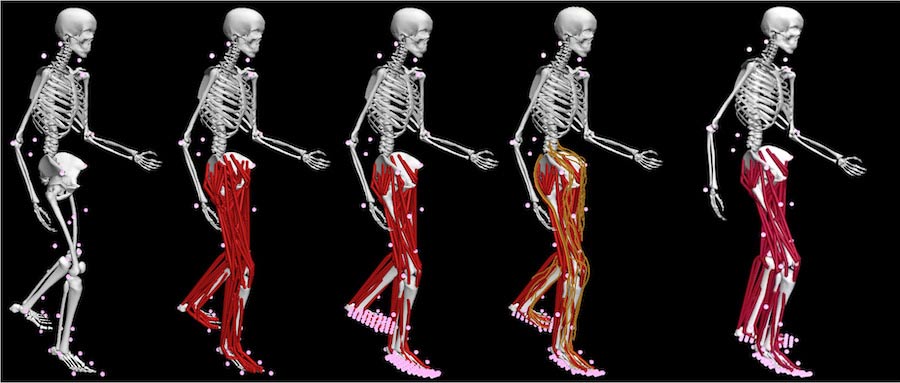
Schematic of the 4 steps involved in the model personalization process, from personalizing joint models, to muscle-tendon models, to ground contact models, to neural control models, resulting in a final personalized model that can be used to predict the patient’s posttreatment walking function. Image courtesy of the Fregly group/Rice University.
A team of Rice University engineers has launched a first-of-its-kind, open-source software that constructs and uses personalized computer models of how individual patients move to optimize treatments for neurologic and orthopedic mobility impairments. Funded by a grant from the National Institutes of Health, the Neuromusculoskeletal Modeling (NMSM) Pipeline software developed by B.J. Fregly, PhD, and collaborators in the Rice Computational Neuromechanics Lab is now available to clinician/engineer teams that would like to utilize computer-aided engineering for clinical treatment design.
The software could be used to design orthopedic surgical plans, neurorehabilitation interventions, physical therapy regimens, and prosthetic devices that maximize recovery of lost function for patients with movement impairments caused by stroke, osteoarthritis, cerebral palsy, Parkinson’s disease, spinal cord injury, traumatic brain injury, limb amputation, and even some forms of cancer.
“Our software makes it easy to create a personalized computer model of a patient’s neuromusculoskeletal system using the patient’s pretreatment movement data, and it then uses that model to predict—and even optimize—the patient’s functional outcome for various treatment designs that a clinician wants to explore,” Fregly said. “Instead of relying on implicit, subjective predictions of a patient’s post-treatment function, clinicians working with engineers could use our software to make explicit, objective predictions, which could not only weed out ineffective or harmful treatments, but also generate highly effective unforeseen ones.”
The physics-based software integrates several different physiological models, including models of central nervous system control, muscle force generation, and metabolic energy expenditure. To encourage the research community to use the software, Fregly and his team are running a 4-year competition at the American Society of Biomechanics annual conference. The competition will challenge researchers to develop personalized treatments that improve walking function for 4 individuals who have had a stroke.
To access the software and learn more about the competition, visit https://nmsm.rice.edu/.






