinematics of the first metatarsophalangeal joint. J Bone Joint Surg Am 1986;68(3):392-398.
18.Van Gheluwe B, Dananberg HJ, Hagman F, Vanstaen K. Effects of hallux limitus on plantar foot pressure and foot kinematics during walking. J Am Podiatr Med Assoc 2006;96(5):428-436.
19. Bojsen-Moller F. Calcaneocuboid joint and stability of the longitudinal arch of the foot at high and low gear push off. J Anat 1979;129(Pt 1):165-176.
20. Clough JG. Functional hallux limitus and lesser-metatarsal overload. J Am Podiatr Med Assoc 2005;95(6):593-601.
21. Flavin R, Halpin T, O’Sullivan R, et al. A finite–element analysis study of the metatarsophalangeal joint of the hallux rigidus. J Bone Joint Surg Br 2008;90(10):1334-1340.
22. Kilmartin TE, Wallace WA, Hill TW. Orthotic effect on metatarsophalangeal joint extension. J Am Podiatr Med Assoc 1991;81(8):414-417.
23. Root ML, Orien WP, Weed JH. Normal and abnormal function of the foot, Vol II. Los Angeles: Clinical Biomechanics Corporation, 1977.
24. Fredericksen R, Cheskin M. Wedge brings new angle to treating hallux limitus. Biomechanics 2008;15(5):57-62.










Great post. I was checking continuously this blog and I’m impressed! Extremely helpful info particularly the last part 🙂 I care for such info much. I was seeking this certain info for a long time. Thank you and good luck.
This forefoot blockade is a significant preexisting and perpetuating factors for so many MSK conditions including CAD injury, TMJ, low bakc pain, knee pain and the list goes on. There is a taping procedure that can help in determining the help an orthotic will provide.
Very insightful article. We use a first ray cut out for flexible flatfoot and hallux limitus
Hello was just trying to establish what are symptoms of structural hallux limitus and how it presents itself, also what is the management plan
Many thanks
Hello, I’m enquiring what the clinical differences between functional hallux limitus and structural hallux limitus and what diagnostic test is best for shl, does shl progress to fhl
Many thanks