Diabetic foot ulcers and the resultant skin defects caused by delayed wound healing are a common and costly challenge for healthcare providers. Recent advances in tissue engineering have given rise to new promising treatment options to help with wound repair and tissue augmentation. Newly available adipose tissue grafts can help clinicians solve troublesome issues such as skin breakdown and impaired wound healing in patients with and without diabetes.1 Autologous fat grafting and dermal fillers have been successfully used for many years in plastics and reconstructive medicine, but more recently the use of adipose tissue grafts has been gaining favor in podiatric surgery and wound care.1 New studies are emerging that show promising results using these fat grafts as an adjunctive therapy in cases of wound healing, pre-ulcerative callus, post-traumatic injuries, internal offloading of pressure points, and as a way of augmenting tissue integrity in diabetic foot ulcers (DFUs) in remission.
The mechanism of action of autologous fat grafts has been studied extensively. Within adipose tissue there is a bounty of adipose-derived stem cells (ADSCs).1 Research has shown that these ADSCs can contribute to better outcomes and improved wound healing.1 ADSCs are pluripotent stem cells that have the ability to differentiate into various cell lines and accelerate multiple tissue regeneration processes.1 It has also been hypothesized that ADSCs can aid in the reduction of inflammation, growth factor secretion, and increase angiogenesis, thus promoting healing and re-epithelialization in wounded tissues.1 Animal studies have shown that subcutaneous implantation of adipose tissue grafts serve as an inductive scaffold to sustain adipogenesis to increase soft-tissue volume and decrease areas of pressure.1
Historically, there have been challenges to using autologous fat grafts. Inconsistent graft retention, donor site morbidity, insufficient harvest and excessive harvesting times were some of the biggest hurdles to using autologous fat grafts.2 These drawbacks have led to the development of commercially available adipose-derived matrices that are formulated from human cadaveric tissue donors and processed for allograft transplantation.2 As an off-the-shelf alternative to autologous fat grafts, these allograft adipose matrices (AAMs) are engineered to act similarly without the need for harvest, thus decreasing the associated morbidity and complications. Preclinical research has proven that the AAM retains the critical structural proteins as well as the growth factors needed to support adipose tissue formation and wound healing.2 These AAMs are stored at ambient temperature so they are easily incorporated into clinics and operating rooms.
Case Example
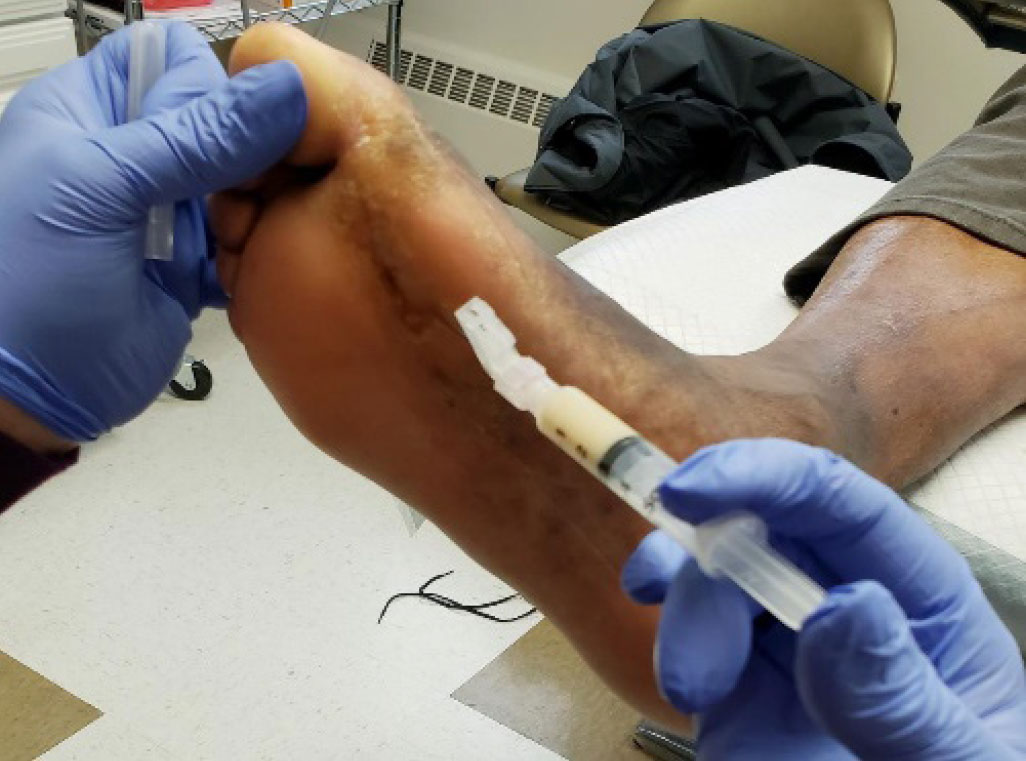
This is a 56-year-old male with a history of non-healing neuropathic DFU under the 1st metatarsal head of the right foot. The ulcer has been present for more than 4 months and many wound care therapies have failed to progress the wound to closure. Figure 1 shows the ulcer at baseline. The wound measures 2.7cm x 0.6cm and probes to subcutaneous tissue. No clinical signs of acute bacterial infection are noted and the patient’s Ankle-Brachial Index (ABI) was 1.04. Patient has been compliant with treatment and offloading. His current A1C is 7%. It was determined that injectable AAM was a viable treatment option to help augment the tissues in this area and accelerate wound closure. The AAM was injected subcutaneously around the peri-wound tissues in my outpatient clinic with the use of local anesthesia (Figure 2). The patient was then placed into a padded secondary bandage and an Ortho-Glass (Essity Medical Solutions [formerly Bsn Medical Inc.], Stockholm, Sweden) posterior splint was applied for offloading. Patient was followed in clinic weekly post-injection. Complete epithelialization of the area of the DFU was noted at week 3 (Figure 3). Patient had no reported adverse events.
Broad Utility
The utility of AAMs is far reaching. As this case study illustrates, AAMs can be very effective when injected around the ulcerative site and can lead to rapid wound healing. AAM products can be used to augment protective padding around areas of increased pressure typically prone to skin breakdown such as boney prominences and even plantar surfaces of patients with Charcot rocker bottom foot deformities.3 AAMs can be injected in areas of callus to help decrease friction and prevent reformation. I have also used AAMs in my clinic to help augment subcutaneous tissues in areas of previous ulceration and skin adhesions to help reverse volume loss.3 AAMs also have potential utility in cases of traumatic injuries where there is the need for reconstructive surgery.
The longevity of these injectable grafts remains to be seen. Current studies show autologous fat grafts and allograft adipose matrices are well-tolerated and provide at least 6 months of volume retention.2 The fact that these products support autologous fat formation and tissue remodeling is promising for long-term outcome potential.2 Larger, long-term follow-up studies will be needed to determine the longevity and efficacy of fat grafts in podiatry and wound care.
This is an emerging area of interest with a great deal of potential. As with most new therapies, reimbursement is still a challenge. The majority of published literature on fat grafts pertains to the use of these products for facial reconstruction or esthetics, areas that do not support full body weight or endure continuous biomechanical tensions. The good news is that there is a lot of opportunity for research among our profession to add to the knowledge of how fat grafting can help our at-risk patient population.
- Wang Y, Zhang H, Zhou M, et al. Autologous fat grafting promotes macrophage infiltration to increase secretion of growth factors and revascularization, thereby treating diabetic rat skin defect. Diabetes Metab Syndr Obes. 2020;13:4897-4908.
- Gold MH, Kinney BM, Kaminer MS, Rohrich RJ, D’Amico RA. A multi-center, open-label, pilot study of allograft adipose matrix for the correction of atrophic temples. J Cosmet Dermatol. 2020 May;19(5):1044-1056.
- Shahin TB, Vaishnav KV, Watchman M, et al. Tissue augmentation with allograft adipose matrix for the diabetic foot in remission. Plast Reconstr Surg Glob Open. 2017;5(10):e1555. Published 2017 Oct 23. doi:10.1097/GOX.0000000000001555