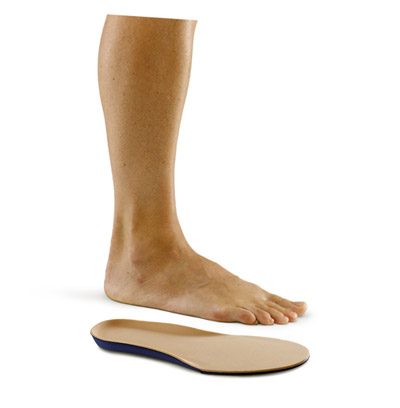
 Diabetic feet need pampering and protection from microtrauma, but they also need stability and support. A diabetic insole, representing the ultimate middle ground between sock and shoe, should offer the best of all worlds: cushioning, structure, shock absorption, and durability.
Diabetic feet need pampering and protection from microtrauma, but they also need stability and support. A diabetic insole, representing the ultimate middle ground between sock and shoe, should offer the best of all worlds: cushioning, structure, shock absorption, and durability.
By Shalmali Pal
Gary M. Rothenberg, DPM, CDE, CWS, would describe himself as an insole man.
“I tend to be much more concerned about insoles than I am about shoes,” said Rothenberg, attending podiatrist and director of residency training at the Miami VA Healthcare System. “The insole is the contact point between the foot and the rest of the world. I’m usually all right with an off-the-shelf shoe that can accommodate the insole that I’ve prescribed.”
Needless to say, if it were up to most patients, that “contact point” would be as soft and comforting as possible. But diabetic patients, and those with neuropathy in particular, need an insole that can offer the best of all worlds: cushioning, structure, shock absorption, and durability.
Materials and configuration
For optimal compressibility and density, the properties of the insole material closest to the skin should be similar to those of human skin, according to Roy H. Lidtke DPM, CPed, FACFAOM, associate professor of podiatric medicine and surgery at Des Moines University in Iowa and director of the Center for Clinical Biomechanics at St. Luke’s Hospital in Cedar Rapids, IA.
“A plastazote with a Shore A20 compressibility factor is very close to skin. But…the soft material is going to compress quickly. What you want is multidensity layering so that the insole lasts longer and you get the best of both worlds,” added Lidtke, who is also an assistant professor of internal medicine, section of rheumatology, at Chicago’s Rush University Medical Center.
The best of both worlds means some combination of a variety of materials that perform a variety of functions. (see table).
For Bill Meanwell, CPed, founder, CEO, and director of the International School of Pedorthics in Broken Arrow, OK, all worthwhile insoles will have a minimum of three specific materials:
1. Plastazote P-cell top cover
Plastazote and P-cell are self-pressure mapping and are designed to relieve pressure points during normal wear. Even distribution of plantar pressures is important in the diabetic foot because areas of elevated peak plantar pressures tend to be prone to ulceration; pressure gradients (steep increases in pressure over a small surface area) can also increase friction and, subsequently, the risk of calluses and ulcers. Another benefit of these topcover materials is that the closed cell construction is resistant to bacteria; patients with diabetes are less resistant than healthy subjects to infection, which can complicate an ulceration or lead to cellulitis in the absence of ulceration.
2. Polyurethane foam
A layer of polyurethane offers tremendous shock absorption. This can help attenuate any aforementioned areas of peak pressure and can also help to compensate for limited range of motion (particularly ankle dorsiflexion), which is common in patients with diabetes. Such limited range of motion can impair a diabetic patient’s ability to smoothly transition through the phases of gait and, consequently, the ability to absorb shock at points of impact. By absorbing the shock, the polyurethane foam layer protects the foot from unnecessary stress while in motion.
3. EVA (ethylene vinyl acetate)
A bottom layer of 35-45 durometer will offer some “guts” to the whole thing, Rothenberg said. Insole stability helps decrease plantar pressures and shear forces, cocooning the foot against lesions such as calluses and ulcers. Stability also helps improve postural control, which can be impaired in patients with diabetes and particularly in those with neuropathy; poor postural control increases a patient’s risk of falling.
Rothenberg’s insole development process begins with a comprehensive exam: A neurological exam, a vascular exam, a dermatological exam, and a musculoskeletal exam.
“The musculoskeletal portion of the exam is key for deciding what type of insoles,” he said. “So if a patient has a callus or a healed ulcer because of a hammertoe or a plantar flexed metatarsal, we may chose to offload or pocket out the insert based on the history of the deformity. So deformity is the major predictor of the type of insole that I go for.”
Off-the-shelf vs custom
Patients with significant changes in foot architecture and deformities, brought on by autonomic or motor neuropathic changes for example, will need custom orthotic devices. But that’s a minority of the diabetic patient population, according to the experts.
“The A5513 is needed occasionally,” Meanwell said, referring to the Healthcare Common Procedure Coding System (HCPCS) used to obtain Medicare reimbursement for custom insoles. “The problem that we have in our industry is that we get paid more for the custom device than the OTS (off the shelf). You are thinking with your wallet and not with your head.”
Marybeth Crane, MS, DPM, FACFAS, CWS, managing partner of Foot and Ankle Associates of North Texas in Grapevine, also stressed that a heat moldable OTS is suitable for the majority of patients. A properly fitted shoe with a moldable insole should be sufficient, she said.
“There are very strict guidelines that (insoles) have to meet for reimbursement ” she said. “Beyond that, they have to be comfortable, they have to be soft, and they have to actually fit the patient’s foot. You can make small accommodations — adding a metatarsal pad, adding a heel lift, adding a reverse Morton’s extension — very quickly can be done to an OTS device.”
These types of accommodations can address a multitude of issues in the diabetic foot, such as a forefoot valgus deformity and excessive plantar pressure during gait. The ultimate goal is to alleviate loading in key areas of the foot, alleviate pain, and reduce the potential for soft tissue damage.
Rothenberg added that he sees very few indications for custom shoes, such as Charcot arthropathy or patients with partial foot amputations. But more often than not, he said he is able to get such patients into an OTS shoe paired with a heat moldable OTS insole.
“If they bring in a reasonable shoe that they purchased at a WalMart or Kmart, then I can at least get them the right insole,” he said, adding, “I practice in South Florida, so my bigger battle is getting patients to give up their flip-flops!”
Neuropathy
Insoles are often prescribed to reduce elevated plantar pressure because the latter is associated with a risk of foot ulcer development in the neuropathic foot. Published data on the effectiveness of insoles for preventing ulceration is available but not always entirely reliable, according to a systematic review done at the University of Plymouth in the UK and published in the 2011 Journal of Diabetes and its Complications.
Joanne Paton, PhD, a lecturer in podiatry at the university, and colleagues culled 342 papers on the topic, but they narrowed that down to five that met their inclusion criteria: Published inception as of 2008 and published follow-up. The studies could have been randomized or non-randomized controlled studies (see Table 2). Two studies looked at plastazote-based casted insoles, with one assessing ulcer relapse rate (Ucciloi) and the other reduction in peak pressure (Mohamed). One trial investigated the effect of an EVA and polyethylene foam insole on peak pressure (Lobmann) while another evaluated the effective of magnetic insoles in reducing neuropathic pain (Weintraub). The last study looked at the effect of a TL-2100 graphite casted insole on peak pressure and contact surface area (Albert).
Paton’s group concluded that, based on the collective results of all five studies, insoles appeared to be useful for preventing neuropathic diabetic foot ulcers, reducing peak pressure under the first metatarsal head region by 20% to 30%. However, as other researchers have noted, it is much easier to find evidence in the diabetic foot care literature demonstrating plantar pressure reduction with footwear and insoles than proof that these effects actually affect ulceration rates. In the University of Plymouth review, only one study (Uccioli) used ulcer relapse as an outcome. Patients in that study who used an insole with a therapeutic shoe had a 27.7% relapse rate while the control group had a 58.3% relapse rate (wearing non-therapeutic shoes and no insoles).
But Paton’s group also noted that all but four of the studies suffered from poor methodology (Weintraub was the exception). Weaknesses included a lack of generalizability, potential for bias because patients were not blinded to the interventions used, and lack of randomization. They called on the diabetic healthcare community to produce more comprehensive studies.
“The evidence suggests insoles are effective in reducing plantar loads under the diabetic neuropathic foot,” she said. “In practice, where the treatment aim is to reduce plantar pressure to an area, insoles may be of benefit… It is not clear at this stage if insoles are effective in reducing ulceration rates and we do not recommend they are used in isolation but rather as part of the ulceration prevention strategy.”
A study out of the Netherlands supports that recommendation. In a 2004 paper in Clinical Biomechanics, researchers from the University ofAmsterdam found that custom-made insoles were more effective than flat insoles in off-loading the first metatarsal head region, but that this off-loading varied considerably between individual patients.
Insole education
Paton’s study stressed that insoles required frequent review and replacement to remain useful. The experts LER spoke with said they recommended that insoles be changed, at a minimum, three times a year, which is the number of insoles allowable under Medicare’s Therapeutic Shoe Bill. Some patients may prefer to obtain all three pairs at once and then swap them out on a regular basis. Others will go for one pair at a time.
Ribotsky has the expiration date put on an insole as a reminder of those thrice-yearly exchanges for his patients who are eligible for the TSB program.
“I also send out automatic e-mails that remind people to change their insoles,” he said.
Rothenberg, who serves as the chair of the foot care specialty practice group for the American Association of Diabetes Educators, said that his group sees the high-risk patients on a quarterly basis, which is a prime opportunity to change the insoles. Some patients also prefer to obtain all three pairs upfront so that they can rotate them throughout the year, he added.
Patients with diabetes who are not covered by the TSB, however, may be able to go longer between insole replacements without significantly affecting plantar pressure attenuation, according to another study from Paton’s group at the University of Plymouth. Their insole durability study, presented in September at the International Foot & Ankle Biomechanics (iFAB) conference, found that although the cushioning materials in an insole do compress significantly during the first six months of wear, peak plantar pressures are not significantly affected for at least six more months.
Materials for insoles
Open-cell construction
- Polyurethane foam (latex)
- Microcellular rubber
- Polyvinyl chloride (PVC)
Closed-cell construction
- Polyethylene foam (plastazote)
- Neoprene
Ethylene vinyl acetate (EVA)
Other
- Ortho felt
- Leather
- Charcoal
- Bamboo
Five studies included in systematic review
Albert S, Rinoie C, Effect of custom orthotics on plantar pressure distribution in the pronated diabetic foot, Journal of Foot and Ankle Surgery 33:6, 598-604, 1994
Ucciloi L, Fagia E, et al. Manufactured shoes in the prevention of diabetic foot ulcers, Diabetic Care 18:10, 1376-1378, 1995
Lobmann R, Kayser R, et al. Effects of preventative footwear on foot pressure as determined by pedobarography in diabetic patients: A prospective study, Diabetic Medicine 18:4, 314-319, 2001
Weintraub M, Wolfe G, et al. Static magnetic field therapy for symptomatic diabetic neuropathy: A randomized, double-blind, placebo-controlled trial, Archives of Physical Medicine & Rehabilitation 84:5, 736-746, 2003
Mohamed O, Cerny K, et al. The effects of Plastazote and Aliplast/Plastazote orthoses on plantar pressures in elderly persons with diabetic neuropathy, Journal of Prosthetics & Orthotics 16:2, 55-65, 2004
Sponsored by an educational grant from Dr. Comfort








1978 – a few leaders in the pedorthic profession recognized that total contact, even weight distribution, accomodative orthoses would help prevent diabetic ulcerations and reduce the risk of recurring ulcerations. These were made by direct mold process using 1/4″ pink (soft) plastazote full foot over 1/4″ white (firm) plastazote to the sulcus. The orthotic device was placed inside proper designed, controlling, and fitted footwear (not WalMart or Kmart), and the patient was instructed to wear the footgear for 4 weeks. At that time, the soft plastazote fully compressed dynamically, pressures were easily detectable, any additional modifications added, and a full length layer of 1/8″ PPT added to the bottom of the device. Any necessary modifications to the footwear was also performed. The orthotic device would last an average of ONE YEAR. These pioneering pedorthists created the model for todays modern diabetic footgear. Thank you to all that contributed to this model.
The OTS inserts may be fine for the average diabetic foot that does not show apperances of high plantar pressure areas. And, there is no way an OTS diabetic insert can supply accurate even weight distribution. Even customized with additional metatarsal pads or forefoot wedging, the OTS will not protect pressures nearly as well as a custom molded total contact device. Total contact means “total” contact. This is key to unloading high pressure areas. And where do most plantar ulcerations occur? In the forefoot region….metatarsal heads and digits. This is how the early diabetic inserts designed as mentioned will fill up the space between the metatarsal heads and naturally create a toe crest to help unload digit tip pressures.
Why provide a patient with an OTS insole that compromises? What is more important to you and your patient…..money or the patients well being? It’s their choice… and yours.