 By Windy Cole, DPM, CWSP
By Windy Cole, DPM, CWSP
Millions of Americans are afflicted with painful, open, draining ulcers on their lower extremities. Venous leg ulcers (VLUs) cause significant clinical and economic burden to the healthcare system and society.1,2 It is not uncommon for clinicians to see patients who have suffered for years with VLUs.
The Problem
VLUs are the result of chronic venous insufficiency. This malady is caused by an abnormality of the veins in the lower extremity. The lower extremity venous system is composed of both a superficial and deep system connected by an elaborate series of perforating veins (Figure).2,3 Under normal conditions, valves within these veins direct blood from the superficial into the deep system, which in turn carries the blood back toward the heart. The flow in the deep system is directly impacted by the pumping action of the musculature in the legs during physical activity. A host of illnesses and disease states can directly affect the anatomic function of the venous system. Deep vein thrombosis, for example, damages the valves in the veins of the deep and superficial systems. Pregnancy increases the risk of chronic venous insufficiency and VLUs: functional and structural changes occur in the venous system secondary to elevated hormone levels and damage caused by elevated pressure on the inferior vena cava by the enlarging fetus.4 In addition, there is a hereditary predisposition toward valvular dysfunction eventually leading to the development of VLU. Obesity and sedentary lifestyle can also contribute to the development of venous insufficiency.
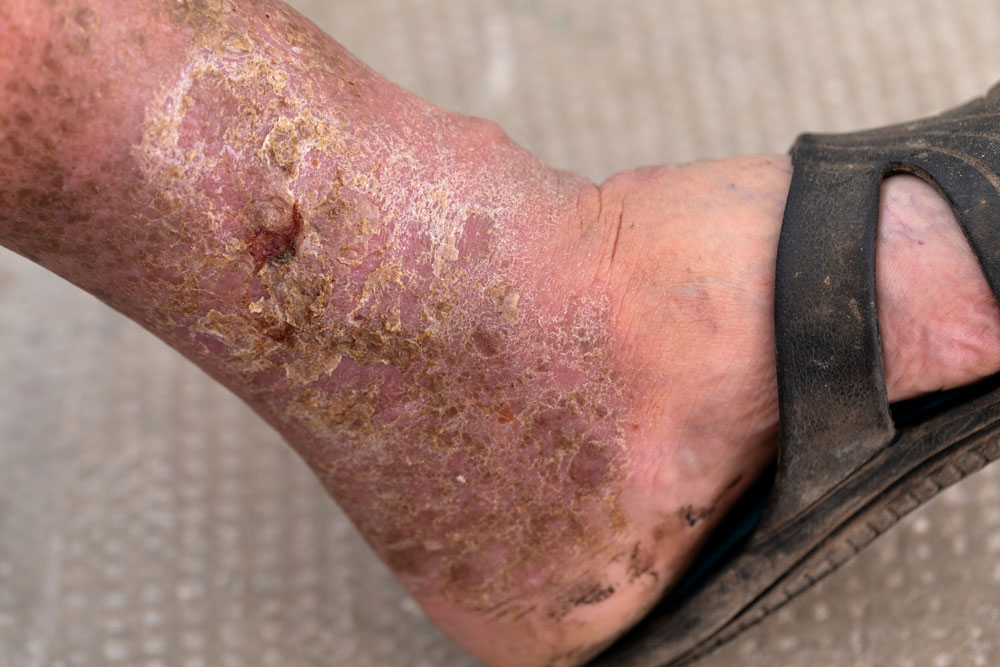
The common etiology of venous insufficiency is the reversal of blood flow from the deep to the superficial venous system.2,3 This reversal of flow leads to pooling of the blood and fluid in the legs. The patient may first experience swelling or edema in the lower extremities as a first sign of disease. Over time, hallmark trophic changes in the tissues appear: hyper-pigmentation, venous stasis dermatitis, hemosiderin deposits, loss of hair, thickened nails, atrophy blanch, and lipodermatosclerosis. As a result of these changes, skin breakdown can occur resulting in ulceration. Finally, VLUs typically occur in the medial gaiter region of the lower leg. This corresponds to the position of the perforating veins connecting the superficial and deep systems.
The Pathophysiology
Several competing theories aim to describe the progression from chronic venous hypertension to skin breakdown and ulceration. A popular hypothesis is that hypertension in the venous system leads to the development of a pericapillary fibrin cuff that forms a barrier to oxygen diffusion. The skin and subcutaneous tissue become hypoxic and subsequently ulcerate.5,6 Another theory suggests that white cells plug the capillaries causing tissue hypoxia.6 Many older theories all share a final common pathway: tissue ischemia. A more recent theory of ulcer pathogenesis suggests that increased inflammation brought on by a cycle of chronic ischemia-reperfusion leads to skin breakdown.6 Neutrophils, activated by repeated ischemia-reperfusion release oxygen-derived free radicals (ROS). The ROS stimulate the formation of capillary cuffs that impair oxygenation and trap more neutrophils creating a vicious cycle of inflammation. The repeated activation of this cascade eventually overwhelms the body’s compensatory capacity and the balance tips in the favor of tissue destruction.7 In many cases, the immediate cause of the ulceration is a traumatic event; however, healing is disrupted by one or a combination of factors described above.7 Correction of the underlying venous hypertension is the crux of treatment for VLUs.

Figure. Relationship between the fascia and veins of the lower extremity.The fascia covers the muscle and separates the deep from the superficial compartment. Superficial veins (a) drain the subpapillary and reticular venous plexuses and they are connected to deep veins through perforating veins (b). The saphenous fascia invests the saphenous vein. The saphenous compartment is a subcompartment of the superficial compartment. Reprinted from Meissner MH et al. The hemodynamics and diagnosis of venous disease. J Vasc Surg. 2007;46(6 Suppl):S4-S24 (https://doi.org/10.1016/j.jvs.2007.09.043), with permission from Elsevier. All rights reserved.
Compression Therapy
Compression therapy harnesses the basic principles of physics to reduce lower extremity edema. LaPlace’s law describes the relationship between the application tension and sub-bandage pressure: The greater the tension applied with the bandage the greater the sub-bandage pressure. In addition, sub-bandage pressure is inversely proportional to the radius of the limb. A bandage applied to a thin leg will result in greater pressure. Finally, the greater the number of layers the higher the pressure.8 The practical consequence of LaPlace’s law is that a wrap placed with constant tension to a limb that increases in size from ankle to knee will result in graduated compression: greatest compression at the ankle decreasing as the wrap covers the more proximal limb.9
Multilayer compression bandages contain both inelastic and elastic wraps. This combination allows for use across all patients with VLUs. The elastic component benefits ambulatory patients with poor calf pump function, while the inelastic portions provide higher sub-bandage pressure benefiting all patients. There are many multilayer compression kits on the market. These products vary widely, and it is always wise to review the product insert prior to application.
Treatment guidelines and manufacturers strongly recommend obtaining an objective measure of the patient’s vascular status, such as ankle brachial index, prior to the application of compression. Peripheral arterial disease is a contraindication to compression therapy.10
After successful treatment, transition to maintenance compression therapy reduces the risk of recurrence.10 Most prevention guidelines recommend graduated compression stockings worn daily along with routine elevation of the extremities. The suggested compression levels of 30 to 40 mmHg are recommended for the treatment of chronic venous insufficiency and venous ulcer prevention.10 Patients who cannot don stockings easily may have success with Velcro-closure adjustable devices.
Conclusions
Edema causes an alteration in endothelium that begins a complex cascade of detrimental events. Neutrophils become activated and adhere to capillary walls thus creating ischemia-reperfusion injury releasing free oxygen species.6 The resulting inflammation damages the vasculature and soft tissues.6 As hypoxia ensues, inflammation worsens, and harmful matrix metalloproteinases cause dermal tissue fibrosis and eventual ulceration.6 Compression therapy facilitates the removal of lower extremity edema. White blood cells detach from the endothelium, and inflammation lessens.11 As perfusion improves the tissue environment stabilizes and tissue fibrosis decreases. New devices are entering into the space that have the potential to improve patient outcomes—see box on page 31 for additional information.
Windy Cole, DPM, CWSP, is an adjunct professor and Director of Wound Care Research at Kent State University College of Podiatric Medicine. Dr Cole also serves as the National Director of Professional Development and Clinical Education for Woundtech. She is board certified by the American Board of Foot and Ankle Surgery and the American Board of Wound Management. She has been a dedicated wound care advocate for two decades with interests focused on medical education, diabetic foot care, wound care, limb salvage, and clinical research. Her passion to help others has led her to participate in humanitarian efforts around the world. Dr. Cole has published numerous peer-reviewed and industry articles on these topics and is a sought-after speaker both nationally and internationally. She is a feature writer for Podiatry Management and Today’s Wound Clinic as well as a contributing writer for Podiatry Today. She is an Editorial Board member of Wound Management and Prevention, Podiatry Today, The Foot Journal, and Lower Extremity Review. She is also the Podiatry Section Editor for the ePlasty Journal. She is a wound care advocate on the forefront of wound research and was the 2020 World Union of Wound Healing Silver Medal Award recipient for her work in Technology-driven Research. She sits on the advisory board of multiple emerging biotech companies and has been integral in collaborating on innovative research protocols in the space.
- Ballard JL, Bergan JJ, editors. Chronic venous insufficiency. Diagnosis and treatment. Springer-Verlag: 2000.
- Negus D. Leg ulcers: A practical approach to management. 2nd ed. Butterworth Heinemann: 1995.
- Olivencia JF. Pathophysiology of venous ulcers: surgical implications, review and update. Dermatol Surg. 1999;25(11):880-885.
- Ropacka-Lesiak M, Kasperczak J, Breborowicz GH. Czynniki ryzyka rozwoju niewydolności zylnej kończyn dolnych w ciazy–cześc I [Risk factors for the development of venous insufficiency of the lower limbs during pregnancy–part 1]. Ginekol Pol. 2012;83(12):939-42. Polish.
- Browse NL. Venous ulceration. BMJ. 1983;286:1920-1922.
- Coleridge Smith PD, Thomas P, Scurr JH, Dormandy JA. Causes of venous ulceration: a new hypothesis. BMJ. 1988;296:1726-1727.
- Falanga V. The “trap” hypothesis of the venous ulceration. Lancet. 1993;341:1006-1008.
- Agren MS, Eaglestein WH, Ferguson MW, et al. Causes and effects of the chronic inflammation in venous leg ulcers. Acta Derm Venereol Suppl (Stockh). 2000;210:3-17.
- Bergan JJ, Schmid-Schonbein GW, Coleridge Smith PD, Nicolaides AN, Boisseau MR, Eklof B. Chronic venous disease. New Engl J Med. 2006;355:488-498.
- Compression Therapy Study Group. Compression: consensus document based on scientific evidence and clinical experiences. Edizioni Minerva Medica Torino: 2009.
- Cullum N, Fletcher AW, Nelson EA, Sheldon TA. Compression bandages and stockings in the treatment of venous ulcers. Cochrane Database syst Rev 2000;(3):CD000265. Update in: Cochrane Database Syst Rev. 2001;(2):CD000265.







After months of discomfort, I finally found the best vein center near me that took my symptoms seriously. Their non-invasive treatments and follow-up care made a huge difference. Highly recommend getting checked