A pilot study has demonstrated the feasibility and potential success for employing the Internet to deliver targeted individualized exercise routines for patients with knee osteoarthritis, which may help to address the underutilization of exercise in this patient population.
A pilot study has demonstrated the feasibility and potential success for employing the Internet to deliver targeted individualized exercise routines for patients with knee osteoarthritis, which may help to address the underutilization of exercise in this patient population.
By Alison Brooks, MD; Bryan Heiderscheit, PT, PhD; and John E. Beaulieu, PhD
In the US, knee osteoarthritis (OA) is the most common joint disorder and ranks as one of the five leading causes of disability.1,2 There are an estimated 19.5 million adults in the US with symptomatic knee OA,3,4 with a projected increase in prevalence of 40% over the next 20 years.1,5,6 For community-dwelling adults aged 50 years and older, knee OA is the leading cause of disability during daily activities (eg, walking).7 This resulting decline in functional mobility places an undue burden on the aging population and seriously threatens their ability to live independently.8 Individuals with knee OA on average make six more visits annually to their physician and four more nonphysician visits to inpatient hospitals and emergency departments than their OA-free peers.2 For the years 1996 to 2005, the annual aggregate direct medical expenditures for OA were $185.5 billion.9
Treatment of knee OA with exercise is considered the cornerstone of conservative management of the disease.10 Aerobic, balance, and resistance training exercises, especially those involving the quadriceps and gluteal muscles, have produced beneficial changes in pain and function.11-15 The use of exercise has been consistently recommended in a number of recent national and international clinical practice guidelines for the nonarthroplasty management of those with knee OA.16-20
In two systematic reviews of the use of exercise for treating knee OA, it was found that more than 50% to 75% of the studies that used strengthening exercises reported greater improvements in pain and physical functioning compared with usual care, which included normal care by family physicians, nonweight-bearing exercises without progression, and health educational booklets on knee OA care.7,21 A meta-analysis of 32 randomized control trials with 3800 participants found that treating patients with knee OA using strengthening and aerobic exercises resulted in a pain reduction of about 40%.7
Exercise underutilization
Eighty-five percent of patients with knee OA enter the healthcare system through their primary care provider (PCP).22 The reported use of exercises to treat musculoskeletal problems is very low: 14% to 18%.23,24 It was observed that only 18% of patients with knee OA treated by rheumatologists had been counseled to incorporate exercises in their treatment plan.25 Considering that rheumatologists are two to three times more likely than PCPs and general internists to prescribe exercise for treatment of knee OA,24 a general estimate for the percentage of patients with knee OA that receive a general exercise prescription is likely less than 10%. Although the likelihood of exercise prescription or referral to physical therapy increases for patients with more severe knee OA,26 those with mild to moderate stages of the condition often do not receive this benefit. This is unfortunate, as strength exercises have been shown to be an effective front-line treatment for knee OA and are potentially most beneficial in its early stages.27,28
The primary reasons for the low rate of exercise prescription for musculoskeletal conditions by PCPs appear to be: limited contact time with the patient, lack of knowledge of published clinical guidelines, lack of training that results in an inadequate knowledge base about exercises, and lack of appropriate support materials.26,29-33 Many of these barriers may be overcome through simple changes in practice patterns; however, demands on physicians’ time continue to increase from a variety of directions. For example, the Affordable Care Act is expected to provide healthcare coverage for 30 million to 40 million new patients. Estimates are that, by 2025, the workloads for family practitioners and internists will increase by 28%.34
Further compounding the issue, it is estimated that by 2025 there will be a shortage of 46,000 PCPs.35 With the supply of physicians stretched thin, patients will confront longer delays for necessary care and potentially receive a lower quality of care. With physicians facing daunting patient loads and less time to provide quality care, suggestions for alleviating the situation include expanded roles for other healthcare providers (eg, nurse practitioners, physician assistants) and the integration of new technologies such as the Internet to improve the delivery of patient care.35
Internet possibilities
Currently more than 208 million US adults (81%) use the Internet.3,36 The average age at diagnosis of knee OA is 50 years, which means that 71% of adults aged 50 to 64 years and 40% of adults 65 years and older are online.36 Of Internet users living with a chronic medical condition, approximately 83% search online for information about their condition.37 Given the population’s familiarity with the Internet and the educational power it affords, developing a web-based knee OA exercise resource based on current practice standards has the potential to benefit both patients and providers.
Adherence to exercise programs by people with knee OA is known to be low.38 Although the benefits of exercise for treating knee OA are well known, adherence by knee OA patients to exercise programs ranges from 50% to 95%.39 Pain and stiffness are commonly cited reasons for knee OA patients not continuing with exercise prescriptions.39-41
Internet-delivered interventions for adults with chronic conditions increase the ability of patients to take an active role in the management of their condition by engaging in regular exercise and seeking and using health information. Tailored interventions that match a patient’s level of ability lead to changes in self-efficacy and desirable health-related behaviors.42 Tailoring exercise programs to individual characteristics, such as pain and function, coupled with self-pacing, are important components of improving exercise adherence in patients with knee OA.39,43
Computer-tailored Internet-based exercise interventions have been shown to produce longer-term physical adherence compared with comparable nontailored interventions.44,45 Further, the use of the Internet has the potential to achieve these positive outcomes at a lower cost of delivery, while requiring fewer professional resources compared with community or institution-based programs. Indeed, many of the barriers associated with in-person training, such as distance, cost of travel, funding limitations, and limited access to healthcare providers in rural areas, can be overcome by Internet-based delivery systems. Users can access the information at any time and from any location, increasing the likelihood of engaging in the intervention.46
Our research
In a recent eight-week pilot study47 funded by the National Institutes of Health, we developed a web-based Therapeutic Exercise Resource Center (TERC) that created and prescribed tailored exercise routines for patients with knee OA based on their self-reported level of stiffness, pain, and daily functioning.
The assigned exercises consisted of flexibility, strength, and balance exercises that targeted the hamstring, gluteal, and quadriceps muscles. Also included, based on published guidelines,48,49 were aerobic recommendations that consisted of a progressive walking program that increased on a weekly basis. We then tested whether the use of the TERC as part of management for knee OA would improve patient-reported clinical outcome measures over an eight-week period.
The structure of the TERC involved five progressively difficult exercise levels, with level 1 being the easiest. Upon entering the TERC, a patient’s level of stiffness, pain, and functioning were assessed using a modified short form of the Western Ontario and McMaster Universities Arthritis Index (mSF-WOMAC), along with an exercise history and general health questionnaire. Based on this information a placement algorithm was designed to assign patients into one of the five exercise levels that was determined to be most appropriate based on their self-reported parameters.
After using the program for a few days, patients could request the TERC to create an easier or more difficult routine. If the patient requested an easier routine, he or she was immediately given a new and easier exercise routine. If a more difficult routine was requested the patient was re-administered the mSF-WOMAC. To receive a more difficult routine the patient’s score needed to be equal to or less than the prior mSF-WOMAC score; otherwise the patient would be given a new routine without changing the level of exercise difficulty.
All exercises were shown to the patient using high-quality motion-captured animations demonstrating the proper execution (Figure 1). Additionally, line drawing representations of exercises could be viewed accompanied by written instructions describing how the exercise should be performed. Patients were asked to perform their exercises five times per week and to maintain an exercise log that included noting whether their knee pain increased as a result of the exercise session.
Throughout the study the TERC monitored each patient’s online exercise log and sent automated email notifications when specific criteria were met. If a patient reported three consecutive sessions with increased pain, an email was sent advising him or her to request an easier routine. If a patient reported no pain over a two-week period and had not requested a more difficult exercise routine, the TERC sent an email recommending the patient request a more difficult exercise routine. If a patient did not record any information for seven consecutive days an email was sent explaining the benefits of exercise for knee OA and encouraging him or her to record workouts in the exercise log. A healthcare professional was available by telephone to address concerns and answer questions about symptoms and exercises.
Sixty-five patients diagnosed with mild to moderate knee OA were enrolled in the pilot study, with 52 completing the full eight weeks. Inclusion criteria included not having had physical therapy during the previous year. However, 41 participants reported receiving some prior physical therapy and 21 of these reported continuing the exercises to some degree. Nonetheless, many of these participants reported improved symptoms over the course of the study.
Findings
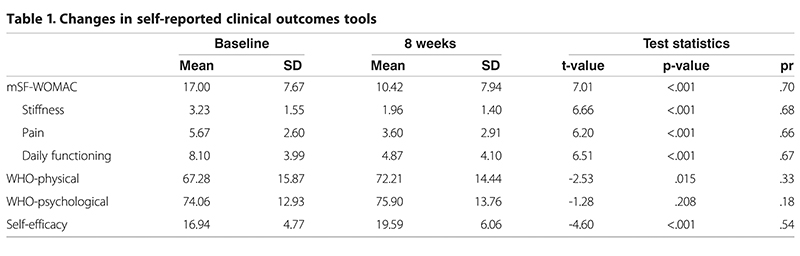
In short, the eight-week pilot study demonstrated the TERC has potential to improve clinical outcomes for patients with mild to moderate knee OA. All patients self-reported measures of pain, stiffness, and functioning as measured by the mSF-WOMAC and demonstrated a significant decrease in their mSF-WOMAC scores, indicating less pain and stiffness and increased function. Significant increases were also seen on the daily activities subscale of the Knee Self-Efficacy (K-SES)50 and in the physical domain of the World Health Organization Quality of Life scale (WHO-QOL)51 (Table 1).
All patients were asked to exercise five days a week. Self-reported compliance with the recommended exercise regimen was high and, on average, patients reported performing their knee exercises four to five times per week.
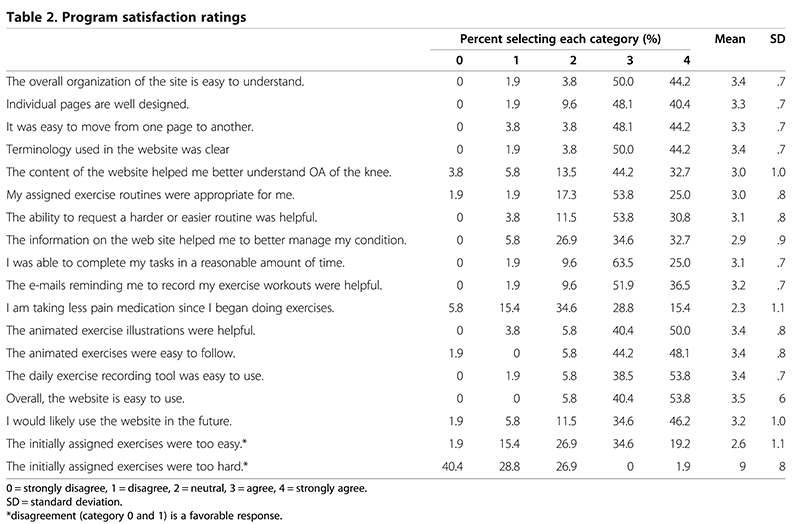
The patient consumer satisfaction survey reported a high degree of satisfaction with the website, with the majority reporting that their participation resulted in better understanding and management of their knee OA condition. More than 90% reported that the animations were especially helpful in demonstrating proper exercise technique. Approximately 79% of the patients thought the initial exercise level placement was appropriate, with just 1.9% requesting an easier exercise level after initial placement. Almost half of the patients reported a reduction in their pain medication over the study duration. Eighty percent of the patients said they would like to continue to use the website in the future, indicating a high degree of user satisfaction (Table 2).
Conclusions
With the plethora of literature supporting the early use of exercise for the treatment of mild to moderate knee OA, it is surprising that so few current patients are offered exercise as a treatment option. And, among those that are, the exercise may often be generic and nontailored to the individual patient’s symptoms and function. The underutilization of exercise for treating knee OA can result in a decline in functional mobility and threaten the ability of the aging population with knee OA to live independently, placing an enormous financial burden on society.8
With a projected increase in knee OA of 40% over the next 20 years, alternative methods of delivering individualized exercise programs will be critical for mitigating the detrimental and costly effects of knee OA on both individuals and society. The internet has several advantages that can make it an important delivery system for treating knee OA. For example, the Internet overcomes barriers of time and travel, can tailor programs to individual characteristics, allows for self-pacing, overcomes limitations of a fixed number of office visits, and can serve as a life-long resource for managing knee OA.
The TERC has the potential to be a complementary Internet-based system that will enhance traditional office-based practices for treating knee OA patients. The TERC contains several safeguards to alert clinic staff to patient needs for further evaluation and treatment. For example, when a patient is placed in exercise level 1 and requests an easier routine, email messages are sent to both the patient and their provider explaining why the TERC is not an appropriate treatment for this patient. In these cases, patient access to the TERC is terminated and the patient is counseled to see their healthcare provider for further evaluation.
The encouraging results of our pilot study demonstrate the feasibility and potential success for employing the Internet to deliver targeted individualized exercise routines for patients with knee OA. If future randomized controlled studies of the TERC support these findings, current practice patterns may evolve such that web-based exercise prescription become more commonplace and extends to other chronic musculoskeletal conditions.
Alison Brooks, MD, is an assistant professor of pediatrics and orthopedics at the University of Wisconsin-Madison School of Medicine and Public Health in Madison. Bryan Heiderscheit, PT, PhD, is a professor in the departments of Orthopedics & Rehabilitation and Biomedical Engineering at the University of Wisconsin-Madison, and codirector of the university’s Neuromuscular Biomechanics Laboratory. John E. Beaulieu, PhD, is president and chief executive officer of Visual Health Information in Tacoma, WA, a company that has been involved with physical rehabilitation for more than 30 years. Beaulieu is the creator of the TERC concept and was principal investigator for the research funded by the National Institutes of Health.
Disclosures:
John E. Beaulieu, PhD, is president/chief executive officer of Visual Health Information (VHI), which obtained the funding for this project through a Small Business Innovative Research Grant through the National institutes of Health. VHI owns the TERC website and has made a patent application for all assets related to the knee osteoarthritis website. Bryan Heiderscheit, PT, PhD, has received consulting fees from VHI for work unrelated to the manuscript under review.
- Dillon CF, Rasch EK, Gu Q, Hirsch R. Prevalence of knee osteoarthritis in the United States: ArthritisdData from the Third National Health and Nutrition Examination Survey 1991-94. J Rheumatol 2006;33(11):2271-2279.
- Wright E, Katz, J, Cisternas M, Kessler C, et al. Impact of knee osteoarthritis on health care resource utilization in a US Population-based national sample. Med Care 2010;48(9):785-791
- Howden LM, Meyer JA. Age and sex composition: 2010. US Census Bureau website. http://www.census.gov/prod/cen2010/briefs/c2010br-03.pdf. Published May 2011. Acessed November 5, 2014.
- Jordan JM, Helmik CG, Renner JB, et al. Prevalence of knee symptoms and radiographic and symptomatic knee osteoarthritis in African Americans and Caucasians: The Johnston County Osteoarthritis Project. J Rheumatol 2007;34(1):172-180.
- Belo JN, Berger MY, Reijman M, et al. Prognostic factors of progression of osteoarthritis of the knee: a systematic review of observational studies. Arthritis Rheum 2007;57(1):13-26.
- Lawrence RC, Felson DT, Helmick CG, et al. Estimates of the prevalence of arthritis and other rheumatic conditions in the United States: Part II. Arthritis Rheum 2008;58(1):26-35.
- Fransen M, McConnell FM. Exercise for osteoarthritis of the knee. Cochrane Database Syst Rev 2008;(4):CD004376.
- Dunlop DD, Manheim LM, Yelin EH, et al. The costs of arthritis. Arthritis Rheum 2003;49(1):101-113.
- Kotlarz H, Gunnarsson CL, Fang H, Rizzo JA. Insurer and out-of-pocket costs of osteoarthritis in the US: evidence from national survey data. Arthritis Rheum 2009;60(12):3546-3553.
- Bennell KL, Hinman RS. A review of the clinical evidence for exercise in osteoarthritis of the hip and knee. J Sci Med Sport 2011;14(1):4-9.
- Bennell KL, Hunt MA, Wrigley TV, et al. Role of muscle in the genesis and management of knee osteoarthritis. Rheum Diseases Clin North Am 2008;34(3):731-754.
- Topp R, Woolley S, Hornyak J 3rd, et al. The effect of dynamic versus isometric resistance training on pain and functioning among adults with osteoarthritis of the knee. Arch Phys Med Rehabil 2002;83(9):1187-1195.
- Jan MH, Lin CH, Lin YF, et al. Effects of weight-bearing versus nonweight-bearing exercise on function, walking speed, and position sense in participants with knee osteoarthritis: a randomized controlled trial. Arch Phys Med Rehabil 2009;90(6):897-904.
- Iwamoto J, Sato Y, Takeda T, Matsumoto H. Effectiveness of exercise for osteoarthritis of the knee: A review of the literature. World J Orthop 2011;2(5):37-42.
- Diracoglu D, Aydin R, Baskent A, Celik A. Effects of kinesthesia and balance exercises in knee osteoarthritis. J Clin Rheumatol 2005;11(6):303-310.
- Jordan KN, Arden NK, Doherty M, et al. EULAR Recommendations (2003): an evidence based approach to the management of knee osteoarthritis: Report of a Task Force of the Standing Committee for International Clinical Studies Including Therapeutic Trials (ESCISIT). Ann Rheum Dis 2003;62(12):1145-1155.
- Zhang W, Moskowitz RW, Nuki G, et al. OARSI recommendations for the management of hip and knee osteoarthritis, Part II: OARSI evidence-based, expert consensus guidelines. Osteoarthritis Cartilage 2008;16(2):137-162.
- Hochberg MC, Altman, RD, April, KT, et al. American College of Rheumatology 2012 recommendations for the use of non pharmacological and pharmacological therapies in osteoarthritis of the hand, hip, and knee. Arthritis Care Res 2012;64(4):455-474.
- Zhang W, Doherty, M. EULAR recommendations for knee and hip osteoarthritis: a critique of the methodology. Br J Sports Med 2006;40(8):664-669.
- American Academy of Orthopaedic Surgeons. Treatment of osteoarthritis of the knee; evidence-based guidelines. 2nd edition. http://www.aaos.org/research/guidelines/treatmentofOsteoarthritisoftheKneeGuideline.pdf. Published May 13, 2013. Acessed November 5, 2014.
- Lange AK, Vanwanseele B, Fiatarone Singh MA. Strength training for treatment of osteoarthritis of the knee: a systematic review. Arthritis Rheum 2008;59(10):1488-1494.
- Medifocus staff. Osteoarthritis of the knee: a comprehensive guide to symptoms, treatment, research and support. www.medifocus.com; 2012.
- Freburger JK, Carey TS, Holmes GM, et al. Exercise prescription for chronic back or neck pain: Who prescribes it? Who gets it? What is prescribed? Arthritis Rheum 2009;61(2):192-200.
- Mazzuca SA, Brandt KD, Katz BP, et al. Comparison of general internists family physicians and rheumatologists managing of patients with symptoms of osteoarthritis of the knee. Arthritis Care Res 1997;10(5):289-299.
- DeHaan MN, Guzman J, Bayley MT, Bell MJ. Knee osteoarthritis clinical practice guidelines — How are we doing? J Rheumatol 2007;34(10):2099-2105.
- Glauser TA, Salinas GD, Roepke NL, et al. Management of mild-to-moderate osteoarthritis: A study of the primary care prespective. Postgrad Med 2011;123(1):126-134.
- Farr JN, Going SB, McKnight PE, et al. Progressive resistance training improves overall physical activity levels in patients with early osteoarthritis of the knee: a randomized controlled trial. Phys Ther 2010;90(3):356-366.
- McKnight PE, Kasle S, Going S, et al. A comparison of strength training, self-management, and the combination for early osteoarthritis of the knee. Arthritis Care Res 2010;62(1):45-53.
- Peterson J. Get moving! Physical activity counseling in primary care. J Am Acad Nurse Pract 2007;19(7):349-357.
- Der Ananian CD, Wilcox S, Saunders R, et al. Factors that influence exercise among adults with arthritis in three activity levels. Prev Chronic Dis 2006;3:A81.
- Raissi GR, Mansoori K, Madani P, Rayegani SM. Survey of general practitioners’ attitudes toward physical medicine and rehabilitation. Int J Rehabil Res 2006;29(2):167-170.
- Ainsworth BE, Youmans CP. Tools for physical activity counseling in medical practice. Obes Res 2002;10(1):69-78.
- Østbye T, Yarnhall KS, Krause KM, et al. Is there time for management of patients with chronic diseases in primary care? Annals Fam Med 2005;3(3):209-214.
- Schwartz M, Durning S, Linzer M, Hauer K. Changes in medical students’ views of internal medicine careers from 1990 to 2007. Arch Intern Med 2011;171(8):744-749.
- Dill JM, Salsberg ES. The complexities of physican supply and demand: Projections through 2025. Association of American Medical Colleges. http://www.innovationlabs.com/pa_future/1/background_docs/AAMC%20Complexities%20of%20physician%20demand,%202008.pdf. Published November 2008. Accessed November 5, 2014.
- State of the Media: U.S. Digital Consumer Report. Q3-Q4 2011. Nielson website. http://www.nielsen.com/us/en/insights/reports/2012/us-digital-consumer-report.html. Published February 23, 2012. Accessed November 5, 2014.
- Fox S. Health Topics. Pew Internet & American Life Project. 2011;http://www.pewinternet.org/~/media//Files/Reports/2011/PIP_Health_Topics.pdf Published January 1, 2011. Accessed November 5, 2014.
- Lin SY, Davey RC, Cochrane T. Community rehabilitation for older adults with osteoarthritis of the lower limb: a controlled clinical trial. Clin Rehabil 2004;18(1):92-101.
- Marks R. Knee osteoarthritis and exercise adherence: a review. Curr Aging Sci 2012;5(1):72-83.
- Campbell R, Evans M, Tucker M, et al. Why don’t patients do their exercises? Understanding non-compliance with physiotherapy in patients with osteoarthritis of the knee. J Epidemiol Community Health 2001;55(2):132-138.
- Thomas KS, Muir KR, Doherty M, et al. Home based exercise programme for knee pain and knee osteoarthritis: randomised controlled trial. BMJ 2002;325(7367):752.
- Solomon M, Wagner SL, Goes J. Effects of a web-based intervention for adults with chronic conditions on patient activation: Online randomized controlled trial. J Med Internet Res 2012;14(1):e32.
- Marks R. Knee osteoarthritis and exercise adherence: A review. Curr Aging Sci 2012;5(1):72-83.
- Pekmezi DW, Williams DM, Dunsiger S, et al. Feasibility of using computer-tailored and internet-based interventions to promote physical activity in underserved populations. TeleMed J E Health 2010;16(4):498-503.
- Marcus BH, Lewis BA, Williams DM, et al. A comparison of Internet and print-based physical activity interventions. Arch Int Med 2007;167(9):944-949.
- Russell TG, Buttrum P, Wootton R, Jull GA. Internet-based outpatient telerehabilitation for patients following total knee arthroplasy: A randomized controlled trial. J Bone Joint Surg Am 2011;93(2):113-120.
- Brooks MA, Beaulieu JE, Severson HH, et al. Web-based therapeutic exercise resource center as a treatment for knee osteoarthritis: a prospective cohort pilot study. BMC Musculoskelet Disord 2014;15:158.
- Buchner DM, Bishop J, Brown DR. 2008 physical activity guidelines for Americans: Be active, healthy and happy! Health.gov website. http://www.health.gov/paguidelines/guidelines/. Updated November 5, 2014. Accessed November 5, 2014.
- A national public health agenda for osteoarthritis. Centers for Disease Control and Prevention website. http://www.cdc.gov/arthritis/osteoarthritis.htm. Updated July 8, 2014. Accessed November 5, 2014.
- Thomee P, Wahrborg P, Borjesson M, et al. A new instrument for measuring self-efficacy in patients with an anterior cruciate ligament injury. Scand J Med Sci Sports 2006;16(3):181-187.
- Ackerman IN, Graves SE, Bennell KL, Osborne RH. Evaluating quality of life in hip and knee replacement: Psychometric properties of the World Health Organization Quality of Life short version instrument. Arthritis Rheum 2006;55(4):583-590.