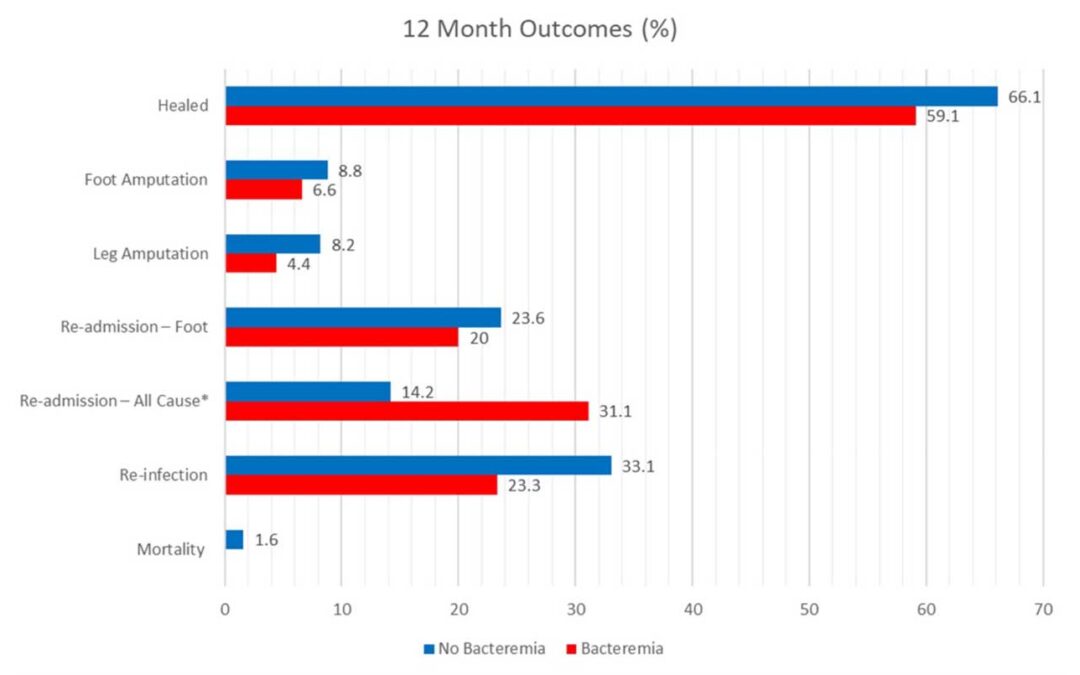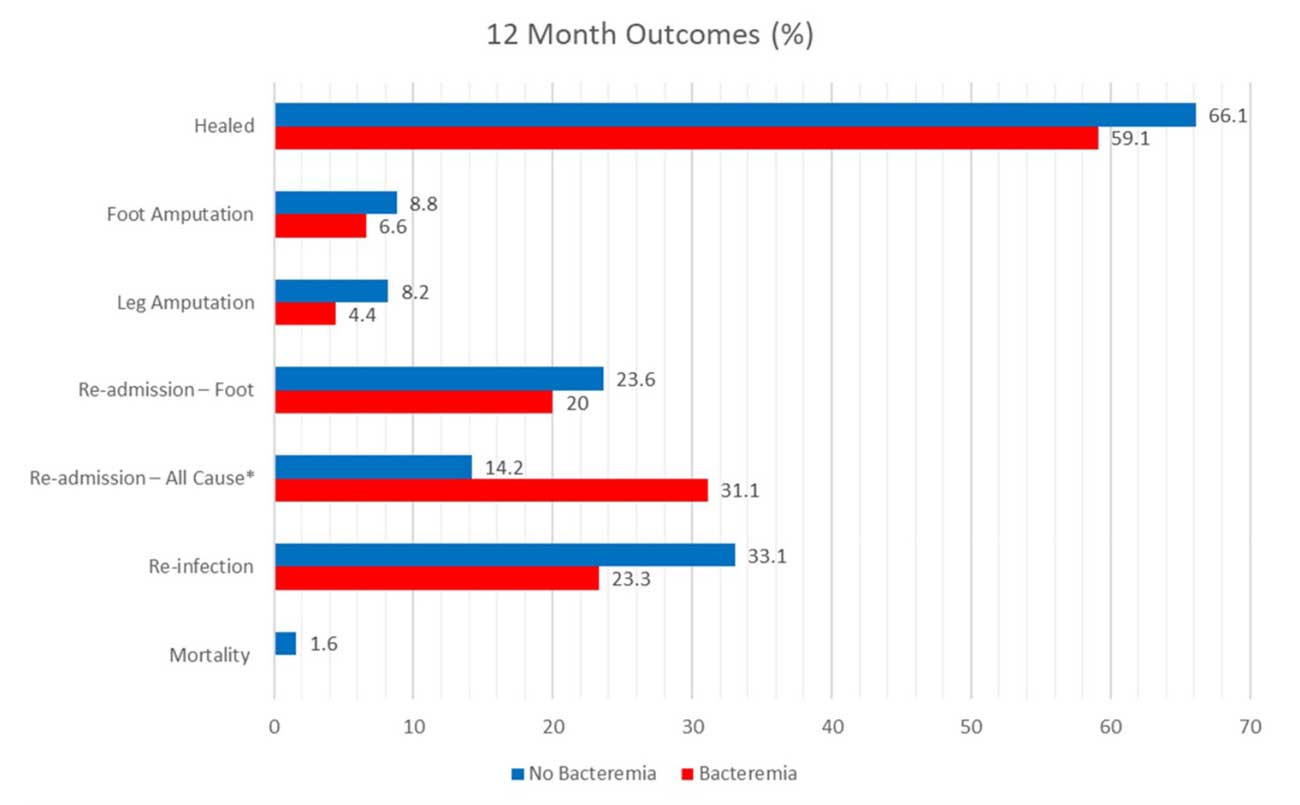
Outcome comparison in patients with bacteraemia or without bacteraemia. This bar chart compares the clinical outcomes in patients with bacteraemia to those without bacteraemia during the 12-month follow-up period after the index surgery. There was a significant difference in all cause readmissions. * is statistically significant.
Diabetic foot infections (DFIs) are one of the most important components causes for foot related hospitalization, surgery and lower extremity amputation. In addition to foot specific complications, DFIs are also associated with an increased risk of systemic complications such as acute kidney injury, central line infections, bacteraemia and endocarditis. This study aimed to identify the incidence of blood stream infections (BSIs) and endocarditis in patients with DFIs, risk factors and clinical outcomes. A post hoc analysis of 280 patients using pooled patient level data from 3 RTCs. Blood cultures were drawn at time of admission for DFI. Deep intraoperative cultures were obtained from infected foot wounds. Data from the 12-month follow-up were used to determine clinical outcomes. 77.1% (N = 216) had blood cultures of which 15.7% (n = 34) had BSI. One patient (3.3%) had endocarditis. Risk factors for BSI included Charcot Neuroarthropathy history (20.6% vs. 7.1%, P = 0.03), low systolic blood pressure (128.3 ± 21.0 vs. 140.8 ± 22.2 P = 0.003), low diastolic blood pressure (71.6 ± 9.4 vs. 79.3 ± 11.5 P <0.001), leucocytosis >12 000 (55.9% vs. 29.1%, P = 0.002) and elevated C-reactive protein (CRP) (26.8 ± 31.2 vs. 12.0 ± 19.6, P <0.001). During the index hospitalization, BSI patients had longer median hospitalizations (14.0, 11.3–18.0 vs. 12.0, 9.0–16.0, P = 0.04). At 12-months, BSI patients were more likely to be admitted to the hospital (all cause hospital admissions 35.3% vs. 18.6%, P = 0.03). There was no difference in re-infection (20.6% vs. 32.9%, P = 0.21), foot-specific hospitalizations (17.6% vs. 22.5%, P = 0.65), wounds healing (64.7% vs. 67.5%, P = 0.88), time to heal (221.0, 74.0–365 vs. 109.5, 46.8–365, P = 0.16) or antibiotic duration (46.0, 39.3–76.5 vs. 45.0, 22.3–67.0, P = 0.09). The most common BSI pathogens were Staphylococcus aureus (79.4%) and Streptococcus spp. (50.0%) species. BSI is common in DFIs. Patients have longer hospitalizations and were more likely to be hospitalized after their initial discharge.
Source: Reyes MC, Tarricone AN, Sideman MJ, Siah MC, Najafi B, Peters EJG, Lavery LA. The infected diabetic foot: bacteraemia and endocarditis complicating moderate and severe foot infections. Int Wound J. 2025;22(5):e70102. doi: 10.1111/iwj.70102.