By Fateme Pol, Zahra Khajooei, Sayed Mohsen Hosseini, Alireza Taheri, Saeed Forghany, and Hylton B. Menz
 It has been demonstrated that foot problems increase the risk of falls in older people.
It has been demonstrated that foot problems increase the risk of falls in older people.
Fear of falling has been described as ongoing concern about falling that ultimately limits the performance of daily activities. It is multifactorial in etiology, and common among community-dwelling older adults, with prevalence ranging from 26–55%. While fear of falling is associated with falls, the causal relationship is unclear and may be bi-directional, as the 2 outcomes share risk factors. One such risk factor is foot structure and function. The foot provides the only contact source while standing and walking, and it has been demonstrated that foot problems increase the risk of falls in older people. However, the associations between foot characteristics, fear of falling, and mobility have not been examined in detail. Therefore, building on their previous work, the study authors set out to investigate whether a comprehensive range of foot characteristics (covering the domains of foot posture, muscle strength, range of motion (ROM), tactile sensitivity, deformity, foot pain, and plantar pressure) have an association with fear of falling and mobility impairment in community-dwelling older people.
Methods
The cohort comprised 187 community-dwelling older adults (106 females) age 62–90 years (mean 70.5 ± 5.2) from Isfahan, Iran, who were recruited between April and November 2020. People were deemed ineligible for the study if they were unable to ambulate for at least 10m without an assistive device, scored < 7 for the Short Portable Mental Status Questionnaire, had diabetic foot syndrome, neurological diseases, or previously had lower extremity surgery.
Foot and ankle characteristics (foot posture, ROM, muscle strength, deformity, tactile sensation, pain, and dynamic function), fear of falling (Fall Efficacy Scale International (FES-I)) and mobility (Timed Up and Go (TUG) test) were measured. Multivariate linear regression analyses were conducted to identify variables independently associated with fear of falling and mobility.
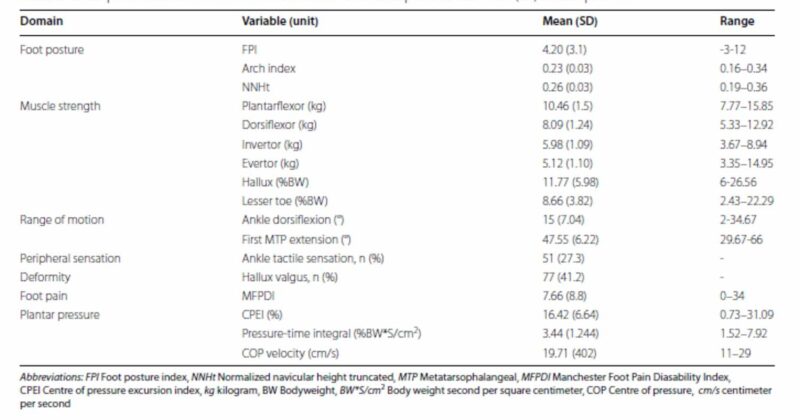
Table 1. Descriptive statistics for foot and ankle characteristics. Data presented as mean (SD) unless specified.
Foot posture was assessed using foot posture index, arch index, and normalized navicular height truncated. Isometric muscle strength of the ankle (dorsiflexion, plantar flexion, inversion, and eversion) was measured with a hand-held dynamometer. Hallux and lesser toe muscle strength were quantified by having participants push down as hard as possible on a pressure plate.
Two measures of foot and ankle passive ROM, passive ankle dorsiflexion, and hallux first metatarsophalangeal (MTP) joint extension were performed via a single standard video camera. Frame-by-frame advance was used to identify the instance of the maximum ROM. Hallux valgus was documented using the Manchester scale.
Tactile sensitivity at the ankle was assessed using a single Semmes–Weinstein-type pressure monofilament. The presence of foot pain was determined with the Manchester Foot Pain and Disability Index (MFPDI).
Foot function was assessed using barefoot plantar pressure analysis using the pressure plate and scientific software was used to calculate the pressure-time integral (PTI) in the total foot, center of pressure (COP) velocity of the total foot, and the center of pressure excursion index (CPEI), a measure of the mediolateral shift in COP throughout the gait cycle.
The Falls Efficacy Scale International (FES-I) was used to assess the level of concern of falling during 16 activities of daily living, including social activities. Mobility was assessed using the TUG test.
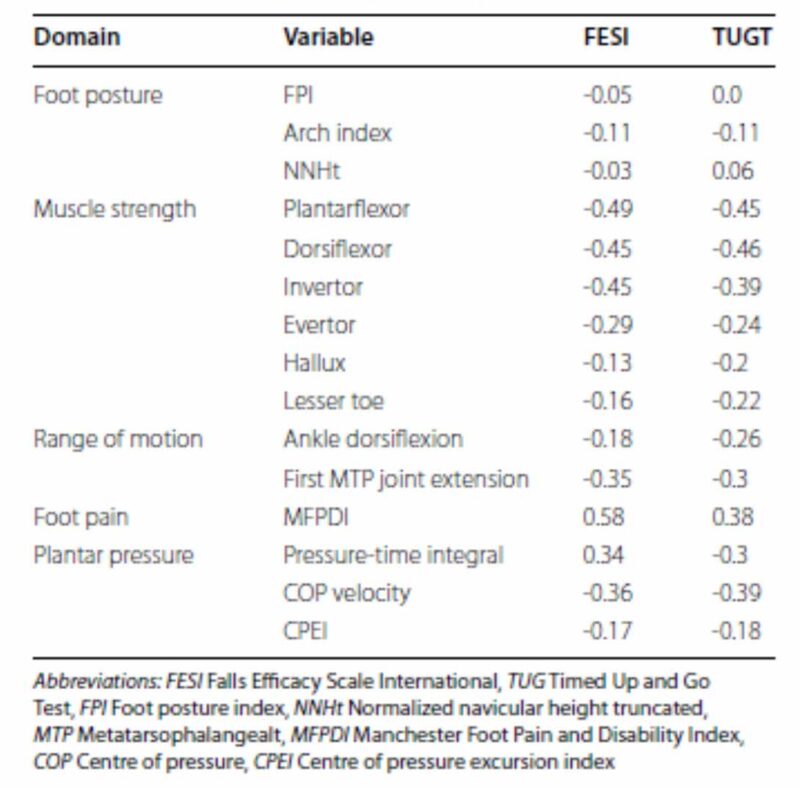
Table 2. Associations between fear of falling and mobility with foot and ankle characteristics (Pearson’s r).
Results
Of the 187 participants recruited into the study, 109 (58.6%) had poor visual acuity (using a 10% low-contrast letter chart), 40 (21.5%) used psychoactive medications, and 95 (51.1%) reported taking >4 medications per day.
Tables 1 and 2 show the associations between the foot and ankle characteristics with fear of falling and mobility performance on continuous (Pearson’s r) and dichotomous variables (independent sample t-tests), respectively. Independent sample t-tests revealed that participants who failed the ankle tactile sensation and vision test and use >4 medications per day scored worse on FES-I and TUG test (p < 0.001). FESI scores were worse in older adults who used psychoactive medications (p = 0.06).
Linear regression analysis revealed that less ankle plantar flexor muscle strength, greater pressure-time integral, foot pain, and reduced tactile sensitivity of the ankle were significantly and independently associated with increased fear of falling. The total variance explained by the model was 59%. Less ankle plantar flexor muscle strength, greater pressure-time integral, and slower center of pressure velocity were significantly and independently associated with poorer mobility. The total variance explained by the model was 48%. (Table 3)
Discussion
The study findings indicate that foot and ankle characteristics contribute to both fear of falling and impaired mobility in older adults. Decreasing plantar flexor muscle strength and increasing PTI, foot pain, and tactile sensitivity were significantly and independently associated with increased fear of falling. Independent associations between decreased plantar flexor muscle strength and increased PTI and decreased COP velocity with impaired mobility were observed.
The study results confirm that leg muscles play an important role in balance as ankle plantar flexor muscle strength was independently and significantly associated with the FES-I and TUG test.
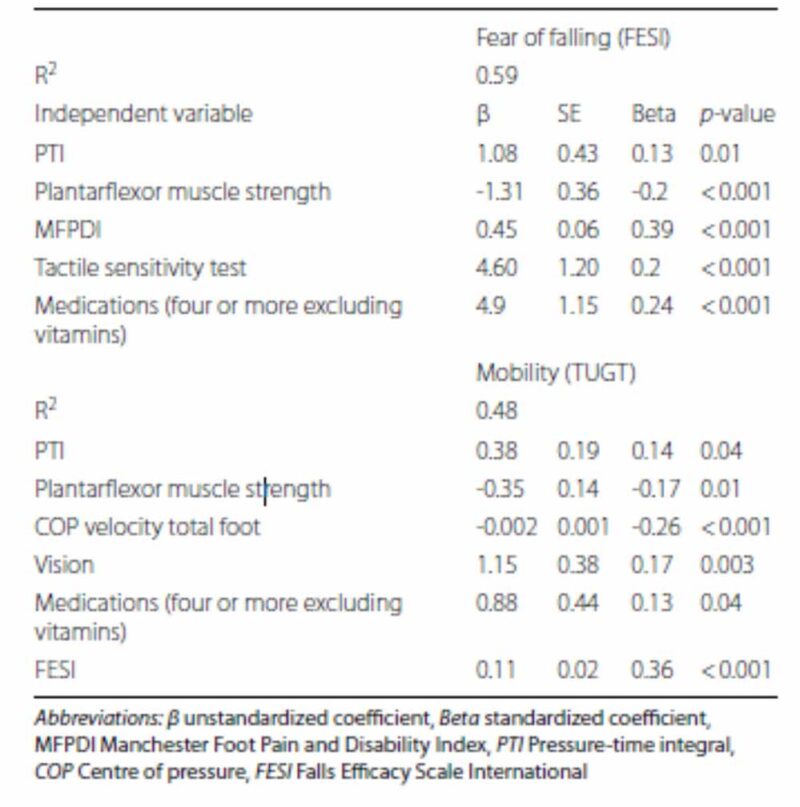
Table 3. Linear regression analysis showing an association between fear of falling and mobility (dependent variables) and foot and ankle characteristics (independent variables).
The association between plantar loading patterns during walking with fear of falling and mobility performance is a novel finding. The significant association between increased PTI with higher FES-I and TUG test scores is noteworthy. According to the study authors, the underlying mechanism for this is difficult to determine, but the greater duration and magnitude of plantar loading when walking may predispose to foot pain, which has been shown to impair balance and functional ability in older people. Alternatively, an increased PTI may be a reactive response to perceived instability to increase the duration of foot contact with the ground.
Foot pain was found to be independently associated with fear of falling. Clinicians working with older adults should therefore consider foot pain as an individual risk factor for fear of falling.
Older adults who failed the tactile sensitivity test scored worse in FES-I, and the results of the linear regression model showed that it has a strong association with the FES-I score. The integration of visual, vestibular, and somatosensory information is necessary to generate appropriate balance responses. Individuals rely primarily on proprioceptive and cutaneous input to maintain standing balance, and several studies have shown that age-related peripheral sensory loss is associated with increased postural sway and is an independent predictor of falls. The perceived loss of balance due to impaired tactile sensitivity may therefore induce fear of falling in older people.
The COP on the plantar surface of the foot reflects the progression of the whole-body center of mass during gait, therefore the forward velocity of the COP may potentially affect walking speed and sit to stand, the 2 components of the TUG test. The negative association observed between COP velocity and higher TUG test scores (indicative of poorer mobility) suggest that both walking speed and sit to stand, to some extent, require the same strategies in which the goal is to regulate speed and to remain upright during the transfer of bodyweight.
Conclusion
Foot and ankle characteristics, particularly plantar flexor weakness and higher plantar pressures when walking, are associated with fear of falling and mobility impairment in community-dwelling older people. Given that these characteristics are modifiable, clinical interventions such as foot strengthening programs, footwear, and foot orthoses may play a role in reducing fear of falling and optimizing mobility impairment in this age group when combined with other targeted interventions such as medication review, home hazard modification, and balance exercises.
This article has been excerpted from “Foot and Ankle Characteristics Associated with Fear of Falling and Mobility in Community-dwelling Older People: A Cross-sectional Study” J Foot Ankle Res 15, 86 (2022). https://doi.org/10.1186/s13047-022-00593-w. Editing has occurred, including the renumbering of tables, and references have been removed for brevity. Use is per CC Attribution 4.0 International License.








