 By Mathias B. Forrester, BS
By Mathias B. Forrester, BS
Background: A portion of people use or carry cell phones while using bicycles and other non-motor vehicles (eg, scooters, skateboards, skates). This can increase the risk of injury. This study described cell phone-related lower extremity injuries while using non-motor vehicles that were treated at United States (US) hospital emergency departments (EDs).
Methods: Cell phone-related lower extremity injuries while using non-motor vehicles reported to the National Electronic Injury Surveillance System during 2000-2023 were examined. The NEISS collects data on product- and activity-related injuries treated at a representative sample of 100 US hospital EDs. These records can be used to calculate national injury estimates.
Results: An estimated 1,261 cell phone-related lower extremity injuries while using non-motor vehicles were treated at US hospital EDs during 2000-2023, representing 14.8% of the estimated 8,536 such injuries affecting all body parts. The type of non-motor vehicle was 90.0% bicycle, 8.8% skateboard, and 1.3% roller skates. The affected body part was 49.1% knee, 17.6% lower leg, 12.4% ankle, 13.9% upper leg, 6.9% toe, and 0.0% foot. The most severe diagnoses were 33.0% contusion or abrasion, 26.5% strain or sprain, 16.7% fracture, 8.9% laceration, and 14.9% other or not stated. The patient disposition was 90.6% treated or evaluated and released from the ED, 4.9% treated and admitted for hospitalization (within same facility), and 4.5% left without being seen or against medical advice.
Conclusion: Relatively few cell phone-related injuries while using non-motor vehicles, particularly involving the lower extremity, were reported to US hospital EDs during the 24-year period. Most of these injuries involved bicycles. Almost half of the severe diagnoses involved the knee. The most common severe diagnoses were contusion or abrasion followed by strain or sprain. Most patients were treated or evaluated and released from the ED. The information in this study may be useful for education and prevention efforts in the future.
Cell phones are ubiquitous in the United States (US), with 98% of adults reporting ownership of a cell (mobile) phone in 2023.1 With so many people using such devices, cell phone-related injuries are likely to occur. Much of the literature has focused on injuries that occur while being distracted by cell phones while driving or while walking.2-7
 However, cell phone-related injuries also may occur when riding a bicycle or using other non-motor vehicles (eg, bicycles, scooters, skateboards, skates). Studies in China and the Netherlands reported 3-5% of bicyclists used cell phones while cycling.8-10 A study in Boston, Massachusetts, found that 13.5% of bicyclists observed at selected intersections in the city had visual/tactile distractions (object/cell phone in hand or on handlebars) at the time.11 Bicyclists who use a cell phone exhibit more unsafe behaviors than those bicyclists who are not performing a secondary task.12 A study in China observed an increased risk of traffic injury among bicyclists who had used a cell phone within 1 minute of the injury.13
However, cell phone-related injuries also may occur when riding a bicycle or using other non-motor vehicles (eg, bicycles, scooters, skateboards, skates). Studies in China and the Netherlands reported 3-5% of bicyclists used cell phones while cycling.8-10 A study in Boston, Massachusetts, found that 13.5% of bicyclists observed at selected intersections in the city had visual/tactile distractions (object/cell phone in hand or on handlebars) at the time.11 Bicyclists who use a cell phone exhibit more unsafe behaviors than those bicyclists who are not performing a secondary task.12 A study in China observed an increased risk of traffic injury among bicyclists who had used a cell phone within 1 minute of the injury.13
The objective of this study was to characterize cell phone-related lower extremity injuries while using a non-motor vehicle managed at US hospital emergency departments (EDs).
Methods
The data source for this retrospective epidemiologic study was the National Electronic Injury Surveillance System (NEISS) database at https://www.cpsc.gov/cgibin/NEISSQuery/home.aspx. Details of the NEISS database have previously been described in Lower Extremity Review.14 In brief, operated by the US Consumer Product Safety Commission (CPSC), NEISS collects data on consumer product- and activity-related injuries from a probabilistic sample of the EDs of approximately 100 US hospitals. National estimates are calculated from database records according to the sample weight assigned to each case based on the inverse probability of the hospital being selected for the NEISS sample.15,16 Since the data are publicly available and de-identified, the study is exempt from institutional review board approval. Previously published studies used NEISS data to examine cell phone-related injuries.17-23 While, none of these studies focused on injuries while using non-motor vehicles, several studies did focus on lower extremity injuries.17,18
Cases were cell phone-related injuries while using non-motor vehicles reported to NEISS during 2000-2023. The NEISS database contains three numeric fields for coding the product or activity involved in the injury (Product_1, Product_2, Product_3). (Product_3 was added to the NEISS database in 2018 but does not appear to have been used until 2019.)16 The NEISS database includes product code 550 (telephones or telephone accessories), but this code is used not only for cell phones but also for landline phones, intercoms, and other such devices. Consequently, product code 550 alone cannot be used to identify cell phone-related injuries. For this analysis, first, all records with product code 550 in any of the three product code fields or “phone” in the Narrative text field (a text field that summarizes the circumstances of the injury) were identified. Second, the Narrative fields of all of the records were individually reviewed to determine whether the injury appeared to be related to a cell phone while using non-motor vehicles. A record was included even if its Narrative field did not explicitly state that the phone was a cell phone because it was assumed that a landline phone, even a cordless phone, would not be used with a non-motor vehicle. Records where the patient was not in or on the non-motor vehicle with the cell phone (eg, the patient was walking down the street and was hit by a bicycle whose rider was texting on their cell phone) were excluded.
 The examined variables were the affected body part, type of non-motor vehicle, year and month of treatment, patient age and gender, location of the incident, most severe diagnosis, and patient disposition. The type of non-motor vehicle was identified from the record Narrative. Some vehicles may or may not have a motor (eg, bicycle, scooter, wheelchair). For such vehicles, if the record did not specifically indicate that the vehicle had a motor, it was included in the analysis.
The examined variables were the affected body part, type of non-motor vehicle, year and month of treatment, patient age and gender, location of the incident, most severe diagnosis, and patient disposition. The type of non-motor vehicle was identified from the record Narrative. Some vehicles may or may not have a motor (eg, bicycle, scooter, wheelchair). For such vehicles, if the record did not specifically indicate that the vehicle had a motor, it was included in the analysis.
A person injured while using a non-motor vehicle may experience multiple injuries to multiple body parts. The NEISS database contains multiple fields for documenting the diagnosis and/or affected body part; however, only 2 fields were used consistently throughout the study period: Diagnosis (a numeric field for coding the most severe diagnosis) and Body_Part (a numeric field for coding the body part associated with the most severe diagnosis). (All diagnoses are supposed to be documented in the Narrative, but this is not performed in a consistent manner.) Therefore, only the Diagnosis and Body_Part numeric fields were used to analyze the diagnosis and affected body part.
Analyses were performed using Microsoft 365 Access and Excel (Microsoft Corporation, Redmond, Washington, US). For the selected variables, the distribution of the national injury estimates was determined for cell phone-related injuries while using non-motor vehicles affecting (1) any body part (total injuries) and (2) the subset of lower extremity injuries (based on the Body_Part field). Comparisons were made between the two groups for the studied variables by calculating the lower extremity rate (lower extremity injury estimate/total injury estimate x 100, presented as a percentage). National injury estimates were calculated by summing the values in the Weight numeric field in the publicly available NEISS database. The CPSC considers an estimate unstable and potentially unreliable when the estimate is <1,200.15
Results
An estimated 1,261 cell phone-related injuries while using non-motor vehicles were treated at US hospital EDs during 2000-2023 where the most severe diagnosis affected the lower extremity, representing 14.8% of the estimated 8,536 such injuries affecting all body parts. The distribution of lower extremity injuries by affected body part was 620 (49.1%) knee, 222 (17.6%) lower leg, 156 (12.4%) ankle, 176 (13.9%) upper leg, 87 (6.9%) toe, and 0 (0.0%) foot.
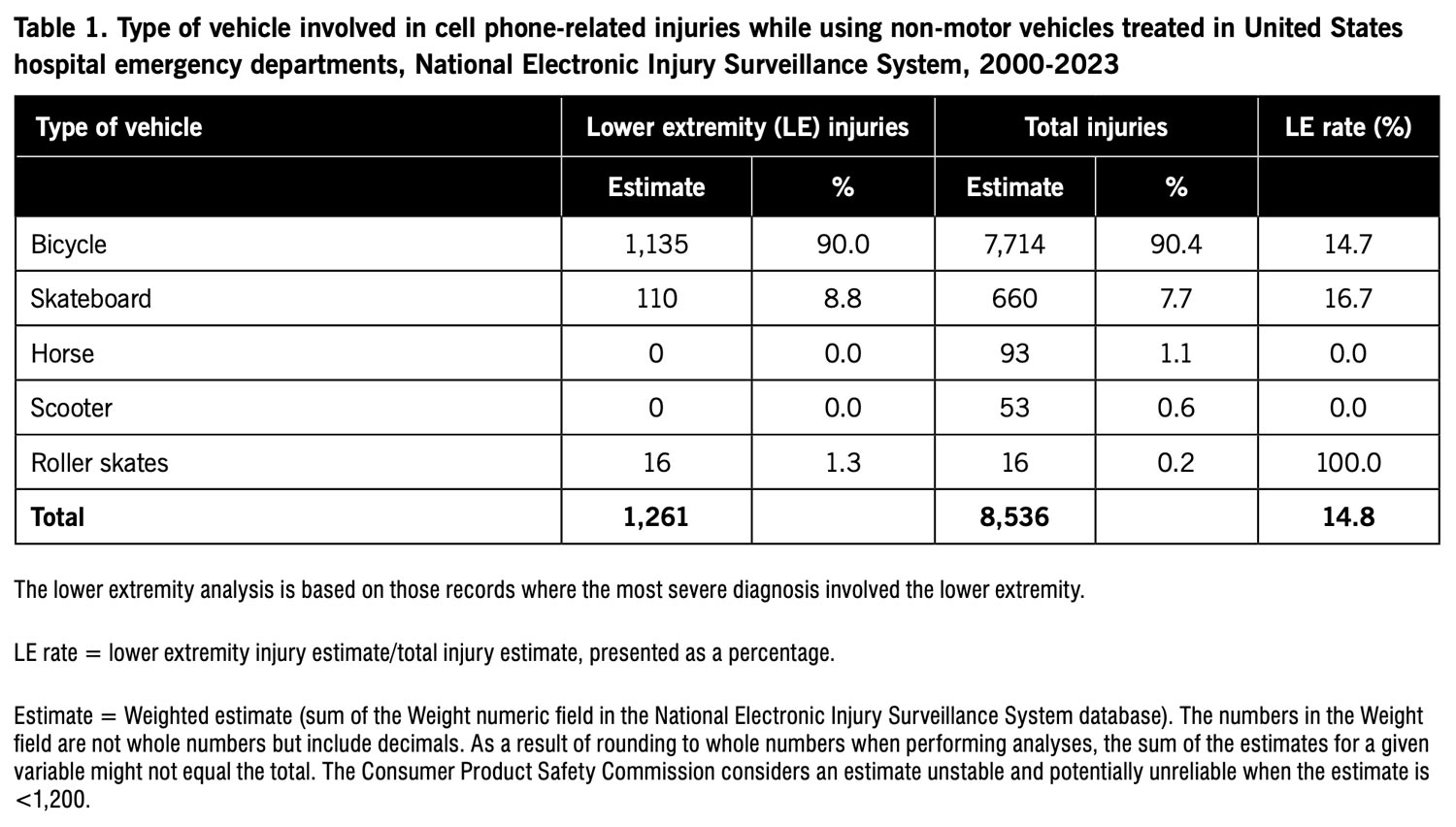
Over 90% of both total injuries and lower extremity injuries involved bicycles (Table 1). However, a small proportion involved skateboards, scooters, roller skates, and even horses.
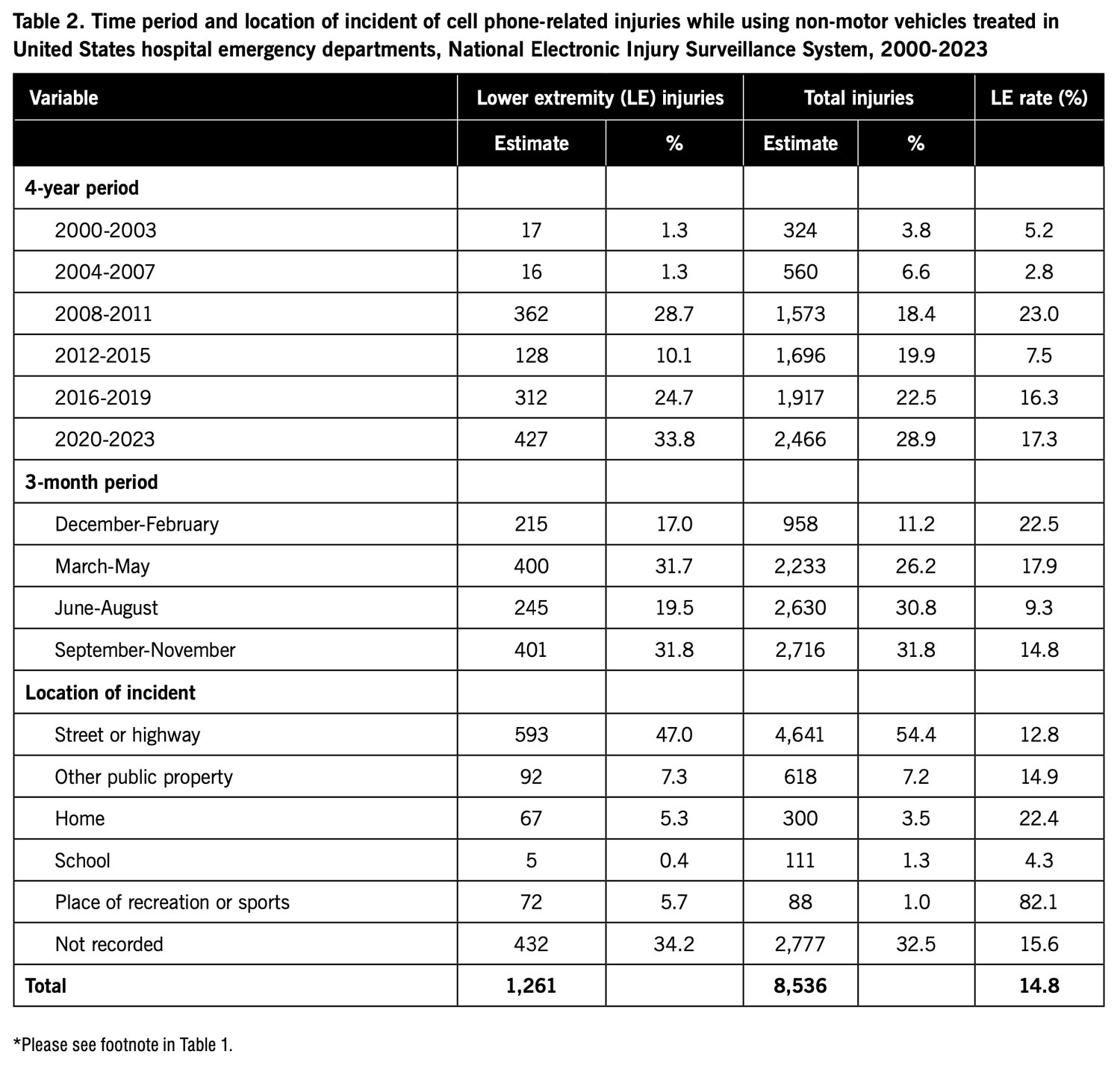
Table 2 shows the distribution of cell phone-related injuries while using non-motor vehicles by time period and location of the incident. When the 24-year period was divided into 6 4-year periods, the estimated number of total injuries increased with each 4-year period. While the highest estimated number of lower extremity injuries was reported during the most recent 4-year period (2020-2023), the next highest estimated number of lower extremity injuries was reported during 2008-2011. However, for lower extremity injuries, the general trend was an increase in estimated injuries over time.
 For both lower extremity and total injuries, the lowest proportion of injuries were treated during December-February. However, the lower extremity rate was higher for December-February than for any other 3-month period. For those injuries where the location of the incident was recorded, most of the lower extremity injuries and total injuries occurred on a street or highway. Smaller proportions of injuries occurred at other public property, home, school, and a place of recreation or sports.
For both lower extremity and total injuries, the lowest proportion of injuries were treated during December-February. However, the lower extremity rate was higher for December-February than for any other 3-month period. For those injuries where the location of the incident was recorded, most of the lower extremity injuries and total injuries occurred on a street or highway. Smaller proportions of injuries occurred at other public property, home, school, and a place of recreation or sports.
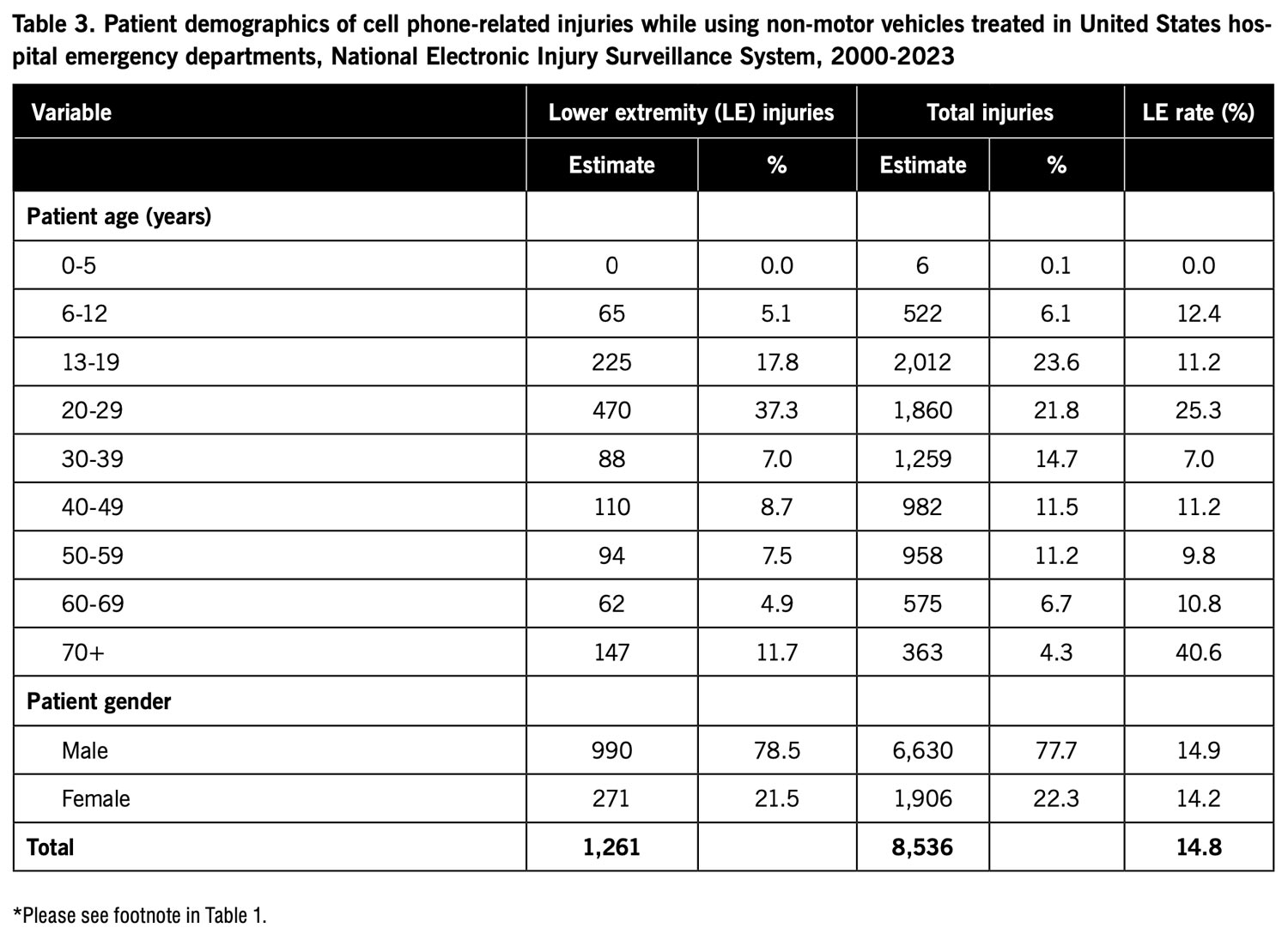
When cell phone-related injuries while using non-motor vehicles were examined by patient age (Table 3), relatively few injuries were reported among patients aged 0-12 years. For lower extremity injuries, the highest proportion of patients were aged 20-29 years, followed by patients aged 13-19 years. For total injuries, the highest proportion of patients were aged 13-19 years, followed by patients aged 20-29 years. The lower extremity rate was twice as high for patients aged 20-29 years than for patients aged 13-19 years. For both lower extremity injuries and total injuries, most patients were male (Table 3). The lower extremity rate did not differ greatly between the sexes.
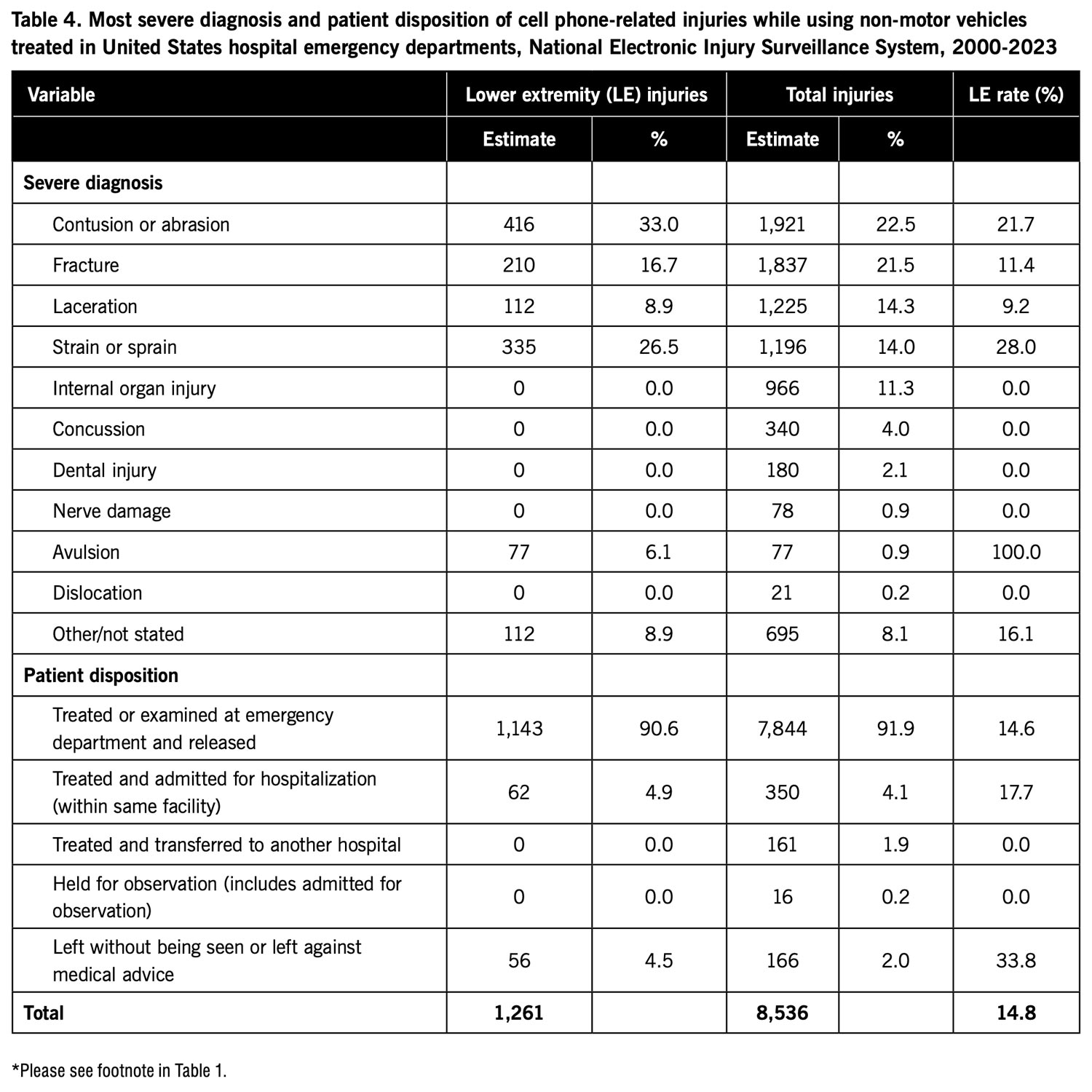
Table 4 presents the distribution of cell phone-related injuries while using non-motor vehicles by most severe diagnosis and patient disposition. For total injuries, the most frequently reported diagnosis was contusion or abrasion followed by fracture, laceration, and strain or sprain. For lower extremity injuries, the most frequently reported diagnosis was contusion or abrasion followed by strain or sprain, fracture, and laceration. The lower extremity rate was highest for strain or sprain and lowest for laceration. For both lower extremity injuries and total injuries, most of the patients were treated or examined in the hospital ED and released.
Discussion
Cell phone-related injuries while using non-motor vehicles treated at US hospital EDs were relatively uncommon. Only an estimated 8,536 such injuries were reported during a 24-year period, and of these, only an estimated 1,261 (15%) had the most severe diagnosis affect the lower extremity. However, the estimated number of injuries increased over this time period, with 30% of total injuries and 34% of lower extremity injuries reported during the most recent 4 years (2020-2023). If this trend continues, cell phone-related injuries while using non-motor vehicles might become more common and a greater public health issue in the future.
The increase in cell phone-related injuries while using non-motor vehicles over the time period is consistent with several other studies using NEISS data that also observed temporal increases in cell phone-related injuries,20,22,23 including several that focused on lower extremity injuries (but not injuries while using non-motor vehicles).17,18 This increase is likely due to an increase in the number of people owning cell phones. A November 2024 Pew Research Center fact sheet indicated that the proportion of adults reporting ownership of cell phones increased from 62% in 2002 to 98% in 2024.1 Alternately, it may be that, over time, the hospital staff providing records to NEISS increasingly documented in the Narrative field that the injury was related to cell phone use while using non-motor vehicles.
Of the most severe diagnosis affecting the lower extremity, almost half involved the knee while an additional 30% involved the lower leg and ankle. This indicates that all lower extremity body parts are not at equal risk of cell phone-related injuries while using non-motor vehicles.
For both lower extremity injuries and total injuries, the lowest proportion of injuries were treated during December-February. This might be expected because the weather is usually coldest in the US during these months. Consequently, during December-February, people may be less likely to ride bicycles or use other non-motor vehicles outside. Although December-February had the smallest proportion of injuries, it had the highest lower extremity rate. It may be that there are seasonal differences in the types of activities causing cell phone-related injuries while using non-motor vehicles and their likelihood to involve the lower extremity.
For both lower extremity injuries and total injuries, relatively few of the patients were aged 0-12 years and the highest proportion of patients were aged 13-29 years. Moreover, almost 80% of the patients were male. It may be that persons aged 13-29 years and males are more likely to use bicycles and other non-motor vehicles. Alternately, persons of this age group and sex may be more likely to use cell phones while using non-motor vehicles.
 The lower extremity rate was twice as high for patients aged 20-29 years than for patients aged 13-19 years. It may be that people aged 13-19 years are less likely than people aged 20-29 years to engage in the types of activities causing cell phone-related injuries while using non-motor vehicles that affect the lower extremity.
The lower extremity rate was twice as high for patients aged 20-29 years than for patients aged 13-19 years. It may be that people aged 13-19 years are less likely than people aged 20-29 years to engage in the types of activities causing cell phone-related injuries while using non-motor vehicles that affect the lower extremity.
Several other studies used the NEISS database to examine other types of cell phone-related injuries during the same time period. Among cell phone-related injuries while walking, relatively few of the patients were aged 0-12 years, and the highest proportion of patients were aged 13-29 years, like the age pattern observed in the present study. However, most patients in those studies were female.17 Additionally, among cell phone-related injuries while in or on a motor vehicle, while relatively few of the patients were aged 0-12 years, the highest proportion of patients were aged 20-39 years. Moreover, while most of the patients with lower extremity injuries were male, patients with total injuries were more evenly divided by sex.18 This suggests that education and prevention efforts may need to focus on different demographic groups depending on which type of cell phone-related injuries are being targeted.
Lower extremity injuries and total injuries differed by the pattern of diagnosis. For total injuries, the most frequently reported diagnosis was contusion or abrasion followed by fracture, laceration, and strain or sprain. For lower extremity injuries, the most frequently reported diagnosis was contusion or abrasion followed by strain or sprain, fracture, and laceration. These differences might partly be expected considering certain diagnoses (eg, internal organ injury, concussion, dental injury) cannot affect the lower extremity.
In most cases, the most frequently reported diagnoses (contusion or abrasion, fracture, laceration, and strain or sprain) might not be expected to require extensive hospital management. In fact, this study found that over 90% of the patients were treated or examined in the hospital ED and released.
There are limitations to this study. As described in the Methods section, the NEISS database does not have any fields or codes to easily identify cell phone-related injuries. For this study, all records where the product code for telephones or telephone accessories was used in any of the product code fields or “phone” was used in the Narrative field were identified. Then the Narrative for each record was reviewed to determine whether the injury was related to a cell phone while using non-motor vehicles. The study would not include any records that did not include the telephones or telephone accessories product code or “phone” in the Narrative field.
A person experiencing a cell phone-related injury while using a non-motor vehicle may experience multiple injuries of multiple body parts. This study was limited to the data fields that coded the single most severe diagnosis and affected body part because these were the only fields that consistently documented diagnosis and affected body part throughout the entire study period. Thus, a higher proportion of patients may have experienced lower extremity injuries.
A single person selected the records for inclusion in the study. In addition, the study included only those patients treated at hospital EDs. Examination of patients treated elsewhere would provide a more complete understanding of injuries that occur while using a cell phone while using non-motor vehicles.
In conclusion, relatively few cell phone-related injuries while using non-motor vehicles, particularly involving the lower extremity, were treated at US hospital EDs during the 24-year period. Most of these injuries involved bicycles. Almost half of the severe diagnoses affecting the lower extremity involved the knee. The most common severe diagnoses affecting the lower extremity were contusion or abrasion followed by strain or sprain. Most patients were treated or evaluated and released from the ED. The information in this study may be useful for creating educational activities to prevent or manage these injuries in the future.
Mathias B. Forrester, BS, is an independent researcher in Austin, Texas. Now retired, he has performed public health research for various university and government programs for 39 years.
- Pew Research Center. Mobile fact sheet. November 13, 2024. Available at https://www.pewresearch.org/internet/fact-sheet/mobile/. Accessed March 1, 2025.
- Russo BJ, James E, Aguilar CY, Smaglik EJ. Pedestrian behavior at signalized intersection crosswalks: Observational study of factors associated with distracted walking, pedestrian violations, and walking speed. Trans Res Rec. 2018;2672(35):1-12.
- Barkley JE, Lepp A. Cellular telephone use during free-living walking significantly reduces average walking speed. BMC Res Notes. 2016;9:195.
- Basch CH, Ethan D, Rajan S, Basch CE. Technology-related distracted walking behaviours in Manhattan’s most dangerous intersections. J Community Health. 2015;40(4):789-792.
- Caird JK, Johnston KA, Willness CR, Asbridge M, Steel P. A meta-analysis of the effects of texting on driving. Accid Anal Prev. 2014;71:311-318.
- Thompson LL, Rivara FP, Ayyagari RC, Ebel BE. Impact of social and technological distraction on pedestrian crossing behaviour: an observational study. Inj Prev. 2013;19(4):232-237.
- Redelmeier DA, Tibshirani RJ. Association between cellular-telephone calls and motor vehicle collisions. N Engl J Med. 1997;336(7):453-458.
- Wu X, Xiao W, Deng C, Schwebel DC, Hu G. Unsafe riding behaviors of shared-bicycle riders in urban China: A retrospective survey. Accid Anal Prev. 2019;131:1-7.
- de Waard D, Westerhuis F, Lewis-Evans B. More screen operation than calling: the results of observing cyclists’ behaviour while using mobile phones. Accid Anal Prev. 2015;76:42-48.
- de Waard D, Schepers P, Ormel W, Brookhuis K. Mobile phone use while cycling: Incidence and effects on behaviour and safety. Ergonomics. 2010;53(1):30-42.
- Wolfe ES, Arabian SS, Breeze JL, Salzler MJ. Distracted biking: An observational study. J Trauma Nurs. 2016;23(2):65-70.
- Terzano K. Bicycling safety and distracted behavior in The Hague, the Netherlands. Accid Anal Prev. 2013;57:87-90.
- Ren J, Chen Y, Li F, et al. Road injuries associated with cellular phone use while walking or riding a bicycle or an electric bicycle: A case-crossover study. Am J Epidemiol. 2021;190(1):37-43.
- Forrester MB. Pickleball-related injuries involving the lower extremity treated in emergency departments. Lower Extremity Review. 2021;13(5):24-30.
- United States Consumer Product Safety Commission. National Electronic Injury Surveillance System (NEISS). Available at https://www.cpsc.gov/Research–Statistics/NEISS-Injury-Data/Explanation-Of-NEISS-Estimates-Obtained-Through-The-CPSC-Website. Accessed March 1, 2025.
- United States Consumer Product Safety Commission. NEISS Coding Manual. January 2021. Available at https://www.cpsc.gov/s3fs-public/January-2021-NT-CPSC-only-NEISS-Coding-Manual.pdf?xa_nMM1kB4SGpuSMOwf0NHkkkIqNcn8F. Accessed March 1, 2025.
- Forrester MB. Cell phone-related lower extremity injuries while walking. Lower Extremity Review. 2024;16(11):46-53.
- Forrester MB. Cell phone-related lower extremity injuries while in or on a motor vehicle. Lower Extremity Review. 2025;17(1):30-34.
- McLaughlin WM, Cravez E, Caruana DL, Wilhelm C, Modrak M, Gardner EC. An epidemiological study of cell phone-related injuries of the hand and wrist reported in United States emergency departments from 2011 to 2020. J Hand Surg Glob Online. 2023;5(2):184-188.
- Zheng H, Giang WCW. Risk perception and distraction engagement with smart devices in different types of walking environments. Accid Anal Prev. 2021;162:106405.
- Guyon PW Jr, Corroon J, Ferran K, Hollenbach K, Nguyen M. Hold the phone! Cell phone-related injuries in children, teens, and young adults are on the rise. Glob Pediatr Health. 2020;7:2333794X20968459.
- Nasar JL, Troyer D. Pedestrian injuries due to mobile phone use in public places. Accid Anal Prev. 2013;57:91-95.
- Smith DC, Schreiber KM, Saltos A, Lichenstein SB, Lichenstein R. Ambulatory cell phone injuries in the United States: an emerging national concern. J Safety Res. 2013;47:19-23.







