Aquatic walking can help relieve arterial stiffness among patients with peripheral artery disease (PAD), according to results from a clinical trial published in the Journal of Applied Physiology.
The study also showed that aquatic walking boosts patients’ ability to tolerate exercise, cardiorespiratory capacity, and muscular strength, and that patients are largely more inclined to maintain this exercise regimen. That abets the notion that aquatic walking could be a new and, potentially, more comfortable type of exercise aimed at treating and preventing flareups of the condition.
Participants in the trial were recruited from community health centers in South Korea, made up primarily of females. Participants, all women, were classified as Fontaine stage I or II PAD with an ankle brachial index (ABI) of 0.7–0.9. They were sedentary, which was defined as less than 1 h of regular exercise participation per week within the previous year. To avoid the impact of secondary diseases, current smokers, as well as those with psychiatric conditions and pulmonary, renal and thyroid diseases, were excluded. However, the study did include participants with diabetes mellitus, hypertension, dyslipidemia, heart failure, previous myocardial infarction and knee and/or hip arthritis.
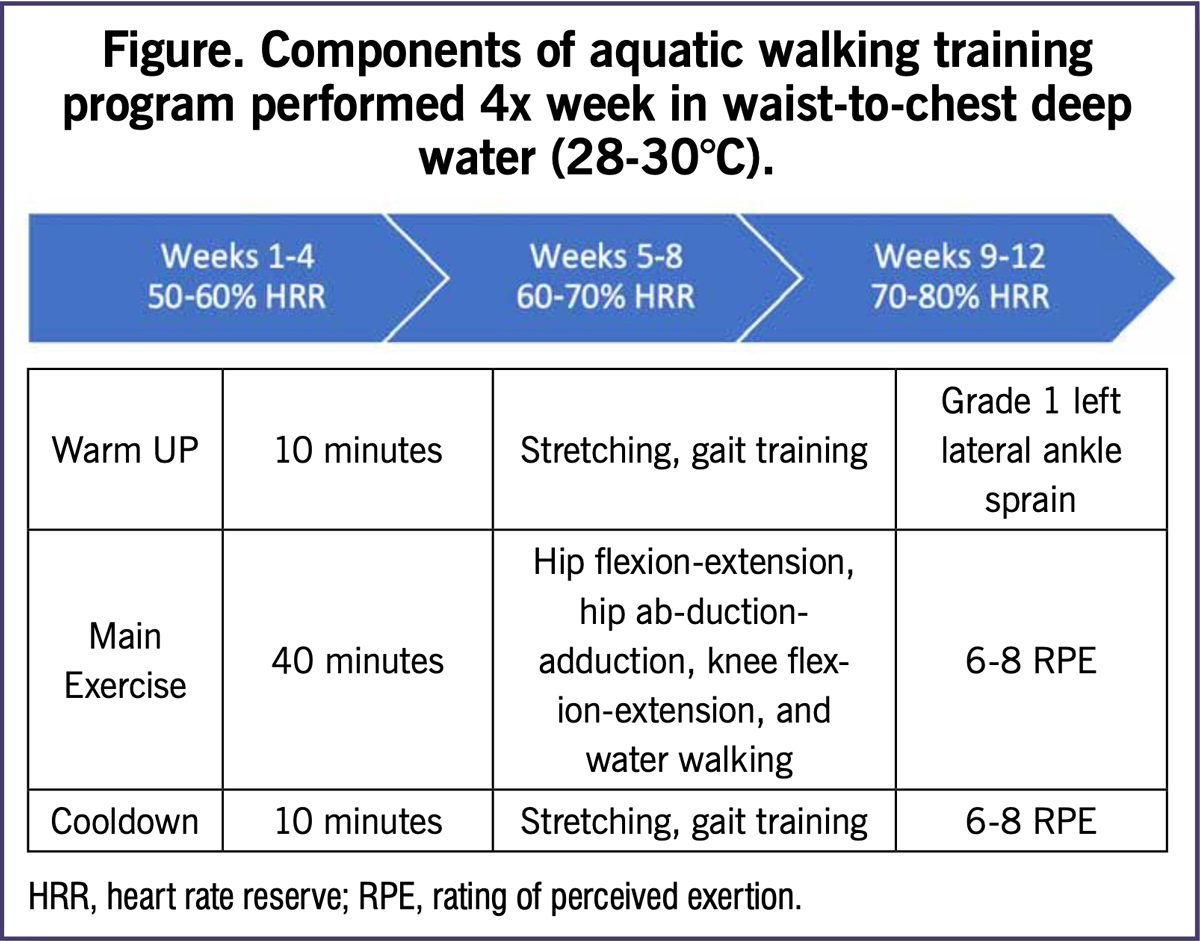
Baseline measures included arterial stiffness, resting heart rate (HR), blood pressure, ABI, VO2 max, 6-minute walking distance, physical function scores, handgrip strength, leg strength, anthropometrics, resting metabolic rate, and flexibility. Participants were then randomly assigned to either a 12-week aquatic walking training group (AQ, n = 35) or a control group (CON, n = 37). Members of the AQ group did walking and leg exercises at progressively increasing intensities four times a week in waist-to-chest deep water, 28-to-30-degree Celsius (see figure). CON group members did not partake in an exercise program, but were present in the lab at the same times as the AQ group was in the pool.
The trial was completed by 72 of the participants with no symptoms or adverse side effects stemming from the training program reported. Additionally, following training, self-reported physical function, a marker of quality of life, showed significant improvement.
The 12-week data showed significant improvements compared to pre-exercise (*P > .05) for the AQ group in several areas:
- legPWV, change (∆) − 2.6 + – 0.7 m/s*
- resting HR, ∆ -2.3 + – 1.4 beats/min*
- VO2 max, ∆ 2.4 + – 1.0 mL . kg−1 · min−1*
- 6MWD, ∆ 50.0 + – 8.0 m*
- physical function score, ∆ 6.0 + – 9.0%*
- handgrip strength, ∆ 1.2 + – 0.1 kg)*
- leg strength, ∆ 1.9 + – 9.1 kg*
The authors also found a moderate association between VO2 max and 6MWD and a weak-to-moderate association between legPWV and 6MWD in the AQ group, suggesting that changes in arterial stiffness may be related to the increased walking distance.
“Although PAD is very prevalent worldwide, no pharmacological treatment has been developed – and only surgical treatment has been used in the severe condition,” said the trial’s second author, Liz Pekas, MS, CSCS, EP-C, University of Nebraska at Omaha, doctoral research assistant, Vascular Research Lab.
The authors observed that aquatic walking may be more comfortable as an intervention for these patients due to decreased joint loading and stress as well as increased muscle relaxation due to the warm temperature. Aquatic walking also addresses issues related to falls prevention in this high-risk population.
Source: Park SY, Kwak YS and Pekas EJ. Impacts of aquatic walking on arterial stiffness, exercise tolerance & physical function in patients with peripheral artery disease: a randomized clinical trial. J Appl Physiol. 2019;127(940-949).
Chuck Green is a freelance writer based in Chicago, Illinois.