 In this original investigation, researchers analyzed the biomechanical effects of a foot orthosis in patients with flexible flat foot during walking and the extent to which those functional effects are consistent with proposed theories about the device’s mechanism of action.
In this original investigation, researchers analyzed the biomechanical effects of a foot orthosis in patients with flexible flat foot during walking and the extent to which those functional effects are consistent with proposed theories about the device’s mechanism of action.
By Bruce Elliott, PT, DPT, COMT, and Juan Garbalosa, PhD, PT
Low arches, or flat feet, are associated with an increased risk of injury among physically active people, and it is widely believed that this type of foot tends to be more flexible than other foot types, allowing a disproportionate amount of pronation during the gait cycle.1,2 Researchers have theorized that flexible flat feet affect the movement and muscular activity patterns of the lower leg, predisposing such individuals to lower extremity musculoskeletal injuries.3-5
Excessive pronation at the subtalar joint and the transverse tarsal joint is associated with a flexible flat foot.6,7 It has been suggested that this foot type will contribute to a loss of ligamentous and osseous stability, necessitating increased muscular activity in the lower leg and foot to maintain that stability.8 Additionally, the lack of stability may cause an increase in the magnitude of the stress and shear forces that are transmitted to the soft connective tissues. Excessive pronation is the etiological variable most commonly linked to overuse injuries, and the subsequent increase in muscular activity and transmitted forces can ultimately lead to muscular fatigue, which is associated with a variety of overuse injuries.5,9
A biomechanical foot orthosis is commonly used for the management of lower extremity injuries that are related to overpronation or flexible flat feet.8,10 According to Root, realigning the posture of the foot is considered an effective intervention because abnormal foot posture is generally considered the cause of a wide variety of pathological conditions,11 and the flexible flat foot is managed with orthosis intervention more often than other foot types.4,5,9,12-14
Increasingly, foot orthoses have been successfully used as an adjunct treatment for symptoms that are secondary to increased flexibility. Of 465 podiatric patients reporting various maladies, 62% acknowledged complete resolution of their chief complaint after orthotic treatment, and an additional 33% gained partial resolution. Similarly, in a retrospective study with both temporary soft orthoses and permanent rigid orthoses, 96% of patients experienced pain relief, while 70% were able to return to previous levels of activity.15,16
Additionally, Nigg et al17 reported that at least 70% of runners who experience lower extremity musculoskeletal exertional pain will have a reduction in their symptoms with the use of a biomechanical orthosis. Based on static radiologic data, Bleck and Berzins,18 and later Bordelon and Lusskin,19 reported that significant correction of flexible flat foot deformity could be achieved by the use of orthoses. In contrast, Penneau et al20 and Wenger et al21 suggested the use of an orthotic device could not make permanent changes to a flat foot.
The use of foot orthoses in the treatment of abnormal foot biomechanics has been extensively described in the literature, and those interventions can be grouped into two categories—accommodative or corrective. Regardless of the orthotic prescription, it is difficult to judge the scientific merit of the recommendations that have been generated by these studies because of the conflicting opinions regarding the effectiveness of different orthoses.1,7,14,22
We conducted a study comparing the stance phase mechanics of symptomatic individuals with flexible flat feet during normal walking in a conventional sandal and in the same sandal with a maximal arch supination stabilization orthosis. The purpose of the study was to document the effect of the orthosis on the forefoot, medial longitudinal arch, and first ray mechanics of flexible flat feet during normal overland walking at a self-selected speed.
Methods and materials
We screened a convenience sample of 20 individuals for participation in this study. Thirteen met the inclusion criteria; two were lost to follow-up, and one participant’s data file became unusable. The 10 individuals (six women) who completed the study ranged in age from 20 to 54 years and reported various complaints of foot, heel, leg, and knee pain. Informed consent and a medical history were obtained from each participant prior to taking any measurements. Individuals were excluded if they had sustained any lower extremity fractures or injury to the capsular or ligamentous structures of the lower leg or foot within the past 12 months.
The inclusion criteria for the experiment were defined by the navicular drop test and the modified Gib test. Individuals were included in the study if they had a navicular drop greater than or equal to 10 mm bilaterally, and if they had at least 60° of frontal forefoot or rearfoot passive range of motion (as determined by the modified Gib test, illustrated in Figure 1)23 in both feet. The modified Gib test is recommended for orthosis prescription by the manufacturer; however, because of the subjective nature and less-than-adequate reliability of this test, we also used the navicular drop test to define an individual’s inclusion in the study.
Upon completion of the structural evaluation, participants were casted for a custom pair of orthoses according to standardized casting procedures of the orthosis manufacturer. One investigator performed all of the casting tasks. This sequential process entailed a gait-referenced weightbearing foam box casting, which captures the maximal amount of arch that one can comfortably achieve at midstance with the heel and forefoot in full contact with the ground (Figure 2). Once accomplished, the casts and orthosis prescription were shipped to the manufacturer.
At the second visit, approximately two weeks later, proper fit of the orthosis was verified and study participants were instructed on their break-in and use. The orthosis featured a semirigid thermoplastic heel cup extending to the base of the metatarsals with a full-length, 1/8-in thick, perforated ethylene vinyl acetate top cover (Figure 3). The individuals used their own footwear during the six-week break-in period and were allowed to take part in normal activities. The only activity that was restricted prior to the actual data collection was recreational running with the orthosis in the shoe.
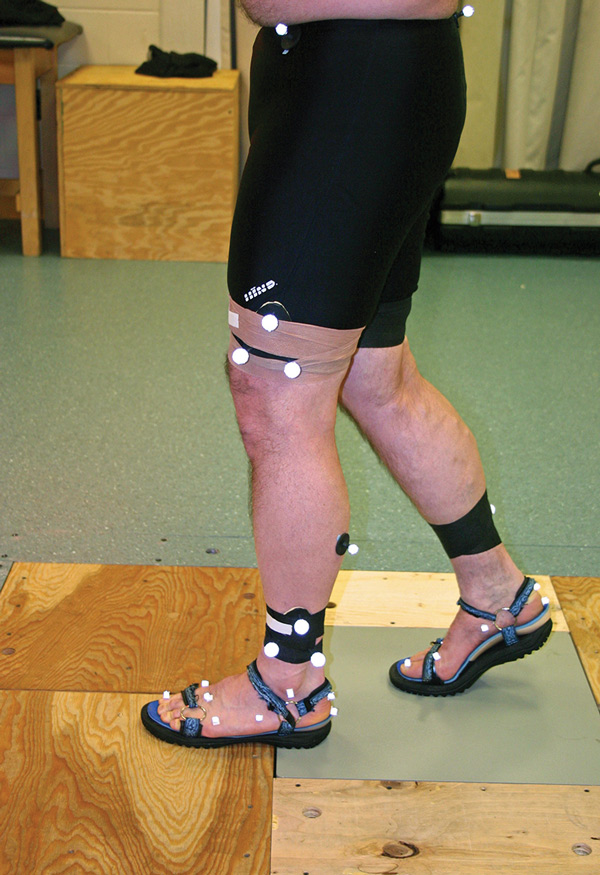
At the end of the accommodation period, all participants attended a data collection session. At this session, retro-reflective markers were placed on the pelvis, lower extremities, and feet over specific bony landmarks (Figure 4). Using an eight-camera video system sampling at a rate of 120 Hz, the 3D displacements of the retro-reflective markers were recorded while the participants walked over level ground at a self-selected walking speed under one of two footwear conditions. The footwear conditions consisted of walking in a sandal and walking in a sandal with the orthosis, which was secured to the sandal with two-sided tape. A modified Teva sandal was used for the walking trials (Figure 5). To allow for full visibility of the foot markers, the sandals were modified by removing the straps (with the exception of the anchoring straps) and replacing them with half-inch Velcro straps.
A walking trial consisted of the participant walking continuously at a self-selected walking speed within the laboratory setting, making wide-angle turns at each end of the room. Twelve trials of video data were collected for each participant (six trials in each footwear condition). Each individual walked in the sandal-only condition first, followed by walking in the sandal with orthosis.
Data analysis
We used marker displacement data to obtain the 3D angular displacements of the rearfoot, forefoot, and first ray, as well as the dynamic arch index, during the walking trials. We defined dynamic arch index as the vertical distance to the navicular marker from the floor, divided by the distance from the inferior calcaneal to the first metatarsal marker. The stance phase of the walking trials was extracted and time normalized to 100 frames (1 and 100 representing heel strike and toe off, respectively). We obtained maximum, minimum, and range (maximum minus minimum) of the rearfoot, forefoot, and first ray angles and dynamic arch index of five stance phases for each footwear condition.
To determine the effect of condition (orthosis vs no orthosis) we analyzed six dependent variables simultaneously: forefoot kinematic movement in the sagittal, frontal, and transverse planes; first ray kinematic movement in the sagittal and transverse planes; and kinematic movement of the medial longitudinal arch (arch index). The level of statistical significance was set at p<.10.
Results
We found a significant difference between conditions for maximum forefoot movement in the transverse plane, for both left and right feet. There was also a significant difference between conditions for minimum forefoot movement in the transverse plane for right feet. However, we found no range-of-motion differences between conditions for any of the other dependent variables, including the arch index, in either lower extremity.
Discussion
The orthosis used in this study is typically prescribed for patients with symptoms associated with flexible flat feet and abnormal pronation. The manufacturer states that the orthosis attempts to control the subtalar joint indirectly by controlling the amount of medial longitudinal arch deformation through direct and total contact of the arch.23 This is based on the theory that a direct relationship exists between arch height and subtalar pronation; therefore, if arch height is controlled, pronation is also effectively controlled.
An additional claim of the manufacturer is that the orthosis will hypothetically increase first metatarsal plantar flexion by directing a mechanical control over the tarsus of the foot, theoretically creating an indirect force on the calcaneus and talus.23 The purpose of this is to increase first metatarsophalangeal (MTP) joint dorsiflexion in an effort to create a more rigid lever through the stance phase of the gait cycle.23 The results of this study do not show significant differences in the maximum and minimum positions of the first ray with the use of the orthosis and do not support this claim. The lack of an effect on first ray motion agrees with the results of Nawoczenski and Ludewig,24 who also failed to identify any significant change in movement of the first ray during the weightbearing phase of the gait cycle with orthosis use.
During normal walking, first metatarsal plantar flexion is needed to allow unrestricted first MTP joint dorsiflexion during the push-off phase of gait. Nawoczenski and Ludewig compared a forefoot posted orthosis with a maximal arch supination stabilization orthosis and assessed the ability of each to alter motion at the first metatarsal and hallux.24 Neither orthotic design was associated with significant effects on first MTP joint dorsiflexion, either at midstance or at push-off. Individual participant responses to the maximal arch supination stabilization orthosis revealed that 83% of the participants experienced no change in first MTP joint dorsiflexion; the remaining participants were split between having increased dorsiflexion and decreased dorsiflexion of the first MTP joint.24
The maximal arch supination stabilization orthosis is calibrated to deliver a range of forces that overlap the range of downward forces exerted on the device by the human body.25 The orthosis, which is fabricated from thermoplastic, applies a corrective force to the plantar surface of the foot. Depending on the relative flexibility of the orthosis, there will be a certain amount of movement observed in the transverse plane of the forefoot, a finding we saw in our study.
Anecdotally, all but one participant in our study continued to wear the orthoses after the study’s completion, and six of the 10 participants reported either a decrease or complete resolution of their symptoms after several weeks of orthosis use. These phenomena may be attributed to the proprioceptive change the orthosis provides within the shoe.
The major limitation associated with this study was the use of a sandal instead of a shoe for the data collection. The heel counter and upper of a shoe have the ability to improve the fit of the orthosis, prevent movement of the orthosis with respect to the plantar surface of the foot, and potentially enhance the overall effectiveness of the orthosis.
Conclusions
This experiment examined the effectiveness of a clinically recommended orthosis on the joint kinematics of flexible flat feet during normal self-paced overland walking. Although the orthosis did not have an effect on most of the joint kinematics of the forefoot, medial longitudinal arch, and first ray, it did have a significant and consistent effect on transverse movement at the forefoot.
Bruce Elliott, PT, DPT, COMT, is an assistant professor in the School of Physical Therapy at MCPHS University in Worcester, MA. Juan Garbalosa, PhD, PT, is a clinical professor of physical therapy and the director of the Motion Analysis Laboratory at Quinnipiac University in Hamden, CT.
- Christensen K. Foot biomechanics during weightbearing. Dynamic Chiropractic 1999;17(5):1-5.
- Cornwall MW, McPoil TG. Relative movement of the navicular bone during normal walking. Foot Ankle Int 1999;20(8):507-512.
- Hunt AE, Smith RM. Mechanics and control of the flat versus normal foot during the stance phase of walking. Clin Biomech 2004;19(4):391-397.
- Reed L, Bennett PJ. Changes in foot function with the use of Root and Blake orthoses. J Am Podiatr Med Assoc 2001;91(4):184-193.
- Reischl SF, Powers CM, Rao S, Perry J. Relationship between foot pronation and rotation of the tibia and femur during walking. Foot Ankle Int 1999;20(8):513-520.
- Donatelli R. The Biomechanics of the Foot and Ankle. Philadelphia, PA: F.A. Davis Company; 1990.
- Eng JJ, Pierrynowski MR. The effect of soft foot orthotics on three-dimensional lower limb kinematics during walking and running. Phys Ther 1994;74(9):836-844.
- Kaufman KR, Brodine SK, Shaffer RA, et al. The effect of foot structure and range of motion on musculoskeletal overuse injuries. Am J Sports Med 1999;27(5):585-593.
- Ferber R, Davis IM, Williams DS 3rd. Effect of foot orthotics on rearfoot and tibia joint coupling patterns and variability. J Biomech 2005;38(3):477-483.
- Heiderscheit B, Hamill J, Tiberio D. A biomechanical perspective: do foot orthoses work? Br J Sports Med 2001;35(1):4-5.
- McPoil TG, Cornwall MW. Footwear and foot orthotic effectiveness research: a new approach. J Orthop Sports Phys Ther 1995;21(6):337-344.
- Branthwaite HR, Payton CJ, Chockalingam N. The effect of simple insoles on three dimensional foot motion during normal walking. Clin Biomech 2004;19(9):972-977.
- Genova JM, Gross MT. Effect of foot orthotics on calcaneal eversion during standing and treadmill walking for subjects with abnormal pronation. J Orthop Sports Phys Ther 2000;30(11):664-675.
- Razeghi M, Batt ME. Biomechanical analysis of the effect of orthotic shoe inserts: a review of the literature. Sports Med 2000;29(6):425-438.
- Moraros J, Hodge W. Orthotic survey: preliminary results. J Am Podiatr Med Assoc 1993;83(3):139-148.
- Donatelli R, Hurlbert C, Conway D. Biomechanical foot orthotics: a retrospective study. J Orthop Sports Phys Ther 1988;10(6):205-212.
- Nigg BM. Experimental techniques used in running shoe research. In: Nigg BM, ed. Biomechanics of Running Shoes. Champaign, IL: Human Kinetics; 1986:27-61.
- Bleck E, Berzins U. Conservative management of pes valgus with plantarflexed talus. Clin Orthop Relat Res 1977;(122):85-94.
- Bordelon R, Lusskin R. Correction of hypermobile flatfoot in children by molded insert. Foot Ankle 1980;1(3):143-150.
- Penneau K, Lutter L, Winter R. Pes planus radiographic changes with foot orthoses and shoes. Foot Ankle 1982;2(5):299-303.
- Wenger DR, Mauldin D, Speck G, et al. Corrective shoes and inserts as treatment for flexible flat foot in infants and children. J Bone Joint Surg Am 1989;71(6);800-810.
- Ball K, Afheldt M. Evolution of foot orthotics—part I: coherent theory or coherent practice? J Manipulative Physiological Ther 2002;25(2):116-124.
- Glaser E, Bursch D, Currie S. Theory, practice combine for custom orthotics. Biomech 2006;13(9):33-43.
- Nawoczenski DA, Ludewig PM. The effect of forefoot and arch posting orthotic designs on first metatarsophalangeal joint kinematics during gait. J Orthop Sports Phys Ther 2004;34(6):317-327.
- Glaser E, Phillips R. Point-counterpoint: high medial arched orthoses: new innovation or older technology? Podiatry Today 2011;24(5).











