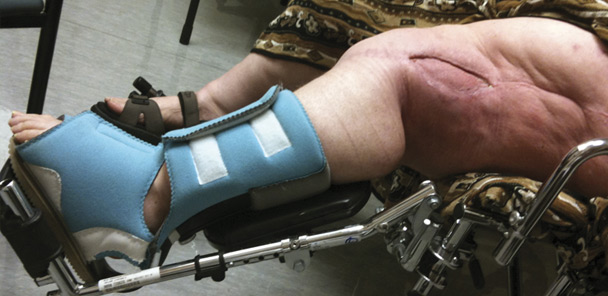
Figure 1. A 10-year-old boy now plays baseball and is happy after undergoing an above-knee amputation. (Photo courtesy of Farbod Malek, MD.)
Studies assessing the relative functional benefits of limb salvage and amputation for lower extremity bone and soft tissue tumors have produced inconsistent results, but the range of subjective and objective tests used in those studies may have influenced the findings.
By Lucy Kupersmith, BA, and
Jeremy S. Somerson, MD
Amputation has long been the gold-standard treatment for bone and soft tissue tumors of the extremities, but in the past 20 years limb salvage surgery (LSS) has become the more popular choice when it is technically feasible. There are many reasons for this change, including a cosmetic preference, preservation of uninvolved tissue, and purported improved functioning compared with the alternative of amputation. However, the functional benefits have yet to be fully illustrated in the literature. Several studies have used a variety of subjective and objective measurements to shed light on what makes LSS the preferable surgery from a functional standpoint, but overall results have been mixed or inconclusive.
There are many indications for LSS and amputation, including trauma and vascular diseases, but studies often focus on bone and soft tissue tumors of the extremities as these diseases often affect young, healthy individuals with few comorbid conditions, good overall preoperative function, and a high likelihood of reaching maximal functional status postoperatively. We identified nine studies1-9 published in the past 10 years that compared LSS to lower extremity amputation as the surgery of choice for bone and soft tissue tumors located somewhere in the lower extremity. Five of these used subjective endpoints exclusively, while four employed at least one objective measurement in conjunction with subjective tests. In an effort to clarify the trends of literature to date, we have analyzed the results of these nine studies as well as the testing modalities used to achieve these results.
Literature using subjective measures
The five subjective studies used an array of functional measurements, but the tests that came up most frequently were the Musculoskeletal Society Tumor Score (MSTS), the Toronto Extremity Salvage Score (TESS), and the Short Form Health Survey (SF-36). The methods, benefits, and limitations of each are discussed here.
MSTS: The MSTS was developed between 1981 and 1989 by the Musculoskeletal Tumor Society and was adopted by the International Symposium on Limb Salvage as a standardized method of evaluating functional status following limb salvage and other orthopedic procedures.10 It includes six parameters upon which the patient is ranked on a scale of zero to five; these are pain, function, emotional acceptance, use of supports, ability to walk, and gait. A score of five indicates optimal function. The scores are then added, presented as a percentage, and rated poor, fair, good, or excellent.
This testing option includes both functional and quality of life (QOL) aspects and has been used for more than 20 years with highly consistent results. By inquiring about the use of supports while walking, it provides more objective data on physical functional impairment than either the TESS or SF-36 subjective testing modalities. However, the inclusion of questions about postoperative limp and the need for a prosthesis may skew the data toward favoring LSS over amputation.1

Figure 2. This child underwent a rotationplasty to salvage the limb but still experiences pain and unhappiness. (Photo courtesy of Farbod Malek, MD.)
TESS: The TESS is a self-administered questionnaire first presented in 1996 to evaluate physical function from the patient’s perspective. It lists 29 to 30 activities of daily life about which the patient is asked to rate his or her ability to perform on a scale of one to five; a score of five indicates normal function. Research has shown that it correlates moderately well with the MSTS, and, when administered repeatedly over a period of time, is able to provide a longitudinal assessment of how a patient is progressing in the years following surgery.1 However, because the test relies on patients’ perception of their abilities, it cannot provide an unbiased evaluation of their limb function. It also contains no direct analysis of function, making it a better gauge of an individual’s ability to cope with limitations after surgery than a true measurement of inherent function.
SF-36: The SF-36 is a 36-point questionnaire that has been used widely since 1988 to evaluate physical and mental health in a variety of patients, as well as in healthy individuals. A general tool for assessing broad categories of physical and mental health, the questionnaire’s 36 items correlate with eight scales on which individuals grade themselves: physical function, role-physical, bodily pain, general health, vitality, social functioning, role-emotional, and mental health.1 Like other subjective tests, the SF-36 consistently demonstrates internal consistency, correlates well with other measures of mental and physical health, and provides an excellent insight into how patients perceive their QOL.
Subjective analyses were the primary functional assessment in five major studies published in the last 10 years on the indications for limb salvage surgery versus amputation. In 2008, Aksnes et al compared the outcomes of 118 patients at least five years after either LSS surgery or amputation for Ewing sarcoma or osteosarcoma of the lower extremity, using MSTS and TESS for functional outcomes and SF-36 for data on QOL.1 They demonstrated that patients undergoing amputation reported clinically significant lower scores on MSTS than patients undergoing LSS, but found no difference bewteen the two groups of patients with the TESS or SF-36 scores. The authors concluded that, after an initial observation period of five years, LSS provides a relative functional benefit over amputation, but both procedures result in similar QOL for patients.
Nagarajan’s 2009 study of QOL in patients with osteosarcoma also used the TESS to evaluate the functional outcomes of any lower extremity amputation versus LSS five years after surgery, and again demonstrated no difference in functional outcomes using this measurement.2 Finally, Robert et al also used TESS results to evaluate functional differences in 57 patients two years after any lower extremity amputation or LSS and determined that lower limb function was comparable in each group after adjustments for length of time following surgery.3
These three studies provide consistent results showing the TESS indicates no functional difference between lower extremity amputation and LSS, although, as stated previously, the TESS is a better indicator of patients’ ability to manage following surgery than an indicator of physical limitations.
In addition to Aksnes et al, two other studies used the MSTS score to evaluate functional status after surgery. Ahakane et al used the SF-36 and MSTS in a 2007 assessment of the relative benefits of above-the-knee amputation (AKA), endoprosthesis, and rotationplasty in 29 patients with malignancy around the knee joint, and found that, according to the SF-36 results, “there was no difference in the way that patients perceived their outcome despite the differences in treatment,” but that there was a statistically significant functional and overall benefit of rotationplasty over AKA based on the MSTS.4
In the third of these studies to employ the MSTS for functional measurements, Zahlten-Hinguranage et al investigated QOL and function in 124 patients at least one year after amputation or ablative LSS.5 As with previous studies, improved function was reported with LSS compared with amputation by MSTS standards, but the authors noted “this advantage is a computed value rather than true superiority in physical functioning.”
An additional conclusion can be drawn from the SF-36 results from Aksnes and Akahane that indicated no difference in QOL outcomes between amputation and LSS groups in either study. From a review of the recent subjective studies it can be concluded that there are no QOL differences or disparities in coping ability demonstrated by SF-36 or TESS scores in patients following LSS or amputation, but that there is some physical function benefit to LSS over amputation established by MSTS results.
Literature using objective measures
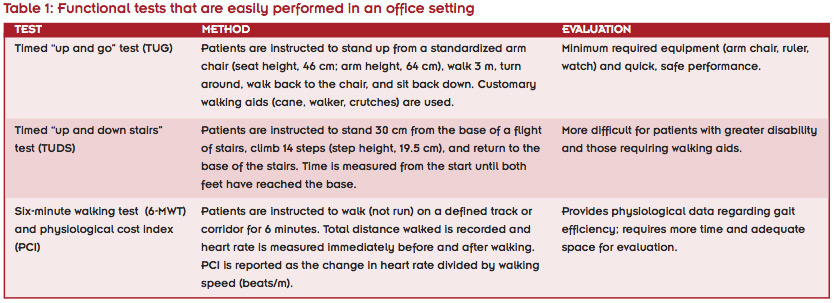
Four studies published in the past 10 years used objective functional measurements in the analysis of physical functional benefits of LSS versus amputation. These measurements range from simple functional tests that can be performed in the office (Table 1) to those requiring highly specialized equipment.
In 2006 Hopyan et al published a study of 123 patients with diagnoses of lower extremity osteosarcoma or Ewing sarcoma comparing functional outcomes of LSS, AKA, and rotationplasty after at least five years.6 Subjects were evaluated using MSTS, TESS, SF-36, and an Uptimer device strapped to the inner thigh for a 24-hour period to record time spent standing or walking versus sitting or reclining. There were no statistically significant differences in Uptime among the groups examined, although data showed a trend for more Uptime in the rotationplasty group than the other two. Additional results for the other measurements were consistent with those of the subjective studies, with no significant disparity between results on the TESS or SF-36, and superior scores on the MSTS in the LSS group compared with the other two tests.
Ginsberg et al evaluated QOL and functional outcomes of 91 adolescents and young adults after LSS or amputation.7 QOL was determined by SF-36, and functional outcome was measured using MSTS, TESS, and the Functional Mobility Assessment (FMA), a test that requires subjects to perform several tasks and grades them from 0 to 5 in six areas: pain; function on timed up and down stairs with evaluation of heart rate and perceived exertion; use of supports; satisfaction; participation in work or school events; and endurance on a nine-minute walk/run with evaluation of heart rate and perceived exertion. A score of five indicates superior performance.
The study included two types of amputation groups, AKA and below-knee (BKA), as well as three types of limb-sparing groups: limb-sparing femur, limb-sparing tibia, and rotationplasty. Results showed the LSS groups performed better than the amputation groups on the FMA, but there were no significant differences between groups on the MSTS, TESS, or SF-36. The FMA tests provide quantifiable and reproducible measurements of functional status, while also including more subjective evaluations of patients’ pain and perceived exertion.
In a 2011 study Bekkering et al compared the functional outcomes of 39 LSS patents and 43 AKA or BKA patients one to five years postoperatively using TESS scores in conjunction with five performance tests: time to walk up and down stairs (TUDS); time to stand, walk 3 m, turn, and sit back down (timed up and go test; TUG); time to lie down and then stand up (LDSU); various walking activities (VWA); and the six-minute walking test (6-MWT), which included data on heart rate, speed, and distance walked that were then used to calculate the physiological cost index (PCI).8
The PCI score was calculated by dividing change in heart rate after the 6-MWT by the average walking speed. Results showed no difference in TESS scores between the two study groups. The researchers also noted no significant differences between groups in PCI score, average speed, or distance walked. LSS patients, however, performed the TUDS and VWA tests significantly more quickly than amputation patients.

Figure 3. Limb salvage can be an appealing option in patients for whom lower extremity function is not a high priority, as in the patient pictured here. (Photo courtesy of Farbod Malek, MD.)
Finally, a study by Malek et al retrospectively assessed QOL, self-reported functionality, and physical gait efficiency in 20 patients following LSS or AKA at least 12 months following surgery using the SF-36, TESS, Reintegration to Normal Living Index (RNL), and PCI, which they calculated from changes in heart rate and distance walked in a five-minute walking test.9 The RNL measures how well patients returned to a normal life by having them answer yes or no to 11 questions regarding activities of daily living. There were no differences between groups for QOL and functionality as measured by the SF-36 and TESS. The RNL showed higher scores in the LSS group, indicating a better ability to return to normal activities of daily living in the postoperative rehabilitation stage. The PCI scores were superior in LSS patients, an objective measurement demonstrating better physical functioning in the LSS group.
Taken as a whole, results for TUDS, VWA, FMA, and distance walked on endurance tests showed statistically significant better scores for LSS groups than amputation groups in three of the four studies. The PCI data from two studies also tended toward better scores in the LSS group, as did the Uptimer results from Hopyan et al.
Conclusion
There may be functional benefits to LSS over amputation for lower extremity tumors when LSS is a viable option. The largest of the objective studies examined here had only 91 participants and the results have not yet been reproduced by other teams using the same FMA test. The objective studies that included the subjective performance exams SF-36, TESS, and/or MSTS demonstrated findings consistent with those of exclusively subjective studies, showing equivalent SF-36 and TESS scores between the two groups, and improved MSTS ratings in the LSS groups. It is thus possible that objective tests such as the TUDS, VWA, and FMA are better able to distinguish small differences in functional outcomes than the ubiquitous TESS and SF-36 scores. It remains unclear which specific elements of the limb salvage technique give these patients the apparent functional benefits over amputation patients, though each exam tool provides one more clue as to where the benefits lie.
These data show that researchers are on the right track in their search for an objective functional exam tool that will allow clinicians to measure functional outcomes quickly and easily in office settings. There is still a long way to go in proving that limb salvage surgery provides lasting, reproducible, and quantifiable functional advantages over amputation, but with larger and more comprehensive studies using more specific testing modalities, the exact nature of the benefit should be elucidated. Advancements in prosthetic technology and new surgical techniques are being developed that will likely have an impact on the relative functional benefits of amputation versus limb salvage in the future, and this will be an exciting field to watch as it continues to evolve.
Lucy Kupersmith, BA, is a medical student and Jeremy S. Somerson, MD, is an orthopedic surgery resident at the University of Texas Health Science Center at San Antonio.
1. Aksnes LH, Bauer HC, Jebsen NL, et al. Limb-sparing surgery preserves more function than amputation: a Scandinavian sarcoma group study of 118 patients. J Bone Joint Surg Br 2008;90(6):786-794.
2. Nagarajan R. Quality of life (QOL) in patients with osteosarcoma. Recent Results Cancer Res 2009;179:339-344.
3. Robert RS, Ottaviani G, Huh WW, et al. Psychosocial and functional outcomes in long-term survivors of osteosarcoma: a comparison of limb-salvage surgery and amputation. Pediatr Blood Cancer 2010;54(7):990-999.
4. Akahane T, Shimizu T, Isobe K, et al. Evaluation of postoperative general quality of life for patients with osteosarcoma around the knee joint. J Pediatr Orthop B 2007;16(4):269-272.
5. Zahlten-Hinguranage A, Bernd L, Ewerbeck V, Sabo D. Equal quality of life after limb-sparing or ablative surgery for lower extremity sarcomas. Br J Cancer 2004;91(6):1012-1014.
6. Hopyan S, Tan JW, Graham HK, Torode IF. Function and upright time following limb salvage, amputation, and rotationplasty for pediatric sarcoma of bone. J Pediatr Orthop 2006;26(3):405-408.
7. Ginsberg JP, Rai SN, Carlson CA, et al. A comparative analysis of functional outcomes in adolescents and young adults with lower-extremity bone sarcoma. Pediatr Blood Cancer 2007;49(7):964-969.
8. Bekkering WP, Vliet Vlieland TP, Koopman HM, et al. Functional ability and physical activity in children and young adults after limb-salvage or ablative surgery for lower extremity bone tumors. J Surg Oncol 2011;103(3):276-282.
9. Malek F, Somerson JS, Mitchel S, Williams RP. Does limb-salvage surgery offer patients better quality of life and functional capacity than amputation? Clin Orthop Relat Res 2012 February 1. [Epub ahead of print]
10. Enneking WF, Dunham W, Gebhardt MC, et al. A system for the functional evaluation of reconstructive procedures after surgical treatment of tumors of the musculoskeletal system. Clin Orthop Relat Res 1993;(286):241-246.