 By Mathias B. Forrester, BS
By Mathias B. Forrester, BS
Background: There are millions of pet dogs in the United States (US), and thousands of people are treated at US hospital emergency departments (EDs) each year for dog bites. Approximately 20-25% of these dog bites affect the lower extremity. The objective of this study was to characterize dog bites of the lower extremity treated at US hospital EDs.
Methods: An analysis was performed of dog bites of the lower extremity using data from the National Electronic Injury Surveillance System-All Injury Program (NEISS-AIP) of the US Consumer Product Safety Commission (CPSC) during 2005-2019.
Results: A total of 18,357 dog bites of the lower extremity treated at a sample of US hospital EDs was identified during 2005-2019, resulting in a national estimate of 1,090,110 dog bites of the lower extremity. Of the estimated dog bites, 49.4% of the patients were age 0-29 years and 50.8% were male. Home was the incident location in 44.4% of the dog bites. The patients were treated or examined and released from the ED in 96.2% of the encounters. The most commonly reported injuries were puncture (33.0%), laceration (16.9%), and contusion or abrasion (10.4%). The most frequently affected body part was the lower leg (53.4%) followed by the upper leg (26.9%).
Conclusions: Patients with dog bites of the lower extremity tended to be younger, particularly age 29 years or less, and a slightly higher proportion were male. Most of the dog bites with a known incident location occurred at home. The majority of patients were treated or examined at the hospital ED and released. The most frequently reported diagnoses were puncture, laceration, and contusion or abrasion, and the most commonly affected body parts were the lower leg followed by the upper leg.
The American Veterinary Medical Association (AVMA) reported that, by year-end 2016, there were 77 million pet dogs in the United States (US), and 38.4% of US households owned a dog.1 According to the 2021-2022 National Pet Owners Survey, 69.0 million US households owned a dog.2
Dog bites are a significant public health issue. Dogs bite approximately 4.5 million people in the US annually.3 During 2005-2013, there was an estimated average of 337,103 visits to US hospital emergency departments (EDs) per year for non-fatal dog bites, and dog bites were the thirteenth most common cause of non-fatal injuries treated at US hospital EDs.4
Several studies have reported that 20-25% of dog bites treated at US hospital EDs were to the lower extremity.4,5 The objective of this study was to describe dog bites of the lower extremity treated at US hospital EDs.
Methods
Data for this study were downloaded from the National Electronic Injury Surveillance System-All Injury Program (NEISS-AIP) at https://www.icpsr.umich.edu/web/NACJD/search/studies?q=national%20electronic&. In 2000, the Centers for Disease Control and Prevention (CDC) collaborated with the Consumer Product Safety Commission (CPSC) to expand the National Electronic Injury Surveillance System (NEISS) to collect data on all types and causes of nonfatal injuries treated in a representative sample of US hospital EDs, creating the NEISS-AIP.6,7 The NEISS-AIP defines a nonfatal injury as bodily harm resulting from severe exposure to an external force, substance, or submission. This bodily harm can be unintentional or violence-related.
 The NEISS-AIP collects data from a stratified random sample of 66 of the more than 5,000 hospitals with 24-hour EDs and six or more beds in the US.6,7 The random sample is stratified by hospital size, geographic location (so that all parts of the US are represented), and hospital type (general and pediatric hospitals). Professional NEISS-AIP coders review the ED records at participating hospitals and, for patients with injuries that meet NEISS-AIP inclusion criteria, collect and code all information in the NEISS-AIP database except for the cause of injury. The coded data and a narrative (description) are electronically transmitted to the CPSC. CPSC coders review all of the data elements and narrative for every submitted record. The CPSC coders then use the narrative and other data to assign codes for the cause (mechanism) of injury for each case. The data in the NEISS-AIP database include age, race, Hispanic origin, and sex of the injured person; diagnosis and body part affected; location where the injury incident occurred; up to two consumer products involved; disposition; cause of injury; intent of injury; and whether the injury is related to work. For transportation-related injuries, the NEISS-AIP collects data about whether the injury was related to traffic and the status of the motor vehicle occupant. For assaults, NEISS-AIP collects data about the relationship of the perpetrator to the injured person and the context of the assault.
The NEISS-AIP collects data from a stratified random sample of 66 of the more than 5,000 hospitals with 24-hour EDs and six or more beds in the US.6,7 The random sample is stratified by hospital size, geographic location (so that all parts of the US are represented), and hospital type (general and pediatric hospitals). Professional NEISS-AIP coders review the ED records at participating hospitals and, for patients with injuries that meet NEISS-AIP inclusion criteria, collect and code all information in the NEISS-AIP database except for the cause of injury. The coded data and a narrative (description) are electronically transmitted to the CPSC. CPSC coders review all of the data elements and narrative for every submitted record. The CPSC coders then use the narrative and other data to assign codes for the cause (mechanism) of injury for each case. The data in the NEISS-AIP database include age, race, Hispanic origin, and sex of the injured person; diagnosis and body part affected; location where the injury incident occurred; up to two consumer products involved; disposition; cause of injury; intent of injury; and whether the injury is related to work. For transportation-related injuries, the NEISS-AIP collects data about whether the injury was related to traffic and the status of the motor vehicle occupant. For assaults, NEISS-AIP collects data about the relationship of the perpetrator to the injured person and the context of the assault.
NEISS-AIP data are publicly available and de-identified. Therefore, this study did not require institutional review board (IRB) approval.
Cases were dog bites of the lower extremity reported to the NEISS-AIP during 2005-2019. (The year 2019 was the most recent year for which data could be downloaded at the time of this study.) Cases were included if either the precipitating cause of injury or immediate cause of injury fields contained the code for “dog bite” and if either the primary body part affected or secondary body part affected fields contained a code for a lower extremity body part (knee, lower leg, ankle, upper leg, foot, toe). (The secondary body part affected field only began to be used in 2019.) The variables examined were year of treatment (three-year period), month of treatment (three-month period), patient age, patient gender, location where the injury occurred, disposition of the patient, diagnosis (type of injury), and affected body part.
Analyses were performed using Office Professional 2007 Access and Excel (Microsoft Corporation, Redmond, Washington, US). The distribution of cases and national injury estimates were determined for the variables. National injury estimates were calculated by summing the values in the Weight numeric field in the publicly available NEISS-AIP database, and 95% confidence intervals (CIs) were calculated for the estimates. The CPSC considers an estimate unstable and potentially unreliable when the number of records used is <20 or the estimate is <1,200.8 For those variable subgroups where the estimate was <1,200, 95% CIs were not calculated.
Results
There were a total of 18,357 dog bites of the lower extremity treated at a sample of US hospital EDs, resulting in a national estimate of 1,090,110 dog bites of the lower extremity. This represented 21.2% of the 5,151,538 estimated dog bites of any body part.
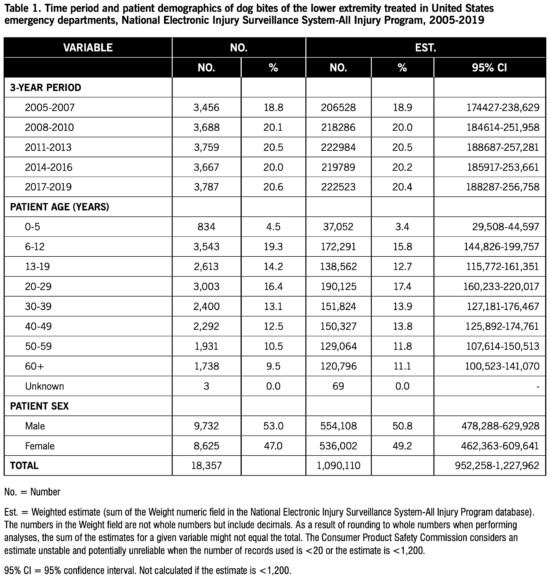
The number of dog bites tended to be stable over the study period (Table 1). By three-month period, the estimated number of dog bites of the lower extremity was 202,406 (18.6%, 95% CI 170,858-233,954) in November-January, 246,785 (22.6%, 95% CI 209,345-284,225) in February-April, 353,113 (32.4%, 95% CI 302,003-404,223) in May-July, and 287,806 (26.4%, 95% CI 245,027-330,585) in August-October. Patients age 0-29 years accounted for 9,993 (54.4%) of the cases and 538,030 (49.4%) of the estimated dog bites, and a slightly greater proportion of patients were male (Table 1). By location of the injury incident, the estimated number of dog bites of the lower extremity was 483,949 (44.4%, 95% CI 416,624-551,275) home/mobile home, 128,998 (11.8%, 95% CI 107,557-150,438) other public property, 98,736 (9.1%, 95% CI 81,653-115,819) street or highway, 31,429 (2.9%, 95% CI 24,834-38,024) place of recreation or sports/school/farm/ranch/industrial place, and 346,998 (31.8%, 95% CI 296,661-397,335) unknown.
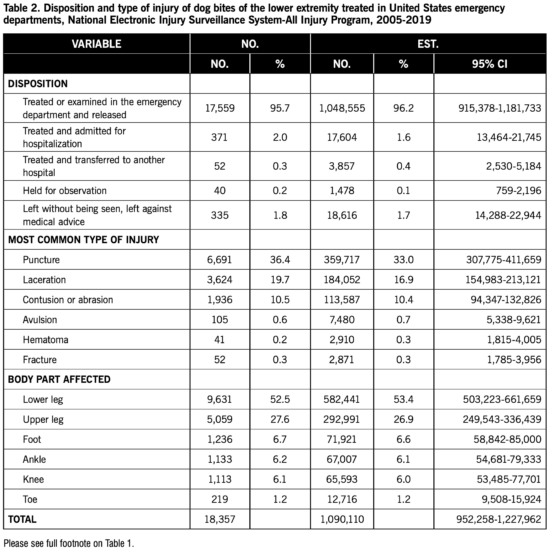
Table 2 presents the distribution of dog bites of the lower extremity by disposition, diagnosis, and affected body part. Most of the patients were treated or evaluated at the hospital ED and released. The most frequently reported diagnoses were puncture, laceration, and contusion or abrasion. The majority of dog bites involved the lower leg with the next most common body part being the upper leg.
 Discussion
Discussion
This study characterized dog bites of the lower extremity treated at US hospital EDs. As shown by the current and several previous studies, dog bites of the lower extremity account for 20-25% of all dog bites treated at US hospital EDs.4,5
The number of dog bites remained relatively stable during the 15-year period of the study. However, the AVMA reported that 2016 was the highest rate of dog ownership in the US since the AVMA began measuring in 1982; the rate increased from 36.1% in 2001 to 38.4% in 2016. Furthermore, the number of pet dogs in the US increased 10% since 2011.1 One study using data from the Healthcare Cost and Utilization Project (HCUP) Nationwide Emergency Department Sample (NEDS) distributed by the US Department of Health and Human Services Agency for Healthcare Research and Quality (AHRQ), a stratified sample of US hospital-owned EDs, reported that the prevalence of dog bites decreased during 2010-2014.9 Another study found the rate of dog bites increased during 2005-2011 and then declined to 2018.10 However, these latter two studies included all dog bites while the current study examined only dog bites of the lower extremity. A study of dog leash-related injuries of the lower extremity treated at US hospital EDs found that the number of injuries increased during 2000-2020.11 The difference in time trends between the present dog bite study and the dog leash-related study could be due to differences in data sources and the circumstances under which the two types of injuries occurred.
A seasonal pattern in dog bites of the lower extremity was observed; the highest proportion of dog bites was seen during May-July and the lowest during November-January. Another study of dog bites treated at US hospital EDs found dog bites were more common in the summer.3 It may be that, during warmer weather, people are more likely to be outside and active, thus more likely to be in circumstances that may lead to dog bites.
Patients with dog bites of the lower extremity tended to be younger, with roughly half being 29 years or less. In addition, only a slightly higher proportion of patients were male. These demographic patterns were similar to those observed in earlier dog bite studies. 4,5,9,12 In contrast, patients with dog leash-related injuries of the lower extremity tended to be older, and the majority were female.11
Most dog bites of the lower extremity with a known location of the incident occurred at home, with the next most common locations being other public property and street or highway. A previous study of all dog bites treated at US hospital EDs reported a similar pattern by incident location,3 as did the study of dog leash-related injuries of the lower extremity.11 This suggests that most dog bites involve family dogs or dogs known to the patient and not stray or unfamiliar dogs. Such information could be useful for educating the public on how to prevent dog bites.
The most common diagnoses were puncture, laceration, and contusion or abrasion, a pattern similar to earlier studies of all dog bites.4,5 The most frequently affected body parts were the lower leg followed by the upper leg. However, the most frequently reported diagnoses among dog leash-related injuries of the lower extremity were strain or sprain, fracture, and contusion or abrasion, and the most commonly affected body parts were the knee, ankle, and lower leg.11 The contrasts in the pattern of diagnosis and affected body part between the current study and the dog leash-related injury study could be due to differences in the circumstances in which the two types of injury occur.
Since the most frequently reported diagnoses might be considered to be relatively minor, it might be expected that the majority of patients would be treated or examined in the ED and released. This study did find that over 95% of the patients were treated or examined in the ED and released. Earlier studies of all dog bites treated at hospital EDs likewise found that the majority of patients were treated or examined and released from the ED.4,5,12
The results of this study do not explicitly indicate ways to prevent dog bites. However, recommendations have been made by others to reduce or prevent such injuries, particularly among children. Parents, particularly those with young children, should be educated to supervise their children when near dogs and to teach their children how to properly interact with dogs, such as not disturbing dogs while the animal is eating or sleeping or with its puppies, not reaching through or over a fence when a dog is on the other side, moving slowly around a dog, not being aggressive or rough when playing with a dog, asking permission from an owner before petting their dog, and not approaching unfamiliar dogs.13,14
This study has limitations. The NEISS-AIP collects data from a small sample of all US hospital EDs. However, it is possible to estimate the total number of injuries based on this sample.7 Furthermore, the NEISS-AIP database only includes injuries treated at a hospital ED. Studies that include information on dog bites of the lower extremity not evaluated at hospital EDs would provide a more complete view of dog bites.
In conclusion, the number of dog bites of the lower extremity remained relatively stable during 2005-2019. Dog bites were seasonal, with a higher proportion being reported during May-July. Patients tended to be younger, particularly age 29 years or less, and a slightly higher proportion were male. Most of the dog bites with a known incident location occurred at home. The majority of patients were treated or examined at the hospital ED and released. The most frequently reported diagnoses were puncture, laceration, and contusion or abrasion, and the most commonly affected body parts were the lower leg followed by the upper leg.
Considering the differences observed between dog bites and dog leash-related injuries of the lower extremity with regard to such factors as time trends, patient age and sex, and diagnosis and affected body part, this suggests that risk of dog-related injuries of the lower extremity depends on the exact type of the injury and the circumstances that lead to the injury. Thus, the particulars of a dog-related injury should be taken into account when trying to reduce the risk of such injuries.
Mathias B. Forrester, BS, is an independent researcher in Austin, Texas. Now retired, he previously performed public health research for various university and government programs for 34 years.
- American Veterinary Medical Association. AVMA Pet Ownership and Demographics Sourcebook. 2017-2018 Edition. American Veterinary Medical Association; Schamburg, Illinois, 2018.
- American Pet Products Association. Pet industry market size, trends & ownership statistics. Available at: https://www.iii.org/fact-statistic/facts-statistics-pet-ownership-and-insurance. Accessed September 1, 2022.
- World Health Organization. Animal bites. February 5, 2018. Available at https://www.who.int/news-room/fact-sheets/detail/animal-bites. Accessed September 1, 2022.
- Loder RT. The demographics of dog bites in the United States. Heliyon. 2019;5(3):e01360.
- Gilchrist J, Gotsch K, Annest JL, Ryan G. Nonfatal dog bite-related injuries treated in hospital emergency departments – United States, 2001. MMWR Morb Mortal Wkly Rep. 2003;52(26):605-610.
- Ehlman DC, Haileyesus T, Lee R, Ballesteros MF, Yard E. Evaluation of the National Electronic Injury Surveillance System – All Injury Program’s self-directed violence data, United States, 2018. J Safety Res. 2021;76:327-331.
- United States Department of Health and Human Services. Centers for Disease Control and Prevention. National Center for Injury Prevention and Control, and U.S. Consumer Product Safety Commission. National Electronic Injury Surveillance System All Injury Program, 2019. Inter-university Consortium for Political and Social Research [distributor], December 15, 2021.
- United States Consumer Product Safety Commission. National Electronic Injury Surveillance System (NEISS). Available at https://www.cpsc.gov/Research–Statistics/NEISS-Injury-Data/Explanation-Of-NEISS-Estimates-Obtained-Through-The-CPSC-Website. Accessed September 1, 2022.
- Holzer KJ, Vaughn MG, Murugan V. Dog bite injuries in the USA: Prevalence, correlates and recent trends. Inj Prev. 2019;25(3):187-190.
- Tuckel PS, Milczarski W. The changing epidemiology of dog bite injuries in the United States, 2005-2018. Inj Epidemiol. 2020;7(1):57.
- Forrester MB. Dog leash-related injuries of the lower extremity treated at hospital emergency departments. Lower Extremity Review. 2022;14(6): 41-42,45,47,49.
- Holmquist L, Elixhauser A. Emergency department visits and inpatient stays involving dog bites, 2008. November 2010. Rockville, Md.: Agency for Healthcare Research and Quality; 2010. Available at http://www.hcup-us.ahrq.gov/reports/statbriefs/sb101.pdf. Accessed September 1, 2022.
- Dixon CA, Mistry RD. Dog bites in children surge during Coronavirus Disease-2019: A case for enhanced prevention. J Pediatr. 2020;225:231-232.
- Parente G, Gargano T, Di Mitri M, Cravano S, Thomas E, Vastano M, Maffi M, Libri M, Lima M. Consequences of COVID-19 lockdown on children and their pets: Dangerous increase of dog bites among the paediatric population. Children. 2021;8(8):620.








