
Photos by Vincent Giordano/Trinacria Photography (www.trinacriaphotography.com), courtesy of Marc Ginsburg, DPM.
More and more surgeons are embracing the idea that physical therapy after bunion surgery can improve range of motion and other functional outcomes. But some practitioners still aren’t sure it’s right for everyone.
By Linda Weber
Most surgeons will tell you outcomes of hallux valgus surgery are very good, often quoting a 90% to 100% percent success rate. A survey-based study published in the December 2001 issue of Foot and Ankle International is typically cited as evidence.
But consensus is harder to come by in determining to what degree post-operative physical therapy contributes to functional outcomes. Some doctors send patients home with a self-administered exercise and self-massage routine and nothing more. Others prescribe an extensive, twice-weekly supervised physical therapy protocol that lasts from four to eight weeks on top of home-based exercises. To complicate matters, patients start PT at various times after surgery, depending on the rate of healing and the type of procedure.
Not all practitioners are ready to accept the idea that physical therapy, and not just surgical technique, can have a substantial impact on the success of hallux valgus procedures.
“Some physicians may think if they send a patient for physical therapy after surgery, it reflects poorly on their surgical procedure,” said Juan J. Rivera, DPM, a private practice podiatrist with the Ankle + Foot Center of Tampa Bay, who views physical therapy as complementary. “In actuality, you are helping your patient optimize their ultimate results and overall post-surgical experience.”
In the last year, two studies, one published and one presented at the American College of Foot and Ankle Surgeons’ annual meeting, have revived the debate. They suggest that post-operative physical therapy can significantly improve range of motion and weightbearing outcomes.
Enter new evidence
Photos by Vincent Giordano/Trinacria Photography (www.trinacriaphotography.com), courtesy of Marc Ginsburg, DPM.
In the September 2009 issue of Physical Therapy, investigators from the Foot and Ankle Center in Vienna, Austria, analyzed 30 patients who underwent surgical correction of mild to moderate hallux valgus deformity, including 20 Austin osteotomies and 10 Scarf osteotomies. Prior to initiating the study, the researchers had observed that despite favorable clinical results, including pain relief, the ability to wear a wider variety of shoes, and the ability to participate in recreational activities, gait patterns did not spontaneously alter after surgery.
“We noticed that patients who underwent hallux valgus surgery didn’t use their great toe for push off, even though the deformity was corrected sufficiently,” said Reinhard Schuh, MD, a first-year resident in the department of orthopaedic surgery at Innsbruck Medical University and lead author of the study.
“To achieve bony union of the osteotomy, we had to avoid loading for four weeks,” Schuh said. “But we instructed patients to perform passive ROM exercises starting two days after surgery.”
At four weeks, patients began a comprehensive, 45-minute rehabilitation program once a week for four to six weeks. The standard protocol included elevation of the leg, lymphatic drainage, activation of the muscle pump, and cryotherapy in the first session to reduce swelling. Other modalities, such as scar tissue massage, mobilization, manual therapy, soft tissue techniques, proprioceptive training for the lower leg, strengthening exercises, and gait training, were added progressively over the next four weeks.
Although the researchers did not use a control group, they found that at six months after surgery patients experienced significant improvements in first metatarsophalangeal joint range of motion and function. Weight bearing at the great toe and first metatarsal head, specifically related to maximum force levels and force-time integral, also improved significantly. Participants’ mean functional score on the American Orthopaedic Foot & Ankle Society forefoot scale improved from 60.7 out of 100 before surgery to 94.5 out of 100 at six months. By comparison, previous plantar pressure studies have documented a lack of weight bearing in the medial forefoot and first ray after hallux valgus surgery not followed by physical therapy.
Believe it or not
Photos by Vincent Giordano/Trinacria Photography (www.trinacriaphotography.com), courtesy of Marc Ginsburg, DPM.
In the second study, which has been submitted for publication, researchers studied 55 patients who had undergone Scarf procedures at the Weil Foot and Ankle Institute in Des Plaines, IL. The large, 16-office practice in the Chicago area handles 500 bunion surgeries a year. According to Lowell Weil, Jr., DPM, MBA, senior investigator of the study, surgeons in his practice fall into two camps.
“The advent of screws and proper screw fixation eliminated the need for complete immobilization. Patients are able to return to activities and start physical therapy earlier, which has tremendous benefits. We developed physical therapy protocols for patients undergoing these types of procedures,” he said. “Despite that, some doctors in our practice weren’t prescribing physical therapy; they didn’t believe it made a difference.”
So Weil and a few colleagues set out to investigate. Their nonbelieving colleagues’ patients, who did not receive PT, served as a control group.
They studied 44 patients (65 feet) who underwent Scarf osteotomy procedures between 2006 and 2008, followed by a program of once- or twice-weekly physical therapy sessions. The 30 to 45 minute sessions continued for one to six weeks. Another group of 11 patients (14 feet) received no post-operative therapy.
Follow up occurred between November 2009 and January 2010. The physical therapy group significantly outperformed the control group on the Foot Function Index (FFI) and the ACFAS Universal Foot and Ankle Scoring System (see table).
Opinions about post-operative physical therapy in hallux valgus cases are as varied as surgical procedures. For PT proponents, like Michael Loshigian, DPM, a podiatric foot and ankle surgeon in private practice with the Metropolitan Foot Group in New York City, the benefits are indisputable.
“My own experience is fairly clear. Patients who have some sort of formal or informal physical therapy after hallux valgus surgery have better overall results and the progression of healing is more consistent and reliable,” Loshigian said.
Getting a head start
 Loshigian, who performs these surgeries at least weekly, says the physical therapy protocol often begins shortly after surgery.
Loshigian, who performs these surgeries at least weekly, says the physical therapy protocol often begins shortly after surgery.
“In a joint fusion case, there should not be any attempt to move the joint, obviously. But in the majority of cases, we’re reorienting the MTP joint, restoring normal range of motion and alignment and function of that joint. In those cases, I have patients start their own range of motion exercises the day after surgery,” he said.
A primary objective is to prevent the soft tissue contracture and joint stiffening that can result from cutting and repositioning of bone.
“It’s easier to maintain good range of motion from the beginning than to attempt to restore it after it has been lost,” he said. “If we give those soft tissues an opportunity to tighten up, movement becomes difficult.”
Loshigian usually starts patients on formal twice-weekly physical therapy two to three weeks after surgery, once he removes the stitches. For most patients, the complete course of therapy lasts six to eight weeks.
At three or four weeks after surgery, patients can start weight bearing without the protection of a post-op shoe; at that point, Loshigian recommends strengthening the muscles and tendons that control the great toe along with continuing ROM exercises and techniques to reduce swelling. The final stage involves strengthening the lower legs and improving patterns of gait, agility, and balance.
Contributing factors
Rivera says many factors influence his decisions about the timing and course of therapy.
“Surgical procedures —MTP joint fusion, arthroplasty, chevron, opening base wedge, closing base wedge, first metatarsal-cuneiform joint fusion—all have various timeframes to stay offloaded, which can lead to disuse atrophy,” he said. “Many patients have such low pain tolerance, they need gait retraining to overcome post-operative pain and swelling and regain joint flexibility. Older patients need more help with loss of balance and proprioception.”
Another issue is the amount of time a patient with an operable deformity has postponed surgery; long delays can lead to compensatory gait patterns that are difficult to unlearn without additional physical therapy.
“A common example for me is the patient who undergoes hallux limitus correction surgery,” he said. “The biomechanical compensation for a painful arthritic great toe joint is to ambulate with the foot in an inverted position. Post surgery, the patient continues to ambulate in that position out of habit, delaying the healing of the foot.”
Not for everyone
Donald R. Bohay, MD, a professor of orthopedic surgery at Michigan State University who is also in private practice at Orthopaedic Associates of Michigan in Grand Rapids, views hallux valgus surgery and its aftermath from a slightly different perspective.
“I’m a believer in physical therapy that can help your patient get better faster,” Bohay said. “But I don’t think we know for sure that the patient who gets physical therapy versus the patient who doesn’t is necessarily better after a year.”
Bohay, who favors tarsometatarsal arthrodesis with a modified McBride procedure, says that his patients wear a post-op splint for two weeks. They then wear a short leg cast with heel weightbearing for six weeks, followed by a weightbearing boot for two to four weeks.
Most of the surgeons interviewed for this article would prescribe supervised physical therapy for a procedure requiring so much healing time and immobilization. However, Bohay instructs most of his patients to do home-based range-of-motion exercises and soft self-massage with vitamin E oil to desensitize the foot. When he considers it necessary, he does prescribe formal physical therapy.
“You get a sense that some patients aren’t going to do the program. Those patients do well by going to PT,” he said. “Then there are patients who have a lot more done, who are very swollen, very stiff. For them, physical therapy helps reestablish control, range of motion, and desensitization.”
The therapist’s perspective

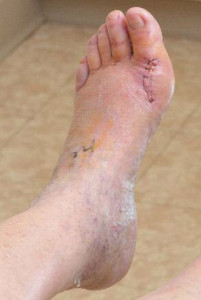
Figure 1. After completing the physical therapy protocol, this bunionectomy patient has full extension of the toes. (Provided by Lowell Weil Jr., DPM)
Despite the general consensus among surgeons that PT is a useful tool after bunion correction, at least in certain cases, physical therapists express frustration that surgeons don’t take full advantage of their expertise.
“It’s a misconception that physical therapy is cookie cutter,” said Clarke Brown, PT, DPT, OCS, ATC, who is in private practice in Rochester, NY, and president of the American Physical Therapy Association’s foot and ankle special interest group. “We study these procedures. We develop separate protocols for them, and adapt them for each patient.”
Physical therapy following bunion surgery, Brown said, should extend well above the ankle.

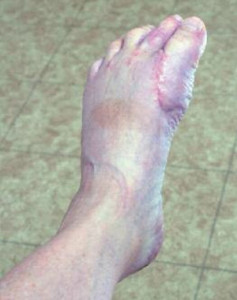
Figure 2. Patient has regained full flexibility after bunionectomy and physical therapy (Provided by Lowell Weil Jr., DPM).
“The most challenging thing about feet is that they radically change what happens all the way up the kinetic chain. The good practitioner looks at the whole system, all the way up to the knee, the hip, and the back. We look at the range of motion in all the joints and the strength of the entire leg,” he said. “Most chronic bunion patients can’t effectively lift the bunion leg in side-lying. The hip muscles atrophy.”
Brown notes that the foot and ankle subspecialty in physical therapy is just developing. Even though it’s not something surgeons have clamored for, those who witness the benefits of specialized therapy are sold, he said.
“We found that the faster we started to move the patient’s foot and toes, the more quickly the swelling went down,” he said. “One podiatrist used to take his sutures out after two weeks. But when we moved aggressively, the incisions would sometimes open up. Now he takes the stitches out at 21 days, saying ‘I’ll leave these in longer so you guys can do more.’ The more we communicate with each other, the better.”
A proactive approach
Stephen Paulseth, PT, DPT, SCS, ATC, who runs a private practice in West Los Angeles, often sees patients who have complications or problems that he believes could have been avoided by introducing physical therapy earlier.
“If doctors would send their patients for prehab, they would be doing so much better,” said Paulseth, who preceded Brown as president of the foot and ankle SIG. “I sometimes see patients six weeks in who haven’t really done much. They’ve been told to ice, strengthen, and do some gentle motion, but they just can’t tolerate it.”
He believes proper therapy and patient training can reduce the progression of bunion surgeries.
“Calf length is number one. Inadequate dorsiflexion of the ankle leads to all kinds of distal forefoot issues, including hallux valgus. Patients should begin calf stretching as soon as possible, and they have to continue calf stretching after they’ve healed,” Paulseth said.
Surgeons contend that most patients who undergo hallux valgus surgeries are happy with the results.
“From my experience, the vast majority of patients who have gone through this procedure are very satisfied with the results and in retrospect would choose to undergo the same procedure again,” Loshigian said. “As for their initial post-op experience, the feedback I get from most patients is that it is less stressful and painful than they anticipated.”
In Brown’s estimation, that already good patient experience could be even better if the relationship between patient, doctor, and physical therapist were more collaborative.
“When patients do better quicker, the word of mouth is more positive for the doctor,” he said. “Everybody wins.”
Linda Weber is a freelance writer based in Clemmons, NC.










As a practicing Pedorthist is good to see groups expressing a willingness to work with each other . This practise can only strenghten the medical field, inprove patient’s confidence and i think increase patient compliance .
Also on the subject of bunionectomy, correct footwear will always play an important role in the maintenance of this surgery.
We see alot of patients who after having the surgery are not happy , simply because footwear was not discussed.
Had bunionectomy 7/25th. I’ve been doing knee/ankle self PT at home almost immediately after.
Went back to work 9/15th. Feel good enough to start my usual hiking/running but, can’t get
my foot into the footwear. Swelling only on top of foot and slight stiffness in th big toe is the
problem still in 70th day. Starting to concentrate on big toe in/and/out PT to expedite healing.
Any other quick fix ideas to fit into my shoes? Thanks.Dee in Seattle .
I had an Austin bunionectomy about 6 weeks ago. My big toe is very stiff. It is quite worrying. I have been told that I should massage and ice it myself, but I am wondering if I should go for physio now although I am not yet at the 8 week mark. It’s a little disconcerting how tight everything is there, although I will agree that the surgery has been far less painful overall than I anticipated.
Tracy,
I also had the Austin bunionectomy on Jan. 11th, 7 weeks tomorrow. My big toe is very stiff as well and when I try to force it to bend, it does not. I do have a pin and screw in my foot that goes into the bone where the bone was cut, but it does not go into my big toe. My dr did not recommend any outside PT, but he did suggest that I massage it myself and try using warm foot baths, followed with ice. As of today, I still have swelling in the toes, bottom forefoot and some on the top of the my foot. I have been out of the walking boot since the 5th week. I can walk on it, but I cannot put full pressure on the ball of my foot. Everyone keeps telling me that I am doing great with it, and that it takes 8 months to a year to be completely back to normal. 🙁 I would love to hear how you are doing now. regards, Vicky
I had a Keller bunionectomy 7 weeks ago. My surgeon has given me the all clear and I do not need to return for any follow up visits. My great toe is extremely swollen and stiff. I can move it back and forth only slightly and the balance of my other toes are also very stiff. I am now attempting to walk in a very stiff sandle with patience. My surgeon did not suggest physical therapy, but now I am wondering just how long will this take to get back to normal walking.
Any suggestions would be greatly appreciated.
I had minimum incision bunionectomy on my both feet. Right at Feb /2013 and left in April 2013. My podiatrist did not recommend the physical therapy but I wanted it since I was afraid to move my toes and they were all stiff. Even the toes that I did not do surgery. It has been now 10 weeks from my left foot surgery and three weeks for my physical therapy. I can now move my toes but a little pain when I bend them too much. The ultrasound and laser has been very helpful. It is very comforting after each session. I think I will continue for another three weeks until I get the full flexibility back.
I last posted Feb. 28th, 7 weeks following my bunionectomy. It has now been 5 months + 1 week. Just had my 4th follow-up visit with my dr (Podiatrist). I am able to walk with full pressure on the foot that the bunion was removed. Only a tiny bit of swelling left. Sometimes I still get some tingling/throbbing pains if I have been on my feet all day. Nothing was done to my big toe in order to realign it. So, therefore it does still shift towards the other toes. I have voiced my concerns more than once about it to my dr and he suggested I try wearing a bunion nightsplint. I have two ordered and awaiting them via the mail. I chose to also wear one on my right foot until the surgery is performed on it. Which I hope is later this year. My dr also suggested I do my own PT by massaging my foot while soaked in warm water. I have been doing this some and also moving and bending it while sitting around. This has helped loosen it up and I am able to bend my toes more, but not as I could before the surgery. I continue to do this and am told that it can take up to 1 year to get complete mobility back. I enjoy reading what others have to say and hope my post are also helpful. Best wishes to all of you!
I had a recent bunionectomy and I am just at the 2 weeks mark and I fell on my foot without my boot on and landed on it with my full body weight. Does anyone know what will happen or if I should go the ER since my doctor is out of the office? Thank you!
I had a bunionectomy and hammertoe surgery on my right foot on 6/24/13; Im 3.5 weeks post op. I iced my foot all day/night long changing the velcro ice bag 3-4 times in 24 hrs. I have a pin screw on my big toe which will not be removed. I’m able to walk slowly with the surgical boot shoe for about 30-mins per hour pain free. My stitches were removed 14 days after surgery and my dr told me to start exercising my big toe back and forth 5x a day as far as I can with no pain. My big toe is moving better each day. I’m massaging my foot with Vit E oil (per dr) and applying the oil with Qtip on stitches. My foot swells only after a warm shower so after the exercise and massage I’m icing it for 30-mins in bed and so far it’s healing better than expected. I’ve had no pain since day 4 post op and slight swelling after a warm shower. My husband rented a knee scooter (no crutches for me) which was the best gift ever to get around the house , so I did not lay in bed all day. I’m still using the knee scooter to go to church, stores and the mall 🙂 I just had to post some positive feedback .
Its my 2 weeks mark after my surgery. Bilateral bunion and toe alignment.I have 2 pins and a screw.
One foot is slightly swollen, with slight discomfort. Didn’t have any pain so far. Elevating it all day. I used a wheel chair to move around and started using the boots since 2 days.
What’s worrying me is that while sleeping, my body does a kind of stretching once or twice, which reaches up to my toes, and I can’t stop it. It makes my whole toe move, which scares me. Although I get no pain afterwards. But is that OK? or will it cause the pins to move or something? Can anyone tell me please?
This appears to be a good forum to get some honest answers, at least I hope so. I recently (Aug 20th) had surgery for a bone spur, bunion and 2 pins put in my big toe. I am concerned about swelling at the ball of my big toe as well as numbness. My Dr said that I would have swelling for 6-8 months but I wanted to hear it from actual patients. It is difficult to do physical therapy when the swelling and numbness hinders the movement of my big toe. It is also difficult to walk correctly because of the swelling. Has anyone else experienced this? Vickie seems to have been in a similar boat but I was wondering what you all thought/experienced.
Also, has anyone used a compression sock for this type of surgery and what it its purpose?
Thank you for any and all responses.
De
I had a bunionectomy November 1st. I was instructed to not bear with any weight on it until the stitches were removed on November 13th. At this point I was given a rather heavy but sturdy walking boot. My foot was so painful to bear weight on that I left the office on my trusty knee scooter (they are worth the 85.00/month to rent). Despite elevating my foot and icing it as recommended, the swelling would persist. Determined to heal, I forced my foot into the boot and walked on it anyway, but over the next 3 weeks, I was never able to put my full weight on it because the swelling made it so painful to walk.
Had my follow up appointment 12/11/13 to see if I could fit in a shoe. Nope. Foot is still too swollen. Oh, that big toe is way too stiff! I was going to have to get aggressive before the window of physical therapy benefit closes leaving me stiff toed forever. That’s what my doc told me. Alarmed, I am now doing hot foot bath soaks followed by bending my toe as far as I can and holding it there as long as I can before it’s too painful. This causes swelling on top of the swelling I already have. So, I elevate and ice which helps. I am using a shoe part time and the boot the rest. It is painful to bear my weight on my surgery foot when I walk but I have come to the conclusion that if I don’t I will not return to a normal gait or improve range of motion in my toe. Kinda sucks that this far out post op, I am having these pain/swelling issues that are hindering my healing.
Before, I was bending my toe back and forth in sets of ten several times a day. This seems to be useless for improving range of motion for me. So I am pressing all of my toes against a hard surface and holding it there. This appears to be helping some.
I think the key for me is too not baby my foot so much or worry about the swelling. I am more swollen then the average patient per my doc but not out of the range of what is normal. So, it’s taking me longer to heal. But there’s not much I can do about it.
I read stories of other people who seem to recover quickly and easily from bunionectomy surgery. I have come to the sad conclusion that I am NOT one of those people. Damn! Best of luck to all of you.
Hi Everyone!
Hope somebody can advise me please. I am 5 weeks post op, bunion, osteotomy, tendon release. I had a block put in the back of my thigh for the operation, when i was moved from the gurney to the operating table, the machine went off and my whole body from toes to my neck started shake like a fit, when they stopped it, the put me under and performed the op. I asked when i came around what had happened they said they didn’t no! Well, i keep getting terrible muscle spasms from my hip to my bad foot and the foot spasms and shakes, it seems to happen more during the evening. Sometimes if i touch where the block was put in it shoots pain down, surgeon doesn’t seem bothered. Has anybody experienced this or maybe there is an anesthetist who may be able to advise, it is terrible and i can only walk with crutches and have lots of ankle pain and swelling.
Any advise, i am desperate.
Thanks
Hi! I am 4 weeks post bi-lateral bunionectomy without toe alignment. I have been very surprised at how relatively easy it has been. The first week was painful, but I actually walked (shuffled in my post-op shoes) into the doctor’s office for my 6 day post-op appointment and they were shocked. I have been going to physical therapy for range of motion (and also to hopefully correct my left big toe migrating towards my second toe). I am in running shoes now, and walking almost normally (slower, but not bad). My scars look really good, and overall I am very pleased. I’m 46, very active in tennis, aerobics, kick-boxing, etc. so maybe that could partly explain my good outcome (plus I didn’t wait too long to get the surgery). I am definitely thanking God for blessing me with a good recovery! Just wanted to put a good story out there to combat the horror stories that I read before my surgery!
9 months post bunionectomy of the right great toe. Mine required the surgeon to break two bones to straighten it out since it had been this way for 30 years and just getting worse each year. Pain was excruitiating for 4 days, then improved over the next two week. I have full extension but not full extension. The swelling did not completely go away until 6 months. It was about that time that I noticed I was walking normally in terms of pace and putting full weight on the ball of the foot. I started trying to do range of motion exercises at three weeks after the pin was removed. I had to have a pin in the second break because my
bones were not very dense. I think recovery time depends on the surgery (what the surgeon has to do to correct and straighten), amount of swelling, and bone density. I am having the left one done in a few months (almost a year since the last surgery). That bunion started to develop about 7 years ago and rapidly progressed. The surgeon said he did not think the recovery would be as bad with this one. We shall see. I am planning on the 6 months and if it is shorter than that I will be pleasantly surprised.
Meant to say full extension but not full flexibility. Surgeon said extension is more important (upward motion of toe vs. bending it downward).
As someone who has had multiple foot surgeries on boot feet, time and PT are the biggest healers. In the beginning, PT is uncomfortable and my fabulous PT requires me to do stretching at home every day. You will be all the better for it. I have had a fused toe and clips in another toe due to my abnormalities. I began running again after the last surgery 8 months out working up to 1.5 miles daily. In my opinion, full recovery can take up to 1 year. I had to buy special running shoes and inserts in order to run. I added biking and swimming on days that I was experiencing pain. I also started modified cross fit again working up to 6 times a week. I have always been very active and decided if amputees can continue being very active SO CAN I!
I was pain free with no swelling at the end of 1 year!
Dear Sarah( Jan 06,2014),
I’m sorry that happened to you. I hope you finally got the correct diagnosis and recovered. had a similar thing happen after surgery starting with shooting electrical pains down the blocked nerve and my food was red, puffy and burnt continually like in an oven,. Doc’s didn’t take me seriously till I almost had a nervous breakdown. It even spread to my other leg and foot.Turned out I had ( have ) RSD ( CRPS ,and it was almost too late to treat . I had sympathetic nerve injections with great relief. But unfortunately it was too late for complete healing. I still have some problems , have to sleep with my feet uncovered. I take Neurotin every night before bed , and increasing the dose when more symptomatic. I hope this can can help someone , since no one helped me when I needed it and still suffer .
6 months out, recurrent hallux values, no flexor of bigtoe, continued pain and swelling and stiffness. PT has been a losing game for me…they do nothing and never gave me home exercises even after request. OS is “disappointed” but being an @$$ about doing more correction and stabilization. It is so frustrating. can only walk a few minutes on foot. I fear I will never be able to return to work or hiking
Here is my physical therapy post bunionectomy video that several people have told me has helped them! All these techniques are from my physical therapist and just wanted to share because its so informative! Enjoy and positive recoveries!
https://youtu.be/MSIPn2VOszQ
I had bunionectomy surgery on August 19,2020 it is now 10/17/2020 I can walk a while before it starts swelling up. My Dr didn’t prescribe physical therapy I’ve been working on my foot on my own I wish the Dr. Would have at least recommended some exercises if he wasn’t gonna send me to therapy. My big toe is still a little stiff but overall my foot feels good and it wasn’t has painful has I thought, especially after one of the nurses tried telling me how very painfull it was right before she rolled me into surgery it was kinda mind boggling for her to tell me that right before surgery. I still can’t bend my toe all the way but I try and it doesn’t hurt at all and I can fit into my footwear. I think my Dr. Did a great job on my foot because I had a sever bunion.
Had big toe arthrodesis surgery Dec 7 2020. Post op and stitches out Dec. 22. 2020. Physiotherapy accessment Jan 4 2021. Given a couple of stretches to do at home and appointments setup for 2 x a week starting January 19 2021. Given additional exercises to do at home twice a day for toes, ankle, thigh, calf, knees, hip and back. Next visit added balance, weight bearing . March 9 added waking outside for 10 min or on treadmill for 5 min . Friday March 26th reassessed and let go. Mobility of ankle back to normal (90 degrees). Toes can bend even the top of my big toe. Walking gait good. Walking on my foot normally now instead of the side of my foot. Have to continue on my own with exercises to prevent stiffness and help reduce swelling. Walking outside now for 20 min. I highly recommend physiotherapy. No pain. Still have swelling but that can last for 6 – 12 months.
I had a scarf osteotomy and 2nd toe realignment with 3 screws inserted, 9 weeks ago. I am 58 and I am struggling to walk without pain. My whole leg shakes when I put my toes down and heel up, even when not weight bearing. Swelling goes down but trying to use the foot on clutch to drive has also proved too painful and starts the whole swelling thing off again.. Hoping (praying) for further improvement. Still can’t work and beginning to seriously worry. My foot’s a nice shape though!
I had bunion surgery 7 was ago. I am now on weight bearing with boot. I have been using a knee scooter.can l still used this knee scooter to begin my weight bearing on the right foot