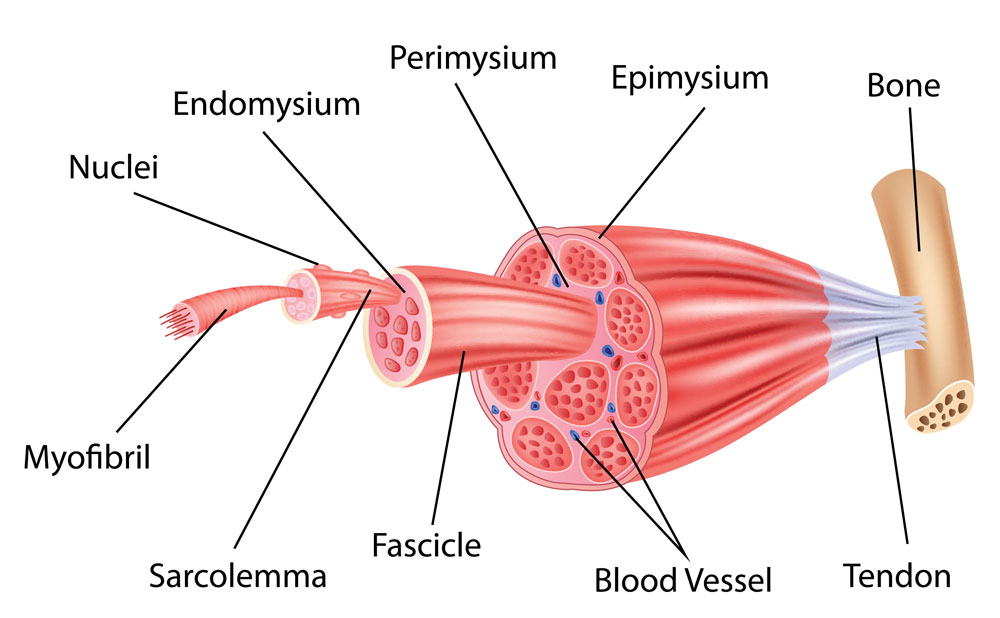
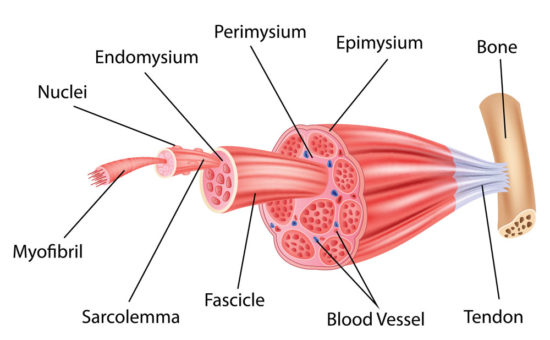
These authors tap unusual but useful historic data sets to enlighten the search for the mechanisms that cause exercise-associated muscle cramps.
By Ronald J. Maughan and Susan M. Shirreffs
Few athletes escape the painful experience of muscle cramps. Cramps that occur during or soon after a bout of physical activity have been termed exercise-associated muscle cramps (EAMC), and these are commonly experienced as a “painful, spasmodic contraction of the skeletal muscle that occurs during or immediately after muscular exercise.”
This review is based in part on a review of the literature using the Web of Science database and the key words ‘cramp’, ‘muscle’ and ‘exercise’. Titles and abstracts of the 379 results returned were screened for relevance. The same search on PubMed returned 236 items. Earlier publications were identified from various sources.
Several surveys have attempted to identify the prevalence of EAMC in different sports populations, but comparing results across studies is hampered by different definitions and different measurement periods, and also by the use of different assessment tools. Nonetheless, EAMC has been reported to affect 67% of triathletes during or after training or racing, 18–70% of marathoners or endurance cyclists, and 30–53% of American football players. Although seemingly suggesting that cramp is common, these data are a mixture of incidence rates in single events and lifetime incidence. Most often, cramping is a relatively minor inconvenience: Schwabe et al. reported the incidence of serious muscle cramping to be less than one per thousand runners in a large cohort (65,865 runners) of participants in half-marathon and ultra-marathon events. To put these data in perspective, Abdulla et al. reported that among an outpatient sample aged 65 years or older, 50% of outpatients experienced frequent muscle cramps, and that another survey of a similar population reported a similar prevalence of 56%, with half having cramps occurring at least once per week. About 7–12% of patients with amyotrophic lateral sclerosis (ALS), a progressive, fatal neurodegenerative disorder, present with muscle cramping.
Key Points
- Exercise-associated muscle cramp (EAMC) is a temporary but intense and painful involuntary contraction of skeletal muscle occurring during or soon after a period of physical activity.
- EAMC is highly unpredictable and it seems likely that different mechanisms may operate in different scenarios.
- Proposed mechanisms include disturbances of water and electrolyte balance, and abnormal spinal reflex activity.
- No prevention strategy or treatment is consistently effective.
The statistics on EAMC from athlete populations do not reveal the fact that for some of those afflicted, it may be a rare occurrence—perhaps only one or two incidents over the course of a whole career, and therefore mostly of negligible impact—while others may be affected much more frequently and much more severely. The intensity and duration of cramps can vary greatly, from a minor spasm that resolves spontaneously within a few seconds, to the whole-body ‘lock up’ lasting several minutes that some athletes describe. In severe cases, the muscle pain may persist for hours or even days after the acute contraction has resolved, and may result in an inability to train or compete. At worst, repeated episodes can result in a premature end to an athlete’s career.
There are many different potential causes of muscle cramps, most of which are not associated with exercise but with a range of clinical conditions or the use of drugs for the treatment of those conditions. Even within the narrow area of EAMC, the highly localized cramp in the calf that afflicts the football (soccer) player late in the game is very different from the whole-body cramps that some American football players and tennis players describe and that have been reported in some industrial settings. These in turn are different from the cramp that afflicts small muscles used in repetitive exercise, such as the hand in writers or typists. Cramps typically occur spontaneously and may or may not occur predictably. Some cramps are associated with fasciculations or other prodromal symptoms, but there may be no warning in other cases. Cramp in some small muscles can be induced in the laboratory, but not all cramps can be induced reliably and not all individuals are susceptible, making cramps difficult to study. Likewise, some cramps occur early on during exercise, while some occur only after prolonged periods of exercise; others still occur some minutes or even many hours after exercise. It is not clear that the mechanisms underpinning these different types of cramp are the same.
This uncertainty is reflected in the conclusion of several recent reviews that the causes of EAMC, and therefore the treatment options, remain uncertain. Two main hypotheses have been proposed and continue to be debated: a disturbance of water and salt balance, and a neurological cause resulting in sustained abnormal discharge of motor drive to the afflicted muscles. Each of these has some support, but neither can fully explain the nature of EAMC.
Risk Factors for Exercise‑Associated Muscle Cramp (EAMC)
Although EAMC has been observed in both training and competition in almost every type of sport, it does seem to be more associated with endurance-type activities and in team sports. A 2006 analysis by Cooper et al. of cramp among American football players showed that the great majority (95%) occurred during periods of hot weather: EAMC occurred most often during the first 3 weeks of practice, when fitness and acclimation levels are likely to be lowest and when the training load is often the highest. The incidence of heat cramps was 37% during the first week of the training camp, then 27%, 18% and 4% in the succeeding weeks. The incidence of EAMC may also be high in endurance events taking place in cool or cold environments: Maughan found that 15 of 92 (18%) runners experienced cramp during a single marathon race taking place at 10–12 °C. Most cases occurred in the later stages of the race, after an average of 35 km had been completed: no cases were reported to have occurred before 24 km, and 5 of the 15 instances occurred during the last 1.5 km.
Schwellnus and colleagues have suggested that EAMC in marathon runners is associated with high intensity, long duration, and hilly terrain, which can lead to ‘premature muscle fatigue’ in competitors with a history of cramping. It is not immediately obvious what is meant by ’premature’ fatigue and how this might differ from the fatigue that is an inevitable consequence of participation in such events. Schwellnus et al. reported that, in a prospective cohort study in 210 Ironman triathletes, independent risk factors for EAMC were a history of the condition and competing at a higher than usual exercise intensity, but that dehydration and serum sodium changes did not predict EAMC. Other risk factors included older age, a longer history of running, higher body mass index (BMI), shorter daily stretching time, irregular stretching habits, and a positive family history of cramping.
In a more recent analysis of cross-sectional data from almost 16,000 participants in two races over a distance of 21.1 km and 56 km, Schwellnus et al. identified a number of differences between runners who reported a history of EAMC (n = ~ 3000) and a control group with no such history (n = ~ 13,000). Factors associated with a history of EAMC included underlying chronic disease (including cardiovascular, respiratory, gastrointestinal, nervous system, kidney, bladder and hematological disease), as well as cancer, allergies, regular medication use, and a history of injury. More experienced runners were also at greater risk. Whether some underlying common factors underpin these associations is not clear.
Possible Causes of EAMC
Two main causes for muscle cramps have been proposed. This suggests an either/or dichotomy, and this is how the literature is often presented, though the picture is not at all clear, and the evidence on both sides is weak. It is unlikely that a single mechanism can account for all cramps in all situations, therefore the search for a single causal mechanism is probably futile. It follows from this that strategies for the prevention and treatment of the condition are also unlikely to be one-dimensional. However, whatever the primary cause, it is clear that cramp is accompanied by active contraction of the afflicted muscle, as evidenced by high levels of muscle electrical activity.
Disturbances of Hydration and Electrolyte Balance
The role of changes in hydration status and electrolyte balance as a factor in the etiology of EAMC was dismissed by Schwellnus, who said that “Scientific evidence in support of the ‘electrolyte depletion’ and ‘dehydration’ hypotheses for the etiology of EAMC comes mainly from anecdotal clinical observations, case series totalling 18 cases, and one small (n =10) case–control study.” This assessment has been repeated in many subsequent publications: there may however be more evidence.
The strongest evidence that sweat-related electrolyte imbalances are a factor in some muscle cramps is found in the large-scale observational and prospective studies of industrial workers—mainly studies on miners, ship’s stokers, construction workers and steel mill workers that were conducted in the 1920s and 1930s—where administration of saline drinks or salt tablets was able to greatly reduce the incidence of cramps. These studies were inevitably limited by the methods available at the time, but they did have the advantage of access to large populations and the keeping of careful medical records related to productivity. It is easy to dismiss much of the older literature, but some of the observations were extensive and meticulous.
Although methodologies were limited, some of the observations were acute and sometimes remarkably prescient. For example, in 1923 Moss documented cases of cramp among coal miners, attributing the onset of cramps, which in some cases were debilitating, to (1) high air temperatures; (2) excessive drinking of water caused by dryness of the mouth and throat; and (3) continued hard work. He also observed that cramps tended to occur during the second half of a working shift and in men who were less physically fit, thus implicating not only sweat losses but also fatigue in the etiology. It should be noted that cramp was not attributed to dehydration or increased serum electrolyte concentrations, but rather “to a form of water poisoning of the muscles brought about by the combination of great loss of chloride by sweating, excessive drinking of water, and temporary paralysis of renal excretion.” Chloride was normally measured in body fluids as there was no good assay for sodium at the time, but there is a close relationship between sodium and chloride concentration in sweat. This does not implicate dehydration, but rather inappropriate, and perhaps excessive, intake of plain water in combination with large losses of electrolytes in sweat.
[Furthermore,] in 1936 Dill et al. reported the findings of intervention studies carried out at the site of construction of the Hoover Dam and in the steel mills of Youngstown, Ohio. At both locations, large numbers of men undertook hard physical work in extremely hot environments on a daily basis. They found that those suffering from cramp displayed the following characteristics: (1) dehydration; (2) lowered concentration of sodium and chloride in blood plasma; (3) little or no sodium or chloride in urine; (4) increased serum protein concentration; (5) increased red cell count; and (6) normal osmotic pressure.
This presents a complex picture: some of these findings are typical of dehydration (1, 4 and 5), while others are consistent with overhydration (2, 3). However, they also reported that injection of isotonic saline normalized the blood profile and brought immediate relief from the symptoms. In the largest intervention study, reported in the same paper, they added saline to the water given to the 12,000 men employed in one of the mills, while those at neighboring mills continued to be provided with plain water; this was effective in almost completely abolishing cases of muscle cramp, [whereas] in previous years, and at other mills in the same year where plain water was given, up to 12 cases of cramp required hospitalization in a single day.
In a controlled environment, severe restriction of dietary sodium intake can result in hyponatremia and may be associated with generalized skeletal muscle cramping in the absence of exercise. Some more recent studies have assessed changes in hydration status and plasma electrolyte concentrations in athletes who have experienced muscle cramps, including marathon runners, participants in a 56 km road race, competitors in an Ironman triathlon, and participants in a 161 km ultramarathon. None of these showed any association between cramp and serum electrolyte changes, but it is important to note that serum electrolyte concentrations may be of little relevance. Local intracellular and extracellular electrolyte concentrations may be relevant as they will affect the resting membrane potential of both muscle and nerve, but it is unlikely that changes in plasma concentrations can track these changes; there is good evidence that changes in the plasma concentration of these electrolytes do not reflect local intramuscular changes during either intense or prolonged exercise.
There is some experimental evidence (small studies, case reports, etc.) that individual athletes who lose large amounts of salt in their sweat may be more prone to muscle cramps. Stofan et al. found that sweat sodium losses during training sessions were larger in cramp-prone football players (n = 5) than in a group of players with no history of EAMC. Subsequently, the same research group investigated a reference group of American football players (n = 8) without a cramping history, and a cramp-prone group (n = 6). Whole blood sodium concentration (plasma sodium concentration) remained unchanged after training in the control group (138.9 ± 1.8 to 139.0 ± 2.0 mmol/L), while it tended to decline (137.8 ± 2.3 to 135.7 ± 4.9 mmol/L) in the cramp-prone players.
In support of a role for disturbances of water and salt balance as a causal factor, Ohno and Nosaka showed that a body fluid deficit of 3% of body mass induced by intermittent sauna exposure without exercise increased the number of subjects who developed EAMC during a muscle cramp test in the toe flexors, but not in the knee extensors. Jung et al. had participants perform a fatiguing protocol in the calf muscles to induce EAMCs. In one trial, subjects consumed a carbohydrate electrolyte drink at a rate similar to sweat rate, while in the other trial, no fluid was consumed and mild (1% loss of body mass) hypohydration developed. Nine participants experienced cramps in the carbohydrate–electrolyte trial, compared with seven in the hypohydration trial. Of the seven individuals who had EAMC in both trials, time to onset was more than doubled in the carbohydrate–electrolyte trial (36.8 ± 17.3 min) compared with the hypohydration trial (14.6 ± 5.0 min). Subjects who experienced cramps sweated more (2.0 ± 0.9 L/min) than those who did not (1.3 ± 0.6 L/ min).
Although numerous papers have disputed the findings above, two recent publications seem likely to reopen the debate on the role of disturbances of water and salt balance in the development of EAMC. Ohno et al. systematically investigated the susceptibility of voluntarily-induced EAMC in hamstrings after hypohydration of 1, 2, and 3% of body mass induced by sauna exposure without exercise. No EAMC occurred in the nine participants in the control condition or after 1% dehydration; three subjects experienced EAMC in the 2% and six in the 3% condition. In the study by Lau et al., 10 men ran downhill in a hot environment until they lost 2% of their initial body mass [46]. Ten minutes after completing the run, they ingested either plain water or a commercially available oral rehydration solution (ORS) containing sodium (50 mEq/L), chloride (50 mEq/L), potassium (20 mEq/L), magnesium sulphate (2 mEq/L), lactate (31 mEq/L) and glucose (18 g/L) in a volume equal to the mass lost. Susceptibility of the calf muscles to electrically-induced cramp was assessed by a threshold frequency (TF) test applied at baseline before running, immediately after running, and 50 and 80 min after drink ingestion. Muscle cramp susceptibility did not change from baseline to immediately after running in either condition, but TF decreased after water intake by 4.3 Hz (at 30 min) and 5.1 Hz (at 60 min post-run), but increased after ORS intake by 3.7 and 5.4 Hz, respectively. The investigators reported that serum sodium and chloride concentrations decreased after water intake but were maintained after ingestion of the electrolyte-containing drink.
In accord with the mechanisms proposed by Moss and others in the 1920s, these results suggest that the combination of sweat loss and water intake makes muscles more susceptible to electrical simulation-induced muscle cramp, but the susceptibility to muscle cramp decreases when a drink with a high electrolyte content is ingested. It is interesting to note that cramping is a recognized accompaniment of hyponatremia (defined as a serum sodium concentration < 135 mmol/L) in clinical settings. However, literature on exercise-associated hyponatremia generally makes no mention of muscle cramping.
While cramp is often associated with large sweat losses during prolonged exercise in the heat, it also occurs in cool environments with little or no sweat loss, suggesting that sweat loss alone and the consequent disturbances of electrolyte balance cannot account for all cramps.
Part 2 of this article, which will appear in our February issue, will cover altered neuromuscular control and possible prevention and treatment strategies.
This article has been excerpted from “Muscle Cramping During Exercise: Causes, Solutions, and Questions Remaining,” by the same authors, which was published online November 6, 2019 in the journal Sports Medicine. Sports Medicine. doi.org/10.1007/s40279-019-01162-1. Editing has occurred, including breaking the article into 2 parts, and references have been removed for additional brevity. Part 2 will appear in our February 2020 issue. Use is per the Creative Commons Distribution 4.0 International License. Readers are encouraged to read the full article at https://link.springer.com/article/10.1007/s40279-019-01162-1