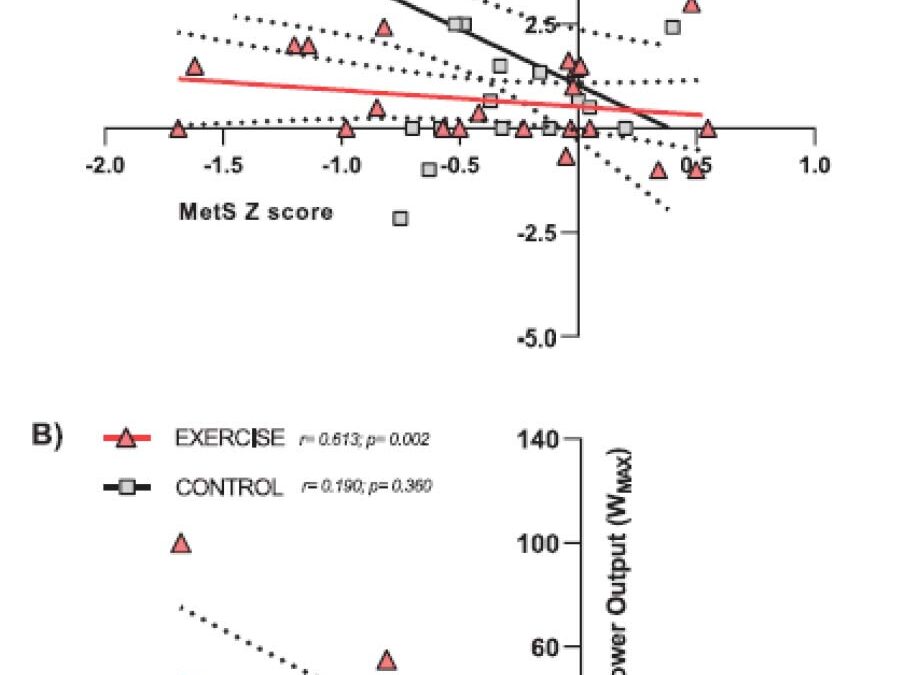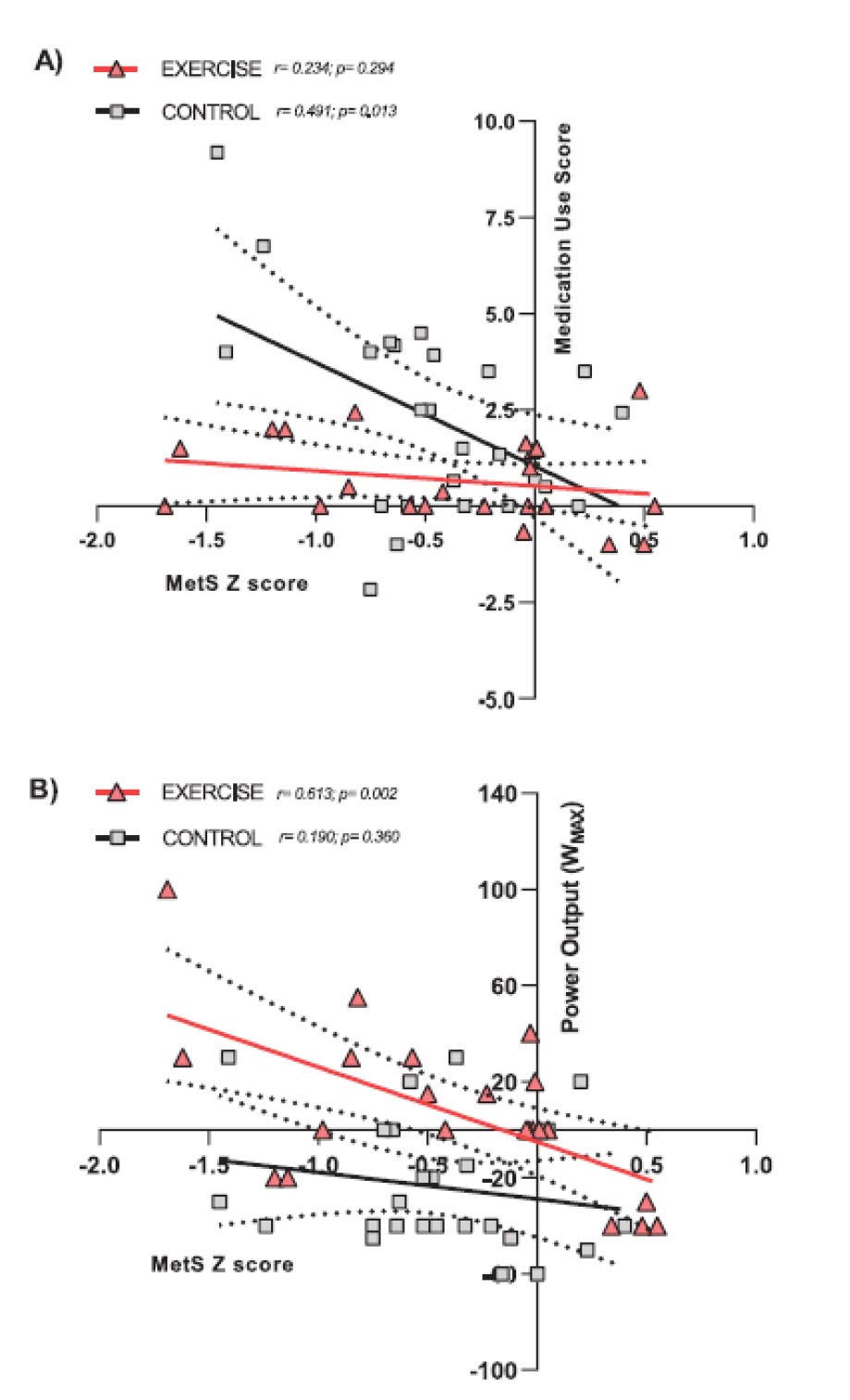
Figure. Pearson correlation between improvements in MetS Z score (Δ MetS Z score) after 8 years of follow-up and changes in medication use score (Δ medication use score [A]) and WMAX (Δ power output [B]) in the EXERCISE and CONTROL.
Metabolic syndrome (MetS) is a set of 5 cardiometabolic risk factors including obesity and Type 2 diabetes, that typically worsen with age. One exercise-training program is effective at improving those factors in middle-aged individuals with MetS. This study determined the effectiveness of a periodized exercise training program for individuals with MetS after a follow-up period of 8 years.
Forty-seven individuals with MetS were block-randomized into an EXERCISE (n = 22, 52 ± 8 years old, 23% women) or a CONTROL group (n = 25, 53 ± 8 years old, 32% women). Both groups received standard health care, including medical counselling and lifestyle advice at least every 6 months, while participants in EXERCISE also underwent a supervised exercise program. The intervention lasted 8 years and consisted of 4 months per year (November to March) of high-intensity interval training thrice weekly. At baseline, and after 4 and 8 years of treatment, researchers assessed body composition, MetS components (ie, MetS ≥ score), medication use, cardiorespiratory fitness (CRF; assessed by VO2MAX) and maximal leg cycling power output (WMAX).
Results: Paradoxically, MetS Z score and body weight were reduced after 8 years (participants aged from 52 to 60 years old) in both groups (time effect P < 0.001 and P = 0.008; time × group interaction P = 0.253 and P = 0.130). However, in those 8 years, the medicine use score increased threefold in CONTROL (137% increase; from 1.7 to 3.9; P < 0.001) while it did not change in EXERCISE (33%; from 2.0 to 2.7; P = 0.066). In 8 years, CRF and WMAX increased in EXERCISE by 14% (3.4 ± 5.6 mL±kg−1 • min−1) and 4% (7 ± 37 W) while decreasing in CONTROL by −7% (−1.6 ± 3.4 mL±kg−1 • min−1) and −14% (−24 ± 27 W) being different between groups after 4 and 8 years (both time × group interaction P = 0.002). Pearson correlations showed that MetS Z score improvements were significantly associated with increases in medication use score in the CONTROL group r = 0.491; P = 0.013) and with WMAX enhancement in the EXERCISE group (r = 0.613; P = 0.002).
On closer analysis, the researchers concluded that the data revealed that the nonexercising CONTROL group reduced their MetS Z score at the expense of tripling their oral medication. This provides evidence of a worsening of their disease that had to be compensated by increasing pharmacological therapy. On the other hand, the EXERCISE group did not need to increase medication in 8 years to improve their MetS. The factor that better predicted MetS evolution was leg cycling power in the EXERCISE group while it was medicine use score in the CONTROL group (Figure). In summary, this data suggest that individuals with cardiometabolic disease, who do not exercise regularly as they age, render the control of their disease to pharmacological treatment alone. Lastly, our data suggest that exercise training has similar clinical power to tripling oral medication to control MetS as individuals age 50 to 60 years.
Source: Morales-Palomo F, Moreno-Cabañas A, Alvarez-Jimenez L, Mora-Gonzalez D, Mora-Rodriguez R. Long-term effects of high-intensity aerobic training on Metabolic Syndrome: an 8-year follow-up randomized clinical trial. J Cachexia Sarcopenia Muscle. 2025;16(2): e13780. Doi: https://doi.org/10.1002/jcsm.13780