Photo courtesy of Sechrist Industries.
Recent analyses cautiously recommend the short-term adjunctive use of hyperbaric oxygen therapy (HBOT) for diabetic foot ulcer healing under certain conditions, but in the absence of high-quality clinical trials, experts continue to debate the controversial therapy’s benefits.
By Hank Black
The rationale for including hyperbaric oxygen therapy (HBOT) as an adjunctive therapy for diabetic foot ulcers may be a little clearer following developments in recent months, but controversy over its use shows no sign of going away soon.
Proponents of HBOT for diabetic foot ulcers are bolstered by a literature review from the Undersea & Hyperbaric Medical Society (UHMS) that found sufficient evidence to recommend its use in severe wounds and issue the group’s first clinical practice guidelines for use of the therapy for diabetic foot ulcers.1 And, in June, an updated Cochrane review of randomized controlled trials (RCTs) reached a cautiously optimistic conclusion about the treatment’s short-term benefits.2
However, contradictory conclusions from other reviews have continued to muddy the HBOT waters: The Ontario Health Technology Advisory Committee (OHTAC) in August recommended against expanding public funding for the treatments,3 and a month later, the International Working Group on the Diabetic Foot (IWGDF) published a systematic review that concluded lower limb practitioners should consider using the treatment for that indication, though they described the strength of that recommendation as weak.4
Hyperbaric oxygen treatments involve delivering near 100% oxygen to a patient in a hyperbaric chamber at typically 2 to 2.5 atmospheres for 90 to 120 minutes once or twice daily for 15 to 30 treatments.2 Some elements of healing are very oxygen-dependent, and HBOT delivers an increased partial pressure of oxygen to the tissues.5
Better studies needed
The source of the disagreements about HBOT is acknowledged by what has become a standard disclaimer in most analyses: Recommendations are difficult to make because controlled studies remain few and continue to be of poor methodological quality, primarily with regard to the size and heterogeneity of the populations studied. All parties call for more definitive studies to tease out the answers to primary questions.
Enoch Huang, MD, coauthor of the UHMS review and clinical practice guidelines, said the preponderance of research on HBOT for diabetic foot ulcers is positive, on balance, even if it’s not robust.
“The literature provides enough objective data that we know HBOT works,” Huang said. “But the question is who does it work best for? That’s what we need to focus on: How do we effectively use the technology to treat the right patient at the right time?”
Huang is the medical director of wound healing and hyperbaric medicine at Adventist Medical Center in Portland, OR, where he utilizes a three-chamber hyperbaric facility that treats four to eight patients every weekday. He also is president of the UHMS.
He, like others, found that the “right patient” is difficult to define. The authors’ final analysis included five RCTs and five observational studies.
“We could not pool every study because of the heterogeneity of the patient populations enrolled. The only common factor we could use to select studies was by wound severity and whether the wound was acute postoperative or nonhealing after thirty days or more of care. We used the Wagner wound classification scale,6 which is not perfect, but no other system of wound categorization provided a basis for a prospective comparative study,” Huang said.
The “right time” to treat a patient is also complicated, he said.
“We have been pushed by recent practice patterns to wait thirty days before starting HBOT. Our analysis determined HBOT helped healing but did not necessarily decrease the amputation rate. But, if we eliminated the waiting period to narrow the timeframe between when someone comes in with a bad foot and when HBOT is started, we saw a decrease in the amputation rate.”
The UHMS selected four clinical questions for review of the role of HBOT in diabetic foot ulcers:
- Is HBOT with standard care more effective than standard wound care alone?
- Is it more effective in a patient with a Wagner Grade 2 (ulcer penetrating deeper than superficial layers but without abscess or osteomyelitis) or lower wound than standard care alone?
- How about a patient with a Wagner Grade 3 ulcer (deeper than superficial, with abscess or osteomyelitis)?
- And what about the patient with an ulcer of Wagner Grade 3 or higher who has just had a surgical debridement of the foot?
Critical outcomes for the review included major amputation and incomplete healing at one year.
The questions resulted in three recommendations:
- No HBOT in patients with diabetic foot ulcers of Wagner Grade 2 or lower (very low evidence supporting HBOT).
- Add HBOT to standard of care in patients with Wagner Grade 3 or higher wounds (moderate level of evidence supporting HBOT).
- Add HBOT in patients with Wagner Grade 3 or higher wounds who have just undergone debridement of an infected foot (moderate level of evidence supporting HBOT).
“It’s very expensive to conduct a RCT for hyperbaric oxygen treatment of diabetic foot wounds, especially with enrollment numbers that will make a difference,” Huang said. “However, the UHMS would be glad to coordinate multicenter trials and unification of
protocols.”
The Cochrane review published this year included an analysis of 10 RCTs with a total of 531 participants with diabetic foot ulcers, up from eight trials and 455 participants in its 2012 review.7 Analysis of data obtained from pooling five trials with 205 participants showed an improvement in ulcer healing rates with HBOT at six weeks (RR 2.35; 95% CI 1.19 to 4.62; p = .01), a benefit not found at one-year follow-up. No significant difference was found in major amputation rates in five pooled trials with 312 people enrolled (RR 0.36; 95% CI .11 to 1.18).
The Cochrane and UHMS reviews have been welcomed by those who were discomfited by the 2013 publication in Diabetes Care of a large observational study by Margolis et al that found HBOT did not improve ulcer healing or reduce amputations compared with no HBOT.8 Critics of that study have averred that many confounding factors may have led to selection bias: the majority of patients had less severe ulcers (Wagner Grade 2); follow-up was limited to 16 weeks; the proportion of those completing all hyperbaric treatment sessions is unknown; and it is not clear whether all patients had achieved optimal limb perfusion prior to receiving HBOT.9 The observational study was large (6259 patients with nonischemic diabetic foot ulcers), but its critics point out that it was based on retrospective data from one large, for-profit wound management company.
The shift of most HBOT care for diabetic foot ulcers to outpatient facilities, Huang said, is because the Centers for Medicare and Medicaid Services (CMS) mandates a 30-day period of standard wound care with no measurable signs of healing after diagnosis of a Wagner Grade 3 wound or higher before it will reimburse for the treatment (plus standard care),10 effectively leaving inpatient treatments to be bundled with other charges.
Wound classification
Michael B. Strauss, MD, an orthopedic surgeon at Long Beach Memorial Hospital in California and a coauthor of the UHMS practice guidelines, said the Wagner system should be replaced. Although the system is often used to grade wound severity in HBOT studies, he said, many practitioners and healthcare organizations find it archaic and some use other classification systems that provide more clinical information.11,12
Strauss said that hyperbaric treatments should be restricted to hospitalized patients, and that outpatient HBOT should only be used for those patients’ continuity of care.13
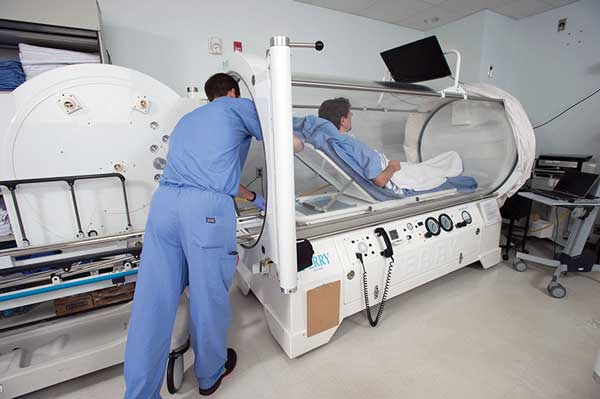
The Department of Plastic Surgery at MedStar Georgetown University Hospital in Washington DC has a four-chamber hyperbaric oxygen facility. (Photo courtesy of MedStar Georgetown University Hospital.)
Predicting which diabetic foot ulcers will heal with HBOT is an unresolved issue. Proper patient selection is mainly based on the severity of wound ischemia, and Löndahl et al found that baseline transcutaneous oxygen pressure correlates with response to treatment.14 Fluorescence angiography is another predictive technology under investigation. The real-time imaging tool is based on use of the short-lived fluorescence agent indocyanine green that absorbs light in the near-infrared spectrum. Huang said his group is performing microvascular perfusion studies using fluorescence angiography, and Georgetown University is designing a study to see whether that technology can help determine when vascularity has improved to the point that HBOT can be discontinued.
“We do need more evidence for diabetic foot ulcer treatment with HBOT; however, what we have is promising, and we plan to be contributing to the research effort,” said Kelly Johnson-Arbor, MD, medical director of MedStar Georgetown University Hospital Department of Plastic Surgery’s four-chamber hyperbaric oxygen facility in Washington, DC.
Potential for abuse
The trend of conducting outpatient HBOT in wound care facilities is also thought to have increased and worsened abuse of the system, according to Phi-Nga Jeannie Le, MD, a hyperbaric and emergency medicine physician in Houston, TX. Le assisted the federal government in its successful prosecution of principals of a HBOT company for conspiracy to commit healthcare fraud, which included double billing. The parties pleaded guilty to the charges and in 2014 were sentenced to five years in prison and ordered to pay millions of dollars in restitution.15 And, as recently as September 30, a federal district judge in Florida unsealed a False Claims Act suit involving HBOT against one of the nation’s largest wound care companies.16
Le, who practices emergency and hyperbaric medicine at multiple hospitals in Houston, TX, recently analyzed several healthcare fraud cases that have involved inappropriate use and documentation issues at facilities conducting hyperbaric oxygen treatments.17 She said that, for a relatively new specialty and the comparative number of patients who receive HBOT yearly, the industry is seen by the federal government and prosecutors as having a high rate of healthcare fraud.
“Lack of self-policing and poor uniform adherence to standards in the field have enabled corporations and individuals to be tempted to find an alternative way to bill for HBOT or gain reimbursement in improper ways,” Le said. “Hyperbaric medicine centers, individual physicians, hospitals, and other entities that administer HBOT appropriately are tainted by the fraud and disreputable activities that have stigmatized an entire industry.”
She also said HBOT introductory courses conducted by wound management companies and marketed to physicians as training programs have led to the misrepresentation of so-called “certification” and qualifications of physicians in hyperbaric medicine. The courses, she said, make physicians vulnerable to conflicts of interest and to coercion.
“Physicians who only undergo a forty-hour introductory course in HBOT sponsored by private, for-profit companies, thinking that this is all they need to become qualified to practice, are ill-equipped to present themselves as hyperbaric medicine specialists,” Le said.
A patient-centric role
David G. Armstrong, DPM, MD, PhD, professor of surgery and codirector of the Southern Arizona Limb Salvage Alliance (SALSA) at the University of Arizona College of Medicine in Tucson, said HBOT has a role in treating diabetic ulcers.
“Yet, I don’t think that place is for but a fraction of the millions of diabetic wound patients around the world,” Armstrong said. “I believe our really progressive colleagues operating HBOT-centric wound healing centers are now converting those into patient-centric wound healing, reconstruction, and risk-reduction units that may also include HBOT. That would help move us from volume-based to value-based care.”
Armstrong also is concerned about the amount of time patients must devote to the treatment.
“Going into a hyperbaric chamber for sixty to ninety minutes a day for a month or two is really hard on patients–regardless of which movie is playing on the DVD,” he said. “We need to think hard about the patient-centric aspects of this care and continue to try to
improve it.”
Those treatment sessions may be put to good use: Johnson-Arbor said she is preparing a study to determine if delivering focused diabetes education to patients during the in-chamber treatment period can result in improved blood sugar control.
In Ontario, as noted above, the OHTAC recently recommended against expanding the use of public funding for HBOT in the treatment of diabetic ulcers of the lower limb.3 Its report to the Ontario Ministry of Health and Long-Term Care was based on findings from three studies. One is a 2013 Mayo Proceedings systematic review that concluded HBOT improves healing rates and reduces lower extremity amputations in patients with diabetes compared with no HBOT.18 The other two–a systematic review published in 201319 and a clinical trial20 developed from that review–originated from the Programs for Assessment of Technology in Health (PATH) Research Institute at St. Joseph’s Healthcare Hamilton in Ontario.
PATH’s literature review concluded HBOT might reduce risk of major amputation, but the effect was not statistically significant in a pooled analysis of six RCTs. Results of the PATH RCT have been submitted for publication, according to Daria O’Reilly, MD, MSc, associate professor of clinical epidemiology and biostatistics at McMaster University in Ontario and chair of the study.
The 103-patient trial found no significant difference in the rates of healing and major amputation between patients with diabetic ulcers randomized to HBOT and those randomized to sham treatment. Public comment on the OHTAC recommendations closed on October 15.
So the push-and-pull over HBOT continues. In September, a panel of the International Working Group on the Diabetic Foot (IWGDF) recommended that practitioners should consider the use of systemic HBOT for diabetic foot ulcers. The group’s 2012 review21 had provided some evidence to suggest that HBOT may reduce the rate of major amputation. In its latest review, which included three small nonblinded RCTs22-24 and the observational study by Margolis et al,8 the panel of experts on wound healing found little high-quality evidence to add to the discussion.
The organization echoed the many calls from practitioners and researchers for more high-quality RCTs to confirm the treatment’s cost-effectiveness and to identify the population most likely to benefit from its use.
Georgetown University’s Christopher Attinger, MD, interim chair of the Department of Plastic Surgery and a member of the IWGDF panel, said, “Much like the IWGDF, I am not sure of the role of hyperbaric oxygen in the diabetic foot.”
Trials in the pipeline
The HBOT community can look forward to results from at least two multicenter RCTs in the near future, although they will study different populations and thus not by themselves resolve the heterogeneity issue that has made data comparison and pooling a challenge. One is PATH’s unpublished study, which enrolled patients without large vessel disease who are not candidates for revascularization. The other is the Dutch DAMOCLES (Does Applying More Oxygen Cure Lower Extremity Sores) trial, which will study HBOT’s ability to increase wound healing and prevent amputations in patients with ischemic diabetic ulcers, as well as whether the treatment is cost-effective.25 The rationale for DAMOCLES came from a 2014 systematic review conducted by the researchers, which found some evidence of the effectiveness of HBOT for this population.9
“DAMOCLES definitely has the potential to emphatically cement the place of HBOT in the treatment of diabetic ulcer,” said Michael H. Bennett, MD, a coauthor of the recent Cochrane review and head of the Diving and Hyperbaric Medicine Research Program at the Prince of Wales Clinical School in Randwick, Australia. “I am not aware of any major methodological flaws. It’s a large trial and will have good power to more accurately determine the true impact of HBOT on these patients.”
Bennett said he is encouraged to see the cost-effectiveness analysis included in the study plan, as few previous studies have done. Two commonly cited studies found the cost of HBOT was more than offset by reductions in other costs, such as office visits, dressings, and major amputations.26,27
Another Cochrane author, Peter Kranke, MD, MBA, professor in the Department of Anesthesia and Critical Care at University Hospitals of Wuerzburg in Germany, seemed less sure.
“I am a bit pessimistic that new and much better evidence will come up in the near future,” Kranke said.
Hank Black is a freelance writer in Birmingham, AL.
- Huang ET, Mansouri J, Murad MH, et al. A clinical practice guideline for the use of hyperbaric oxygen therapy in the treatment of diabetic foot ulcers; UHMS CPG Oversight Committee. Undersea Hyperb Med 2015;42(3):205-247.
- Kranke P, Bennett MH, Martyn-St. James M, et al. Hyperbaric oxygen therapy for chronic wounds. Cochrane Database Sys Rev 2015;6:CD004123.
- Hyperbaric oxygen therapy for non-healing ulcers in diabetes mellitus. Health Quality Ontario website. http://www.hqontario.ca/Evidence/Publications-and-OHTAC-Recommendations/Ontario-Health-Technology-Assessment-Series/Hyperbaric-Oxygen-Therapy-for-Non-Healing-Ulcers-in-Diabetes-Mellitus. Accessed October 30, 2015.
- Bakker K, Apelqvist J, Lipsky BA, et al. The International Working Group on the Diabetic Foot (IWGDF). The IWGDF guidance on the management and prevention of foot problems in diabetes 2015: Wound Healing. IWGDF website. http://www.iwgdf.org/files/2015/website_development.pdf. Published September 16, 2015. Accessed October 30, 2015.
- Barnes RC. Point: Hyperbaric oxygen is beneficial for diabetic foot wounds. Clin Infec Dis 2006;43(2):18-92.
- Wagner F. The dysvascular foot: a system for diagnosis and treatment. Foot Ankle 1981;2(2):64-122.
- Kranke P, Bennett MH, Martyn-St. James M, et al. Hyperbaric oxygen therapy for chronic wounds. Cochrane Database Syst Rev 2012;4:CD004123.
- Margolis DJ, Gupta J, Hoffstad O, et al. Lack of effectiveness of hyperbaric oxygen therapy for the treatment of diabetic foot ulcer and the prevention of amputation. A cohort study. Diabetes Care 2013;36(7):1961-1966.
- Stoekenbroek RM, Ubbink DT, Koelemay MJW. Hyperbaric oxygen for the treatment of diabetic foot ulcers: A systematic review. See comment in PubMed Commons belowEur J Vasc Endovasc Surg 2014;47(6):647-655.
- National Coverage Determination (NCD) for Hyperbaric Oxygen Therapy (20.29). CMS.gov website. https://www.cms.gov/medicare-coverage-database/details/ncd-details.aspx?NCDId=12&ncdver=3&NCAId=37&NcaName=Hyperbaric+Oxygen+Therapy+for+Hypoxic+Wounds+and+Diabetic+Wounds+of+the+Lower+Extremities&IsPopup=y&bc=AAAAAAAAIAAA&. Accessed October 30, 2015.
- Lipsky BA, Berendt AR. Hyperbaric oxygen therapy for diabetic foot wounds: Has hope hurdled hype? Diabetes Care 2010;33(5):1143-1145.
- Strauss MB, Lew DC, Miller SS. The Wagner Wound Grading System: What is it? What are its ramifications for hyperbaric medicine? Wound Care Hyperbar Med 2012;4(4):38-44.
- Strauss MB, Miller SS, Aksenov IV. Making the scoring of wounds objective: Adding rhyme and reason to wound evaluation and management. Wound Care Hyperbar Med 2012;3(1):21-37.
- Löndahl M, Katzman P, Hammarlund C, et al. Relationship between ulcer healing after hyperbaric oxygen therapy and transcutaneous oximetry, toe blood pressure, and ankle-brachial index in patients with diabetes and chronic foot ulcers. Diabetologia 2011;54(1):65-68.
- United States of America v Stanley Thaw. US District Court for the Northern District of Texas. Case number 3:12-CR-00261-P(1). June 5, 2014. United States of America v Michael Kincaid. US District Court for the Northern District of Texas. Case number 3:12-CR-00261-P(2). June 5, 2014.
- US Ex Rel Arnold et al. v Healogics, Inc. US District Court for the Middle District of Florida. Case number 6:14-cv-01064.
- Le P-N J. Lessons to learn from federal convictions of HBOT fraud. Today’s Wound Clinic 2015;9(2):27-31.
- Liu R, Li L, Yang M, et al. Systematic review of the effectiveness of hyperbaric oxygenation therapy in the management of chronic diabetic foot ulcers. Mayo Clin Proc 2013;88(2);166-175.
- O’Reilly D, Pasricha A, Campbell KI, et al. Hyperbaric oxygen therapy for diabetic ulcers: a systematic review and meta-analysis. Int J Technol Assess Health Care 2013;29(3):269-281.
- O’Reilly D, Linden R, Fedorko L, et al. A prospective, double-blind, randomized, controlled clinical trial comparing standard wound care with adjunctive hyperbaric oxygen therapy (HBOT) to standard wound care only for the treatment of chronic, nonhealing ulcers of the lower limb in patients with diabetes mellitus: a study protocol. Trials 2011;12(1):69.
- Game FL, Hinchliffe RJ, Apelqvist J, et al. A systematic review of interventions to enhance the healing of chronic ulcers of the foot in diabetes. Diabetes Metab Res Rev 2012;28(Suppl 1):119-141.
- Khandelwal S, Chaudhary P, Poddar DD, et al. Comparative study of different options of grade III and IV diabetic foot ulcers to reduce the incidence of amputations. Clin Pract 2013;3:20-24.
- Ma L, Li P, Shi Z, et al. A prospective, randomized, controlled study of hyperbaric oxygen therapy: effects on healing and oxidative stress of ulcer tissue inpatients with a diabetic foot ulcer. Ostomy Wound Manage 2013;59(3):18-24.
- Wang CJ, Wu RW, Yang YJ. Treatment of diabetic foot ulcers: a comparative study of extracorporeal shockwave therapy and hyperbaric oxygen therapy. Diabetes Res Clin Pract 2011;92(2):187-193.
- Stoekenbroek RM, Santema TB, Koelemay MJW, et al. Is additional hyperbaric oxygen therapy cost-effective for treating ischemic diabetic ulcers? Study protocol for the Dutch DAMOCLES multicenter randomized clinical trial. J Diabetes 2015;7(1):125-132.
- Chuck AW, Hailey D, Jacobs P, et al. Cost effectiveness and budget impact of adjunctive hyperbaric oxygen therapy for diabetic foot ulcers. Int J Technol Assess Health Care 2008;24(2):178-183.
- Gomez-Castillo JD, Bennett MH. The cost of hyperbaric therapy at the Prince of Wales Hospital, Sydney. J South Pacific Underwater Med Society 2005;35(4):5.








