By Alex Kor, DPM, MS; Amy Young, OMS-III; Travis Montgomery, DPM
The canine-human relationship has changed over time, becoming increasingly more intimate. While many humans have enjoyed the increased companionship, sometimes, it hasn’t worked out as intended.
The pandemic has affected all of us – regardless of age, demographics, occupation, medical history, whatever measure you choose to use. Whether it was required work from home or shelter in place orders, or continuing work as a student or teacher virtually, we have all been confined in our homes more than ever before with minimal social encounters. Naturally, there are ramifications of such drastic changes to what was our normal routine and those changes can affect pets in the home, too.
At the start of the pandemic, in March 2020, there was an optimistic naivety that all would go away quickly and with that in mind, many individuals chose to adopt a new pet. Indeed, shelters were cleared of dogs and cats as we sought the companionship of 4-legged friends. But pets, particularly dogs, are attuned to the rhythms of the household and dramatic changes can affect their behavior as well as their humans. A recent article in the Journal of Pediatrics1 reported that since late March 2020, there has been a nearly “3-fold increase in rates of visits to the pediatric [Emergency Department, ED] because of dog bites.” During this same period, the author(s) have encountered another sequelae of the pandemic on patients who have neuropathy (decreased sensation) and who are dog owners. Although the adage, “A dog is a man’s best friend,” is true, these authors want to provide a warning for future dog-owners who may have decreased sensation to their feet.
Neuropathy, which can cause numbness, tingling, burning of the feet (and the hands), is typically the manifestation of many medical conditions such as diabetes, vitamin deficiency, heavy metal toxicity, radiculopathy, and even alcohol abuse. Patients with neuropathy often do not feel sharp pain in the affected extremity, even when there is trauma, such as a nail through the bottom of the shoe. These patients are discouraged from walking barefoot or using just socks, even when at home. Without proper protection, these patients are at risk of stepping on a foreign body (think small dog toy or loose screw) and receiving a puncture wound which results in a subsequent infection.
During natural disasters, including pandemics, social isolation is a common consequence. To quell the emptiness of being alone, dog adoption seems to be one remedy. In fact, a recent paper by Morgan et al2 found a substantial increase in the dog adoption rate during the pandemic in Israel. In addition, it was discovered that the more stringent the social restrictions during the COVID-19 pandemic in Israel, the number of potential adopters, as well as the dog adoption rate, increased significantly, while the dog abandonment was unchanged. A similar study in the United States by Bussolari et al3 in Animals interviewed 4,105 adults regarding their companion dogs during the initial months of the pandemic and found 76.8% believed that their dog helped them cope during the lockdown. In addition, their dog reduced stress and provided more positive than negative experiences. Thus, regardless of location, people have embraced the idea of adding a dog to their household.
Realizing that the experiences in Israel regarding dog adoption are likely common throughout the world, one must wonder if more people having dogs, and more people being isolated might have deleterious repercussions. At our county hospital in central Indiana where we have experienced one government-issued shelter-in-place since March 2020 through early April 2021, the podiatry service has treated 2 patients that both have diabetes and diabetic neuropathy and who had a portion of their foot and/or ankle apparently consumed by their domesticated dog. This paper presents these 2 case studies, and we believe it serves as a warning to future dog owners who have some form of neuropathy.
Case #1: 72-year-old male
This male patient lives alone and has a history of atrial fibrillation, GERD, heart failure, hyperlipidemia, hypertension, peripheral neuropathic pain, and poorly controlled Type 2 diabetes mellitus (most recent HBA1C: 9.2). Neuropathic wounds of both 1st metatarsal heads responded to traditional conservative measures in the summer of 2020. By mid-October 2020, both wounds had closed.
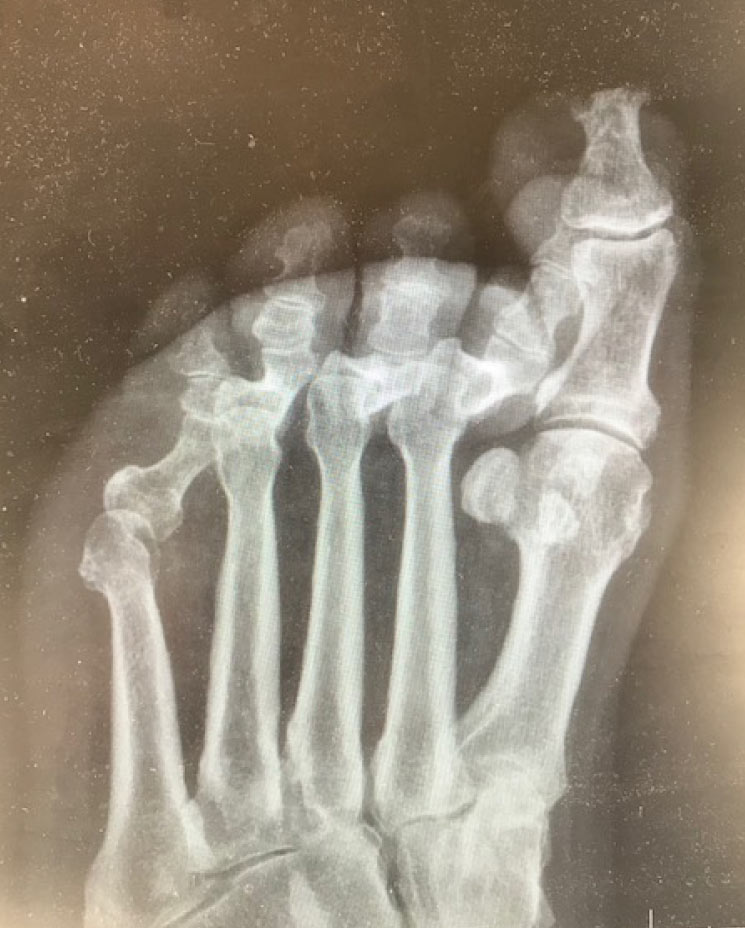
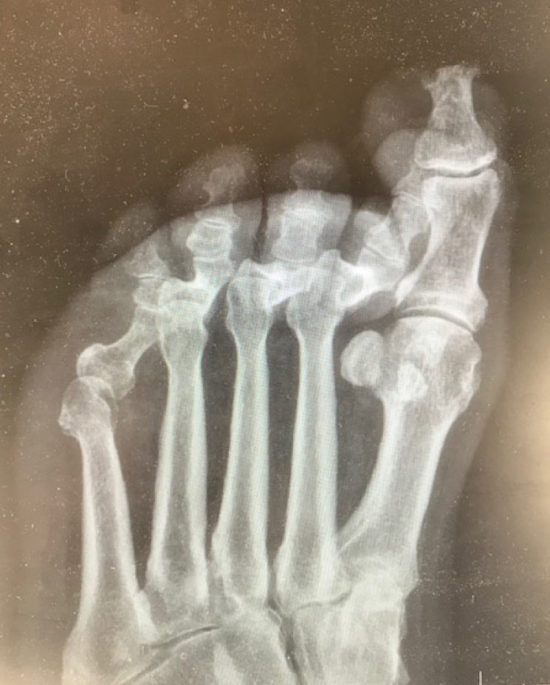
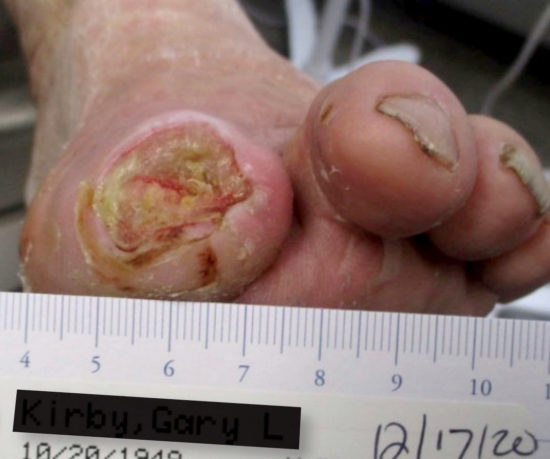
On 10/29/20, he presented to the Emergency Department (ED) for new wounds of both great toes. The patient related that the right great toe wound was from his new diabetic shoes. Regarding the wound on his left great toe, the patient suspected that his new puppy (a Jack Russell terrier puppy) “may have tried to bite his left great toe.” He related that he had noticed dried blood and scratches in the toe area. He acknowledged “not feeling his feet,” but denied any pain. After a thorough exam in the ED, he was discharged on oral antibiotics, given an urgent referral to return to the wound clinic, and was given these instructions: “Wear diabetic socks. Keep wound clean and covered. Do not wear the shoes that rub your right great toe. Make sure your puppy/dog does not chew on feet…”
Although this patient is reasonably compliant, his Jack Russell puppy did not heed the same advice. Two days later, on 10/31/2020, the patient again presented to the ED after noticing his puppy actively chewing on his left great toe. Cultures in the ED found Group C streptococcus from the dog bite wound. The patient reiterated in the ED that he has no sensation in his toes and was unsure of how long the puppy had been chewing on his toe. His physical exam demonstrated significant avulsion injury with a palpable bone at the tip of his left hallux and “no identifiable landmarks.” Once more, the patient did not endorse any pain at the time of exam despite the impressive open wound. His blood glucose was 398 and the team was concerned about blood flow to the foot. He was admitted to the hospital, started on IV clindamycin, and an urgent podiatry consult was submitted. Blood flow studies occurred 2 days later, after a bedside incision and drainage had been completed. Meanwhile, he was advised to give up the dog and did so.
On 11/03/2020, as a result of the injury, the patient underwent a partial amputation of the left hallux (the distal phalanx and a portion of the proximal phalanx). His intra-operative cultures found the following bacteria: Kluyvera intermedia, Enterococcus faecalis, and Methicillin-resistant Staphylococcus aureus. After discharge, he was closely followed by the wound clinic from mid-November through late January 2021. Treatment included a long course of IV antibiotics, debridement, dressing changes, and living skin equivalents. By late January, the residual wound had not closed, his wound grew Staphylococcus lugdunensis and it was determined that he had recurrent osteomyelitis. Subsequently, the patient was returned to the operating room on 02/05/2021 for a definitive resection of the remainder of his left hallux. As of mid-February 2021, the patient has home health dressing changes and is also seen as an out-patient by the wound clinic.
Case #2: 62-year-old female
This patient is a chronic smoker (1 ppd since age 16), who has a history of Type 2 diabetes with neuropathy, depression, hypertension, and hyperlipidemia. Patient lives alone with her pit bull terrier.* She had 2 previous dog bites of her right hand in 2017 and 2019 by a previous dog; both wounds required ED visits, and one required surgery by a hand surgeon and extended wound care with IV antibiotics. She initially presented to the wound clinic in August 2020 complaining of 2 painful venous stasis ulcers of her left ankle. Initial X rays in August 2020 identified “no acute or destructive bony process.” In-office cultures obtained during subsequent periodic debridements of the wounds revealed Enterobacter cloacoa, Enterococcus faecalis, and Haemophilus parainfluenzae. Despite taking appropriate oral antibiotics, getting a consult from interventional cardiology, offering home health, etc., patient’s left ankle wounds persisted. An MRI performed in October 2020 found evidence of osteomyelitis of her left medial malleolus and she was offered surgical intervention. The 2 options discussed were bone debridement of the medial malleolus and below-the-knee amputation. She elected to proceed with bone debridement and limb salvage.

Figure 3. Case #2. Early post-op image shows the left ankle appearing to heal; but this did not last.
On 10/22/2020, the patient was taken to the operating room for a surgical debridement of a portion of the left medial malleolus due to the sequelae of an infected venous stasis ulcer. Intra-operative cultures found Citrobacter freundii. Post-operatively the patient initially appeared to be doing well as the wound of the left ankle appeared to be slowly resolving. With frequent outpatient visits (every 3 days) to the wound clinic as well as the use of the KCI Wound Vac (KCI USA, San Antonio, TX), the wound healing appeared to show promise. However, by late November 2020, the wound had not closed, and all living skin equivalents suggested were not reimbursed by her insurance provider. Thus, another provider (author, TM) from the wound clinic offered to perform a muscle flap operation with bone graft. On 1/19/2021, the patient underwent a muscle flap procedure (reverse hemi soleus) with the placement of an external fixator.
On 1/29/2021, the patient was re-admitted to the hospital after being found unconscious by her family on the evening of 1/28/2021 on the floor of her home with the dog next to her. She had apparently collapsed. The patient recalls nothing, but the family member reported blood and feces throughout the home. Cultures of the wound done in the ED found Streptococcus viridans and Coagulase-negative staphylococci. In addition, her left ankle wound (at the site of the muscle flap) had been consumed and traumatized by the pit bull. When this provider (author, AK) examined the patient on the surgical floor after having received reports of her dog “gnawing away” at her recently placed muscle flap, the provider found extensive tendon injury, palpable bone exposure, and no pain. At that time, efforts were again directed to salvage the patient’s limb and a reverse soleal flap with external fixation was chosen for correction. After the procedure on 1/29/2021 the patient remained in the hospital assisted living facility with multiple providers attending her wound for approximately 19 days prior to discharge. She was advised multiple times to get rid of the dog, but she refused.
Discussion
There is no doubt that the 2 case studies illustrate a likely worst-case scenario of owning a dog if the owner lives alone and has neuropathy. Conversely, the authors recognize the known and well documented mental health and well-being benefits of having a dog.4 Since March 2020, due to the pandemic and subsequent lockdown, feelings of loneliness and isolation have dominated the psyche of all humans. Thus, it comes as no surprise that dog adoption has increased dramatically since the arrival of COVID-19.2
Writing as part of One Health, a program of the U.S. Centers for Disease Control that looks at the interconnection between people, animals, plants and their shared environments, Overgaaw and colleagues5 examined how the bond between humans and pets has evolved over time. The role of dogs in particular has changed—from hunting and herding to providing companionship. With this change, they write, humans have allowed their pets to get intimately closer such as sleeping in the same bed or licking the human’s face. As companions, the authors explain, dogs perceive their role as caretakers for humans, and just as they would lick the wounds of their young, they lick the wounds of their humans to show compassion. This is particularly true for young animals who are seeking approval but need to be properly trained to not lick or “chew.”
Despite the obvious loyalty demonstrated by dog owners that rely on their 4-legged friends for companionship, dogs have been known to not always share that same level of kinship. This, at times, translates into aggressive behavior (i.e., bites) by the domesticated dog against the owner and/ or familiar person. Writing in the Journal of Pediatrics, Children’s Hospital Colorado physicians reported their Emergency Department had seen nearly 3 times as many children with injuries from dog bites since the start of the pandemic lockdowns as they had the previous year.6 The cause, they note is multifactorial, but increased exposure is certainly key. Other possible reasons for increased dog aggression they wrote may include increased stress for dogs as the canines are able to perceive magnified household stress during the pandemic.
Infection and the possible loss of an appendage is the greatest threat to humans as a result of dog bites. Like any animal bite, dog bites tend to be polymicrobial (both aerobic and anaerobic), but the vast array of bacteria is limitless.7 The most common pathogens are Pasteurella multocida, Pasteurella canis, Neisseria, Cornebacterium, Staphlococcus, and Streptococcus spp, and the gram-negative rod Capnocytophaga canimorsus, as well as several anaerobes. The origin of the bacteria can be influenced by the flora of the biting animal, the bacteria of ingested prey, the victim’s own skin, and the physical environment of the area where the dog bite occurred.
Conclusion
In summary, the 2 cases should serve as a cautionary tale that patients with neuropathy need to operate at a higher level of awareness when owning pets than non-neuropathic patients. Studies do show that pit bulls are responsible for the majority of dog bites seen in emergency rooms, a fact that has been consistent for decades.8,9 Physicians may want to inquire of neuropathic patients what kinds of pets they have at home so they can provide appropriate advice. The authors also request that future dog owners be more selective of which breeds they buy, and that humane societies, pet stores, breeders, etc., be more selective in selling dogs and be more aware of possible dog aggression particularly against compromised populations.
Alex Kor, DPM, MS, is a clinical assistant professor at Marian University College of Osteopathic Medicine in Lebanon, Indiana. He is at past president of the American Academy of Podiatric Sports Medicine. Amy Young is a third-year osteopathic medical student. Travis Montgomery, DPM, FACFAS, AMOS, is a foot and ankle surgeon in private practice in Carmel, Indiana.
Breed-Specific Legislation Map
 BSL Census is a database of currently known cases of Breed Specific Legislation across the United States. Breed Specific Legislation (BSL) bans OR restricts certain types of dogs based on their appearance because they are perceived as “dangerous” breeds or types of dogs.
BSL Census is a database of currently known cases of Breed Specific Legislation across the United States. Breed Specific Legislation (BSL) bans OR restricts certain types of dogs based on their appearance because they are perceived as “dangerous” breeds or types of dogs.
Map is current as of 2019. https://bslcensus.com/
States in green signify that there is not BSL currently being enforced. This can either be due to state level legislation, or because there simply is no BSL in that state.
States in yellow signify locations where there is some sort of state level law that prohibits BSL from being enforced but there are cases that are being allowed due to either being grandfathered in or are part of a home-rule exemption due to the language of the legislation.
States in red signify that there is currently BSL being enforced and there is no state/province/territory level legislation that prohibits BSL.
- Dixon CA, Mistry RD. Dog Bites in Children Surge during Coronavirus Disease-2019: A Case for Enhanced Prevention. J Pediatr. 2020 Oct: 225: 231-232.
- Morgan, L. Protopopova, A., Birkler, R.I.D. et. Al. Human-dog relationships during the COVID-19 pandemic: booming dog adoption during social isolation. Humanit Soc Sci Commun . 2020. 7: 155, 1-11.
- Bussolari C, Currin-McCulloch J, Packman W, Kogan L, Edrman P. “I Couldn’t Have Asked for a Better Quarantine Partner!”: Experiences with Companion Dogs during Covid-19. Animals (Basel). 2021 Jan 28: 11 (2): 330.
- Ratschen E, Shoesmith E, Schabab L, Silva K, Kale D, Toner P, Reeve C, Mills DS. Human- animal relationships and interactions during the Covid-19 lockdown phase in the UK: Investigating links with mental health and loneliness. PLoS One. 2020 Sep 25:15(9) e0239397.
- Overgaauw PAM, Vinke CM, Hagen MAEV, Lipman LJA. A One Health Perspective on the human-companion animal relationship with emphasis on zoonotic aspects. Int J Environ Res Public Health. 2020 May 27;17(11):3789.
- Dixon CA, Mistry RD. Dog bites in children surge during coronavirus disease-2019: a case for enhanced prevention. J Pediatrics. 2020;225:231-232.
- Abrahamian FM, Goldstein EJ. Microbiology of animal bite wound infections. Clin Microbiol Rev. 2011 Apr: 24 (s): 231-46.
- Bailey CM, Hinchcliff KM, Moore Z, Pu LLQ. Dog bites in the United States from 1971 to 2018: a systematic review of the peer-reviewed literature. Plast Reconstr Surg. 2020 Nov;146(5):1166-1176.
- Brice J, Lindvall E, Hoekzema N, Husak L. Dogs and orthopaedic injuries: is there a correlation with breed? J Orthop Trauma. 2018 Sep;32(9):e372-e375.