www.istockphoto.com #13413701
Devices that improve proprioception, balance, and biomechanics can help patients avoid the significant morbidity and mortality associated with falls. In some cases, however, a device may actually increase the risk of falling. That’s why matching the right intervention to the right patient is essential.
by Cary Groner
Anyone who’s ever slipped on ice knows that falls can bruise more than just your dignity. But for older adults, those with sensation loss due to diabetic neuropathy, or people who use prosthetic or orthotic devices, falls routinely cause serious injuries including broken bones, concussions, and even death. Moreover, those who use devices such as prosthetic knees soon discover that the devices may either raise or lower the risk of falls, depending on how they are designed and used.
“Clinicians should evaluate not just the condition we’re treating, but the potential for a given device to either enhance or decrease postural control and potentially contribute to the risk of falling,” said Douglas Richie, DPM, owner of Seal Beach Podiatry in Seal Beach, CA, and associate clinical professor in the Department of Applied Biomechanics at the California School of Podiatric Medicine in Oakland. “In some cases, we might want to prescribe a device with ankle-joint motion rather than a solid AFO that restricts motion.”
Stats paint grim picture…

www.istockphoto.com #14632712
Most of the available statistics relate to falls in older people. The risks of falling and being injured increase with age, according to the Centers for Disease Control (CDC).1 One in three adults over age 65 falls each year, and the rate of serious injury is four times higher in those over 85 than in those aged 65 to 74. In 2007, more than 21,700 Americans died due to falls, according to the National Safety Council;2 of these, roughly 18,000 were older adults.
In 2000, direct medical costs related to falls totaled more than $19 billion—a figure that is projected to top a staggering (so to speak) $54 billion by 2020. Most of this expense is related to nonfatal fall injuries, which may entail hospitalization, surgery, and lengthy rehabilitation. Of fatal falls, the most common and costly are traumatic brain injuries, and trauma to the hips, legs, and feet, which together account for 78% of deaths and 79% of fatal-fall costs.
…and it’s not just the elderly
Biomechanical studies, too, have focused largely on the elderly, and it isn’t yet clear to what extent they can be extrapolated to younger, stronger subjects such as soldiers returning from war fitted with prosthetic limbs. However, researchers are turning more of their attention to such populations, and in any case there is overlap because older people comprise a significant population of O&P device wearers.
“It’s reasonable to assume that many of the factors that increase fall risk in the elderly will apply to O&P populations,” said Matthew Major, PhD, a postdoctoral fellow at the Northwestern University Prosthetics-Orthotics Center in Chicago.
Fall risks are magnified in amputees, research indicates. In a 2001 paper published in Archives of Physical Medicine & Rehabilitation, researchers at the University of British Columbia reported that 52.4% of lower extremity amputees reported having fallen in the previous year.3 Analysis revealed that fall risk was particularly associated with having an above-knee amputation, back and joint pain, and multiple residual limb and prosthesis problems. Of above-knee amputees, two-thirds report falling annually—twice the rate in able-bodied adults over age 65.4
The biomechanical forces involved in falls are similar in all populations regardless of age. What separates the groups—those who recover after a slip versus those who fall and break a hip—has more to do with reaction time, muscle strength, and comorbidities such as loss of proprioception, poor vision, or vestibular dysfunction.5
Trips and slips
“Basically, a person falls when their center of mass is outside their base of support,” said Kenton Kaufman, PhD, who is the W. Hall Wendel Jr. Musculoskeletal Research Professor, and director of the Biomechanics/Motion Analysis Laboratory, at the Mayo Clinic in Rochester, MN. “A more sophisticated analysis looks at the extrapolated center of mass—that is, not only the position but also the velocity of the center of mass relative to the base of support. If the velocity will take the center of mass back into the base of support, you can still avoid the fall. The important things are neuromuscular control—how quickly you can respond—and strength.”
Our bodies know instinctively what to do when a fall threatens; we shoot our hips forward or back, throw out our arms, and make adjustments with our feet. All of this happens immediately and without any conscious input. Analysis of the biomechanics of balance and falling, however, has helped shed light on exactly what happens when, and how to compensate when the system fails.
Generally, biomechanics researchers have investigated two primary causes of falls: slips and trips. (Contributing factors such as balance deficits and loss of sensory or proprioceptive input will be discussed separately.)
In slips, the foot in contact with the ground unexpectedly slides forward or sideways. In trips—which cause about half of all falls in older people—something impedes the non–weight-bearing foot as it moves forward in swing phase.6
The body has two primary approaches to recovering from trips.7,8 In the lowering strategy, the obstructed foot drops to the ground for stability while the other leg performs a recovery step. In the elevating strategy, the obstructed foot is lifted up over the impeding object and swung quickly forward to take weight.
“Where you position your leg will determine whether you’ve got your center of mass in front of your base of support or within it, and that determines whether you fall,” Kaufman said.
If the trip occurs early in swing phase, subjects typically use an elevating strategy, said Jeremy Crenshaw, MSc, a postdoctoral candidate in the Clinical Biomechanics and Rehabilitation Laboratory at the University of Illinois, Chicago. If the trip occurs later in swing, they’re more likely to use a lowering strategy.
Slips, which are the second most common gait-related mechanism for falls in the elderly, usually occur shortly after heel strike; recovery requires complex neural mechanisms to detect the sliding motion and quickly respond.6 Slips often result in injury because falling backward or sideways generates significant impact forces.
Fall risk from slipping is associated with factors that include faster gait speed, greater forward heel displacement, and a larger angle of the leg relative to the ground. When young adults slip, they typically respond with rapid (60 ms to 90 ms onset) postural adjustments involving large bursts of muscle activity—activation of the tibialis anterior, biceps femoris, and rectus femoris on the slipping leg—as well as increased flexion torque at the knee and extensor activity at the hip.6 Older people react with similar strategies, but with less speed and strength, making it harder for them to control the heel’s forward slide and recover from the body’s displaced center of mass.
Amputee strategies
Amputees have developed at least one unique response to near-falls. In addition to the lowering or elevating approaches to a trip, Kaufman and his colleagues have observed a third recovery strategy in their lab.
“If the prosthetic limb is obstructed, subjects lower it and step over the obstacle with the sound limb,” he said. “But if the non-prosthetic limb is obstructed, and
they don’t trust the prosthesis, they’ll transfer all their weight to the sound limb and hop several times.”
One reason a transfemoral amputee may not trust a prosthetic limb, Kaufman explained, is that if it’s suddenly obstructed, it may remain in swing phase and collapse when weight is put on it.
“Even if the limb switches to stance phase, it won’t offer resistance any greater than that for normal walking, whereas you and I would fire our muscles completely to hold ourselves stable,” he said.
The subject’s amputation level may affect such responses, as well. A study from the Netherlands, published in Gait & Posture last year, reported that unilateral transtibial amputees recovered from evoked forward falls just as well as able-bodied control subjects did, though the amputees did use slightly different strategies for the sound versus the prosthetic limb. When leading with the prosthetic limb, for example, they responded faster and took a longer step.9
A study of differences in postural responses to dynamic perturbations between transtibial amputee fallers and nonfallers, published in the Archives of Physical Medicine & Rehabilitation in 2009, reported that fallers relied more on visual input than nonfallers, and bore significantly more weight on their intact limb during perturbations.10
Sensorimotor issues
As noted earlier, the decline in sensory input associated with aging can contribute to fall risk. In particular, poor vision, reduced vibration sense and tactile sensitivity, a decline in proprioception and muscle strength, vestibular dysfunction, and diminished reaction times contribute significantly to the incidence of falls.6
Some of these problems may be present in other patient populations, such as people with diabetes. Diabetes patients with insensate feet due to neuropathy have a greater risk of falling than those with normal sensation; moreover, some research suggests that they may not respond to strengthening regimens as effectively as patients without neuropathy do.11 Diabetic neuropathy has also been associated with impaired ankle strength and poor balance recovery.12 In older patients with diabetes, those reporting a fall in the previous year were more likely than nonfallers to have neuropathy (86% vs. 56%), a higher threshold of vibration perception, slower gait velocity, lower muscle strength in the feet and ankles, and a higher incidence of bony prominences and prominent metatarsal heads.13 And Swiss researchers reported in 2009 that even in the absence of detectable neuropathy, patients with type 2 diabetes had decreased gait capacity and increased fall risk versus nondiabetic subjects.14
Lower extremity amputees become susceptible to falls not just for the reasons already noted having to do with prosthetic limbs, but because of the loss of sensory information associated with their injuries.
“Amputees must compensate for a significant loss of sensory information that would otherwise be provided by an intact physiological structure,” Matthew Major said.
Surprisingly, unilateral lower extremity amputees have diminished somatosensation in both the residual limb and the sound limb, according to Major.
“It’s counterintuitive,” he acknowledged. “You’d expect that sensation would either remain the same or that, due to plasticity mechanisms, the sound limb would become hypersensitive to compensate for sensory loss in the residual limb. Strangely, this seems not to be the case.” Researchers have documented the phenomenon but aren’t sure why it occurs.15
Major noted several other neurophysiological factors that put amputees at greater risk for falling. For example, unilateral below-knee amputees place heavy demands on the muscles of their residual limb during walking to maintain stability, body support, and forward propulsion; as a result, weakness in that limb may increase their fall risk by reducing their ability to generate sufficient forces beneath the prosthesis to redirect their center of mass when necessary.16-18
Thank your ankles
Doug Richie emphasized that clinicians must carefully assess fall-related risk factors in each patient before making decisions about assistive devices. A number of individual pathologies may compromise balance, proprioception, and postural control, and these must be taken into account if interventions are to improve matters rather than make them worse.
According to a presentation Richie made at the annual conference of the American Podiatric Medical Association in Seattle last August, these variables include ankle ligament tears and insufficiency; degenerative joint disease of the ankle, subtalar joint, and midfoot; adult acquired flatfoot; peroneal, Achilles, or tibialis anterior tendinopathy; and Charcot deformity or ulceration.19 Neuromuscular control, in turn, may be compromised by pain, loss of proprioception from joint mechanoreceptors or muscle-tendon stretch receptors, and loss of sensory input from plantar mechanoreceptors.
Nevertheless, the body does its best to compensate and maintain balance through redundant biomechanical, neurological, and vestibular strategies. One example, Richie explained, is the stretch feedback mechanism.
“As the body sways, the Achilles or other tendons around the ankle get stretched,” he said. “Through the tendons or the muscle spindles, they send feedback to the central nervous system that a stretch is occurring. This gives clues about body sway and stimulates muscle firing to correct postural alignment.”
When the body sways, Richie explained, feedback is provided from the eyes all the way to the soles of the feet. Research has demonstrated, for example, that foot somatosensation is critical to detecting and responding to slips.20 When the muscle-tendon stretch reflex engages, one result is the “ankle strategy” to correct alignment. “Here’s the problem, then,” Richie said. “When you put a patient in a solid AFO, you’re eliminating the feedback from the muscle spindles and inhibiting the ankle strategy response. For a patient with diabetic neuropathy, there’s no question that you’re putting them at further risk for falling.”
Some research does suggest that the right AFO design in the right patient can improve balance. Although this theoretically would seem to imply a reduced risk of falls, that remains to be demonstrated.
“ I’ve never seen a study proving that AFOs reduce the risk of falls, because most are studies on postural control, not falling,” Richie said.
A systematic review published in the Journal of Prosthetics & Orthotics last year concluded that while sports AFOs were unlikely to compromise balance when used prophylactically in normal populations, the effect of ambulatory AFOs on balance depended on design. Under dynamic conditions, rigid AFOs compromised balance; by contrast, leaf-spring AFOs, which allowed sagittal-plane motion, seemed to facilitate both static and dynamic balance.21
When an AFO is deemed necessary, clinicians should provide patients with counseling, advice (care going down stairs and getting rid of throw rugs are always high on the list), and a cane, which allows the hand to become a proprioceptor, Richie said.
“Clinicians need to evaluate the potential of an AFO to either enhance or decrease postural control and contribute to fall risk,” he said. “For example, they may want to consider a device with ankle joint motion rather than a solid AFO.”
Foot orthoses look good, lack evidence
Research suggests that foot orthoses may improve balance by a number of mechanisms, including increasing the sensory receptive field, moving joints to more optimal positions, and reducing or increasing joint moments.22,23

www.istockphoto.com #14628732
Keith Rome, PhD, a professor of podiatry at the Auckland University of Technology in New Zealand, studies insoles and postural stability. He said that although the evidence isn’t yet as strong as he would like, there are indications that insoles could be particularly helpful for some patient groups.
“People with long-term neuromuscular and musculoskeletal problems may benefit from them,” he said.
In an article coauthored with Doug Richie, Rome noted that orthoses can augment the medial longitudinal arch, altering the muscular work involved in maintaining foot posture. They may also enhance afferent feedback from the plantar surface of the foot, help correct anatomical malalignment, stabilize the rearfoot, and limit excessive pronation. The problem, of course, is that although these effects improve postural stability, the evidence doesn’t yet support the contention that they also reduce fall risk.24
“This is a brand new area,” Rome said. “We’re doing studies now, but we’re still analyzing the data. Some studies have shown that textured insoles had an impact on some balance parameters, but not all.25 We don’t yet know the true impact of foot orthoses, including textured or contoured insoles, on fall prevention.”
Knee control

www.istockphoto.com #9570881
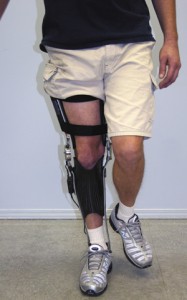
Stance-control orthoses, worn by patients recovering from joint trauma or those with lower limb paresis or paralysis, can be designed to engage upon knee collapse, theoretically providing support during a fall.26,27
“Stance-control orthosies provide stability during stance, so that should aid in fall reduction,” said Kenton Kaufman. “And allowing natural motion to occur is important so the patient can use inherent control strategies to prevent a fall, but few if any studies have looked at falls as a primary outcome in orthotic wearers.”
Evidence suggests that artificial knees with microprocessors may not only improve gait and balance but also decrease fall risk, however.28-30 In one study comparing artificial knee designs, falls decreased 64% when the knees contained a microprocessor.31
“If the non-prosthetic limb is obstructed, the prosthetic limb has to decide to remain in stance while the other limb steps over the obstacle, or you’re going to fall, so the control algorithm is going to determine how helpful the prosthesis is,” Kaufman said.
Because the artificial knee must also “decide” whether to remain in swing phase or switch to stance phase when it is the obstructed limb, accelerometers are now being tested to help with the implementation of advanced algorithms.
Other inteventions
In older people, exercise interventions including those for strengthening, balance, and agility training have been shown to decrease the risk of falling as well as the associated injury risk.6,32 Doug Richie recommends a program that includes reduction in postural sway, improvement in stability, increased use of sensory inputs for postural control, better ability to survive balance perturbations, and increased strength and endurance.19
At the University of Illinois at Chicago, Mark Grabiner, PhD, has reported that the ability to limit trunk motion—a skill subjects can learn—discriminates fallers from nonfallers.33 Grabiner, director of the school’s Clinical Biomechanics and Rehabilitation Laboratory, is collaborating with Kaufman and Marilynn Wyatt, PT, on a project in San Diego to teach fall prevention to U.S. Navy and Marine lower-extremity amputees recently returned from service in Iraq and Afghanistan.
“We’ve learned that with a specially designed treadmill, we can deliver a particular disturbance pattern that optimizes the body’s learning curve,” Grabiner said. “For each individual, we want to maximize the utilization of the available musculature and make sure subjects use their trunk and hip extensors, as well as plantar flexion, to restore trunk control.”
The researchers want to give their subjects the greatest possible range of strategies to prevent falls, and to increase their trust of their prostheses.
“Because the harness prevents them from actually falling, they’ll be able to explore the possibilities of the movement library, so to speak—what is possible with both the prosthetic and the nonprosthetic limb,” Grabiner said.
Ultimately, by reducing both the likelihood and the fear of falls, the approach may improve subjects’ quality of life and increase their options, whether they want to return to active duty or transition to civilian life.
“Better body armor has meant that blast injuries are less often lethal, but they’re really affecting the upper and lower extremities, which don’t have the armor,” Grabiner said. “These are ideal people to work with in a rehabilitation environment, because they really want to get better; if anything, we have to prevent them from pushing themselves too fast. The more of these injuries there are, the more important our mission becomes.”
Cary Groner is a freelance writer based in the San Francisco Bay Area.
References
1. Centers for Disease Control and Prevention. Falls among older adults: An overview. Available at: http://www.cdc.gov/HomeandRecreationalSafety/Falls/adultfalls.html Accessed February 25, 2011.
2. Centers for Disease Control and Prevention. Web–based Injury Statistics Query and Reporting System (WISQARS). Available at: http://www.cdc.gov/injury/wisqars Accessed February 25, 2011.
3. Miller WC, Speechley M, Deathe B. The prevalence and risk factors of falling and fear of falling among lower extremity amputees. Arch Phys Med Rehabil 2001;82(8):1031-1037.
4. Crenshaw J, Kaufman K, Grabiner M. Failed trip recoveries of above-knee amputees suggest possible fall prevention interventions. Presented at the annual conference of the American Society of Biomechanics, Providence, RI, August 2010.
5. Lockhart TE, Smith JL, Woldstad JC. Effects of aging on the biomechanics of slips and falls. Hum Factors 2005;47(4):708-729.
6. Lord S, Sherrington C, Menz H, Close J. Falls in older people. 2nd ed. New York: Cambridge University Press; 2007.
7. Eng JJ, Winter DA, Patla AE. Strategies for recovery from a trip in early and late swing during human walking. Exp Brain Res 1994;102(2):339-349.
8. Pavol MJ, Owings TM, Foley KT, Grabiner MD. Mechanisms leading to a fall from an induced trip in healthy older adults. J Gerontol A Biol Sci Med Sci 2001;56(7):M428-M437.
9. Curtze C, Hof AL, Otten B, Postema K. Balance recovery after an evoked fall in unilateral transtibial amputees. Gait Posture 2010;32(3):336-341.
10.Vanicek N, Strike S, McNaughton L, Polman R. Postural responses to dynamic perturbations in amputee fallers versus nonfallers: a comparative study with able-bodied subjects. Arch Phys Med Rehabil 2009;90(6):1018-1025.
11. Kruse RL, Lemaster JW, Madsen RW. Fall and balance outcomes after an intervention to promote leg strength, balance, and walking in people with diabetic peripheral neuropathy: “feet first” randomized controlled trial. Phys Ther 2010;90(11):1568-1579.
12. Gutierrez EM, Helber MD, Dealva D, et al. Mild diabetic neuropathy affects ankle motor function. Clin Biomech 2001;16(6):522-528.
13. MacGilchrist C, Paul L, Ellis BM, et al. Lower-limb risk factors for falls in people with diabetes mellitus. Diabet Med 2010;27(2):162-168.
14. Allet L, Armand S, de Bie RA, et al. Gait alterations of diabetic patients while walking on different surfaces. Gait Posture 2009;29(3):488-493.
15. Kavounoudias A, Tremblay C, Gravel D, et al., Bilateral changes in somatosensory sensibility after unilateral below-knee amputation. Arch Phys Med Rehabil 2005;86(4):633-640.
16. Fey NP, Silverman AK, Neptune RR. The influence of increasing steady-state walking speed on muscle activity in below-knee amputees. J Electromyogr Kinesiol 2010;20(1):155-561.
17. Isakov E, Keren O, Benjuya N. Transtibial amputee gait: time-distance parameters and EMG activity. Prosthet Orthot Int 2000;24(3):216-220.
18. Isakov E, Burger H, Krajnik J, et al. Knee muscle activity during ambulation of transtibial amputees. J Rehabil Med 2001;33(5):196-199.
19. Richie D. Postural control: clinical evaluation and implications for gait. Presented at annual American Podiatric Medical Association conference, Seattle, August 2010.
20. Beschorner K, Redfern M, Cham R. Role of proprioception and foot somatosenssation in detecting slipping accidents. Presented at the annual conference of the American Society of Biomechanics, Providence, RI, August 2010.
21. Ramstrand N, Ramstrand S. AAOP state-of-the-science evidence report: the effect of ankle foot orthoses on balance — a systematic review. JPO 2010;22(10 Suppl):P4-P23.
22. Richie DH Jr. Effects of foot orthoses on patients with chronic ankle instability. J Am Podiatr Med Assoc 2007;97(1):19-30.
23. Hertel J et al. Effect of rearfoot orthotics on postural control in healthy subjects. J Sport Rehabil 2001;10(1):36-47.
24. Rome K, Richie D Jr, Hatton AL. Can orthoses and insoles have an impact on postural stability? Podiatry Today 2010;23(10):43-51.
25. Hatton AL, Dixon J, Martin D, Rome K. The effect of textured surfaces on postural stability and lower limb muscle activity. J Electromyogr Kinesiol 2009;19(5):957-964.
26. Lemaire ED, Goudreau L, Yakimovich T, Kofman J. Angular-velocity control approach for stance control orthoses. IEEE Trans Neural Syst Rehabil Eng 2009;17(5):497-503.
27. McMillan AG, Kendrick K, Michael JW, et al. Preliminary evidence for effectiveness of a stance control orthosis. JPO 2004;16(1):6-13.
28. Kaufman KR, Levine JA, Brey RH, et al. Gait and balance of transfemoral amputees using passive mechanical and microprocessor controlled prosthetic knees. Gait Posture 2007;26(4):489-493.
29. Hafner BJ, Willingham LL, Buell NC, et al. Evaluation of function, performance, and preference as transfemoral amputees transition from mechanical to microprocessor control of the prosthetic knee. Arch Phys Med Rehabil 2007;88(2):207-217.
30. Highsmith MJ, Kahle JT, Bongiorni DR, et al. Safety, energy efficiency, and cost efficacy of the C-Leg for transfemoral amputees: a review of the literature. Prosthet Orthot Int 2010;34(4):362-377.
31. Kahle JT, Highsmith MJ, Hubbard SL. Comparison of nonmicroprocessor knee mechanism versus C-leg on prosthesis evaluation questionnaire, stumbles, falls, walking tests, steady ascent, and knee preference. J Rehabil Res Dev 2008;45(1):1-14.
32. Sandler R, Robinovitch S. An analysis of the effect of lower extremity strength on impact severity during a backward fall. J Biomech Eng 2001;123(6):590-598.
33. Grabiner MD, Donovan S, Bareither ML, et al. Trunk kinematics and fall risk of older adults: translating biomechanical results to the clinic. J Electromyogr Kinesiol 2008;18(2):197-204.