By Victoria Exley, Katherine Jones, Grace O’Carroll, Judith Watson, and Michael Backhouse
Ingrown toenails are a common nail pathology, yet there is a lack of good quality evidence to guide practice.
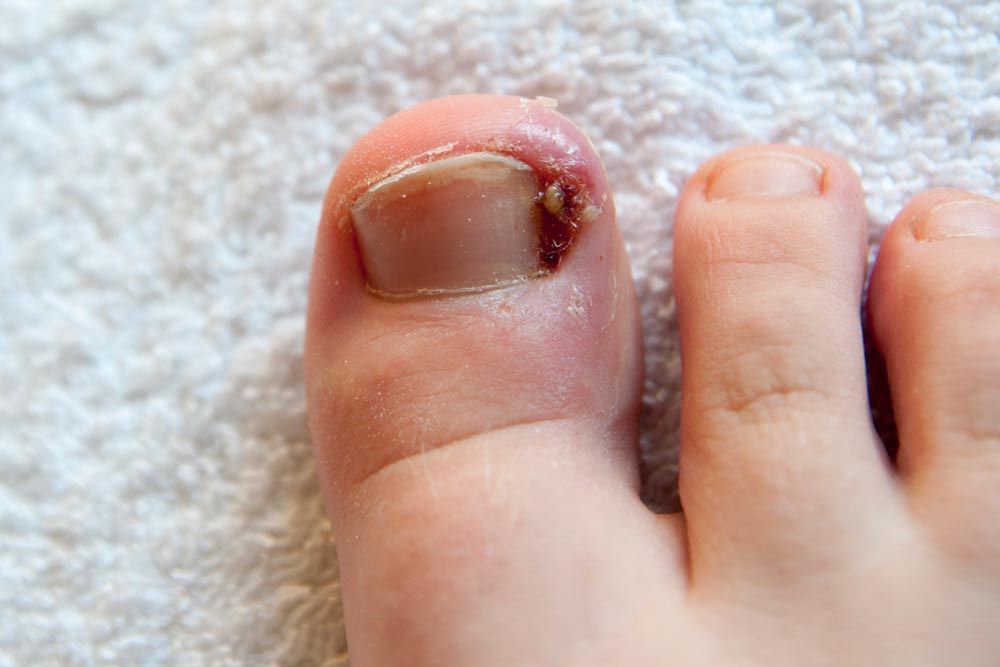
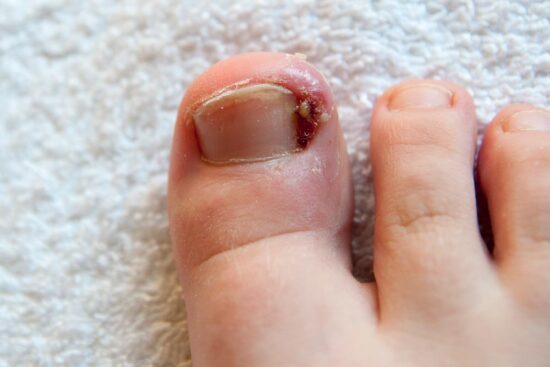 An ingrown toenail, or onychocryptosis, is a common nail pathology that occurs when the nail plate punctures the periungual skin causing substantial pain, inflammation, discomfort, and increased risk of infection if left untreated. Several factors have been proposed as contributory to the occurrence or worsening of ingrown toenails with varying degrees of evidence. These include poor nail cutting technique, hyperhidrosis, ill-fitting footwear, nail deformity, trauma, obesity, and peripheral edema.
An ingrown toenail, or onychocryptosis, is a common nail pathology that occurs when the nail plate punctures the periungual skin causing substantial pain, inflammation, discomfort, and increased risk of infection if left untreated. Several factors have been proposed as contributory to the occurrence or worsening of ingrown toenails with varying degrees of evidence. These include poor nail cutting technique, hyperhidrosis, ill-fitting footwear, nail deformity, trauma, obesity, and peripheral edema.
Conservative approaches have all been advocated in the literature for use in mild to moderate stages (stage I and II) with varying success rates and quality of evidence. However, when conservative treatment fails, where there is nail deformity, or in more severe cases (stage II and III), a surgical approach is often recommended aiming to remove the problem part of the nail and destroy the underlying matrix to avoid recurrence. Despite recent narrative reviews, there is a need for an up-to-date and rigorous systematic review of surgical methods for treating ingrown toenails. The aim of this study, therefore, was to systematically search and synthesize the literature relating to the effectiveness/efficacy of surgical methods for treating ingrown toenails.
Methods
Five databases (MEDLINE, Embase, CINAHL, Web of Science and CENTRAL) and two registers (Clinicaltrials.gov and ISRCTN) were searched to January 2022 for randomized trials evaluating the effects of a surgical intervention(s) for ingrown toenails with a follow-up of at least 1 month. Two independent reviewers screened records, extracted data, assessed risk of bias and certainty of evidence.
Results
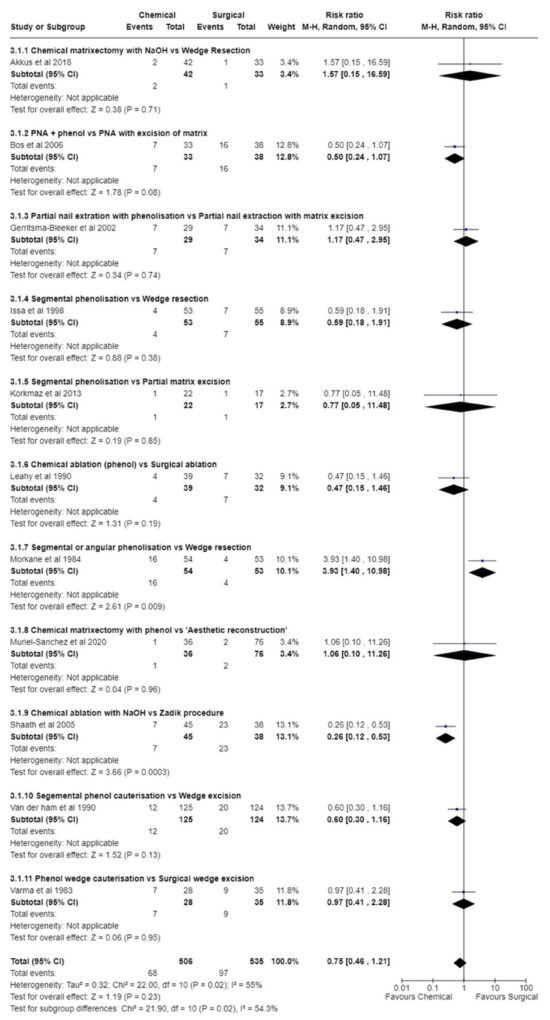
The systematic search identified 1,641 potential publications which, after screening, enabled 36 studies with 3,756 (62.7% males) participants covering a range of techniques that were included in the review. Of these, 31 were included in the meta-analysis for recurrence (Figure 1) and 5 were reported narratively. In addition, synthesis of evidence for relief of symptoms was reported narratively due to the small number of studies reporting this outcome. Recurrence was reported in all but 1 study. The definition of recurrence varied between studies and 2 studies were unclear and reported the “number of successes/number of failures” and “number symptom-free,” respectively. Therefore, these studies were reported narratively. Follow-up ranged from 1 to 24 months.
Interventions
Chemical matrixectomy vs conservative management
Two studies found that phenol matrixectomy did not significantly decrease the rate of recurrence when compared to a conservative approach such as nail tube splinting or nail elevation and flexible tubing (RR 0.55 [95% CI 0.19 to 1.61], I2 0%; P = 0.280).
Surgical matrixectomy vs conservative management
Two studies compared surgical matrixectomy to a conservative approach, however neither method was significantly more effective at preventing recurrence (RR 0.72 [95% CI 0.33 to 1.56] I2 34%; P = 0.410).
Chemical matrixectomy vs surgical matrixectomy
Combining the 11 studies where chemical matrixectomy was compared to surgical matrixectomy, found no significant difference in their ability to prevent recurrence (RR 0.75 [95% CI 0.46 to 1.21] I2 55%; P = 0.230) (Fig. 1).
Chemical matrixectomy vs chemical matrixectomy
Two studies compared phenol to trichloroacetic acid, however neither chemical proved to be more effective at preventing recurrence (RR 0.19 [95% CI 0.01 to 3.80] P = 0.280).
Surgical matrixectomy vs other (eg, CO2 laser, electrocautery)
In 3 studies, a surgical intervention (partial nail matrixectomy or curettage) did not significantly decrease the rate of recurrence when compared to an alternative method of matrixectomy such as electrocautery or CO2 laser (RR 1.61 [95% CI 0.88 to 2.95] I2 37%; P = 0.120).
Chemical matrixectomy vs other (e.g., CO2 laser, electrocautery)
When comparing chemical matrixectomy to an alternative method of matrixectomy in 2 studies, there was no significant difference in prevention of recurrence (RR 0.58 [95% CI 0.25 to 1.37] I2 0%; P = 0.220).
Avulsion vs avulsion + chemical matrixectomy
Avulsion with phenol matrixectomy was compared with nail avulsion alone in 2 studies. There was a significant reduction of recurrence in favor of phenol matrixectomy (RR 0.13 [95% CI 0.06 to 0.27] I2 0%; P < 0.001).
Surgical matrixectomy vs surgical matrixectomy
One study compared the Winograd procedure using a new suturing technique to the same surgical intervention using a traditional suturing technique. After 12 months, the new suturing technique was found to be more effective at preventing recurrence compared to the traditional technique (RR 0.42 [95% CI 0.21 to 0.85]). Another compared central toenail resection to wedge toenail resection. After 6 months, the central toenail resection was considered more effective at preventing recurrence (RR 0.05 [95% CI 0.0 to 0.79]).
Surgical matrixectomy vs surgical + chemical matrixectomy
Two studies compared a surgical intervention, either nail bed excision or wedge resection, with the same surgical intervention plus the addition of phenol. However, addition of phenol was not significantly more effective at preventing recurrence (RR 3.68 [95% CI 0.20 to 67.35] I2 76%; P = 0.380).
Chemical matrixectomy vs surgical + chemical matrixectomy
In 2 studies, surgical matrixectomy plus phenolization did not significantly decrease the rate of recurrence when compared to phenolization alone (RR 1.92 [95% CI 0.06 to 62.30] I2 62%; P = 0.710).
Local anesthetic vs local anesthetic + adrenaline (epinephrine)
Two studies compared local anesthetic (4 mL solution of 2% mepivacaine; 2% lidocaine, respectively), with a combination of the same local anesthetic plus adrenaline (epinephrine). The use of adrenaline did not significantly decrease the rate of recurrence (RR 1.03 [95% CI 0.22 to 4.86] I2 0%; P = 0.970).
Chemical application time: 30 s vs 60 s
Of the 1 study that was included in the meta-analysis, the study authors compared the recurrence rate between phenol applications of 30 s or 60 s, finding the 60-s application was more effective at preventing recurrence (RR 2.00 [95% CI 0.19 to 21.41]).
Antibiotics vs no antibiotics
 Of the 1 study included in the meta-analysis, it was shown that after 12 months the use of topical antibiotics alongside a chemical or surgical matrixectomy did not significantly decrease the rate of recurrence (RR 0.54 [95% CI 0.12 to 2.52] I2 58%; P = 0.430).
Of the 1 study included in the meta-analysis, it was shown that after 12 months the use of topical antibiotics alongside a chemical or surgical matrixectomy did not significantly decrease the rate of recurrence (RR 0.54 [95% CI 0.12 to 2.52] I2 58%; P = 0.430).
Relief of symptoms
Five studies assessed relief of symptoms. Two studies assessed symptoms using a visual analogue scale ranging from 0 to 10; the remaining 3 studies did not specify the instrument used. No definitions were provided for relief of symptoms.
Chemical procedures
In 2 studies, no statistically significant differences were identified between patients receiving 3 min application of 80% phenol, 2 min of 10% sodium hydroxide, and 1 min of 10% sodium hydroxide.
Chemical and surgical procedures
No significant differences were found between partial nail extraction with phenolization and partial nail extraction with matrix excision at 1, 3, or 12 months (P = 0.130, P = 0.270, P = 0.290, respectively).
Surgical procedures
Central toenail resection was shown to be significantly better in relieving symptoms compared to wedge toenail resection after 4 and 8 weeks (both P = 0.001).
Surgical and conservative procedures
Following either partial nail extraction with partial matrix excision or orthonyxia, no differences were noted after 12 months.
Conclusion
This paper presents the co-primary outcomes from a systematic review with meta-analysis that should be interpreted in conjunction with its second paper, which will appear in a coming issue. Despite the high number of publications on this topic, the quality of research was poor and the conclusions that can be inferred from existing trials is limited. Phenolization of the nail matrix reduces the risk of recurrence following nail ablation, and 1 min appears to be the optimum time for application. Despite this being a widely performed procedure there remains a lack of good quality evidence to guide practice.
This article has been excerpted from “A systematic review and meta-analysis of randomized controlled trials on surgical treatments for ingrown toenails part I: recurrence and relief of symptoms.” J Foot Ankle Res 16, 35 (2023). https://doi.org/10.1186/s13047-023-00631-1. Editing has occurred, including the renumbering of tables, and references have been removed for brevity. Use is per CC Attribution 4.0 International License.