By Marianne Mørk, Helene Lundgaard Soberg, Aasne Fenne Hoksrud, Marte Heide, and Karen Synne Groven
Plantar fasciopathy pain forces individuals to make adjustments in physical activity leading to reduced quality of life.
 Plantar fasciopathy (PF) is the most common cause of heel pain, and is associated with decreased physical activity level and quality of life. There has been limited research on the experiences of patients with PF. With an emphasis on including psychosocial aspects along with the biomedical approach in treating patients with PF, the present study seeks to bridge a gap in the literature and contribute with in-depth insight into the bodily experiences of individuals with PF. This was done by addressing the following question: “What are the experiences, thoughts, and concerns of patients with persistent plantar fasciopathy, and how do they cope with everyday life?”
Plantar fasciopathy (PF) is the most common cause of heel pain, and is associated with decreased physical activity level and quality of life. There has been limited research on the experiences of patients with PF. With an emphasis on including psychosocial aspects along with the biomedical approach in treating patients with PF, the present study seeks to bridge a gap in the literature and contribute with in-depth insight into the bodily experiences of individuals with PF. This was done by addressing the following question: “What are the experiences, thoughts, and concerns of patients with persistent plantar fasciopathy, and how do they cope with everyday life?”
Methods
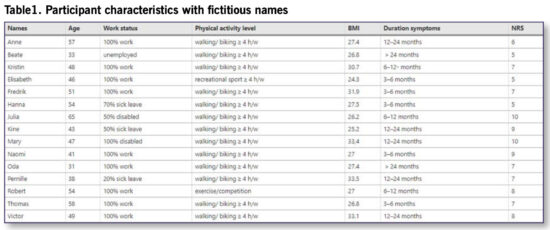
The study cohort comprised 15 participants with longstanding PF (11 females, 4 four males; age 31–65). In order to capture a range of characteristics, the study authors used a purposeful selection method based on gender, age, body mass index (BMI), work status, duration of symptoms, and pain intensity (numeric rating scale (NRS) ranging from 5–10) (See Table 1). Face-to-face, semi-structured interviews were audio recorded, transcribed verbatim, and analyzed using Braun and Clark’s reflexive thematic analysis. An inductive approach led by a phenomenological theoretical framework was used.
Results
Three core themes and 9 sub-themes were identified. The first theme was ‘Struggling to stay active’ with sub-themes ‘Struggling with pain and how to adjust it,’ ‘Finding alternative activities,’ and ‘Longing for the experience of walking.’ The second main theme was ‘Emotional challenges’ with the sub-themes ‘Feelings of frustration and self-blame’ and ‘Worries of weight gain and related consequences.’ The third main theme was ‘Relations to others’ with the sub-themes ‘Participation in family and social life,’ ‘Visible in new ways,’ ‘Striving to avoid sick leave,’ and ‘Bothering others.’
Discussion
The study authors aimed to explore the experiences of individuals with longstanding PF. To address their research question, they discussed their findings with reference to the body from a phenomenological theoretical perspective, supplemented with previous research.
A major finding in the study was that participants regarded pain during and after walking as the most problematic aspect of living with PF. They experienced fear of pain and uncertainty as they struggled to find a balance between challenging their pain and trying not to aggravate it, and expressed how their foot pain became the focus of their attention. They could not take their body for granted anymore, and experienced their body as an obstacle in everyday life. These doubts led them to continuously monitor their pain and dominated their decisions regarding avoiding painful physical activities, limiting their freedom to move.
This study highlights the participants’ challenges with having to adjust their physical activity. While some expressed negative emotions associated with becoming significantly less active, others elaborated on the importance of finding alternatives to weight bearing activities when coping with PF. Participants felt that swimming, biking, rowing, and strengthening exercises were all feasible activities that contributed to positive experiences.
Participants in this study emphasized the importance of walking prior to being diagnosed with PF. Many participants experienced better mood, more energy, and the feeling of happiness when walking. Prevented from walking as they had before, participants described a longing for the experiences of eu-appearance when walking, a bodily awareness in which mind and body work harmoniously together.
 Participants in this study described how their heel pain led to a limping gait, the need for crutches, or being unable to maintain the same pace as others, which made them feel embarrassed and uncomfortable. The body became thematized as a problem disrupting communication with others.
Participants in this study described how their heel pain led to a limping gait, the need for crutches, or being unable to maintain the same pace as others, which made them feel embarrassed and uncomfortable. The body became thematized as a problem disrupting communication with others.
The participants in this study experienced their heel pain at present as severe and overriding, giving rise to feelings of powerlessness regarding how to influence or speed up the healing process. These results show that the participants experienced frustration and psychological distress due to their present pain and being unable to stay as physically active as they used to, as well as sadness for what they missed out on, but at the same time, many had hope for the future, albeit with some uncertainty.
According to the study findings, participants experienced that heel pain limited their participation in social activities. Being unable to join friends and family in physical activities like they used to triggered feelings of loneliness and distanced them from those closest to them. They experienced guilt for not being able to contribute to family life as they had before and increasing the burden on others.
According to the study findings, concerns regarding being overweight, in the sense that their BMI was classified as overweight or obese (BMI range from 24–33), predominated. Participants commonly feared developing lifestyle diseases and also mental illnesses like depression due to weight gain. Those who had previously emphasized intensive physical activity as a means of preventing overweight, anxiety, or depression, worried about their future in terms of how stress and fear would develop. Participants in this study often felt overwhelmed, passive, and out of control when handling their pain, but at other times, some felt in control when finding alternative ways to stay active and avoid weight gain.
The study participants described the value of working on a daily basis and interacting socially with colleagues, both of which helped them to focus on something other than pain. They worried about how they would cope on sick leave, and feared experiencing isolation, depression, and an increased focus on their pain. Some of the participants struggled for a long time at work, trying to ignore their foot pain. When the pain began affecting their sleep, it became impossible to perform their duties at work and they had to go on sick leave. Being on sick leave seemed to entail less heel pain for those with standing or walking jobs; however, participants found it hard to come to terms with both in regard to their own self-respect as well as the fear of losing the respect of others.
Along with the desire to remain in work, participants explained how avoiding involving family, friends, colleagues, and employers was the best way to handle the pain. They did not wish to be seen as whiners, and many were uncomfortable asking others for help.
Some of the participants in this study experienced fear of being disbelieved by others, in particular by their colleagues and employers. Not being met with empathy made the participants hesitant to involve others in handling their pain. By not involving others, they avoided focusing on their painful heel, and the fear of being objectified or not being met with empathy. On the other hand, by not reaching out for support, they missed out on empathy, compassion, and support from others.
Although the majority of the participants in this study managed to stay in work and believed it helped them to cope, they might also experience increased pain and higher level of psychosocial distress, which could influence their recovery from heel pain.
Conclusions
The study results demonstrate how heel pain permeated the participants’ lives in a complex and intertwined way. The suffering from persistent PF does not seem to be limited to the foot alone. Participants in this study explained how they struggled on an individual level, but also how their pain affected their relationship with others and their surroundings. Aggravated pain while walking and the efforts to stay physically active predominated the participants’ lives. Furthermore, feelings of frustration, hopelessness, self-blame, diminished social interaction with others, and worries of weight gain and its related consequences became daily experiences for participants with persistent PF. They emphasized the importance of finding alternative ways to stay active and avoiding sick leave.
The clinical implications of these findings point to supplementing a bio-psycho-social perspective with a bodily phenomenological approach acknowledging the lived experiences of pain in order to provide holistic and individually tailored care for individuals with persistent PF. Clinicians should help individuals with PF to find ways to stay in work and remain physically activity, either with load management regarding weight-bearing activities or by finding alternative activities. Furthermore, these results suggest that it is important to show empathy and interest regarding the patients’ concerns about living with longstanding heel pain. Caregivers should seek to understand each unique subjective experience of people living with PF in order to help individuals trapped with stubborn heel pain.
This article has been excerpted from “The Struggle to Stay Physically Active—A Qualitative Study Exploring Experiences of Individuals with Persistent Plantar Fasciopathy,” J Foot Ankle Res 16, 20 (2023). https://doi.org/10.1186/s13047-023-00620-4. Editing has occurred, including the renumbering or removal of tables, and references have been removed for brevity. Use is per CC BY 4.0 International License.








