By Asim Raja, DPM, FACFAS
Orthobiologics is the science of harnessing and concentrating substances (substrates) that occur naturally in the body. It is theorized that in higher concentrations, biologics may help to enhance (or) improve the healing process.
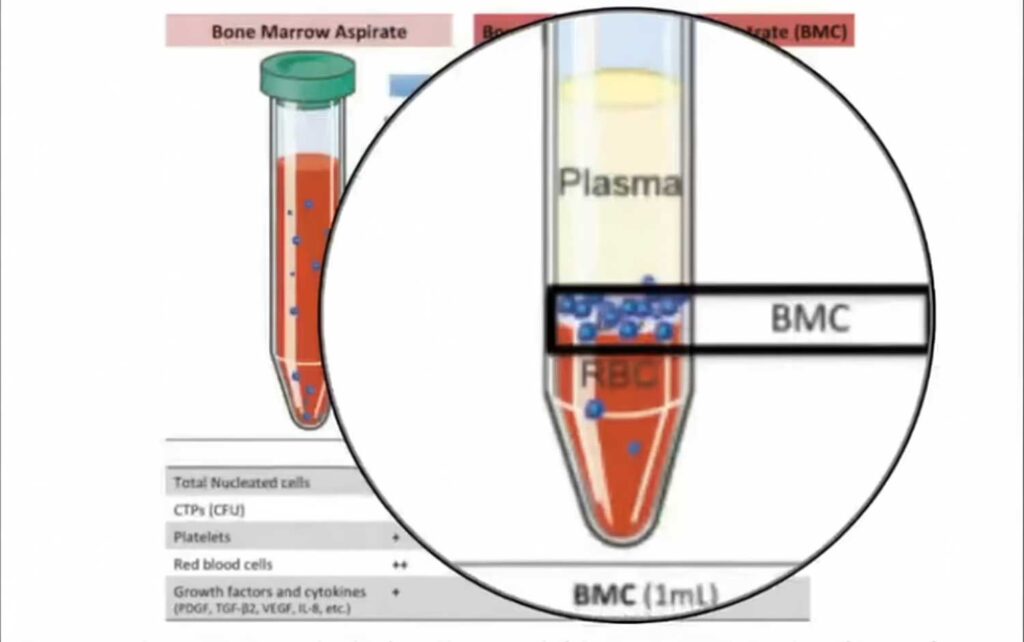
Figure 1. Bone marrow aspirate concentrate (BMC) is obtained by one or multiple bone marrow aspiration (BMA) centrifugations. After centrifugation (density separation), the buffy coat (BC), which lies in between the plasma and the red blood cells (RBC) containing most of the nucleated cells, (some of which are stem and progenitor cells), platelets, growth factors, and cytokines is obtained.
Source: Piuzzi NS, Khlopas A, Newman JM, Ng M, Roche M, Husni ME, Spindler KP, Mont MA, Muschler G. Bone Marrow Cellular Therapies: Novel Therapy for Knee Osteoarthritis. J Knee Surg. 2018 Jan;31(1):22-26.
Orthobiologics and bone substitutes represent groundbreaking advancements in regenerative medicine. They focus on enhancing the body’s natural healing processes by utilizing naturally occurring substrates like cells, scaffolds, and signaling molecules. These elements work together to accelerate recovery from bone fractures and other tissue injuries. The U.S. Food and Drug Administration (FDA) classifies these biologic products as “human cells, tissue, and cellular/tissue-based products” (HCT/P), emphasizing their role in transplantation and repair. By concentrating these biologically active components, orthobiologics offer promising medical solutions for improved bone healing and tissue regeneration.
The Science Behind Biologics
Biologics are transformative in the medical field, offering advanced solutions for bone healing by harnessing the body’s natural substrates. Understanding the scientific foundations and regulatory aspects of biologics is crucial for both practitioners and patients.
FDA Classification and Definition: The FDA classifies biologics under “Human Cells, Tissues, and Cellular/Tissue-Based Products” (HCT/P). This broad category includes any articles containing or consisting of human cells or tissues intended for implantation, transplantation, infusion, or transfer into a human recipient. This classification emphasizes the natural origins of these products and the necessity for regulation in their usage, ensuring they are minimally manipulated and maintain their intended purpose.
The “3 S’s” of Biologics: The concept of biologics is best explained through the 3 key components: Cell, Scaffold, and Signal, often compared to a construction site.
- Cell: These are akin to workers, where immature cells like mesenchymal stem cells can differentiate into specialized bone cells essential for healing.
- Scaffold: Serving as the framework, scaffolds provide the necessary structure for cells to adhere, migrate, and grow, facilitating the healing process.
- Signal: Similar to a foreman, signals direct the activity of cells, guiding them through the healing process.
Types and Sources of Cells in Biologics: Cells utilized in biologics are categorized into undifferentiated cells, like mesenchymal stem cells which have the potential to mature into osteocytes or chondrocytes, and mature cells with defined roles. Bone marrow and adipose tissue are prime sources for these cells, offering accessibility and a high concentration of precursor cells. The process of creating Bone Marrow Aspirate Concentrate (BMAC) involves a centrifuge to concentrate these cells, enhancing their availability for therapeutic applications.
 Scaffolds in Bone Healing
Scaffolds in Bone Healing
Scaffolds are integral to bone healing, providing the physical support necessary for cell integration and tissue regeneration. They come in various forms, each with its own advantages and challenges.
Autogenous bone grafts, harvested from the patient, provide a robust scaffold because of their osteogenic, osteoinductive, and osteoconductive properties. However, they require an additional surgical site and are limited in availability. Alternatively, allografts, sourced from donors, negate donor site morbidity and are readily available, though they pose a risk of disease transmission and potential immune reactions.
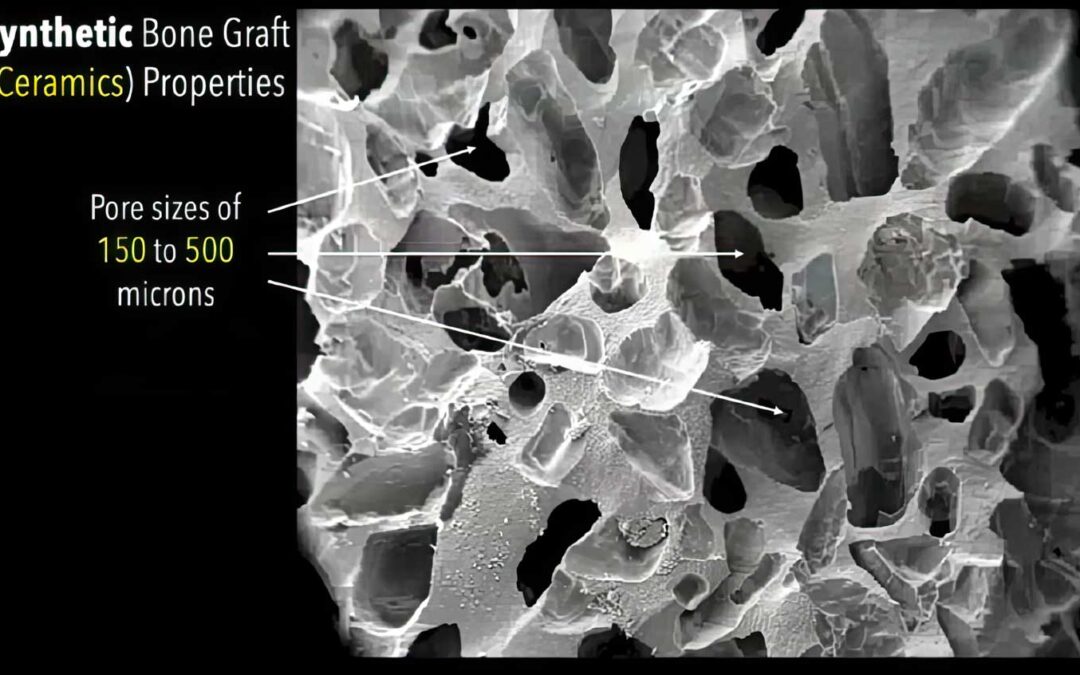
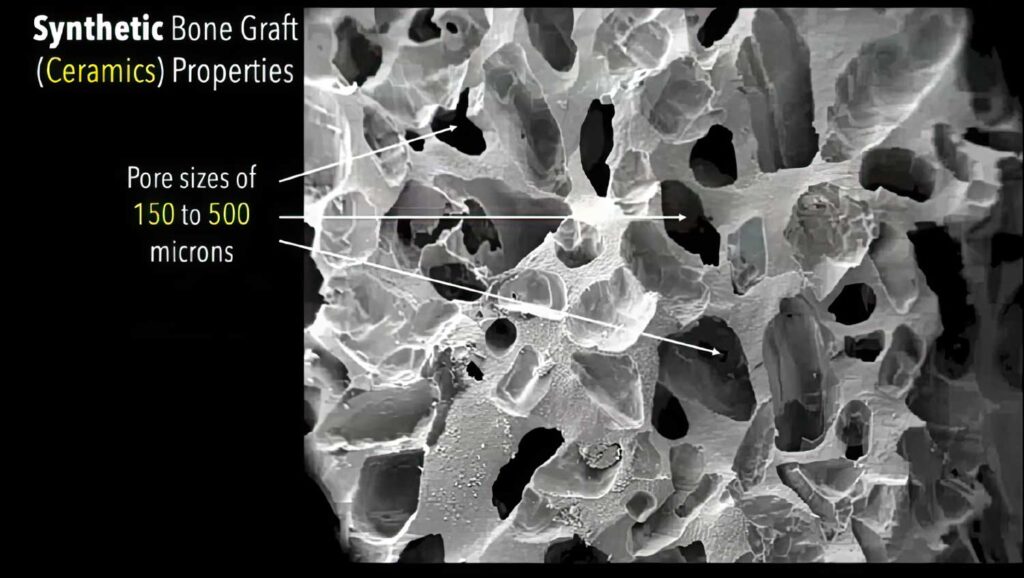
Synthetic bone grafts, such as those made from bioactive glass, calcium sulfate, and tricalcium phosphate (TCP), are engineered to mimic the bone’s natural structure, with bioabsorbables designed to integrate and resorb over time. Metallic implants, often 3D printed using materials like titanium, promote osteointegration and long-term bone integration, although their success depends on factors such as pore size and surface preparation.
Soft tissue scaffolds involve the use of tendon and nerve allografts, typically stripped of cells and signals, serving purely as structural intermediaries to aid in repair and regeneration. Skin substitutes, often in sheet form, support skin growth and are primarily used for treating wounds, providing an essential scaffold in regenerative medicine.
 Signals and Their Roles in Healing
Signals and Their Roles in Healing
Understanding how signals work in biologics is crucial to maximizing their potential in enhancing bone healing and regeneration. Primary signaling agents involved in these processes include:
Cytokines play a significant role in directing the healing process. Produced mainly by leukocytes or white blood cells, they facilitate communication between cells during immune responses and inflammation. Examples include interleukins and interferons, which are pivotal in combating infections and regulating cellular activities.
Growth factors are predominantly released by activated platelets. They are essential for stimulating cell growth, proliferation, and differentiation. For example, Platelet-Derived Growth Factor (PDGF) and Transforming Growth Factor-beta (TGF-beta) are crucial for bone growth and tissue repair. Vascular Endothelial Growth Factor (VEGF) promotes the formation of new blood vessels, enhancing nutrient delivery to healing tissues.
Platelet-Rich Plasma (PRP) formulations have become a cornerstone in augmenting healing in both orthopedic and podiatric applications. PRP is derived by centrifuging a patient’s blood to concentrate platelets and growth factors. This results in various formulations, including leukocyte-rich PRP, which is beneficial for tendon healing due to its inflammatory response, and platelet-pure plasma, preferred for joint injections to minimize inflammation.
Demineralized Bone Matrix (DBM) is rich in proteins, particularly Bone Morphogenetic Proteins (BMPs), such as BMP-2 and BMP-7, known for their ability to induce bone formation. BMPs are osteoinductive, meaning they signal immature cells to develop into bone-forming cells, facilitating the repair and regeneration of bone material.
Regulatory and Practical Considerations
Navigating the regulatory landscape is essential for practitioners using orthobiologics and bone substitutes to ensure compliance and optimal patient outcomes.
The FDA classifies biologics as Human Cells, Tissues, and Cellular/Tissue-Based Products (HCT/P). However, there are notable regulatory gaps, as the FDA does not mandate verification of cell concentrations or the homogeneity of biologic products. This oversight can lead to significant variability in product efficacy and consistency.
Marketing Restrictions: The FDA imposes restrictions on marketing claims for biologics, particularly those promising “regenerative” outcomes. Additionally, they restrict the approved sources for adult stem cells to bone marrow or adipose tissue, ensuring careful consideration of product claims and sourcing.
Practical Applications in Podiatry and Orthopedic Surgery
In clinical practice, understanding the nuances of product claims and the regulatory landscape helps practitioners make informed decisions. For instance, PRP formulations can be tailored to specific injuries or conditions, such as using leukocyte-rich formulations for tendons or platelet-pure formulations for joint environments. In podiatry and orthopedic surgery, orthobiologics serve as adjunctive tools, enhancing natural healing processes when applied within a well-considered treatment plan.
For successful applications, practitioners should focus on optimizing the patient’s overall biological health, creating favorable conditions for orthobiologics to exert their maximal therapeutic effect. This holistic approach ensures improved healing outcomes and patient satisfaction.
Conclusion
In summary, orthobiologics and bone substitutes represent pioneering advancements in regenerative medicine, offering promising avenues for enhanced bone healing. By leveraging the body’s natural substrates and processes, biologics such as cells, scaffolds, and signals work in concert to support the repair and regeneration of damaged tissues. However, these innovations are largely adjunctive, meaning they serve to complement existing healing processes rather than replace them outright. Success in using these medical solutions is highly contingent upon optimizing the patient’s biological environment, addressing any underlying health issues, and selecting the right combination of biologic components. As scientific research and technological advancements continue to unfold, the potential uses for these biologic products are expected to expand, providing more targeted and effective treatment options for bone-related medical conditions.
Asim Raja, DPM, FACFAS, is Service Chief of Podiatric Surgery in the Department of Surgery at the Fayetteville Veterans’ Administration Medical Center in Fayetteville, NC.
This article is a summary of Dr. Raja’s presentation, “Orthobiologics and Bone Substitutes,” from the 35th Annual No-Nonsense Seminar, held March 7-9, 2025. To view the full presentation with questions and answers—and see the agenda for the 3-day program, visit visit https://nononsense2025.lerexpo.vcom. Continuing education credits are available for this and many other lerEXPO programs.