 By Giacomo Farì, Laura Dell’Anna, Francesco Paolo Bianchi, Rachele Mancini, Enrica Chiaia Noya, Carlo De Serio, Riccardo Marvulli, Luisa De Palma, Danilo Donati, Roberto Tedeschi, Maurizio Ranieri, Marisa Megna, and Andrea Bernetti
By Giacomo Farì, Laura Dell’Anna, Francesco Paolo Bianchi, Rachele Mancini, Enrica Chiaia Noya, Carlo De Serio, Riccardo Marvulli, Luisa De Palma, Danilo Donati, Roberto Tedeschi, Maurizio Ranieri, Marisa Megna, and Andrea Bernetti
Integrating targeted exercises focused on AH strengthening, both pre- and post-surgery, offers a comprehensive approach to HV management.
The abductor hallucis (AH) is the most important muscle in the etiopathogenesis of hallux valgus (HV), but the effectiveness of its rehabilitation clashes with the difficulty of identifying the most suitable exercises to activate it. Therefore, the aim of this study was to compare 4 different therapeutic exercises in the activation of AH in these patients.
Methods
In this observational case-control study, 48 patients suffering from HV of moderate/severe grade, according to traditional radiographic classification and the Manchester scale, were divided into 2 groups: the case group underwent a monthly rehabilitation protocol for their foot deformity, whereas the control group was only evaluated without any intervention. The intervention comprised 3 40-minute sessions per week. The exercises were as follows: Toe Spread Out (TSO), Short Foot (SF), Forefoot Adduction (FA), and Flexion of the Metatarsophalanges (FM). Both groups were analyzed at baseline and 1 month later (at the end of rehabilitation for the case group) while performing the 4 exercises. Analysis was conducted using a surface electromyograph (sEMG) to record the muscle activity of AH in terms of root mean square (RMS) and maximum voluntary contraction (MVC).
Results
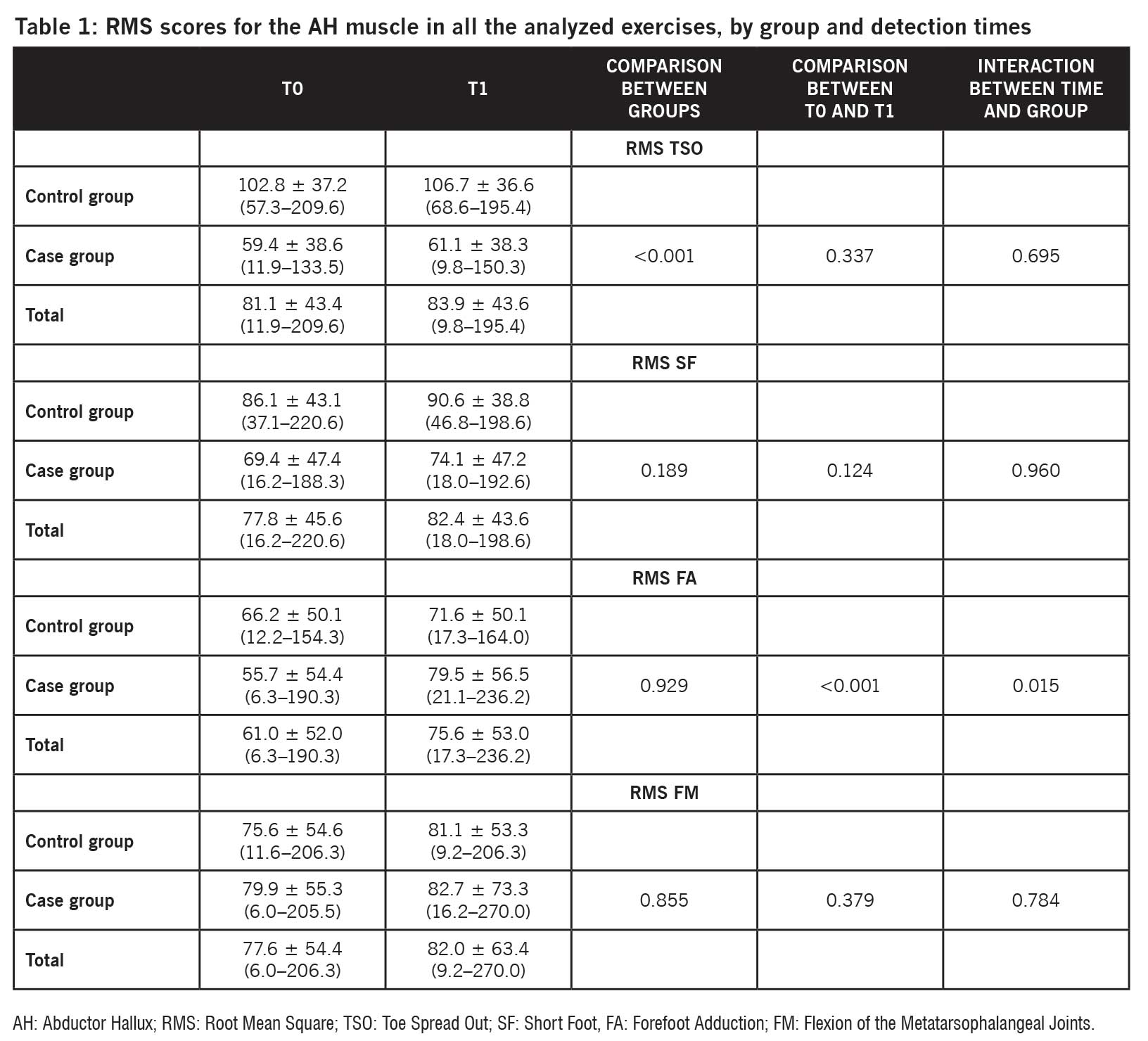
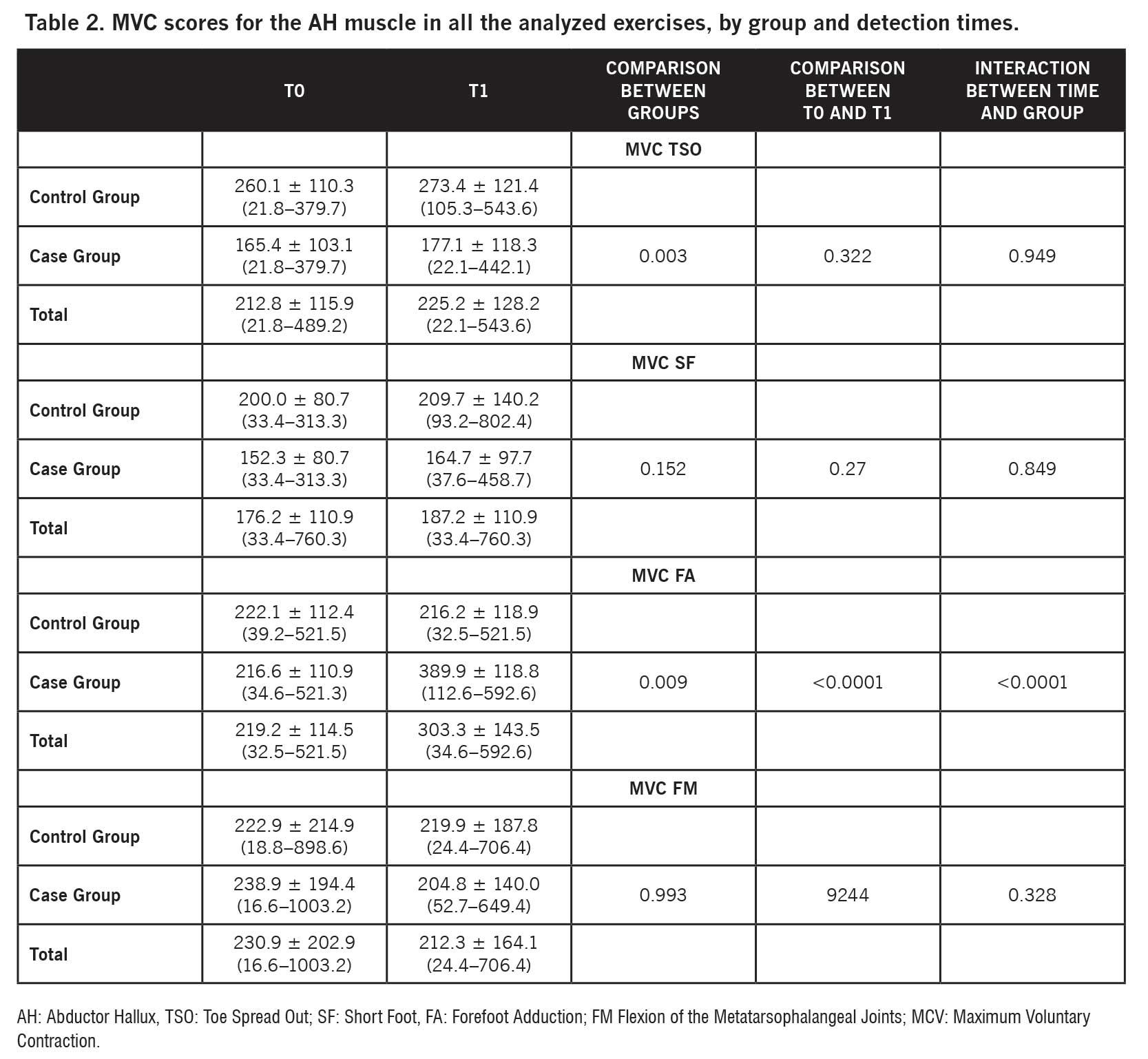
FA was the only exercise to determine a statistically significant improvement in AH at the end of the rehabilitation cycle, both in terms of RMS (P = 0.015; Table 1) and MVC (P < 0.0001; Table 2).
Discussion
These findings suggest that FA effectively stimulates the intrinsic AH muscle, enhancing the coordination and control of foot movements. Assessment of the MVC values further emphasized the results observed in the RMS measurements.
 TSO, SF, FM, and FA could play an important role in the rehabilitation of individuals suffering from HV, as enhancing the strength of the AH muscle can lead to better foot function, pain reduction, and the prevention of additional deformities. Strengthening the AH supports the medial longitudinal arch, potentially mitigating the severity of HV by maintaining proper foot alignment and reducing excessive pronation. Post-operative rehabilitation could be equally useful in restoring function and minimizing complications. By focusing on AH activation, rehabilitation can accelerate recovery and enhance post-surgical satisfaction by reinforcing foot mechanics and preventing recurrence.
TSO, SF, FM, and FA could play an important role in the rehabilitation of individuals suffering from HV, as enhancing the strength of the AH muscle can lead to better foot function, pain reduction, and the prevention of additional deformities. Strengthening the AH supports the medial longitudinal arch, potentially mitigating the severity of HV by maintaining proper foot alignment and reducing excessive pronation. Post-operative rehabilitation could be equally useful in restoring function and minimizing complications. By focusing on AH activation, rehabilitation can accelerate recovery and enhance post-surgical satisfaction by reinforcing foot mechanics and preventing recurrence.
Incorporating these exercises—TSO, SF, FM, and FA—into rehabilitation protocols can further facilitate muscle conditioning and stabilization of the first metatarsal joint, which are key factors in managing HV deformities. Integrating targeted exercises focused on AH strengthening, both pre- and post-surgery, offers a comprehensive approach to HV management.
Heo et al’s findings suggest that different exercises elicit varying degrees of AH activation, which is critical for clinicians when designing tailored rehabilitation programs aimed at maximizing muscle engagement. Hwang et al complemented these findings by employing pressure biofeedback units to investigate AH muscle activity specifically in patients with HV. This approach allows for a more comprehensive analysis of muscle function and engagement during rehabilitation exercises, enhancing the understanding of how targeted interventions can lead to improved clinical outcomes. The results on AH performance in TSO and SF can be explained by considering the instability of the first ray joint. The limitations in its range of motion (ROM) in patients with moderate-to-severe degrees of HV deformity hinder the execution of these exercises. The compromised ability to move the first ray is influenced not only by muscle imbalances but also by mechanical joint restrictions.
Exercises such as FA and FM are critical for restoring balance and coordination in individuals with HV. These exercises engage the entire musculature of the foot, bypassing the coordination and ROM necessary to correctly perform TSO and SF.
The findings herein suggest that FA may be easier for patients with severe deformities, leading to improvements in AH activity, primarily because it requires minimal abduction mobility of the first ray, which is typically compromised due to bony issues. Since FA involves a lower degree of mobility and coordination, its incorporation into exercise programs was particularly effective in enhancing the performance and activation of the AH in patients with significant deformities. By integrating FA exercises into rehabilitation protocols, physical therapists can create targeted exercise regimens specifically aimed at addressing deficiencies in muscle function for patients with conditions such as HV and other forefoot deformities. As patients engage in FA exercises, they learn to activate and control key muscle groups effectively, enhancing their overall foot biomechanics, ultimately leading to enhanced outcomes and quality of life.
 An ideal rehabilitation program for HV should encompass various components to effectively address the multifaceted nature of the condition as HV not only affects toe alignment but also influences overall foot mechanics, stability, and patient quality of life. This program may include the use of orthotic devices, such as toe separators, HV splints, and protective barriers for the great toe. Strengthening exercises targeting both the intrinsic and extrinsic muscles of the foot can enhance stability and functionality, thereby mitigating the progression of HV. Equally important are proprioceptive exercises, which should be integrated into the program to improve body awareness and balance. These exercises are essential for enhancing gait mechanics and reducing discomfort, particularly in individuals with compromised foot structures. Furthermore, educating patients on proper footwear choices and activity modifications can foster long-term adherence to rehabilitation protocols and contribute to better outcomes.
An ideal rehabilitation program for HV should encompass various components to effectively address the multifaceted nature of the condition as HV not only affects toe alignment but also influences overall foot mechanics, stability, and patient quality of life. This program may include the use of orthotic devices, such as toe separators, HV splints, and protective barriers for the great toe. Strengthening exercises targeting both the intrinsic and extrinsic muscles of the foot can enhance stability and functionality, thereby mitigating the progression of HV. Equally important are proprioceptive exercises, which should be integrated into the program to improve body awareness and balance. These exercises are essential for enhancing gait mechanics and reducing discomfort, particularly in individuals with compromised foot structures. Furthermore, educating patients on proper footwear choices and activity modifications can foster long-term adherence to rehabilitation protocols and contribute to better outcomes.
Conclusions
FA seems to be the best exercise to activate and train AH, so rehabilitation programs for patients suffering from hallux valgus should consider this exercise as the starting point for improving plantar support and overall foot biomechanics. It is essential to tailor these rehabilitation strategies to the specific characteristics of each case of HV, including the severity of the deformity and the individual’s unique functional limitations. Further studies are needed to deepen the effectiveness of this exercise, with the aim of implementing rehabilitation strategies and rethinking traditional HV therapies, which are currently predominantly surgical.
Giacomo Farì is affiliated with the Department of Experimental Medicine (Di.Me.S.), University of Salento, Lecce, Italy.
Laura Dell’Anna, Rachele Mancini, Enrica Chiaia Noya, Carlo De Serio, Riccardo Marvulli, Luisa De Palma, Maurizio Ranieri, and Marisa Megna are affiliated with the Department of Translational Biomedicine and Neuroscience (DiBraiN), Aldo Moro University, Bari, Italy.
Francesco Paolo Bianchi is affiliated with the Department of Biomedical Science and Human Oncology, Aldo Moro University of Bari, Italy.
Danilo Donati is affiliated with the Physical Therapy and Rehabilitation Unit, Policlinico di Modena and the Clinical and Experimental Medicine PhD Program, University of Modena and Reggio Emilia, Modena, Italy.
Roberto Tedeschi is affiliated with the Department of Biomedical and Neuromotor Sciences (DIBINEM), Alma Mater Studiorum University of Bologna, Italy.
Andrea Bernetti is affiliated with the Infradepartmental University Program of Physical and Rehabilitation Medicine, “V. Fazzi” Hospital, ASL Lecce, Italy.
This article has been excerpted from “Which is the best exercise for abductor hallucis activation in hallux valgus? A comparison study for new rehabilitation perspectives” Applied Sciences. 2025; 15(7):3523. https://doi.org/10.3390/app15073523. Editing has occurred, including the renumbering or removal of tables and figures, and references have been removed for brevity. Use is per CC BY.








Great read. Interesting how foot exercises can help with bunions. Usually, only pads, orthotics or surgery was the only options.
Atlas Biomechanics
https://www.atlasbiomechanics.com