 Arthrodesis remains effective for most patients with end-stage hallux rigidus, but finding an alternative that allows more range of motion can be challenging. Faced with disappointing arthroplasty outcomes, surgeons have had to get creative.
Arthrodesis remains effective for most patients with end-stage hallux rigidus, but finding an alternative that allows more range of motion can be challenging. Faced with disappointing arthroplasty outcomes, surgeons have had to get creative.
By Cary Groner
Given the advances in artificial replacement joints for the knee and hip, nobody sane would opt for joint fusion in those cases if they had a choice. But foot surgeons are faced with a more complicated decision process when dealing with hallux rigidus and the first metatarsophalangeal (MTP) joint of the foot.
Recent studies suggest that implants in that part of the body present a number of problems, but though joint fusion (arthrodesis) still works well for pain relief and general function, some patients want more range of motion (ROM) than arthrodesis offers. For those individuals, surgeons are developing techniques that rebuild the joint without fusing or replacing it.
So how does a surgeon—or a patient—choose? Comparisons can be difficult because outcomes depend to some degree on who performs the operation, and on what the patient wants.
“I’m not sure one procedure is better than the others,” said Paul Kim, DPM, MS, an associate professor of plastic surgery and the director of research at the Center for Wound Healing at Georgetown University School of Medicine in Washington, DC. “Ultimately, the patient just wants the pain to go away and to be able to function. If you get to that endpoint, you’ve won and so has the patient, regardless of the procedure you select.”
The nature of the beast

Preoperative (top, left and right) and postoperative (bottom, left and right) images of a 59-year-old man who underwent first MTP arthrodesis for end- stage hallux rigidus. (Images courtesy of Paul Kim, DPM, MS.)
Hallux rigidus is characterized by diminished ROM and progressive joint degeneration. It can result from traumatic injury; structural deformities, both congenital and acquired; biomechanical abnormalities; neuromuscular disorders; metabolic diseases; and iatrogenic causes. It is the most common form of foot osteoarthritis, affecting roughly 2.5% of the population. The condition leads to decreased dorsiflexion and articular impingement, which promotes osteophyte formation—which, in turn, further limits ROM.1
For milder cases, nonoperative treatment includes appropriate footwear and avoiding activities that aggravate the problem. In more serious cases, however, surgery is usually indicated, and breaks out into two broad categories: Joint salvage (for those with milder stage I and II disease) or joint destruction (stage III or IV).1
Salvage techniques include cheilectomy (resection of the dorsal osteophytic formation and the degenerative portion of the articular surface of the metatarsal), and metatarsal osteotomy (shortening and/or plantar flexion of the first metatarsal, done either distally or proximally, and usually in conjunction with cheilectomy).1
Joint destructive techniques include arthrodesis (with an optimal fused hallux position of 15° to 20° of dorsiflexion relative to the floor, 10° to 20° of valgus, and neutral rotation); resectional arthroplasty (to increase the space between the first metatarsal and the proximal phalanx); and total or partial implant arthroplasty.1
Kim was lead author of a 2012 retrospective review in the Journal of Foot and Ankle Surgery (JFAS) that compared outcomes for three procedures: arthrodesis, hemi-metallic joint implant, and resectional arthroplasty. After three years, the surgeries all appeared to be viable options for treating end-stage hallux rigidus.2 But all had issues: metatarsalgia occurred in 9.8% of arthrodesis patients, bony overgrowth into the joint occurred in 28.3% of the hemi-implant group, and 30.9% of patients experienced floating hallux after resectional arthroplasty. Moreover, particularly when it comes to implant procedures, some clinicians feel three years isn’t long enough to judge outcomes.
Personal preferences
As Kim noted, surgeon training and preference are key determinants of which procedures get done.
“I’m a proponent of two approaches,” he said. “In early stage disease, I do an aggressive cheilectomy to remove some of the dorsal head of the first metatarsal and the base of the proximal phalanx; that’s assuming that most of the pain is at the end of the dorsiflexion range of motion.”
Indeed, a systematic literature review published in JFAS in 2010 found that cheilectomy has a low incidence of revision surgery (8.8%) and should be considered a first-line approach in many patients.3 Revision rates were similarly positive when phalangeal dorsiflexory osteotomy supplemented the cheilectomy.4
In more serious cases, however, Kim chooses arthrodesis.
“Fusions are reliable, and patients do very well with them,” he said. “The only caveat is patient age, because as you get older your bone quality isn’t as good, and you have to have some expectation that the bone will heal.”
When he has such concerns, Kim sometimes opts for a modified Keller arthroplasty—excision of the proximal part of the phalanx.
Implants, both full and hemi, remain controversial in the clinical community. They are prone to loosening, and “silastic” models that include silicone have shown a tendency to degrade and provoke a systemic immune response. Nevertheless, some literature supports their use; one UK study of 108 feet reported good outcomes, in terms of the American Orthopaedic Foot and Ankle Society (AOFAS) scoring system and range of motion, at an average of 8.5 years.5 Studies from the Netherlands and the US, respectively, reported significant pain relief and good patient satisfaction.6,7
Other findings have been less positive. For example, a paper published in JFAS in 2010 reported that revision rates ran as high as 7%, and that arthrodesis offered better functional outcomes.8
Lowell Weil Jr, DPM, told LER that some problems have resulted from poor patient selection.
“Silastic implants were overutilized in the 1970s and 1980s,” he said. “They were used in situations that were not clinically appropriate—in hallux valgus [bunions] and in younger people—and as a result there were a lot of failures.”
Weil, president of the Weil Foot & Ankle Institute in Chicago, and team podiatrist of the White Sox, is nevertheless coauthor of one of the positive articles cited above and defends the use of silastic implants in the right patients.
“If you use them in an older, less active population with exclusive hallux rigidus and no transverse plane deformity, you can get really good results,” he said. “We’ve seen people with successful implants twenty-five to thirty years postoperatively—though when patients ask, I don’t tell them that; I tell them they’ll probably last about ten years.”
Weil added that the breakdown problems of earlier decades have been at least partially addressed by the addition of titanium grommets to the devices.
“The grommets create an interface between the bone and the silastic, so the bone edge won’t roughen and break down the implant prematurely,” he said.
Weil also noted that, contrary to conventional wisdom, revision surgery needn’t necessarily entail arthrodesis, which is difficult in such patients because so much bone has been removed to place the implant.
“We will use bone augmentation to fill the area, then put a new implant in,” he said. “It’s a much easier procedure for patients to recover from than an arthrodesis.”
White Sox vs Giants
Lawrence Oloff, DPM, who practices at Sports Orthopedic & Rehabilitation Medical Associates in Redwood City, CA, and is a team podiatrist for the San Francisco Giants, takes issue with much of this. Oloff graduated from podiatry school in 1976 and calls himself a “dinosaur”—though he thinks he’s learned from his mistakes and adapted. So far he’s avoided extinction.
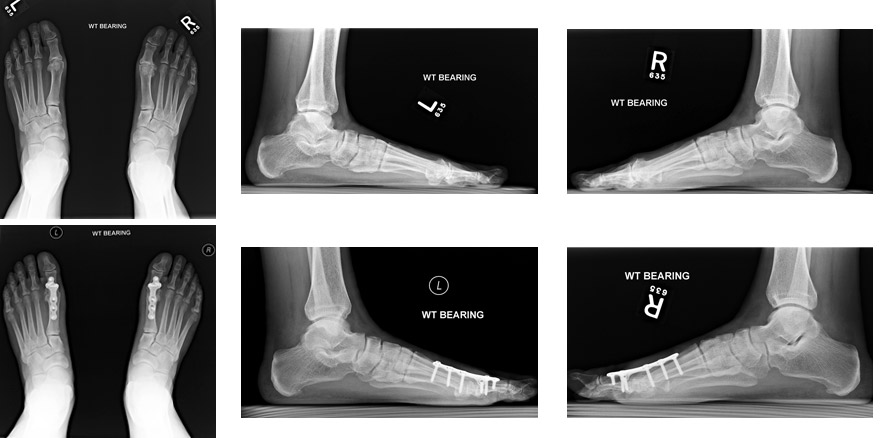
A 72-year-old man with pain in the right greater than left first MTP joint secondary to arthritis (hallus rigidus) for the past two years. He elected to undergo simultaneous bilateral first MTP arthrodeses and did well. Preoperative x-rays (top row) show significant narrowing and irregularity at the MTP joint space. Postoperative images (bottom row) were taken six months after surgery. (Images courtesy of James DeOrio, MD.)
“Back then, we did lots of implants, and the short-term benefit was wonderful,” he said. “But then you get older, and you have patients coming back with problems that are hard to fix. Over time, a silastic implant abrades and particles break off. The body reacts with synovitis, and as a result you lose bone. Then, revision surgery is complex, because you have to extract the implant and import bone for an arthrodesis.”
Oloff suspects that part of the reason implants fail is that they can’t yet account for the complex movements of the MTP joint.
“When the toe moves up, the metatarsal moves down to give more dorsiflexion motion,” he explained. “A hinged implant doesn’t allow for those joint mechanics to occur. We’ve gone from silastic to ultrahigh-molecular-weight polyethylene, to metals, to ceramics; everyone is trying to solve it from a biomaterial perspective, but it’s more complicated than that.”
Oloff is critical of companies that bring new products to market without what he considers adequate testing.
“Companies have an obligation to doctors and their patients to do intermediate and long-term testing, but they put implants out too soon,” he said. “The ceramics look good, but if you read the data, they are having loosening problems, intermediate-term failures, suffering some of the same issues [as earlier models].9 Implants should be for the long haul, not a short-term procedure.”
Other views
Eric Bluman, MD, PhD, an assistant professor of orthopedics at Harvard Medical School in Boston, suggested another reason artificial joints might not work as well in the foot as in other parts of the body.
“The knee and the hip joints are primarily axial weight-bearing,” he said. “The force vector runs directly down the axis of the bones, and the joint functions within that weight-bearing axis.”
The MTP joint, by contrast, is more of a hinge joint, in which weight doesn’t help compress an artificial device so that it stays in place.
Soft issue coverage of the hip and knee is also greater than at the toe joint, Bluman said, which may facilitate functional ROM.
Jeffrey Johnson, MD, associate professor of orthopedic surgery and chief of the Foot and Ankle Service at Barnes-Jewish Hospital at Washington University Medical Center in St. Louis, voiced other concerns.
“I don’t think anybody has shown that these expensive implants are worth it,” he said. “If you’re going to put one in, do you resurface the metatarsal head only? Or only the base of the proximal phalanx? Or both? Are you going to use carbon fiber? Metal? Plastic? I’m not sure anybody knows the answers to these questions.”
Johnson added that published results may be misleading.
“We don’t have long-term data, and we typically don’t have data from people who weren’t originators of the implant,” he said. “My experience is that implants don’t provide any greater range of motion or function than the other forms of arthroplasty or fusion, and they are often stiff.”
David Thordarson, MD, a professor of orthopedic surgery at Cedars-Sinai Medical Center in Los Angeles, acknowledged that, intuitively, an MTP joint implant should make sense.
“You have a bad joint; there’s a replacement we can do; let’s do it,” he said. “But I’ve taken out three hallux implants this month that were put in by other surgeons. Granted, if it’s successful, they don’t come to me to have it fixed. But even though it’s a highly polished metal surface, it’s nearly impossible to get it to match the other surface perfectly, so [patients] still hurt.”
Thordarson echoed Johnson’s concern about follow-up in published research.
“A lot of patients do fine even five years out, but once you get beyond that, these tend to quit functioning,” he said. “The issues are longevity and what the alternatives are, and in this case there are good alternatives to joint replacement.”
Doing no harm
From Larry Oloff’s perspective, it generally makes sense to minimize surgical impact now so that clinicians can avail themselves of better solutions when they become available later.
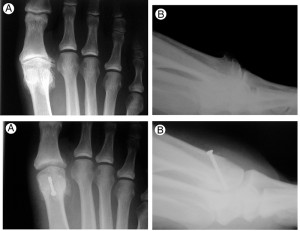
Radiographs show preoperative appearance (top row) and postoperative appearance (bottom row) of grade IV hallux rigidus. A = anteroposterior view, B = lateral view. (Images reprinted with permission from reference 10.)
“Can we do something to preserve the integrity of the joint and buy time, hoping that implants will improve in ten or fifteen years?” he asked. “I think decompressional osteotomy is a viable alternative.”
In such cases, Oloff starts with a cheilectomy to remove bone spurs, then shortens the metatarsal slightly to put slack in the joint for better range of motion.
“I’m high on osteotomy because we’re mainly a sports medicine group, so our patients are younger and active, and they want to get their activity back on track,” he said.
In a 2008 JFAS paper, Oloff reported that the procedure provided significant improvements in pain, ROM, and other measures in patients with grades III and IV hallux rigidus, and that overall patient satisfaction was more than 85%.10
Other research has been less positive. A systematic review of isolated periarticular osteotomy published in JFAS in 2010 reported that though peak dorsiflexion ROM increased, patient satisfaction was only about 73%. Due to these factors and complication risk, the author recommended that the procedure be performed with caution or not at all—another example of the extent to which experienced clinicians may nevertheless disagree.11
“Osteotomy has been developed on the spurious idea that it is necessary to treat a long and/or elevated first metatarsal relative to the second,” the author of that review, Thomas Roukis, DPM, PhD, told LER via email. Roukis practices in the Department of Orthopaedics, Podiatry and Sports Medicine at the Gundersen Lutheran Medical Center in La Crosse, WI; he is also president-elect of the American College of Foot and Ankle Surgeons.
“Shortening the first metatarsal clearly leads to additional problems, such as ‘transfer lesser metatarsalgia’ and medial arch collapse, that can be difficult to treat,” he continued. “As a result, I find no use for first metatarsal head osteotomies to treat hallux rigidus unless the patient has an associated increased one–two intermetatarsal angle.”
Eric Bluman usually opts for an arthrodesis, cheilectomy, or—he’s with Oloff on this—metatarsal osteotomy.
“It’s rare for me to do an arthroplasty of any type,” he said. “You get good functional outcomes from these other procedures without any of the drawbacks, so there has got to be a real necessity that your first MP joint remain mobile for me to consider it.”
There are such cases, however. For example, Bluman has had patients for whom yoga, Pilates, and similar practices requiring full joint ROM are very important.
“A fusion can really limit you in yoga,” he said. “Interpositional arthroplasty makes a lot of sense, but there’s still a risk of stiffness.”
Even so, Bluman admits to being leery even of hemiarthroplasties.
“There’s a hemi device that resurfaces the proximal portion of the phalanx, but most of the joint destruction—the cartilage damage and osteophyte formation—is found on the distal part of the metatarsal head,” he pointed out. “So doesn’t it make sense to replace the diseased part rather than leaving that and replacing another part of the joint?”
Fusion—hot or cold?
Although arthrodesis has been a successful procedure for a long time in terms of relieving pain and improving function, clinicians raise cases in which it may not be appropriate. Disadvantages include the possibility of poor union, interphalangeal (IP) joint arthritis, transfer metatarsalgia, and the loss of joint motion for more active patients.1
“Fusions perform very well, but they are finite and hard to reverse,” Oloff said. “Women may have trouble wearing heels, and hikers may find steep uphills harder. Force that used to get absorbed in one joint is now passed to the joints in front of and behind the MTP, so there is a higher incidence of IP joint arthritis.”
Oloff noted further that fusion closes the door on later joint replacement, should technology improve.
Still, people walk reasonably well and can even run on fused MTP joints. Some surgeons point out, not surprisingly, that success has a lot to do with technique. James DeOrio, MD, a consultant in orthopedic surgery at Duke University Medical Center in Durham, NC, emphasizes that surgeons match the titanium arthrodesis plate carefully to each patient, rather than relying solely on plate angle, to achieve the optimal 20° of dorsiflexion.12
“MTP fusion doesn’t consistently lead to midfoot arthritis,” DeOrio said. “It can happen, though—particularly at the IP joint—if you don’t put the toe in a good position.”
Jeffrey Johnson agreed.
“First MTP joint fusion is an excellent salvage procedure,” he said. “Patients can be really functional; I have a patient whose marathon times got better afterward.”
Johnson noted that in an optimal approach, the big toe is positioned so it doesn’t impede normal heel-to-toe gait; it has a little dorsiflexion, neutral rotation, and a little valgus.
“If you put it too straight, it doesn’t fit well in shoes, and patients feel like they are vaulting over the great toe,” he said. “They’re also more likely to get IP joint arthritis.”
The fixation method, not surprisingly, also affects success. In one study, a technique consisting of two crossed flexible titanium intramedullary nails and a dorsal 10-mm titanium staple resulted in no nonunions in 51 feet, whereas nonunion rates reported in other studies range up to 10%.13
Roukis, the lead author of that paper, believes surgeons should have a better idea of what degree of chondral damage they’re likely to encounter before they operate, and should choose procedures—joint sparing or destructive—accordingly. He has published a classification system that includes clinical and radiographic findings to help clarify the situation.14,15
Interpositional arthroplasty
Thordarson’s preference is interpositional arthroplasty. His approach is to detach the ligaments from around the end of the first metatarsal, then cut a little bone out of the joint and put the ligamentous tissue into it, to provide a cushion.
“The average patient ends up with about a half normal range of motion, but that still enables them to walk without a limp, lets a woman wear a two-inch heel, and takes the stress off the nearby joints, such as the big toe,” he said. “The bottom line is that it lasts forever, because it’s a living part of your body, in contrast to joint replacements.”
Thordarson has done more than 50 of the procedures, and said only two have failed. Those required arthrodesis, but, because the arthroplasty involved so little bone removal, the fusion still worked well. He noted that alternatives to using capsular tissue include allograft tendons and prepared commercial tissues. In 2009, he reported good maintenance of stability and alignment, and outcomes comparable to other forms of interpositional arthroplasty and arthrodesis.16
Jeffrey Johnson also favors interpositional arthroplasty.
“We do a traditional cheilectomy, then fold the dorsal capsule down and drape it over the top and end of the first metatarsal head to create a soft tissue interposition between the base of the phalanx and the metatarsal head,” he said. “To create the space, we do an oblique resection of the base of the phalanx so we retain the attachment of the short flexor muscles. That way, you retain the stability and flexion power of the toe.”
Johnson, too, has published promising results, and other studies support the potential of interpositional arthroplasty, particularly in young and active patients.17-22
Down the road
Despite professional disagreements about the relative value of different surgical procedures for hallux rigidus, it seems likely that arthrodesis will continue to play a significant role in the near future. It’s also probable that many clinicians will continue to do their best to preserve joints, due to both the promise inherent in interpositional arthroplasty and the hope that implant technology may someday surmount the limitations that still afflict it.
Cary Groner is a freelance writer in the San Francisco Bay Area.
1. Oloff L, Traynor C, Vartivarian S. Joint salvage techniques for stage III/IV hallus rigidus. In: Waddell J, ed. The Role of Osteotomy in the Correction of Congenital and Acquired Disorders of the Skeleton. InTech; 2012.
2. Kim PJ, Hatch D, Didomenico LA, et al. A multicenter retrospective review of outcomes for arthrodesis, hemi-metallic joint implant, and resectional arthroplasty in the surgical treatment of end-stage hallux rigidus. J Foot Ankle Surg 2012;51(1):50-56.
3. Roukis TS. The need for surgical revision after isolated cheilectomy for hallux rigidus: a systematic review. J Foot Ankle Surg 2010;49(5):465-470.
4. Roukis TS. Outcomes after cheilectomy with phalangeal dorsiflexory osteotomy for hallux rigidus: a systematic review. J Foot Ankle Surg 2010;49(5):479-487.
5. Morgan S, Ng A, Clough T. The long-term outcomes of silastic implant arthroplasty of the first metatarsal phalangeal joint: a retrospective analysis of one hundred and eight feet. Int Orthop 2012;36(9):1865-1869.
6. Ter Keurs EW, Wassink S, Burger BJ, Hubach PC. First metatarsophalangeal joint replacement: long-term results of a double stemmed flexible silicone prosthesis. Foot Ankle Surg 2011;17(4):224-227.
7. Sung W, Weil L Jr, Weil LS Sr, Stark T. Total first metatarsophalangeal joint implant arthroplasty: a 30 year retrospective. Clin Podiatr Med Surg 2011;28(4):755-761.
8. Brewster M. Does total joint replacement or arthrodesis of the first metatarsophalangeal joint yield better functional results? A systematic review of the literature. J Foot Ankle Surg 2010;49(6):546-552.
9. Dawson-Bowling S, Adimonye A, Cohen A, et al. MOJE ceramic metatarsophalangeal arthroplasty: disappointing clinical results at two to eight years. Foot Ankle Int 2012;33(7):560-564.
10. Oloff LM, Jhala-Patel G. A retrospective analysis of joint salvage procedures for grades III and IV hallux rigidus. J Foot Ankle Surg 2008;47(3):230-236.
11. Roukis TS. Clinical outcomes after isolated periarticular osteotomies of the first metatarsal for hallux rigidus: a systematic review. J Foot Ankle Surg 2010;49(6):553-560.
12. Leaseburg JT, DeOrio JK, Shapiro SA. Radiographic correlation of hallux MP fusion position and plate angle. Foot Ankle Int 2009;30(9):873-876.
13. Roukis TS, Meusnier T, Augoyard M. Nonunion rate of first metatarsal-phalangeal joint arthrodesis for end-stage hallux rigidus with crossed titanium flexible intramedullary nails and dorsal static staple with immediate weight-bearing. J Foot Ankle Surg 2012;51(3):308-311.
14. Roukis TS, Jacobs PM, Dawson DM, et al. A prospective comparison of clinical, radiographic, and intraoperative features of hallux rigidus. J Foot Ankle Surg 2002;41(2):76-77.
15. Roukis TS, Jacobs PM, Dawson DM, et al. A prospective comparison of clinical, radiographic, and intraoperative features of hallux rigidus: short-term follow-up and analysis. J Foot Ankle Surg 2002;41(3):158-165.
16. Hahn MP, Gerhardt N, Thordarson DB. Medial capsular interpositional arthroplasty for severe hallux rigidus. Foot Ankle Int 2009;30(6):494-499.
17. Mackey RB, Thomson AB, Kwon O, et al. The modified oblique Keller capsular interpositional arthroplasty for hallux rigidus. J Bone Joint Surg Am 2010;92(10):1938-1946.
18. Berlet GC, Hyer CF, Lee TH, et al. Interpositional arthroplasty of the first MTP joint using a regenerative tissue matrix for the treatment of advanced hallux rigidus. Foot Ankle Int 2008;29(1):10-21.
19. Hyer CF, Granata JD, Berlet GC, Lee TH. Interpositional arthroplasty of the first metatarsophalangeal joint using a regenerative tissue matrix for the treatment of advanced hallux rigidus: 5-year case-series follow-up. Foot Ankle Spec 2012;5(4):249-252.
20. Roukis TS. Outcomes following autogenous soft tissue interpositional arthroplasty for end-stage hallux rigidus: a systematic review. J Foot Ankle Surg 2010;49(5):475-478.
21. Roukis TS, Landsman AS, Ringstrom JB, et al. Distally based capsule-periosteum interpositional arthroplasty for hallux rigidus. Indications, operative technique, and short-term follow-up. J Am Podiatr Med Assoc 2003;93(5):349-366.
22. DelaCruz EL, Johnson AR, Clair BL. First metatarsophalangeal joint interpositional arthroplasty using a meniscus allograft for the treatment of advanced hallux rigidus: surgical technique and short-term results. Foot Ankle Spec 2011;4(3):157-164.









I have been performing a modification of the Waterman first metatarsal head osteotomy for about twenty years. I clean up the first MPJ damage and then perform a dorsal wedge based osteotomy so the head of the first metatarsal is tilted back. Fixation is from the damaged subchondral bone into the shaft with a screw. The patients typically go from severe limited motion to about 75-90 degrees of dorsiflexion intraoperatably. This procedure decompresses the joint as well and I have seen patients 13 years after performing and they were doing well still.
Brian Gale, DPM, FACFAS
I see quite a lot of H.R. in my orthotic clinic. Many of them surgical failures (definition= 1st ray H.R.+ pain after surgery) and many other are trying to avoid surgery. I have a high rate of improving pain management with full length medial wedge orthotics with a distal drop out on the 1st ray. Supporting the 1st ray reduces the amount of dorsiflexion at heel off. By dropping out the distal aspect of the orthotic, that is from the I.P. joint to the end of the toe leaves room inside the shoe for the heel to rise, reducing the dorsiflexion “moment” by a few degrees. Coupling this modified orthotic with good forefoot rocker shoes, whether they be running shoes or dress type shoes like Dansko effectively can reduce the lever arm on the distal 1st ray by 5-8 degrees. This is often enough to make a person very comfortable. When necessary I have increased the distal rocker on a shoe just by grinding off the anterior sole of the shoe. This article was intended to be all about surgery but orthotic management plays a crucial role in H.R. outcomes.
I had Fusion done to my Great Toe joint about 10 years ago because of Rheumatoid Arthritis. Dr James Brodsky in Dallas did it.
He fused the second toe as well and took a little off the length of the toe. the third toe was long too but he wouldnt do anything with it. It rubs against my shoes and is painful. He told me to buy all new shoes!
Had I been told of the outcome of the surgery and the ROM, I wouldn’t have done it. The joint is still as painful as it was before. I trip over the toes sometimes when i walk. They are a little too low I think. I have terrible burning pain at the tips of both toes and can’t stand any pressure on either toe. Not even my blanket at night . I can’t wear any of my shoes anymore that have even a little heel on them. The two toes rub against my shoes and Im wearing a shoe 1/2 size bigger than I normally wear.
I want to have this reversed if possible. Even restore a little more ROM to the toes. My Orthopedic Surgeon that did my elbow replacement said they could give me more ROM, but not completely reverse it. He wouldn’t do the surgery but suggested I go back to Brodsky to do it. I won’t see him again. His ego is out of control! Very rude and won’t even make eye contact with you.
Can a Dr here advise on what my options are for getting more ROM in those joints? the screws are coming out and I can’t stand to have any pressure over the joint at all.
Thank you
Peyton
Dallas, Tx
I would appreciate any advice. Had a fusion done 5 months ago. I’m 50 years old. Been a runner my entire life. Had pain in the joint for 14 years. Cortisone injections for 12 years, twice per year. My doctor told me fusion was the gold standard. I want to stay active and am trying get back to long walks partial jogging but I’m having pain in the ball of the foot around the interior sesamoid to in between the space of the 2nd toe. I’m concerned I made a poor choice. Can the fusion be reversed? I want to be active but pain free. Any thoughts/recommendations? I would be love a consult if possible. Thank you!