 To understand the association between jumping biomechanics and transmission of forces through the patellar tendon, practitioners must have a working knowledge of the anatomy of the knee, as well as the biomechanical factors that determine force transmission through the knee.
To understand the association between jumping biomechanics and transmission of forces through the patellar tendon, practitioners must have a working knowledge of the anatomy of the knee, as well as the biomechanical factors that determine force transmission through the knee.
By Rob Halle, PT, DPT, OCS, CSCS
Patellar tendinopathy (PT), or “jumper’s knee,” is a cause of knee pain that ultimately results in impaired healing of the tendon and a breakdown of the tendon’s key function: its load-absorbing and transmitting properties.1,2 PT is most common in athletes, particularly those who engage in sports that demand explosive, powerful movements such as jumping.3-5 Among sports, PT is most common in volleyball and basketball, with a prevalence rate in elite volleyball and basketball players of 45% and 32%, respectively; overall prevalence in elite athletes is 14.2%.5 Prevalence among nonelite volleyball players is reported to be 14.4%, with overall prevalence of 8.5% among nonelite athletes.6 PT not only causes pain, which limits the function of the affected tendons, but can also be associated with a loss in performance and ability to participate in sporting activities. Kettunen et al7 reported 53% of athletes suffering from PT had ended their athletic careers due to the condition at a 15-year follow-up.
Despite the prevalence and potential negative repercussions, the etiology of this condition remains largely unknown.3 Possible risk factors include age, gender, body mass index, leg-length difference, arch height, hamstring flexibility, ankle dorsiflexion range of motion, playing surface, amount of training, and stronger quadriceps. The primary risk factors, however, may be related to the biomechanics of jumping and landing from a jump.8,9 Improper landing technique may increase tendon strain and the transmission of forces through the patellar tendon, thereby increasing the likelihood of developing PT.9-11 To understand the association between jumping biomechanics and transmission of forces through the patellar tendon, one must have a working knowledge of the anatomy of the knee, as well as the biomechanical factors that determine force transmission through the knee.
Knee extensor mechanism
The patellofemoral articulation and associated musculotendinous structures are often referred to as the extensor mechanism of the knee. Although this motor unit does provide concentric extension of the knee, it also works eccentrically during the gait cycle and activities like jumping and squatting.12
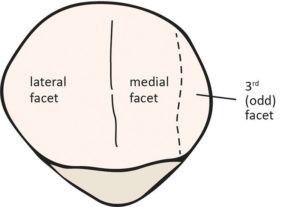
The patella, the largest sesamoid bone in the body, features insertions from the quadriceps muscles proximally and the patellar tendon distally. The superficial surface of the patella is concave, and its articular surface contains three facets (Figure 1) and a vertical central ridge. The lateral facet is broad and is separated from the smaller medial facet and the more medial odd facet by the vertical central ridge. The patella articulates with the anterior articular surface of the distal femur at the femoral sulcus. The lateral articular surface of the femur matches the patella and is broader than the smaller medial articular surface of the femur.12,13
The proximal insertion of the patellar tendon is the inferior pole of the patella, and the distal insertion of the patellar tendon is the tibial tubercle. The tendon transmits force produced by the quadriceps across the knee joint to its insertion on the tibia, thereby generating an extension torque. The transmission of forces and cumulative load placed on the patellar tendon throughout active knee extension is influenced by the patella and its effect on quadriceps function. The mechanical efficiency of the quadriceps is greatly improved by the patella because it enables the patellar tendon to lengthen the moment arm of the quadriceps. The patella therefore functions as an anatomic pulley, deflecting the line of quadriceps action away from the joint. This pulley action increases the angle of pull and the ability of the quadriceps to generate an extension torque.14 The loss of the patella has been shown to decrease torque of the quadriceps by 49% (Figure 2).14 By dividing torque or moment of the quadriceps by the moment arm, it is possible to calculate the force acting on the patellar tendon.9,15 Although mechanical loading is essential for the health and performance of tendons, the magnitude and characteristics of optimal loading are still largely unknown, and overloading the patellar tendon has been shown to increase the risk of an athlete developing PT.15
Landing biomechanics
As mentioned previously, PT is most common in the volleyball and basketball populations, in which jumping is a key aspect of performance. In addition to transmitting force from the quadriceps to create extension, the patellar tendon aids the other joints of the lower limb in dissipating the kinetic energy generated when landing from a jump.9,16
A 2006 cross-sectional study evaluated performance measures in 113 male and female volleyball players, along with their flexibility and strength.16 Outcome measures included sit and reach flexibility, dorsiflexion range of motion, jump height, and ankle plantar flexor strength. Ultrasound imaging of the tendon was also performed.
Approximately 25% of the individuals had hyperechoic and thickened proximal portions of their patellar tendons, known precursors of PT. Of the outcome measures assessed in this study, loss of dorsiflexion range of motion was the only metric associated with PT. Athletes with less than 45° of ankle dorsiflexion were 1.8 to 2.8 times more likely to have abnormal findings on imaging of the patellar tendon than those with more than 45° of dorsiflexion. This may be due to the role the ankle joint plays in the absorption of landing forces. During landing from a jump, the forefoot contacts the ground and the ankle moves into dorsiflexion. This is coupled with eccentric activation of the calf muscles and is responsible for absorbing approximately 37% of the total kinetic energy produced when landing from a jump.16,17 A decrease in ankle dorsiflexion that alters this biomechanical pattern may increase load at the patellar tendon during jumping activities and, in turn, increase the risk of PT or other patellar tendon injury.16
To further elucidate the understanding of joint kinematics and their effects on patellar tendon loads, Edwards and colleagues performed a study comparing two phases of a stop-jump landing task.18 The two phases of the landing task were the horizontal phase and the vertical phase. Each participant was asked to accelerate forward for four steps toward two force plates, stop, and perform a symmetrical two-foot landing on the force plates; this described the horizontal phase. Immediately after landing, the participant would jump vertically, strike a ball that was suspended from the ceiling, and perform a symmetrical two-foot landing on the force plates; this described the vertical phase. The authors used motion-capture cameras, light-emitting diodes placed on the skin, and force plates to measure joint kinetics and kinematics for the two landing phases.

Figure 2: This figure demonstrates the changed action line of the quadriceps (arrow) and the decreased moment arm that results from the removal of the patella (dotted line). MA = moment arm.
Horizontal jump landing, which is common in sports such as volleyball and basketball, was associated with a significantly higher mean patellar tendon load (force), a higher patellar tendon loading rate, a higher mean knee joint moment, greater hip flexion at initial contact, and a faster time to reach maximum patellar tendon force compared with vertical jump landing (Figure 3).
Edwards et al18 speculated that decreased dorsiflexion range of motion and landing with greater knee and hip flexion may lead to increased patellar tendon load (force) experienced during the horizontal landing phase. Joint kinematic data revealed that, during the vertical jump landing, participants also landed with significantly greater plantar flexion at initial contact and proceeded to move into greater dorsiflexion range of motion at the time of maximum patellar load compared with the horizontal landing phase. During horizontal landing, participants’ dorsiflexion range of motion remained virtually unchanged from time of initial contact to time of maximum patellar tendon load. During the horizontal landing phase, participants also landed with significantly greater knee and hip flexion at initial contact relative to the vertical landing phase.18 These results suggest the horizontal phase of the stop-jump movement places the highest load on the patellar tendon, potentially leading to the development of patellar tendinopathy.
Systematic review
A systematic review investigating the relationship between jumping mechanics and PT was performed in 2014.19 It included six cross-sectional studies due to the lack of prospective studies at the time of the review. Several of the studies compared participants with active PT with controls, while others compared controls with participants who had either experienced PT in the past or who were asymptomatic with patellar tendon abnormalities on imaging. In those who had active PT and those with a history of PT, kinematics did not differ significantly from controls.

Figure 3: Depiction of lower limb alignment at time of peak patellar tendon load during the horizontal (left) and vertical (right) landing phases of the stop-jump task.
The authors did note small, albeit statistically insignificant, differences in several areas. Compared with controls, participants with active PT demonstrated smaller maximum ankle dorsiflexion range of motion, a smaller maximum angular acceleration of the hip, and a larger maximum knee flexion angle during landing. Participants with active PT also displayed less angular velocity of the knee than controls during the eccentric portion of jump takeoff. Individuals with a history of PT exhibited smaller plantar flexion angles at initial contact than controls. During landing, they also demonstrated a smaller change in knee range of motion from initial contact to peak vertical ground reaction force, less knee flexion at the time of peak vertical ground reaction force, and a greater eccentric angular velocity of the knee.
Because patellar tendon abnormality is thought to be a precursor to tendinopathy, it has been said that individuals with such abnormalities have jump biomechanics that may lead to the development of PT.11,19 Most differences between the tendon abnormality group and controls existed during the horizontal landing phase. At initial contact, more hip and knee flexion were noted in those with tendon abnormalities than in controls, along with higher hip and knee extension velocities. At the time of peak patellar tendon load, they also had more knee angular velocity, more hip adduction, and greater hip external rotation velocity. These results suggest that patellar tendon abnormality is associated with higher angular velocities and a less upright position during landing. The larger hip and knee flexion angles at landing limit the available range of motion and decrease the displacement of the center of mass after touchdown. This increased stiffness of the landing can increase loading rates and peak patellar tendon forces.19
Prospective findings
 Despite the existence of a relevant systematic review, it is difficult to draw strong conclusions from these data, partially because of the studies’ cross-sectional design. The first prospective cohort to examine the relationship between stiff landing mechanics and the development of PT was published in 2016.8 The 49 study participants (17 women) included the members of three basketball teams, two volleyball teams, and one korfball team. A landing error scoring system (LESS) jump test was performed at the start of the sports season, as was 3D motion analysis measuring kinetics and kinematics of jumping and landing. The horizontal phase of the LESS was performed with the player jumping from a 30-cm high box onto two force plates used to measure ground reaction forces. Each force plate was placed in front of the box at a distance half the participant’s height. Participants were instructed to land with both feet, one on each plate, and immediately perform a maximal vertical jump. Participants were followed over the course of one to two athletic seasons.
Despite the existence of a relevant systematic review, it is difficult to draw strong conclusions from these data, partially because of the studies’ cross-sectional design. The first prospective cohort to examine the relationship between stiff landing mechanics and the development of PT was published in 2016.8 The 49 study participants (17 women) included the members of three basketball teams, two volleyball teams, and one korfball team. A landing error scoring system (LESS) jump test was performed at the start of the sports season, as was 3D motion analysis measuring kinetics and kinematics of jumping and landing. The horizontal phase of the LESS was performed with the player jumping from a 30-cm high box onto two force plates used to measure ground reaction forces. Each force plate was placed in front of the box at a distance half the participant’s height. Participants were instructed to land with both feet, one on each plate, and immediately perform a maximal vertical jump. Participants were followed over the course of one to two athletic seasons.
Of the 49 athletes who participated in the study, only three developed PT, an annual incidence of only 4.5%. Two of the three exhibited less range of motion in the lower extremity joints at baseline than controls, but not for all joints. One had a large hip flexion angle at initial contact, which limited the available range of motion change toward flexion and resulted in a stiffer landing than in the uninjured athletes. Another player who developed PT had a large dorsiflexion angle at initial contact and a heel-first landing, which also limited the amount of joint range of motion change available to absorb excessive impact forces. The kinematics of the third athlete who developed PT did not differ significantly from those of the uninjured athletes.8
Since no common knee, ankle, or hip kinematic patterns could be identified in the three individuals who developed PT, these data suggest there may be more than one altered landing pattern associated with a high risk for PT. The commonality among the patterns in question in this study is that they demonstrated a decreased joint range of motion excursion resulting in a stiff landing, which is often associated with PT.8,16,18
Conclusion
Many risk factors have been identified for the development of patellar tendinopathy, including age, gender, training frequency, quadriceps strength, arch height, and leg-length difference.8,20 It has also been hypothesized that altered biomechanics and kinematics of landing may play a role in the development of PT. Several cross-sectional studies have demonstrated that kinematic differences and alterations exist in a population of individuals with patellar tendinopathy, abnormal patellar tendon imaging, or a history of PT. The majority of this research suggests that a limited excursion of joint range of motion from initial contact to the time of peak force on the patellar tendon contributes at least in part to any increased risk of PT associated with jump landing.8,9,11,17,19 It has also been pointed out that sport-specific horizontal type jump-landing techniques may be associated with a higher risk of developing PT than vertical jump-landing techniques.10,11,19 There is also some evidence to suggest athletes with increased lower extremity stiffness during landing may be at increased risk for developing PT.
Because much of this research is cross-sectional and does not lend itself to strong conclusions, additional research on associations between PT and jump landing in large prospective cohorts is needed. Even if such a relationship exists, it is also plausible that jump-landing biomechanics play only a small role in the big-picture etiology of PT. As noted previously, the onset of PT is often multifactorial, with intrinsic and extrinsic contributing factors. Current evidence suggests stiff landing mechanics combined with limited range of motion may play a part in development of patellar tendinopathy. Recognizing the multifaceted nature of the etiology of PT, treatment plans focusing on increasing dorsiflexion range of motion may aid in the prevention of this condition in the jumping athlete. Similarly, the development of strategies that emphasize joint excursion during landing, thus increasing landing time, may have comparable beneficial effects. Although more research is needed, the current body of knowledge may be useful in developing successful prevention strategies to guard against the development of patellar
tendinopathy.
Rob Halle, PT, DPT, OCS, CSCS, is a board-certified orthopedic physical therapist currently stationed at the United States Military Academy in West Point, NY, and a fellow in the US Army Baylor University Sports Physical Therapy Fellowship at West Point.
Acknowledgment: Special thanks to Jinnie Wick and Eliza Szymanek for their assistance with the preparation of this manuscript.
Disclosure: The opinions or assertions contained herein are the private views of the authors and are not to be construed as official or as reflecting the views of The United States Military Academy, the US Army, or the Department of Defense.
- Kountouris A, Cook J. Rehabilitation of Achilles and patellar tendinopathies. Best Pract Res Clin Rheumatol 2007;21(2):295-316.
- Peers KH, Lysens RJ. Patellar tendinopathy in athletes. Sports Med 2005;35(1):71-87.
- Hale SA. Etiology of patellar tendinopathy in athletes. J Sport Rehabil 2005;14(3):259-272.
- Elvin N, Elvin A, Scheffer C, et al. A preliminary study of patellar tendon torques during jumping. J Appl Biomech 2009;25(4):360-368.
- Lian ØB, Engebretsen L, Bahr R. Prevalence of jumper’s knee among elite athletes from different sports a cross-sectional study. Am J Sports Med 2005;33(4):561-567.
- Zwerver J, Bredeweg SW, van den Akker-Scheek I. Prevalence of jumper’s knee among nonelite athletes from different sports A cross-sectional survey. Am J Sports Med 2011;39(9):1984-1988.
- Kettunen JA, Kvist M, Alanen E, Kujala UM. Long-term prognosis for jumper’s knee in male athletes a prospective follow-up study. Am J Sports Med 2002;30(5):689-692.
- van der Worp H, van der Does HT, Brink MS, et al. Prospective study of the relation between landing biomechanics and jumper’s knee. Int J Sports Med 2016;37(3):245-250.
- Janssen I, Steele JR, Munro BJ, Brown NA. Predicting the patellar tendon force generated when landing from a jump. Med Sci Sports Exerc 2013;45(5):927-934.
- van der Worp H, van Ark M, Roerink S, et al. Risk factors for patellar tendinopathy: a systematic review of the literature. Br J Sports Med 2011;45(5):446-452.
- Edwards S, Steele JR, McGhee DE, et al. Landing strategies of athletes with an asymptomatic patellar tendon abnormality. Med Sci Sports Exerc 2010;42(11):2072-2080.
- Flandry F, Hommel G. Normal anatomy and biomechanics of the knee. Sports Med Arthrosc Rev 2011;19(2):82-92.
- Moore KL, Dalley AF, Agur AM. Clinically oriented anatomy. Baltimore: Lippincott Williams & Wilkins; 2013.
- Levangie PK, Norkin CC. Joint structure and function: a comprehensive analysis. Philadelphia: FA Davis; 2011.
- Frohm A, Halvorsen K, Thorstensson A. Patellar tendon load in different types of eccentric squats. Clin Biomech 2007;22(6):704-711.
- Malliaras P, Cook JL, Kent P. Reduced ankle dorsiflexion range may increase the risk of patellar tendon injury among volleyball players. J Sci Med Sport 2006;9(4):304-309.
- Devita P, Skelly WA. Effect of landing stiffness on joint kinetics and energetics in the lower extremity. Med Sci Sports Exerc 1992;24(1):108-115.
- Edwards S, Steele JR, Cook JL, et al. Characterizing patellar tendon loading during the landing phases of a stop‐jump task. Scand J Med Sci Sports 2012;22(1):2-11.
- Van der Worp H, de Poel HJ, Diercks RL, et al. Jumper’s knee or lander’s knee? A systematic review of the relation between jump biomechanics and patellar tendinopathy. Int J Sports Med 2014;35(8):714-722.
- Janssen I, Steele JR, Munro BJ, Brown NA. Previously identified patellar tendinopathy risk factors differ between elite and sub‐elite volleyball players. Scand J Med Sci Sports 2015;25(3):308-314.








How do you measure the DF as pertaining to this article? Most people have a difficult time obtaining much past 10 to 15 degree’s of DF. Just curious. Thanks
Hello.
I am a 14 year old athlete, training regularly playing basektball and football. As of recent (past 2 months) I have developed what I think is patella tendonopathy/tendonitis. Yet to get diagnosed. From your writing I can tell that increased dorsi-flexion has a role in improving landing mechanics and decreasing load on the tendon. Do you think training the knee joint at maximul bend can strengthen the tendon, or training in positions that put load with your knees over your toes? Do you also reckon any treatments such as acupuncture would (given rest also) actually improve my tendon condition, or simply alleviate pain and not solve the issue?
Thank you for this very useful article. I would be very thankful for a response. Regards,
Henry Lim