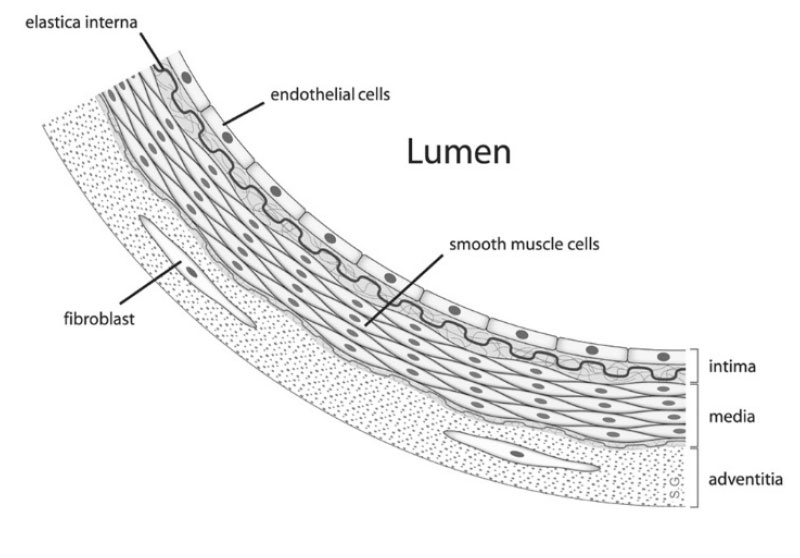
Figure 1. Vertical section of arterial wall reveals the location of endothelial cells. Image courtesy of DRosenback at English Wikipedia CC BY SA 3.0.
On March 11, 2020, the World Health Organization (WHO) characterized infection by COVID-19, caused by the severe acute respiratory syndrome coronavirus (SARS-COV-2), as a pandemic. Worldwide, countries have issued stay-at-home orders of varying degrees, in an effort to stem the spread of the virus and “flatten the curve” on its rising death toll, as well as to prevent the collapse of healthcare systems globally. In response to the profound economic fallout, some countries have slowly begun to reopen. With no vaccine available and limited understanding of the disease itself, the question asked by public health experts is not when the second wave will strike but: How lethal is this virus?
SARS-COV-2 is a novel coronavirus; the human physiologic response has been difficult to tease apart in the rush to save lives. Research is underway on multiple fronts in the search for appropriate testing methods, treatment options, vaccines, and basic clinical care. This is an evolving situation; every day, we learn more about how the virus spreads and its impact on the human body. Here’s a quick recap what we know so far and what’s being done to move things forward.
Person-to-person Spread
According to the US Centers for Disease Control and Prevention, COVID-19 is thought to spread mainly through close, person-to-person contact from respiratory droplets. Unlike prior human contact with coronaviruses—SARS and MERS (Middle East Respiratory Syndrome)—COVID-19 is more easily transmitted, and might even be transmitted by asymptomatic or presymptomatic people. That means people who don’t know they are infected could be infecting others as they go about their daily activities, which is why social distancing is a crucial part of the strategy to combat the spread of the virus. New guidelines about the need to wear a mask are also part of the strategy.
It appears that SARS-COV-2 is spreading easily and sustainably between people. Data collected from numerous countries suggest that this virus is spreading more efficiently than influenza, although not as efficiently as measles, which is highly contagious.
Because COVID-19 is a new disease, information regarding risk factors for severe illness is limited. Based on available information and clinical expertise, older adults and people of any age who have any one or more of several serious underlying medical conditions might be at higher risk of severe illness. Key underlying conditions that raise that risk include cardiovascular disease, diabetes, chronic lung disease, chronic kidney disease treated with dialysis, and liver disease. This list is preliminary, however, and is undergoing constant refinement. Although asthma was included on the original list, it has fallen off; at press time, increased scrutiny is on cardiovascular disease.

Figure 3. Left: Heel of a COVID-19-positive 30-year-old. Right: Toes of a 16-year-old who had 2 family members who tested positive for COVID-19 7 days earlier. Images courtesy of Maria del Mar Ruiz Herrera and COVIDFootRegistry.com.
“Unique Clotting”
While the respiratory symptoms of COVID-19 infection are well known, other significant disease manifestations are coming to light as the pandemic continues and more people are infected—and, sadly, as more autopsies are completed. As Deborah Birx, MD, US Global AIDS Coordinator and a key leader on the US Coronavirus Task Force, told CNN’s Jake Tapper on April 24, 2020, there are “unique clotting” issues associated with COVID-19 infection that need investigation.
The clotting problem has been reported anecdotally to date, but new studies are emerging daily about the impact of COVID-19 on the peripheral vascular system, which is of particular importance to LER readers.
Writing in The Lancet Online First, Varga and global colleagues described endothelial-cell involvement across vascular beds of various organs in multiple patients with COVID-19 infection. They found evidence of viral infection of endothelial cells and diffuse endothelial inflammation, which can result in systemic endothelial dysfunction. Such dysfunction is “a principal determinant of microvascular dysfunction by shifting the vascular equilibrium toward more vasoconstriction with subsequent organ ischemia, inflammation with associated tissue edema, and a pro-coagulant state.”
Varga goes on to say:
Our findings show the presence of viral elements within endothelial cells and an accumulation of inflammatory cells, with evidence of endothelial and inflammatory cell death. These findings suggest that SARS-CoV-2 infection facilitates the induction of endotheliitis in several organs as a direct consequence of viral involvement (as noted with presence of viral bodies) and of the host inflammatory response. In addition, induction of apoptosis and pyroptosis might have an important role in endothelial cell injury in patients with COVID-19. COVID-19-endotheliitis could explain the systemic impaired microcirculatory function in different vascular beds and their clinical sequelae in patients with COVID-19. This hypothesis provides a rationale for therapies to stabilize the endothelium while tackling viral replication, particularly with anti-inflammatory anti-cytokine drugs, ACE inhibitors, and statins. This strategy could be particularly relevant for vulnerable patients with pre-existing endothelial dysfunction, which is associated with male sex, smoking, hypertension, diabetes, obesity, and established cardiovascular disease, all of which are associated with adverse outcomes in COVID-19.

Figure 2. The toes and heel of a 13-year-old boy with unique skin manifestations 2 days before he was given a diagnosis of COVID-19 infection. Images courtesy of Francesco Mazzotta and COVIDFootRegistry.com.
Clinical Observations
Scattered reports suggest early manifestations of COVID-19 infection occur in the peripheral limbs and, in particular, in the feet of children and young people (median age, 13 years) prior to the appearance of other symptoms. In a recent commentary in the International Journal of Dermatology, Landa and colleagues explained that these chilblain-like lesions include erythematous and papular lesions, acral lesions with crusting, and erythematous-violaceous lesions. Patients might describe them as rash, redness, irritation, or bruising. These skin issues can be painless or painful and can itch or cause burning. Timing of the appearance of these skin manifestations is uncertain: some case reports, such as Landa, cite these as post-COVID-19 infection whereas others report they appear pre-diagnostically or in asymptomatic patients.
Mazzotta, an Italian dermatologist, published one of the first cases of manifestations of COVID-19 infection in the feet with the International Federation of Podiatrists (availabe at https://www.fip-ifp.org/news/covid-19/). Disease occurred in a 13-year-old boy. He had skin manifestations on the foot prior to other symptoms of COVID-19 infection; 2 days after the photographs in Figure 2 were taken, the boy tested positive for COVID-19. Mazzotta provided these additional photographs, not published in his case study, to COVIDFootRegistry.com to alert clinicians to potential COVID-19 manifestations in the feet, prior to actual diagnosis.
Herrera, a podiatrist in Spain, shared photographs of 2 patients from her practice (see Figure 3). At left is the heel of a COVID-19-positive 30-year-old. At right are the toes of a 16-year-old who had 2 family members test positive for COVID-19 the week before onset of these skin manifestations.
COVID-19 Foot Registry
To facilitate understanding of the effects of COVID-19 infection on the feet, Michael Nirenberg, DPM, a forensic podiatrist, and a distinguished Expert Advisory Board have launched the COVID-19 Foot Registry. Available at COVIDFootRegistry.com, its mission is to gain insight into the signs and symptoms of COVID-19 in the feet and toes (“COVID toes”); its goal is to improve treatment and prevention of COVID-19 infection with the hope that this knowledge might be useful in addressing future viral disease outbreaks or recurrent COVID-type occurrences.
“In this unprecedented health crisis, all of us must do what we can,” said Nirenberg, the registry’s founder and director. “This Registry may, in a small way, lead to knowledge that helps us fight this disease. But, even if no relationship between COVID-19 and our feet is found, that may be useful to know too.”
The registry is asking for photographs of skin manifestations in and information about persons who have, or might have, COVID-19 infection, which can be provided from physicians, podiatrists, dermatologists, healthcare workers, researchers and individuals, including patients. Submitters need to ensure their authority for submission and de-identification of any Protected Health Information (ie, submission must be HIPAA-compliant).

Source: Rogers LC, Lavery LA, Joseph WS, Armstrong DG. All feet on deck—the role of podiatry during the COVID-19 pandemic: Preventing hospitalizations in an overburdened healthcare system, reducing amputation and death in people with diabetes. JAPMA. 2020; https://doi.org/10.7547/20-051. Table used with permission of the American Podiatric Medical Association. All rights reserved.
Among the specialists assisting in this effort is Congressman Brad Wenstrup, DPM. Wenstrup serves as the US Representative for Ohio’s 2nd Congressional District and is one of only a few representatives in Congress with medical expertise. Other members of the Advisory Board include:
- Lawrence Harkless, DPM, interim dean at the University of Texas Rio Grande Valley’s School of Podiatric Medicine
- David Armstrong, DPM, MD, PhD, professor of surgery and director of the Southwestern Academic Limb Salvage Alliance (SALSA) at the Keck School of Medicine at the University of Southern California
- Rock G. Positano, DPM, MSc, MPH, DSc, associate clinical professor of chronic disease epidemiology at the Yale School of Medicine at Yale University
- Bret Ribotsky, DPM, orthopedic surgeon; past president, American College of Foot & Ankle Orthopedics & Medicine; founder, DermFoot, LLC; and founder, Podiatric Success—Meet the Masters
- Marta I. Rendon, MD, international researcher and lecturer in dermatology; clinical associate professor at Florida Atlantic University, an affiliate of the University of Miami School of Medicine
- Marc Brenner, DPM, past president, American Society of Podiatric Dermatology
“We all need to work together to conquer this disease,” said Brenner, who serves as chair of the Registry’s Advisory Board. “I think we are going to find something important. Something that will make a difference. But we need the public’s help.” Brenner joined Nirenberg early in the project to create a registry, after he consulted on a young patient with odd skin lesions and suspected COVID-19 infection. He emphasized that some medical registries are accessible only by physicians but that, due the seriousness of COVID-19, this foot registry is accessible by anyone.
The Registry will collect data and information, and intends to publish and disseminate findings. The Advisory Board has volunteered its time. The Registry is funded by Nirenberg’s podiatry practice.
“I initially hoped the government or a big organization would put up a foot registry, but that wasn’t happening. I didn’t feel this should wait. This is too important.”