By Windy Cole, DPM, CWSP
By Windy Cole, DPM, CWSP
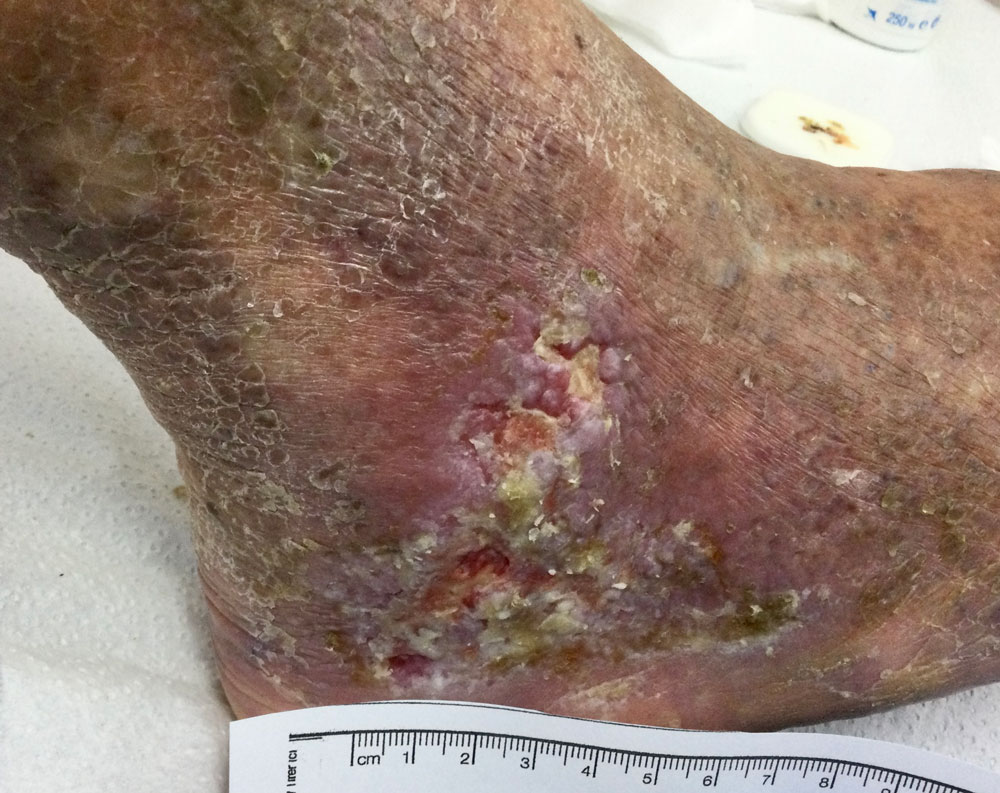
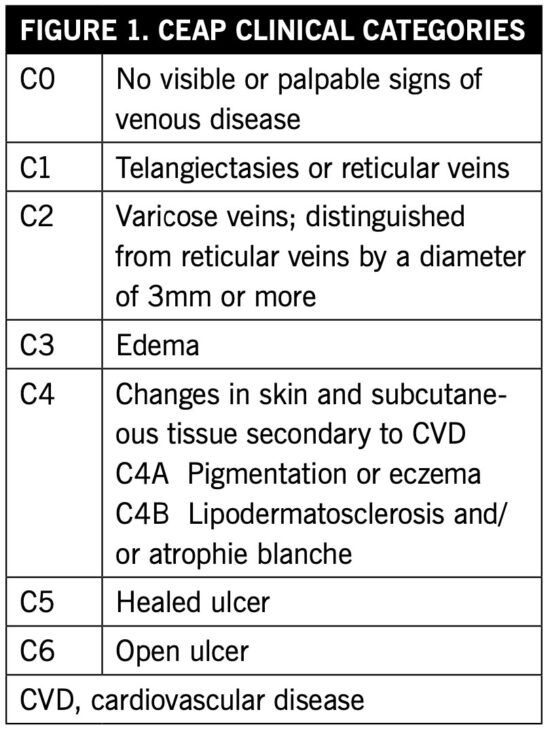
Is there a link between diabetes and chronic venous insufficiency (CVI)? Well, let’s just say that relationship is “complicated.” While diabetes may not directly cause venous insufficiency, it does have an effect on the tissues of the lower extremities. It has been documented that glycosylated hemoglobin is damaging to endothelium, and hyperglycemia and hyperlipidemia injure lymphatic tissue.1 When diagnosed together, these disease states can have an overwhelming negative effect. A 2022 study published in the Journal of Vascular Surgery noted that higher Clinical, Etiological, Anatomical, and Pathological (CEAP; Figure 1) category patients also had a greater prevalence of diabetes.1 Additional research is needed to establish causation and correlation.
There are many underlying health and lifestyle factors seen in patients with diabetes that can contribute to the development of venous disease. High blood glucose levels seen in uncontrolled/undiagnosed diabetes can weaken the structure of the vein walls and can cause damage over time. Additionally, weight gain associated with uncontrolled diabetes could make venous disease more likely by causing additional strain on the venous system. A study conducted by Mani and colleagues examined the point of prevalence of venous disease in the diabetic population.2 The investigators found a significantly higher level of venous incompetence in their study cohort (64% to 70% ) than had previously been reported (~43% to ~50%).2 Furthermore, they reported that the study results suggested the presence of hemodynamic changes and morphological changes in diabetic patients with and without foot disease.2 Conclusions can be drawn that if the hemodynamic changes seen in the venous system of diabetic patients can be controlled, there is potential to decrease the number of diabetic foot ulcers that occur. Additional studies are needed to prove this hypothesis.
 CVI Management
CVI Management
The co-existence of diabetes and CVI impacts wound healing outcomes. Edema causes an alteration in endothelium that begins a complex cascade of detrimental events. Neutrophils become activated and adhere to capillary walls thus creating ischemia-reperfusion injury releasing free oxygen species.3 The resulting inflammation damages the vasculature and soft tissues.3 As hypoxia ensues, inflammation worsens, and harmful matrix metalloproteinases cause dermal tissue fibrosis and eventual ulceration.3 Compression therapy facilitates the removal of lower extremity edema. White blood cells detach from the endothelium. Inflammation lessens. Decreasing edema improves microcirculation. As perfusion improves, the tissue environment stabilizes and tissue fibrosis decreases.
Evidence-based guidelines on managing diabetic foot ulcers and venous leg ulcers strongly advise patients undergo Ankle-Brachial Index/Toe-Brachial Index (ABI/TBI) and venous insufficiency ultrasound to confirm clinical diagnosis and to determine the appropriate treatment pathway. Appropriate vascular evaluations also aid in the proper application of compression therapy to control interstitial edema and lymphedema. Finding a compression therapy solution that is also safe and effective in the diabetic patient will have additional benefits in this at-risk patient population. This is a great opportunity in wound care research to improve outcomes in wound closure that can potentially impact the entire healthcare system.
- Singh TP, Velu RB, Quigley F, Golledge J. Association of chronic venous disease with major adverse cardiovascular events. J Vasc Surg Venous Lymphat Disord. 2022;10(3):683-688. doi: 10.1016/j.jvsv.2021.08.021.
- Mani R, Yarde S, Edmonds M. Prevalence of deep venous incompetence and microvascular abnormalities in patients with diabetes mellitus. Int J Low Extrem Wounds. 2011;10(2):75-9.
- Mariani F, ed. Compression: consensus document based on scientific evidence and clinical experiences. The Compression Therapy Study Group. Task Force 2009. Torino, Italy: Edizioni Minerva Medica S.p.A; 2009.