 By Windy Cole, DPM, CWSP, FAPWH
By Windy Cole, DPM, CWSP, FAPWH
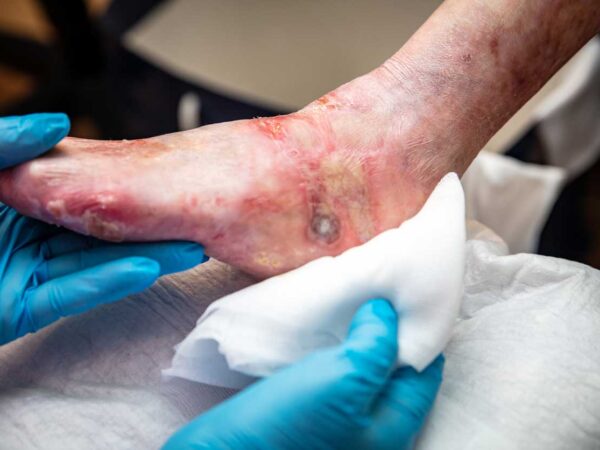
Chronic, hard-to-heal wounds are a major aspect of care in most podiatric offices, which is why antimicrobial resistance (AMR) is an escalating concern for healthcare practitioners. AMR is not only a growing concern for patient health but also poses potential legal and economic ramifications for healthcare providers.
Understanding Antimicrobial Resistance
Antimicrobial resistance occurs when microorganisms such as bacteria, viruses, fungi, or parasites evolve to withstand the antimicrobial drugs designed to eliminate them. This resistance renders standard treatments ineffective, leading to persistent infections and increased transmission of resistant pathogens. The World Health Organization categorizes AMR as one of the top 10 threats to global health, underlining its urgency.
Indeed, the CDC reports that AMR is on the rise, with the 7 most prevalent AMR pathogens causing a combined 20% increase in hospital-onset infections over 3 years.1
Statistics highlight the magnitude of this problem. Globally, an estimated 1.27 million deaths were directly associated to drug-resistant infections in 2019, with millions more associated indirectly. In the United States, AMR kills approximately 23, 000 patients a year and incurs over $20 billion in additional medical expenses. Global economic implications are severe, with potential healthcare costs rising by an estimated $1 trillion by 2050 if AMR is not contained.
The Role of Clinicians in Combatting AMR
Healthcare professionals do bear some responsibility for the rise of AMR due to the overprescription and misuse of antibiotics. In 2022 alone, approximately 236.4 million antibiotic prescriptions were issued in outpatient settings in the US, equating to an astounding 709 prescriptions per 1,000 people.
To mitigate these issues, it is imperative that clinicians refine their wound management practices and enhance antimicrobial stewardship. This involves a thorough understanding of the wound infection continuum and utilizing clinical signs to accurately diagnose infections, rather than yielding to patient pressure or relying on surface-level assessments.
Remembering that many of these patients are not in the best of health is key:
- Presence of peripheral vascular disease (chronic) or altered pharmacodynamics (burn) means antibiotics don’t always reach the site of injury at the correct dose.
- Low levels of antiseptics such as silver increase the chance of developing resistance.
- Biofilms need higher concentration of antimicrobial to be effective.
 Best Practices in Wound Management
Best Practices in Wound Management
Effective wound management begins with precise identification of the cause of the wound and any external factors that may hinder healing. Debridement, or the removal of dead or infected tissue, is crucial. Achieving a balanced moisture environment is equally important—a moist wound bed facilitates healing more effectively than a wound left overly dry or saturated.
Wound cleansing should extend beyond mere surface cleaning. Clinicians should ensure thorough decontamination of both the wound and the surrounding periwound tissue to prevent reinfection. In some cases, employing point-of-care imaging technology, like autofluorescence cameras, can aid in identifying bacterial load and focus debridement efforts more effectively.
Antimicrobial Stewardship: Best Practices
Key best practices for clinicians include:
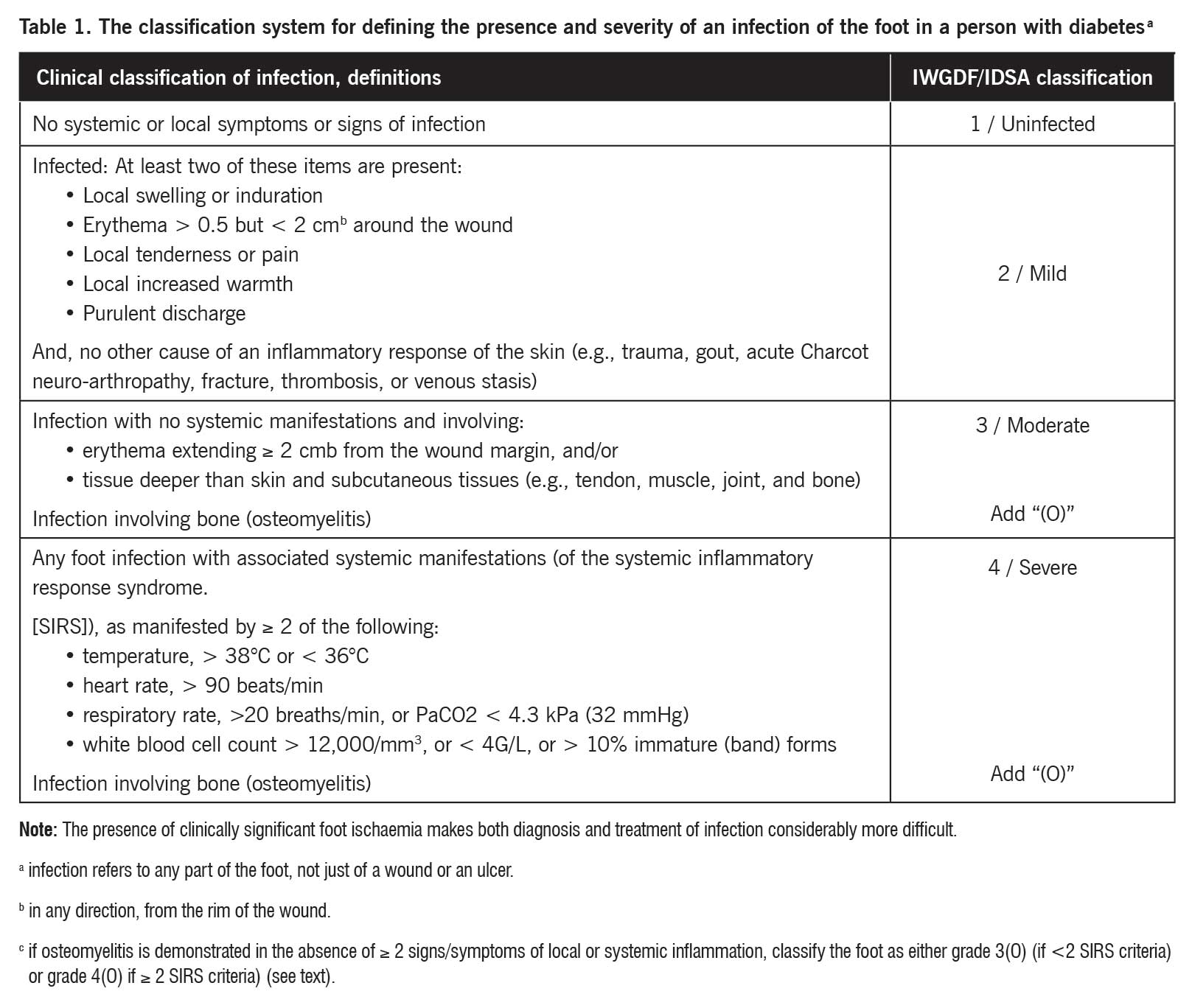
1. Infection Identification: Recognizing clinical signs of infection is crucial. Wounds that show signs of infections like purulent discharge, increased pain, or tissue deterioration should be promptly evaluated. Classification of the infection is critical; Table 1, from the International Working Group on the Diabetic Foot,2 is a good resource.
2. Tissue Sampling: When a wound is suspected of infection, clinicians should prioritize tissue biopsies over swab cultures for more accurate identification of pathogenic bacteria.
3. Antimicrobial Stewardship Programs: These programs involve avoiding unnecessary antibiotic prescriptions, selecting appropriate antibiotic regimens, and ensuring the correct duration of use.
4. Topical Antimicrobial Therapy: In cases where systemic antibiotics aren’t necessary or effective, topical treatments, such as silver dressings, iodine, honey, or PHMB, can be utilized. These should be used for brief periods and alternated to prevent resistance.
5. Advanced Imaging Technologies: Utilization of autofluorescence imaging can help detect bacterial loads in wounds, guiding clinicians to more effectively target treatments and reduce unnecessary systemic antibiotic use.
 Implementing Antimicrobial Stewardship Programs
Implementing Antimicrobial Stewardship Programs
Antimicrobial stewardship programs aim to optimize the use of antimicrobials to improve patient outcomes and limit the development of resistance. Such programs encompass various strategies, including:
1. Educational Initiatives: Educating patients about the appropriate use of antibiotics is essential. Not every wound requires antibiotic treatment, and clinicians must convey this to patients.
2. Preventative Measures: Infection prevention should be a priority, incorporating standard protocols such as hand hygiene and aseptic technique.
3. Collaboration with Infectious Disease Specialists: Engaging colleagues from specialized fields can enhance treatment decisions and ensure the most effective antimicrobial therapies are selected.
4. Appropriate Prescribing Practices: Clinicians should prescribe the most suitable antibiotic, considering the narrowest spectrum required, for the correct duration, and based on tissue culture results where feasible.
5. Monitoring and Reporting: Keeping track of antibiotic prescriptions and outcomes can provide valuable data to support ongoing improvements in practice.
Legal and Ethical Considerations
Many of these wounds are incredibly challenging to treat and clinicians may fear legal consequences if infections progress or treatments prove inadequate. However, thorough documentation of clinical decision-making can provide a robust defense in legal scenarios. Recording the rationale for treatment choices, including instances where antibiotics are withheld, is crucial.
In sum, by adopting rigorous antimicrobial stewardship, practicing diligent wound management, and fostering patient education, lower extremity clinicians can play a pivotal role in curbing the threat of antimicrobial resistance. Such efforts are vital not only for patient safety and clinical efficacy but also for safeguarding the economic and legal interests of healthcare providers.
Windy Cole, DPM, CWSP, FAPWH, has practiced in Northeast Ohio for over 22 years. She is an adjunct professor and Director of Wound Care Research at Kent State University College of Podiatric Medicine. She is double board certified by the American Board of Foot and Ankle Surgery and the American Board of Wound Management. She is an ACCWS board member and a Fellow of the Royal College of Physicians and Surgeons Glasgow. She has been a dedicated wound care advocate for two decades with interests focused on medical education, diabetic foot care, wound care, limb salvage, & clinical research. And she serves on the Editorial Advisory Board of Lower Extremity Review.
This article is a summary of Dr. Cole’s presentation, “Best Antimicrobial Stewardship Practices,” from the 2025 No-Nonsense Seminar held March 7-9. To view the full presentation with questions and answers—and see the agenda for the 3-day program, visit https://nononsense2025.lerexpo.com. Continuing education credits are available for this and many of the lerEXPO programs.
- Antimicrobial resistance threats in the United States, 2021-2022. Centers for Disease Control and Prevention. 2024. Https://www.cdc.gov/antimicrobial-resistance/data-research/threats/update-2022.html
- International Working Group on the Diabetic Foot. Guidelines on the diagnosis and treatment of foot infection in persons with diabetes (Part of the 2023 IWGDF Guidelines on the prevention and management of diabetes-related foot disease). 2023. Available at https://iwgdfguidelines.org/wp-content/uploads/2023/07/IWGDF-2023-04-Infection-Guideline.pdf. Accessed May 30, 2025.







