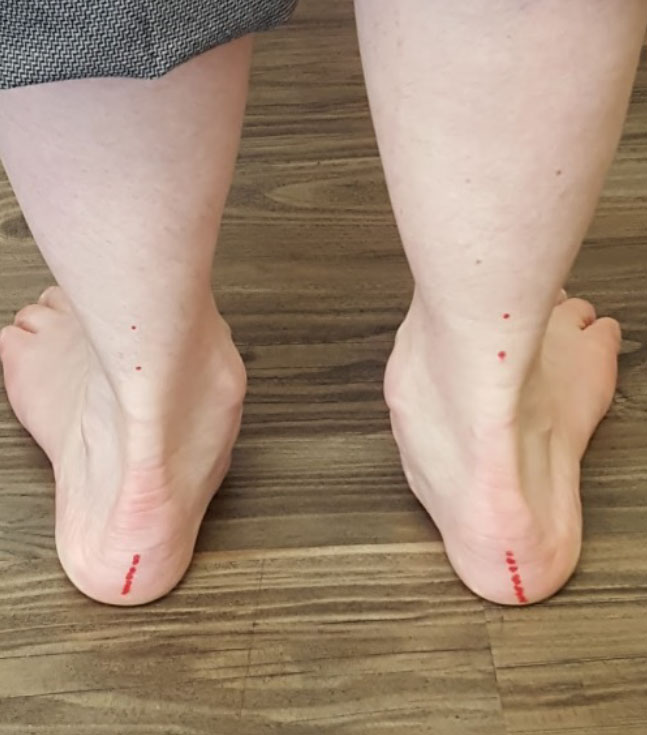
By measuring the relaxed calcaneal stance position we can get a feel for which foot is more pronated and treat with more correction.
By Richard Blake, DPM
One of the most perplexing issues I deal with in biomechanics is trying to take asymmetrical functioning bodies and make them more symmetrical when I think it will help the patient’s symptoms and function. However, asymmetry is part of who we are as people, so some thought has to be put into deciding exactly what needs to be changed because differences in biomechanics can cause chronic problems.
If you work with patients who are over 50 years old, you will spend incredible amounts of time trying to balance their foot function, balance their muscle strength and flexibilities, balance their short legs, etc. These imbalances tend to catch up with us in some fashion. A small asymmetry at the foot can become a big problem over the years. Yet, why are 95% of all orthotics I see prescribed symmetrical – including over-the-counter ones? They sure do not make our feet function that way.
Let us say that I correct for 5 degrees of pronation, for example, in a patient where one foot is 10 degrees everted in resting heel position and the other foot is 7 degrees everted in resting position (each degree at the foot is equivalent to 1/16th of an inch change in the average-sized patient). After the 5-degree change, one foot will now be 5 degrees everted and the other 2 degrees everted. The difference remains, although I agree we have moved the patient into a better position. When you simply take small differences in foot function (one more pronated than the other) combined with a short leg (80% of the population has a 1/16th inch or more discrepancy), along with the asymmetry produced by right-handedness vs. left-handedness, and then add an injury with some permanent weakness or stiffness, these differences easily become big issues. Why do you think 80% of all adults over 60 have back pain to some degree? It can’t all be blamed on prolonged sitting and poor mattresses. I know it has something to do with what we can treat as podiatrists. I have found it good practice to aim for stability, aim for symptom relief, aim for symmetry, and try to do it as naturally as possible. We have to try to motivate our patients to work harder for their health (not an easy task).
Complete Symmetry?
One of the main questions then is, do we want to make people completely symmetrical? It takes a little time to learn what motions and positions cause an individual’s problems. Sometimes the problems are permanently fixed, but the movement in medicine in general is to back off on full correction when the patient gets better. This does not apply to chronic conditions improved by orthotic devices or lifts for a short leg when that treatment brings complete or significant relief. These can also be congenital conditions like ligamentous laxity for which individuals will need stabilization their whole lives. Seeking symmetry is a goal that sometimes is needed to help someone completely resolve their problems. And sometimes, it is okay to accept asymmetry as long as the correction you have given has brought good symptom relief. However, I believe the patient should be part of the process and understand when lack of complete correction occurs. Years later, with some other problem, the patient – who may not even live in your area anymore – will remember that there could be more work to be done.
One classic example concerns treating the biomechanics of windswept feet. These are feet that pronate on one side and supinate on the other, as if the wind was blowing hard from the right or left and was about to sweep them off their feet in the frontal or coronal plane. The prescription must be asymmetrical to control the abnormal pronation on one side and abnormal supination on the other. Other common examples are patients with the residual mechanics of a partially corrected clubfoot on one side, or the sudden change from one side developing stage 2 or 3 posterior tibial tendon dysfunction or post-operatively the changes from almost any lower extremity surgery. This list is long.
Richard Blake, DPM, MS, is adjunct faculty at the California School of Podiatric Medicine. He has practiced podiatry at the Sports and Orthopedic Institute of St. Francis Memorial Hospital in San Francisco, CA. His book, Practical Biomechanics for the Podiatrist, Book 1, is available from Amazon.com and Barnesandnoble.com, as well as from the publisher at bookbaby.com.






