Kickboxing isn’t just for elite martial artists. In fact, preliminary research suggests the kicks, punches, and knee movements associated with the sport can improve balance and mobility in patients with multiple sclerosis. And as an added bonus, it’s also fun.
By Kurt Jackson PT, PhD, GCS, and Kimberly Edginton-Bigelow, PhD
Multiple sclerosis (MS) affects an estimated 350,000 to 400,000 individuals in the US, making it the most common neurologic disease of younger adults.1 Although the precise etiology of MS is unknown, the most widely accepted theory is that it involves an abnormal immune response that damages the insulating myelin surrounding the axons in the central nervous system.1
Symptoms and disease severity can vary widely, but abnormalities in balance have long been recognized as among the most common problems associated with MS and are often reported as the first symptoms of the disease.2-5 In a recent study of middle-aged and older adults with MS, 93.7% reported problems with balance and mobility and more than 50% had experienced an injurious fall.6 Problems with balance and postural control have been found in even minimally impaired individuals with MS.7-9 Unfortunately, these balance problems can cause self-imposed limitations in activity that can lead to a vicious cycle of deconditioning and further losses of mobility and independence.
Researchers have investigated a variety of methods for improving balance in individuals with MS. Specific interventions have included computerized force plate training,impairment-focused (strength and flexibility) activities,task-based functional exercises,sensory training (with altered vision and support surface), motor-focused training (weight shifting, reaching), and multidimensional home exercise training.10-14 Results from these studies have been generally positive, and have demonstrated improvements in a variety of clinical measures, including the Berg Balance Scale (BBS), Timed Up and Go (TUG) test, and Dynamic Gait Index (DGI).
There is no universally accepted method for improving balance in persons with MS, and, when considering various options, it is important to also consider the chronic and progressive nature of the disease. The chronicity of MS makes it essential that any balance training intervention can be continued safely on a long-term basis in a home or community setting. One way to accomplish this is to investigate the effectiveness of already-established community-based exercise programs that may have the potential to improve balance in persons with MS.
Researchers have evaluated the effects of several novel exercise programs that are commonly offered in a community setting. In a randomized controlled trial, Stephens et al15 measured changes in balance and balance confidence in patients with MS who had completed eight classes of Feldenkrais Awareness Through Movement Training (ATM). ATM is a learning-based approach in which participants are verbally led through movement exploration activities. The movements are usually small and slow with a strong focus on the kinesthetic experience. Following such training, study participants showed significant improvements on several measures of postural control, which were assessed using a force plate, and increased balance confidence as measured by the Activities-specific Balance Confidence Scale (ABC).
Tai Chi is another movement-focused activity researchers have studied for its possible effects on balance.16 Tai Chi is often practiced in groups, with an emphasis on slow movements and transitions between various postures known as forms. Like ATM, an important component of the activity is the participant’s conscious awareness of the movement he or she is performing. In a pilot study involving eight individuals with MS, Mills et al17 evaluated the effects of Tai Chi on balance and depression. Following two months of individual instruction and daily home practice, there were significant improvements in single-leg balance ability and in the depression-dejection component of the Profile of Mood States (POMS) scale.
While the results of these studies are encouraging, the slower controlled movements typically used in these programs may not sufficiently challenge faster reactive types of postural control that are often required to maintain balance during an unexpected perturbation.
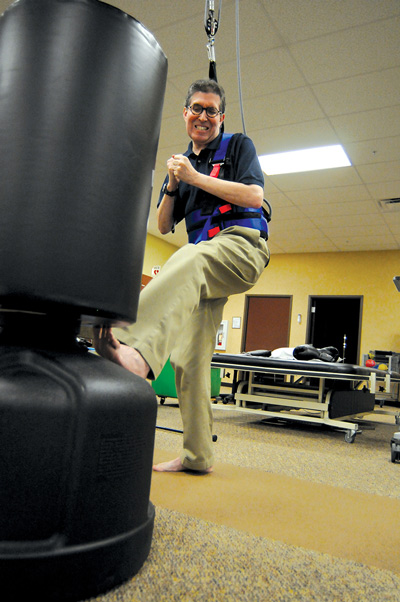
Kickboxing is another novel activity that has become increasingly popular as a form of exercise and is often provided in a group format in fitness and recreation centers. Kickboxing typically involves the execution of various punches, kicks, and kneeing movements individually or in combination. During practice, participants often aim their punches and kicks at padded targets held by another participant or instructor. Heavy bags that hang from the ceiling are also commonly used to develop more powerful kicks and punches.
Although evidence of the therapeutic value of kickboxing is limited,18 the types of movements and activities that are common to kickboxing have been supported by a relatively large body of balance training research in older adults. In a systematic review, Whipple19 described the common elements of successful balance training programs used for older adults. These essential elements, which he referred to as the five Vs, include velocity, fast interactive movements of the head and body; verticality, vertical movements of the body against gravity; vigor, moderate to high intensity exercise; vision, challenges to the visual system; and vestibular, challenges to the vestibular system.
Uniquely, kickboxing appears to incorporate all of these critical elements into a single activity. Kickboxing involves fast movement of the limbs and trunk (velocity); punching and kicking while in a standing position (verticality); powerful and repetitious movements of the limbs (vigor); directing punches and kicks toward moving visual targets (vision), and rotational movements of the head and upper body (vestibular).
Further evidence also suggests that lower extremity power, which is a function of muscle force production in a given amount of time, is related to postural control in individuals with MS.20 The movements associated with kickboxing often require rapid force development, which could lead to improved muscle power.
Given the multiple potential benefits of kickboxing, we recently conducted a pilot study to investigate the effects of a group kickboxing program on balance, mobility, and quality of life in people with MS.21
The kickboxing program
The kickboxing program was performed three times weekly for five weeks at a community-based outpatient rehabilitation center; each class lasted approximately one hour. Instructors with extensive experience in Muay Thai kickboxing led the program. Researchers divided the 15 participants into three groups of five for training. During training all participants wore a safety harness that was suspended from an overhead rail. The harness was used only as a safety device in case of loss of balance—not to provide continuous body-weight support. To further minimize risk, we selected participants who met the following criteria: a confirmed diagnosis of relapsing-remitting or secondary progressive MS, the ability to walk at least 10 m without physical assistance, the absence of any condition that would make participation in a moderate-intensity exercise program unsafe, and no recent exacerbation of their MS or changes to their medications. Participants with resting systolic blood pressure greater than 180 mm Hg or diastolic pressure greater than 100 mm Hg were also excluded.
At the beginning and end of each session, participants performed five to 10 minutes of warm-up and cool-down activities consisting of both seated and standing large amplitude rhythmic movement of the trunk and limbs, diaphragmatic breathing, and stretching. During the first two weeks of the program, participants focused on common punches, including the jab, cross, and hook. Initially participants did not wear boxing gloves and threw punches at imaginary targets. As they progressed, gloves were added, and focus mitts and heavy bags were used as physical targets. During weeks three through five, common kicks and kneeing movements were introduced, including the front kick, side kick, and knee thrust. Similar to the punching progression, participants initially kicked imaginary targets, then progressed to physical targets. Participants also held focus mitts and kick pads for each other to facilitate practice of reactive postural responses.
During the course of training instructors adapted the intensity of the kicks, punches, or knees to each participant’s ability level by adjusting the speed, power, or amplitude of movement through verbal cues and changing the location of the targets. Participants progressed by increasing the intensity, time, and repetitions of each activity while decreasing the amount of rest between skills. They were also challenged by increasing the complexity of the combinations of punches, kicks, and knees. Typically, participants spent two to three minutes on each activity followed by similar amounts of rest.
Outcome measures
To assess the effectiveness of the kickboxing program, we tested the participants on three separate occasions. We performed a baseline test five weeks prior to starting the program. This five-week time frame served as a control period. We conducted a preintervention test immediately before participants started the kickboxing program and did postintervention tests within one week of their completing the program.
We selected outcome measures to represent different aspects of balance and mobility and multiple domains of the International Classification of Functioning, Disability and Health (ICF).22 They included gait speed, TUG, BBS, DGI, Mini-BESTest, ABC, and the Multiple Sclerosis Quality of Life-54 (MSQOL-54).
Our primary outcome of interest was the Mini-BESTest because it is the only clinical balance scale that assesses reactive postural control and rapid stepping responses, which are important for fall prevention and were also key elements of the kickboxing program. The Mini-BESTest consists of 14 tasks designed to assess four subsystems of dynamic balance: anticipatory control, reactive control, sensory orientation, and dynamic gait.23 Each task is rated on a three-point scale. The Mini-BESTest shares a number of activities with the BBS and DGI but includes several distinctive tasks, such as compensatory stepping and dual tasking during gait, that may be important elements of balance not addressed by the other clinical scales.
Results
Of the 15 participants who began the study, 11 completed the kickboxing program and all phases of testing. One participant dropped out due to muscle soreness during training, two dropped out due to an exacerbation of their MS symptoms unrelated to study participation, and one participant did not complete the training due to an upper respiratory infection. Compliance ranged from 73% to 100% of total sessions attended. Our baseline testing indicated that our participants demonstrated moderate impairments in gait (mean gait speed = 1 m/s) and balance (mean DGI = 17.2, Mini-BESTest = 17.4) that were consistent with their disability level and indicative of a higher risk for falls.
Following training, there were significant (p < .05) improvements from baseline in almost all of outcome measures. The Mini-BESTest improved by 35%, gait speed by 10%, TUG by 11%, DGI by 13%, and ABC by 19%. The BBS was the only balance measure that did not show improvement; this, however, seemed to be due to a “ceiling effect” experienced by a number of our higher-functioning participants. Quality of life as measured by the MSQOL-54 showed a trend for improvement but was not statistically significant.
While the results of our study are encouraging, it is difficult to assess the clinical importance of our findings since we did not perform any long-term follow-up testing and did not track any changes in the incidence of falls our participants experienced.
Safety and feasibility
Another objective of our study was to evaluate the safety and feasibility of providing a group kickboxing program to individuals with MS in a community setting. Overall, we found the program practical and safe for our participants. There were no unanticipated adverse events. Several participants complained of moderate levels of muscle soreness following the first several sessions of the program, and left the study due to ongoing soreness. There were no reports of pseudo-exacerbations such as blurred vision or transient motor or sensory disturbances.
During the program we maintained an instructor-to-participant ratio of 2:5, but we feel this ratio could be higher (more participants per instructor) with careful selection of the appropriate participants and the use of proper safety equipment and exercise adaptations. During training our participants used an overhead harness to prevent falls. Although the safety harness allowed them to challenge themselves maximally without fear of falling, we did not feel it was essential to perform the program safely. If a harness system had not been available participants could have utilized other forms of support, such as chairs or walls, if needed.
Joint protection is another important safety consideration when performing the ballistic movements associated with kickboxing. One participant used a wrist brace and another used a hinged knee brace as precautionary protective measures. Participants were also given verbal and manual cues to avoid extremes of range of motion, such as knee and elbow hyperextension during punching and kicking. Additionally, sessions were partitioned into short bouts of activity (two to three minutes) followed by similarly timed rest breaks. We also found it necessary to use large oscillating fans to reduce heat intolerance, which is often experienced by patients with MS.
Conclusion
With proper screening and precautions we found kickboxing is a safe and feasible activity for persons with MS with mild to moderate disability. Following training, our participants demonstrated improvements on a variety of measures of balance and mobility. While the clinical significance of our findings still needs to be determined, group kickboxing appears to influence multiple domains of balance and function and may warrant further investigation.
Management of chronic neurological diseases such as multiple sclerosis, Parkinson disease, and stroke will continue to place a significant strain on our healthcare system. Developing novel ways to promote long-term health and wellness in these individuals that are both effective and affordable will be a challenge. By exploring the effectiveness of established community-based activity programs such as kickboxing, we just might be able to help meet this challenge.
Kurt Jackson PT, PhD, GCS, is an associate professor of physical therapy and neurology coordinator for the Doctor of Physical Therapy Program at the University of Dayton in Dayton, OH. Kimberly Edginton-Bigelow, PhD, is an assistant professor in the Department of Mechanical and Aerospace Engineering and director of the Engineering Safety and Wellness Laboratory at the University of Dayton.
1. Rumrill PD Jr. Multiple sclerosis: Medical and psychosocial aspects, etiology, incidence, and prevalence. J Vocational Rehabil 2009;31(2):75-82.
2. Grénman R. Involvement of the audio vestibular system in multiple sclerosis. An otoneurologic study. Acta Otolaryngol Suppl 1985;420:1-95.
3. Herrera WG. Vestibular and other balance disorders in multiple sclerosis. Differential diagnosis of disequilibrium and topognostic localization. Neurol Clin 1990;8(2):407-420.
4. Shepard NT, Telian SA, Smith-Wheelock M. Balance disorders in multiple sclerosis: assessment and rehabilitation. Semin Hear 1990;11(3):292-304.
5. Nelson SR, Di Fabio RP, Anderson JH. Vestibular and sensory interaction deficits assessed by dynamic platform posturography in persons with multiple sclerosis. Ann Otol Rhinol Laryngol 1995;104(1):62-68.
6. Peterson EW, Cho CC, von Koch L, Finlayson ML. Injurious falls among middle aged and older adults with multiple sclerosis. Arch Phys Med Rehabil 2008;89(6):1031-1037.
7. Benedetti MG, Piperno R, Simoncini L, et al. Gait abnormalities in minimally impaired multiple sclerosis patients. Mult Scler 1999;5(5):363-368.
8. Karst GM, Venema DM, Roehrs TG, Tyler AE. Center of pressure measures during standing in minimally impaired persons with multiple sclerosis. J Neurol Phys Ther 2005;29(4):170-180.
9. Martin CL, Phillips BA, Kilpatrick TJ, et al. Gait and balance impairment in early multiple sclerosis in the absence of clinical disability. Mult Scler 2006;12(5):620-628.
10. Kasser SL, Rose D, Clark S. Balance training for adults with multiple sclerosis: multiple case studies. Neurol Rep 1999;23(1):5-12.
11. Smedal T, Lygren H, Myhr KM, et al. Balance and gait improved in patients with MS after physiotherapy based on the Bobath concept. Physiother Res Int 2006;11(2):104-116.
12. Lord SE, Wade DT, Halligan PW. A comparison of two physiotherapy treatment approaches to improve walking in multiple sclerosis: a pilot randomized controlled study. Clin Rehabil 1998;12(6):477-486.
13. Cattaneo D, Jonsdottir, Zocchi M, Regola A. Effects of balance exercises on people with multiple sclerosis: a pilot study. Clin Rehabil 2007;21(9):771-781.
14. Jackson KJ, Mulcare JA, Donahoe-Fillmore B, et al. Home balance training intervention for people with multiple sclerosis. Int J MS Care 2007;9(3):111–117.
15. Stephens J, DuShuttle D, Hatcher C, et al. Use of awareness through movement improves balance and balance confidence in people with multiple sclerosis: a randomized controlled study. Neurol Rep 2001;25(2):39-49.
16. Maciaszek J, Osiński W. The effects of Tai Chi on body balance in elderly people—a review of studies from the early 21st century. Am J Chin Med 2010;38(2):219-229.
17. Mills N, Allen J, Carey-Morgan S. Does Tai Chi/Qi Gong help patients with multiple sclerosis? J Bodyw Mov Ther 2000;4(1):39-48.
18. Jackson K, Edginton-Bigelow K, Bowsheir C, et al. Feasibility and effects of a group kickboxing program for individuals with multiple sclerosis: a pilot report. J Bodyw Mov Ther 2012;16(1):7-13.
19. Whipple RI. Improving balance in older adults: identifying the significant training stimuli. In: Masdeu JC, Sudarsky L, Wolfson L, eds. Gait Disorders in Aging: Falls and Therapeutic Strategies. Philadelphia, PA: Lipincott-Raven; 1997: 355-379.
20. Chung LH, Remelius JG, Van Emmerik RE, Kent-Braun JA. Leg power asymmetry and postural control in women with multiple sclerosis. Med Sci Sports Exerc 2008;40(10): 1717-1724.
21. Jackson K, Edginton-Bigelow K, Cooper C, Merriman H. A group kickboxing program for balance, mobility and quality of life individuals with multiple sclerosis: a pilot study. J Neurol Phys Ther 2012;36(3):131-137.
22. International Classification of Functioning, Disability and Health (ICF). World Health Organization website. www.who.int/classifications/icf/en. Accessed February 21, 2013.
23. Franchignoni F, Horak F, Godi M, et al. Using psychometric techniques to improve the Balance Evaluation Systems Test: the mini-BESTest. J Rehabil Med 2010;42(4):323-331.













Do you know of any such program in Long Island, NY area?
After an MRI i was diagnosed of MULTIPLE SCLEROSIS. After years on medications, symptoms worsened with tremors on my right hand, numbness and tingling, muscle weakness and loss of speech. Fortunately last year, i learnt about RICH HERBS FOUNDATION and their Multiple Sclerosis alternative treatment (ww w. richherbsfoundation. com), the Multiple Sclerosis treatment made a great difference, most of my symptoms including tremors, weakness and others gradually disappeared. I improved greatly over the 6 months treatment, its been a years since the treatment, i have no symptoms. I have a very good quality of life and a supportive family!
My partner is 67 and has had Parkinson’s for around 3-4 years. It is a debilitating disease that only gets worse and needs some serious funding to find out 1 because the cure is out there. What causes it and 2. some better treatment for it which www .madibaherbalcenter. com have the guaranteed cure for PD. He takes over 13 weeks treatment from madiba herbal center formula that finally cure him, reverse all the symptoms including tremors ,as there is no-one available to help unless you have $4,000.00 per week to pay for a Nurse, but with this herbal system you can get rid of your Parkinson effectively ,he had tremors for several years and was gradually becoming worse before we found PD supplement from www .madibaherbalcenter. com on Facebook that was able to get rid of my husband PD disease and alleviate all symptoms within the short period of his usage.,they have the best medication for PD.
I am 68 I was diagnosed in 2023 neurologist told me I wouldn’t benefit from any meds right now due to age.. My primary care provider introduced me to MS-4 Protocol from uine healthcentre . ne t and i immediately started on their Multiple Sclerosis treatment, this MS-4 treatment has made a tremendous difference for me. My symptoms including muscle weakness, fatigue, mood swings, numbness, double vision and urinary retention all disappeared after the 4 months treatment!