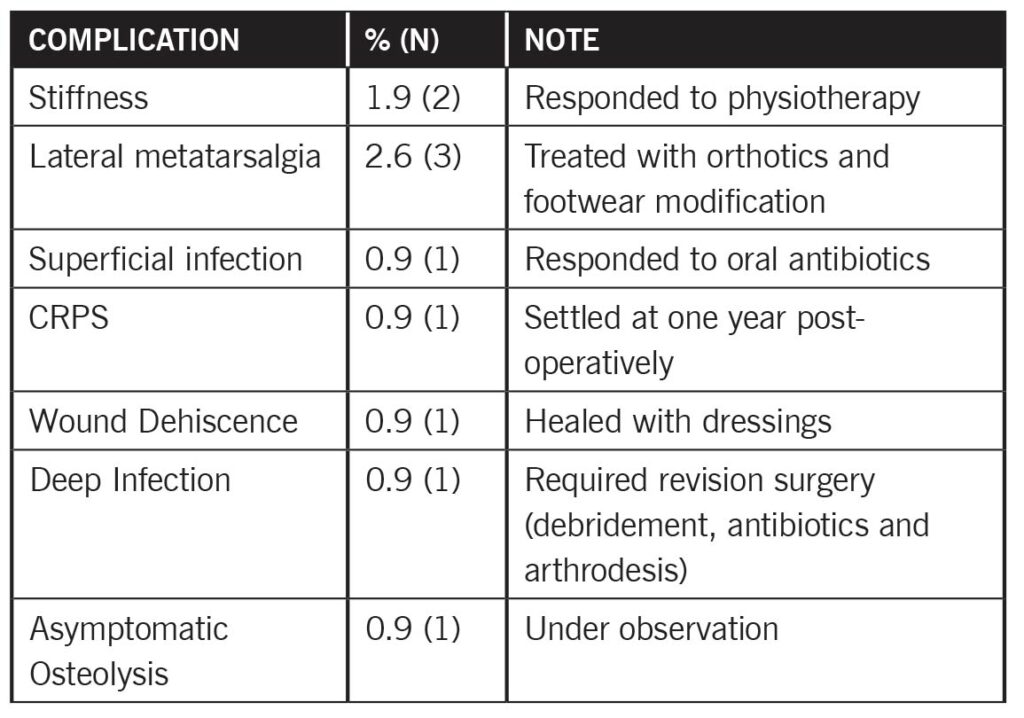
Table 1. Complications of first metatarsophalangeal silastic joint replacement in 112 patients. CRPS: complex regional pain syndrome
Osteoarthritis of the first metatarsophalangeal joint (MTPJ) is a common forefoot problem affecting patients in later years. It leads to pain, gait problems, and difficulty with activities of daily living. Treatment is controversial and varies according to patient symptoms and surgeon preference. Arthrodesis remains the gold standard but it has its own complications. It is associated with adjacent joint arthritis and transfer metatarsalgia. The aim of this study from Great Britain was to analyze the outcome of double-stemmed silastic joint arthroplasty (Wright-Medical, Memphis, TN) for end-stage hallux rigidus.
This retrospective analysis included 117 consecutive first MTPJ silastic arthroplasties done between January 2016 and February 2023 for end-stage hallux rigidus. There were 77 females and 40 males with a mean age of 65 years (46-82 years). Radiological and clinical assessments were performed, and patient-reported outcome measure data (PROMS) and visual analogue scale (VAS) scores were collected pre- and post-operatively.
Findings showed 99.1% survivorship following a silastic joint arthroplasty with a mean follow-up of 4 years (6 months to 7 years). The MOXFQ (Manchester Oxford Foot Questionnaire) score improved from a mean of 81 (59.8-100) to 13 (0-57). The mean VAS scores improved from 7.2 (5-10) to 1.5 (0-7) postoperatively. Five patients were lost to follow-up. Two patients developed deep infection and 1 required revision. The other patient with infection was lost to follow-up. In total 10 patients (8.9%) developed complications, out of which 8 patients responded to simple treatments.
The authors concluded that results have shown good to excellent outcomes following a silastic arthroplasty of the first MTPJ for the treatment of end-stage hallux rigidus. The survivorship at a mean follow-up of 4 years was 99.1% and the patient satisfaction rate was 90.1%. As historically reported, they did not see any soft tissue reaction or progressive osteolysis in any of their patients. It provides comparable and predictable outcomes to joint fusion for end-stage arthritis.
Source: Sethi M, Limaye N, Alderton E, et al. Silastic joint arthroplasty as a joint-preserving alternative for end-stage Hallux Rigidus: outcomes from 112 first metatarsophalangeal joint arthroplasties. Cureus. 2023;15(10): e46561. DOI 10.7759/cureus.46561