Adapted from photo courtesy of Small Bone Innovations.
Study findings and anecdotal reports suggest that newer-generation total ankle replacement can match or exceed ankle arthrodesis when it comes to gait and range of motion, but neither procedure returns gait to normal. Implant survival has also improved, but continues to be a challenge.
By Barbara Boughton
Orthopedic surgeon and researcher Timothy Daniels, MD, recently got a surprising real-life picture of what living with a total ankle replacement is like. Daniels, head of orthopedics at St. Michael’s Hospital in Toronto, Canada, asked a patient with a fusion in one ankle and an ankle replacement in the other to compare the two, and received an unexpected answer.
“On the fusion side I’m good for four hours and then I get shin splints and pain and need to take a rest. On the replacement side, I can go for two and a half hours and then it starts to swell and ache,” said the patient, who is an avid golfer. “But I like the ankle replacement better. It just feels more normal and has better motion. When I need to step into a hole to retrieve a ball on the golf course, I know I can trust the foot with the ankle replacement.”
As Daniels’ story illustrates, patient satisfaction is often higher and both motion and gait are equivalent or better following ankle arthroplasty than with the gold standard surgery for ankle arthritis, arthrodesis. The increased motion and improvements in gait possible with total ankle replacement could reduce the risk of arthritis in nearby joints years down the line, according to Daniels and other experts. Yet arthroplasty—despite some of its benefits—also comes with a price.
Once an arthroplasty is done on a patient, it’s likely to fail during the patient’s lifetime, requiring another total ankle replacement and additional surgery. By contrast, an ankle fusion can last a lifetime. And a patient’s gait after total ankle replacement might be better than after arthrodesis, but gait in either case is still a far cry from what it would be in someone without either arthritis or ankle replacement.
“Patients with total ankle replacements are able to use their ankle motion more than those with fusions, but their gait is still is still not normal or even near to it,” said Daniels, an associate professor at the University of Toronto.
Replacement and ROM

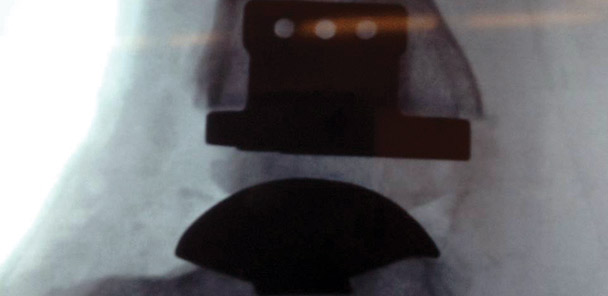
igure 1. Anteroposterior (left) and lateral (right) radiographs of a total ankle replacement. (Images courtesy of Tim Gueramy, MD.)
With an ankle replacement, patients attain an average increased range of motion (ROM) of up to 35°, noted Tim Gueramy, MD, an orthopedic surgeon in Austin, TX. In a 2011 study of 118 patients published in Foot & Ankle International,1 Swiss researchers found the total ROM change after total ankle replacement varied between 26.9° and 35.3°.
Daniels’ research indicates that patients with ankle replacements attain more dorsiflexion, less tibial tilt, a faster gait, and a longer stride than ankle fusion patients.
In a study presented at the annual meeting of the American Orthopaedic Foot & Ankle Society (AOFAS) in 2012, Daniels’ research group found that, two years after surgery, 17 total ankle replacement patients had more sagittal plane ROM and more dorsiflexion ROM than 17 fusion patients.2 Ankle power was also 30% greater in the total ankle replacement patients.
Studies indicate that longer-term patient outcomes after total ankle replacement also may be better than with ankle fusion.
In midterm results of a multicenter study presented at the annual meeting of the American Academy of Orthopaedic Surgeons (AAOS) in March in Chicago, outcomes of 339 patients who received either total ankle replacement or fusion were compared during an average follow up of five years.3 Both groups showed significant improvements in the Ankle Osteoarthritis Scale after surgery, though the improvement in the total ankle replacement group was significantly greater.
Yet, the differences disappeared in multivariate analysis when baseline characteristics such as age and diabetes were considered, results that may not reflect advances in the last five years that have made total ankle replacement a more viable option for younger patients, according to Daniels and colleagues who performed the study.
Daniels’ research group also reported positive three-year results in a study on patient outcomes after total ankle replacement using a third-generation prosthesis, in a paper published in Foot & Ankle International in April.4 After a mean follow up of 40 months on 85 patients with arthritis, Daniels and colleagues found that AOFAS ankle-hindfoot scores improved from 38.2 to 74.8 after surgery. Early results suggest the total ankle replacement provides both pain relief and improved function, Daniels and his colleagues concluded.
The findings are consistent with those of a 2011 study published in Foot & Ankle International, in which German researchers found that a third-generation total ankle prosthesis increased ROM significantly in 218 patients; in particular, flexion/extension ROM increased from 25.1° to 33.1° two years after the surgery.5
“The increased motion provided by ankle replacements means that other joints do not have to work as hard to enable the foot to function,” said Steven Haddad, MD, an orthopedic surgeon at the Illinois Bone and Joint Institute in Glenview, IL, and current president of the AOFAS. Haddad performs 70 to 80 ankle replacements per year, and has done more than 500 in the last 10 years.
Offloading other joints
Ankle replacement surgery is considered a more technical procedure than hip and knee replacements, for example.
“It’s an extremely difficult operation with very little room for mistakes,” Gueramy said.
As well as putting the prosthesis in place, the foot needs to be well-balanced under the replacement—meaning the foot needs to be aligned well during surgery, according to Haddad. Surgeons accomplish this exact alignment by using intraoperative fluoroscopy, he said.
“When the foot is well balanced during total ankle replacement, it puts less stress on the other joints,” Haddad said.
Haddad noted that, because patients with an ankle fusion have an immobilized joint, their other joints have to compensate, and that’s the major reason why more stress and load is put on other joints of the foot.
“The improvements in gait we see with total ankle replacement mean that patients use the ankle more efficiently and there’s less stress put on other joints in the foot. As a result, patients have less risk of developing degenerative arthritis years down the line,” Haddad said.
Haddad noted that a majority of patients with ankle fusion progress to arthritis in a different joint of the foot 20 years later, as documented by a 2001 study published in the Journal of Bone and Joint Surgery (JBJS).6 A mean of 22 years after ankle arthrodesis, a majority of the 23 patients in the study had substantial and accelerated arthritic changes in the ipsilateral foot. Joints more severely affected by osteoarthritis on the ankle fusion side included the subtalar, talonavicular, calcaneocuboid, naviculocuneiform, tarsometatarsal, and first metatarsophalangeal joints.
The risk of arthritis in the subtalar joint after ankle arthrodesis, and the need for an additional fusion, is of particular concern. In another JBJS study, published in 2006, four of 26 patients who had undergone ankle arthrodesis developed moderate to severe arthritis of the subtalar joint just four years later.7
“As yet, however, there’s no data that says we’re saving these joints with replacement as compared to fusion,” Daniels said.
Yet, Gueramy points out that total ankle replacements have been performed for fewer than 20 years. So getting scientifically sound statistics on arthritis in other joints after ankle arthroplasty may be a difficult task.
“You’d need a huge study to show significance, and it would need to be done over more than 20 years. That’s a very long and expensive study,” Gueramy said.
Haddad noted that, because ankle fusions immobilize the ankle joint, more proximal joints such as the knee may sustain additional stress in order to maintain function. Hip and back joints may also undergo greater stress and load, similar to the imbalances seen when a patient wears a cast for an extended period, Haddad said.
“The result can be exacerbation of pre-existing conditions such as disc disease in the back or new pain in the knee, hip, or back over time,” he said.
Gait changes
The gait of a patient with a total ankle replacement, when viewed visually, can seem similar to that of a patient with an ankle fusion—particularly if the patient is wearing a supportive cushioned shoe. Yet a clinician or researcher examining the patient closely can often detect a shorter stride and a slower pace in ankle fusion patients, Haddad said. Gait analysis can also pinpoint these differences.
In a paper published in Foot and Ankle International in 2012, Robin Queen, PhD, and colleagues at Duke University Medical Center in Durham, NC, found that 51 patients with total ankle replacement showed significant improvements in gait mechanics compared with their preoperative function during walking.8 The researchers assessed gait using the Four Square Step Test and Timed Up and Go test. Patients’ AOFAS-hind foot scores also significantly improved two years after surgery compared with preoperative scores.
“In our research, we have found improvement with total ankle replacement in a number of spatial temporal parameters—such as how many steps patients have to take, how much time they spend on the foot with the ankle replacement, and how long a step they can take,” said Queen, director of the Michael W. Krzyzewski Human Performance Lab at Duke.
Queen and colleagues are now planning future studies that will look at survivability of total ankle replacements and postoperative complications as well as gait mechanics.
“We want to show what the entire process looks like when you have a total ankle replacement,” Queen said. “In that way we can improve patient education and tell patients whether they can have better quality of life with a fusion or total ankle replacement.”
Future studies will also look at cost-effectiveness of total ankle replacements, according to Queen.
Survival tactics
One impact of ankle replacement on quality of life is that the prosthesis can probably fail after 10 years, though newer prostheses may have a longer life, according to Haddad. In a review article published in JBJS in 2007, Haddad and colleagues analyzed primary studies on total joint replacements published between 1990 and 2005.9 The review, which included only studies of first- and second-generation implants, showed the 10-year implant survival rate was 77%.
“Two in ten required some sort of revision over ten years. However, we are now on the fourth generation of implants, and we simply don’t know how long these will last. But we assume they will last longer than ten years through improved technology,” Haddad said.
Still, as a result of implant failure, one or two more arthroplasties may need to be performed to preserve ankle function in a patient with arthritis during their lifetime. And that means repeated surgeries—with all their associated risks, Daniels said.
The newer prostheses have a lower profile, meaning the surgeon has to resect less bone for implantation, which means revision surgery may be easier.
“The surgeon would have more bone to work with theoretically, but you also have to consider that, if a prosthesis were to fail, it normally destroys some portion of bone. Thus, in the end the lower profile prostheses may be equivalent [to higher-profile devices],” Haddad said. “Theoretically, however, these prostheses can last longer, so we can use them in younger patients, such as those in their fifties.”
In a study presented at the AAOS annual meeting in 2013, a research team from Portugal contrasted outcomes with total ankle replacement in patients younger than 50 years with results after implant surgery in older patients.10 Forty three total ankle replacement patients younger than 50 years had significantly greater ROM and ankle function at follow up (between two and five years) than 72 patients older than 50 years, according to the study. Yet, implant survivorship was similar between groups, according to study investigator Ricardo Rodrigues-Pinto, MD, an orthopedic surgeon at the Centro Hospitalar do Porto in Oporto, Portugal.
Yet, implanting a total ankle replacement in a 50-year-old may mean a difficult conversation with the patient, Haddad acknowledges.
“With a total ankle replacement you will have more surgeries than with an ankle fusion. If patients want one operation to last their entire life—even though they may sacrifice function and have the risk of arthritis later on—then they have to choose fusion,” Haddad said.
Each patient undergoing a fusion or ankle replacement should have a long conversation with their doctor about the near- and long-term outcomes of each surgery, Daniels said.
“The patient and doctor need to make a true joint decision on whether to choose a fusion or total ankle replacement,” he said.
Daniels also emphasized the importance of educating patients on both the benefits and drawbacks of total ankle replacement, including its effect on gait.
“Patients do appreciate the increase in range of motion provided by total ankle replacement, and the pain relief is similar to that seen with fusion,” he said. “Both surgeries are good solutions for a difficult problem.”
Barbara Boughton is a freelance health and medical writer based in the San Francisco Bay Area.
1. Barg A, Knupp M, Anderson AE, Hintermann B. Total ankle replacement in obese patients: component stability, weight change and functional outcome in 118 consecutive patients. Foot Ankle Int 2011;32(10):925-932.
2. Sinber SB, Klejman S, Pinsker E, et al. Ankle arthroplasty and ankle arthrodesis—prospective gait analysis compared to controls. Presented at the American Orthopaedic Foot & Ankle Society Annual Meeting, San Diego, June 2012.
3. Younger ASE, Daniels TR, Glazebrook M, et al. Multicenter study comparing total ankle arthroplasty and ankle arthrodesis: Mid-term results. Presented at the Annual Meeting of the American Academy of Orthopaedic Surgeons, Chicago, March 2013.
4. Sproule JA, Chin T, Amin A, et al. Clinical and radiographic outcomes of the mobility total ankle arthroplasty system: early results from a prospective multicenter study. Foot Ankle Int 2013;34(4):491-497.
5. Schenk K, Lieske S, John M, et al. Prospective study of a cementless, mobile-bearing, third generation total ankle prosthesis. Foot Ankle Int 2011;32(8):755-763.
6. Coester LM, Saltzman CL, Leupold J, Pontarelli W. Long-term results following ankle arthrodesis for post-traumatic arthritis. J Bone Joint Surg Am 2001;83(2):219-228.
7. Thomas R, Daniels TR, Parker K. Gait analysis and functional outcomes following ankle arthrodesis for isolated ankle arthritis. J Bone Joint Surg Am 2006;88(3):526-535.
8. Queen RM, De Biassio JC, Butler RJ, et al. J. Leonard Goldner Award 2011: Changes in pain, function and gait mechanics two years following total ankle arthroplasty performed with two modern fixed-bearing prostheses. Foot Ankle Int 2012;33(7):535-542.
9. Haddad SL, Coetzee JC, Estok R, et al. Intermediate and long-term outcomes of total ankle arthroplasty and ankle arthrodesis. A systematic review of the literature. J Bone Joint Surg Am 2007;89(9):1899-1905.
10. Rodrigues-Pinto R, Geada JMM, Oliva XM, Amado P. Total ankle replacement in patients under the age of 50. Should this still be contraindicated? Presented at the Annual Meeting of the American Academy of Orthopaedic Surgeons, Chicago, March 2013