By Marlin W. Schul, MD, MBA, RVT
By Marlin W. Schul, MD, MBA, RVT
Sponsored by an educational grant from Medi USA.
Superficial thrombophlebitis (STP) is a common and controversial condition largely overshadowed by its big brother, deep vein thrombosis (DVT).1 Frequent reports of concomitant STP and DVT, with or without pulmonary embolus, align the two pathophysiologies closely.2,3 Superficial thrombophlebitis is associated with an array of presentations.1 Despite the knowledge that has emerged over the past 20 years, a gap in venous education in the U.S., based on established and inaccurate dogma associated with STP, leads many unknowing providers to prescribe a recipe for thrombus extension, the growth of thrombus burden. Thrombus extension can lead to complications of DVT, pulmonary embolus, or both.
 Clinical features
Clinical features
Superficial thrombophlebitis presents as a sudden onset of leg discomfort with firm inflamed varicosities (Figure 1). A palpable cord may be present and fluctuance is noted frequently over the varicosities involved. Inflammation over the region may at times be extreme despite the lack of a true infectious etiology. The most proximal point of thrombus extends on average 15 cm beyond where the thrombus is clinically evident, rendering the physical exam a limited tool.4 The inflammatory process, which is commonly linear, forces clinicians to consider other potential pathology and a broader differential diagnosis (Table 1). Once clinicians confirm the diagnosis of STP, they must verify the true extent and nature of the thrombus burden.
Epidemiology/pathophysiology

Figure 1. Superficial thrombophlebitis presents as a sudden onset of leg discomfort with firm inflamed varicosities.
The Tecumseh Community Health Study was the first large scale effort to define the incidence of venous thromboembolic phenomena including superficial thrombophlebitis, estimating it to occur in 123,000 patients per year, based upon 1970 US Census data.5 As duplex ultrasonography has emerged, we have learned much more about patterns of STP and complications associated with this disease entity.
Data from Lutter’s series of nearly 13,000 lower extremity duplex evaluations for DVT further elucidated the features of STP.6 In this study, 1412 patients were found to have acute venous thrombosis. Of these patients, one in eight was found to have superficial venous system involvement. The location of thrombus most commonly involved the great saphenous vein (69%), followed by the small saphenous vein (30%), and was isolated to varicose veins in 13% of patients. Multisegment involvement is commonly seen, as is bilateral involvement (9%). (Figure 2.)
Histopathology may differ with regard to the extent of inflammation involving the vein wall, and STP involves a tremendous amount of inflammation compared with that found with acute DVT.7 Over time, the region of thrombus may become more organized and incorporated into the vein wall, become completely recanalized, or may remain scarred with venous septae in an otherwise refluxing vessel.8
Risk factors for STP
 Multiple studies9,10 have described the risk factors for developing superficial thrombophlebitis, many of which, not surprisingly, are well aligned with those of DVT (Table 2). Varicose veins in the lower extremity, which occur in 61% to 93% of STP cases, constitute the most common predisposing risk factor. Others include advancing age (≥60 years), female gender, obesity, multiparity, recent surgery or immobilization, hormonal influences, history of prior venous thromboembolism (VTE), and hypercoagulable states, including malignancy. Seasonal variations have also been reported, in which the peak incidence is typically seen in the warmer summer months.11
Multiple studies9,10 have described the risk factors for developing superficial thrombophlebitis, many of which, not surprisingly, are well aligned with those of DVT (Table 2). Varicose veins in the lower extremity, which occur in 61% to 93% of STP cases, constitute the most common predisposing risk factor. Others include advancing age (≥60 years), female gender, obesity, multiparity, recent surgery or immobilization, hormonal influences, history of prior venous thromboembolism (VTE), and hypercoagulable states, including malignancy. Seasonal variations have also been reported, in which the peak incidence is typically seen in the warmer summer months.11
Risk for VTE complications
Although concomitant deep and superficial vein thrombosis was once thought to be a rare finding, duplex ultrasonography reports have revealed that the conditions appear concomitantly at a rate of 8.6% to 24%.6 This confirms that the clinical picture of superficial thrombophlebitis often harbors more serious sequellae than previously suspected.
Lutter et al compared populations with isolated STP to those with combined disease at initial presentation and found that in those aged >60 years, prior history of DVT, recent immobilization, and systemic infection are statistically significant risk factors for developing concomitant DVT and STP. Quenet identified 427 consecutive hospitalized patients with isolated STP.2 During three months of follow up, 4.7% of those patients developed VTE complications of DVT, pulmonary embolus, or both. Regression analysis revealed male sex, history of VTE, severe chronic venous insufficiency, and sudden onset of STP as statistically significant risk factors for developing VTE complications.1
Diagnostic approach
Superficial thrombophlebitis most often occurs in patients with varicose veins, but may also occur in normal saphenous veins in patients with underlying thrombophilia.6 The common findings of DVT and/or pulmonary embolus in patients with superficial thrombophlebitis create a high degree of suspicion for the condition, which requires further diagnostic testing for confirmation. The prevalence of concomitant venous complications in patients with STP mandates duplex ultrasound for each patient in whom this condition is suspected.12,13 The results of the duplex study serve to not only declare the presence or absence of thrombus, but aid in identifying complications found commonly in patients with STP. Simply put, duplex ultrasonography is the most critical study to perform, as it can guide treatment decisions and may indicate a need for more advanced imaging (Figure 3).
Treatment options
Controversies surrounding management of STP are abundant. Best practice guidelines exist for patients with complications of VTE, but data is generally lacking for STP of the lower extremity. The primary goal of management is to prevent thrombus extension and risk of VTE. All other therapy is directed at patient comfort. Existing treatment options are reviewed below, along with existing evidence about preventing VTE complications in patients with STP.
Ambulation vs bed rest

Figure 2. Bilateral involvement is seen in 9% of patients with superficial throm- bophlebitis, according to a 1991 study.
Many reference texts in vascular surgery and primary care continue to tout bed rest as part of the mainstay of therapy for STP and DVT. However, the recommendation for bed rest in patients with acute thrombosis would seem to be simply a recipe for thrombus extension and potential complications related to ongoing venous stasis, given that prolonged immobilization contributes to venous stasis, which is a trigger for thrombus.14 In a randomized study by Partsch et al, compression and walking were superior to bed rest and elevation for reducing edema and discomfort and for minimizing thrombus extension in patients with proximal DVT.15 Although we may not extrapolate the benefits of ambulation in the Partsch study to encompass all thrombotic events of the lower extremity, one cannot dismiss the potential benefits for those patients who are able to walk.
Compression therapy
There should be little argument that compression offers the most scientifically proven benefit for this condition. Established benefits include symptomatic relief as well as prophylaxis against the development of DVT.16 In a recent multicenter epidemiologic study involving 844 patients with STP, 99.7% were prescribed elastic compression stockings or compression bandages until they could be seen by a vascular specialist, which illustrates the widespread professional acceptance of this therapy.17
Research by Decousus et al2,12,17,18 confirms that compression therapy using gradient compression stockings or leg wraps is the current standard of care for patients with STP. A general rule of thumb would be to apply compression to the height of thrombus in the affected limb, with compression of either 20-30 mm Hg or 30-40 mm Hg, depending on the severity of venous insufficiency, skin changes, and presence of edema. The greater the findings, the greater the degree of compression therapy indicated.
Anticoagulation and anti-inflammatory agents
The prevalence of comorbid pathology and risk of complications with acute superficial thrombosis have led many investigators to favor systemic anticoagulation when the thrombus approximates the saphenous junctions and when more than 5 cm of the saphenous trunk is involved, as shown by duplex ultrasonography.18 The 2008 American College of Chest Physicians guidelines recommend low molecular weight heparin at prophylactic or intermediate doses for at least four weeks.19 Thrombosis isolated to superficial varicosities may be managed more conservatively by avoiding anticoagulation in favor of anti-inflammatory agents.
Role of antibiotics
The acute inflammatory response commonly seen with superficial phlebitis (Figure 1) can raise concerns about a potential infectious process. Contrary to their general appearance, these painful superficial lesions are almost always sterile.20 Fever, leukocytosis, and toxicity suggest an infectious process. Patients with suppurative thrombophlebitis require open drainage and broad-spectrum antibiotics. Unless the phlebitis is of the suppurative type or accompanied by clinical ascending lymphangiitis, there is no indication for the use of antibiotics.3,13
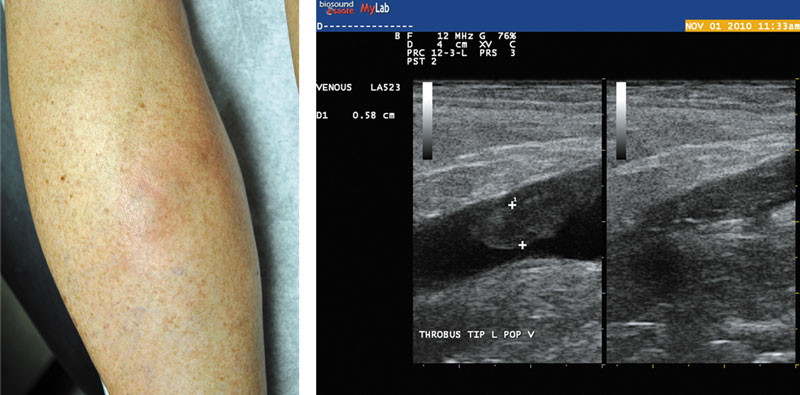
Figure 3. The prevalence of concomitant venous complications in patients with superficial thrombophlebitis mandates duplex ultrasound for each patient in whom this condition is suspected. This example shows a case of STP of the intersaphenous veins of the calf (left); corresponding duplex ultrasound (right) reveals that the pathology extends into the popliteal vein at the saphenopopliteal junction.
Surgical intervention

Figure 4. In cases in which bulbous varices are acutely inflamed, painful, and fluctuant, symptoms may be rapidly relieved with local incision and drainage. This minor in-office procedure is very well tolerated by patients and serves to dramatically reduce inflammation and pain, with the added benefit of reducing risk of pronounced hyperpigmentation over the affected region.
In cases in which bulbous varices are acutely inflamed, painful, and fluctuant, symptoms may be rapidly relieved with local incision and drainage. After cleansing the area, local anesthesia may be infiltrated with a small needle allowing for small incisions or punctures to be made over the regions of fluctuance. This is a simple bedside procedure that any physician or midlevel provider may perform. Once the punctures are made, the physician may effectively expel the superficial thrombus.21 This minor in-office procedure is very well tolerated by patients and serves to dramatically reduce inflammation and pain, with the added benefit of reducing risk of pronounced hyperpigmentation over the affected region (Figure 4).
Conclusion
Superficial vein thrombosis is more than a benign disease process.22 If merely 1% of these cases result in pulmonary embolism or VTE complications, thousands of lives are at risk.23 Diagnostic imaging is critical in determining the best course of action, and referral to a vein specialist may be warranted. Ambulation, compression therapy, and anticoagulant and anti-inflammatory agents make up the current standard of care, which depends on thrombus burden. Although large randomized trials are lacking,24 epidemiologic studies documenting the prevalence of DVT, pulmonary embolism, or both in patients with this condition warrant more aggressive medical therapy.
Marlin W. Schul, MD, MBA, RVT, is a dedicated vein specialist at the Lafayette Regional Vein Center in Lafayette, IN.
References:
1. Hingorani A, Ascher E. Superficial venous thrombophlebitis. In: Gloviczski P, ed. Handbook of Venous Disorders. 3rd ed. Oxford, England: Oxford University Press; 2009:314-319.
2. Quenet S, Laporte S, Decousus H, et al. Factors predictive of venous thrombotic complications in patients with isolated superficial vein thrombosis. J Vasc Surg 2003;38(5):944-949.
3. Feied C. Venous Thrombosis and Pulmonary Embolism. In: Marx J, Hockberger R, Walls R, eds. Rosen’s Emergency Medicine: Concepts and Clinical Practice. 5th ed. St. Louis, MO: Mosby; 2002: 1211-1212.
4. Sobreira ML, Maffei FH, Yoshida WB, et al. Prevalence of deep vein thrombosis and pulmonary embolism in superficial thrombophlebitis of the lower limbs: prospective study of 60 cases. Int Angiol 2009;28(5):400-408.
5. Coon W, Willis P, Keller J. Venous thromboembolism and other venous disease in the Tecumseh Community Health Study. Circulation 1973;48(4):839-846.
6. Lutter KS, Kerr TM, Roedersheimer LR, et al. Superficial thrombophlebitis diagnosed by duplex scanning. Surgery 1991;110(1):42-46.
7. Blättler W, Schwarzenbach B, Largiadér J. Superficial vein thrombophlebitis–serious concern or much ado about little? Vasa 2008;37(1):31-38.
8. Cotran R, Kumar V, Robbins S, eds. Robbins Pathologic Basis of Disease. 4th ed. Philadelphia, PA; WB Saunders Company:1989.
9. Bergqvist D, Jaroszewski H. Deep vein thrombosis in patients with superficial thrombophlebitis of the leg. Br Med J 1986;292(6521):658-659.
10. Dewar C, Panpher S. Incidence of deep vein thrombosis in patients diagnosed with superficial thrombophlebitis after presenting to an emergency department outpatient deep vein thrombosis service. Emerg Med J 2010;27(10):758-761.
11. Kakkos S, Lampropoulos G, Papadoulos S, et al. Seasonal variation in the incidence of superficial thrombophlebitis. Thromb Research 2010;126(2):98-102.
12. Decousus H, Epinat M, Guillot K, et al. Superficial vein thrombosis: risk factors, diagnosis, and treatment. Curr Opin Pulm Med 2003;9(5):393-397.
13. Cesarone M, Belcaro G, Agus G, et al. Management of superficial vein thrombosis and thrombophlebitis: status and expert opinion document. Angiology 2007;58(Suppl 1):S7-S15.
14. Jünger M, Diehm C, Störiko H, et al. Mobilization versus immobilization in the treatment of acute proximal deep vein thrombosis: a prospective, randomized, open, multicenter trial. Curr Med Research Opin 2006;22(3):593-602.
15. Partsch H, Blättler W. Compression and walking versus bed rest in the treatment of proximal deep venous thrombosis with low molecular weight heparin. J Vasc Surg 2000;32(5):861-869.
16. Ramelet A. Compression Therapy. Dermatol Surg 2002;28(1):6-10.
17. Decousus H, Quéré I, Presles E, et al. Superficial venous thrombosis and venous thromboembolism. Ann Intern Med 2010;152(4):218-224.
18. Decousus H, Bregeault M, Darmon J, et al. A pilot randomized double-blind comparison of a low-molecular weight heparin, a nonsteroidal anti-inflammatory agent, and placebo in the treatment of superficial vein thrombosis. Arch Intern Med 2003;163(14):1657-1663.
19. Kearon C, Kahn S, Agnelli, et al. Antithrombotic therapy for venous thromboembolic disease: American College of Chest Physicians evidence based clinical practice guidelines (8th Edition). Chest 2008;133(6 Suppl):454S-545S.
20. Allen E, Barker N, Hines E, et al. Peripheral Vascular Diseases. Philadelphia, PA: WB Saunders Company;1946: 636-638.
21. Neher J, Safranek S, Greenwald J. Clinical inquiries. What is the best therapy for superficial thrombophlebitis? J Fam Pract 2004;53(7):583-585.
22. Olubaniyi BO, Kumar S, Dimitri S, et al. Superficial thrombophlebitis
of lower limb veins – far from a benign condition. Br J Surg 2009;96(S1): 9-10.
23. Skillman JJ, Kent KC, Porter DH, Kim D. Simultaneous occurrence of superficial and deep thrombophlebitis in the lower extremity. J Vasc Surg 1990;11(6):818-824.
24. Leon L, Giannoukas AD, Dodd D, et al. Clinical significance of superficial vein thrombosis. Eur J Vasc Endovasc Surg 2005;29(1):10-17.