 Physical impairments associated with femoroacetabular impingement include limited range of motion, muscle weakness, and altered biomechanics. Attention to these areas during rehabilitation can improve surgical outcomes and may even reduce the risk of osteoarthritis.
Physical impairments associated with femoroacetabular impingement include limited range of motion, muscle weakness, and altered biomechanics. Attention to these areas during rehabilitation can improve surgical outcomes and may even reduce the risk of osteoarthritis.
By Jerrad R. Guenther, BSc, Michael K. Gilbart MD, FRCS(C), MEd, and Michael A. Hunt PT, PhD
Femoroacetabular impingement (FAI) in the hip is a condition that can lead to symptoms of pain and physical dysfunction and may be associated with the development of labral tears or chondral damage within the hip. FAI is quite prevalent and typically presents in active young and middle-aged adults aged between 20 and 50 years.1 Prevalence estimates from multiple studies have reported the number of people with radiographic evidence of FAI is as high as 39% in an asymptomatic population.2-4
Given the proposed alterations in joint biomechanics and known associations with secondary damage to the hip (labrum, cartilage) in the presence of FAI, researchers have suggested it as a strong risk factor for development of early onset hip osteoarthritis (OA).5,6 As a result, research into the causes, functional impairments, and treatment of FAI has increased dramatically in the past few years.
Types of FAI
FAI can occur on the acetabular side of the hip (pincer impingement), the femoral side of the hip (cam impingement), or it can occur on both the acetabulum and proximal femur (combined impingement). Pincer-type FAI occurs when there is excessive acetabular bony over-coverage, typically anteriorly or laterally. Cam-type FAI occurs when there is an abnormal femoral head-neck offset, or increased bone at the femoral head-neck junction. These bony changes are typically anterior and lateral, which causes impingement when the hip is brought into positions requiring large amounts of flexion. In a recent epidemiological study of 1076 individuals with FAI (55% women), researchers reported that 47.6% of hips had a diagnosis of cam-type FAI, 44.5% had combined cam/pincer-type FAI, and 7.9% had pincer-type FAI.7
FAI diagnosis
The diagnosis of FAI includes both a clinical examination of the patient and an evaluation of radiographic images. Patients with FAI often present with pain in the anterior and lateral aspect of the groin, and less commonly they may have posterior hip pain. This pain is often worse with activity, especially with hip flexion, and many patients have pain with sitting for prolonged periods. FAI can lead to tears of the hip acetabular labrum and to acetabular chondral damage, which is usually the source of pain and discomfort for patients. Patients will often indicate the location of their pain by a positive “C” sign, which is performed when a patient grabs the anterior aspect of the groin with the index finger and the posterior hip region with the thumb of the same hand.
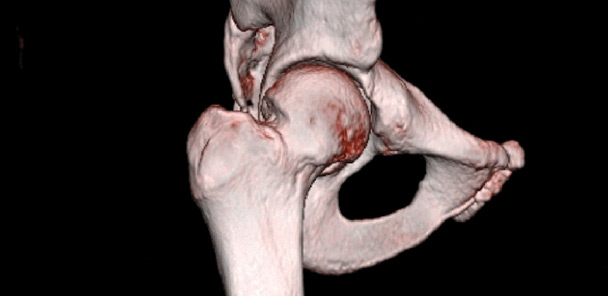
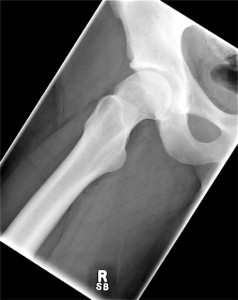
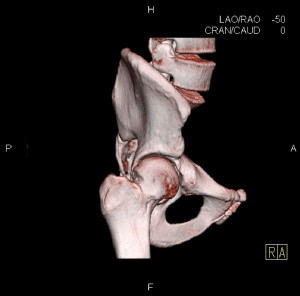
The diagnosis of FAI is largely confirmed through assessment of radiographs. The radiographic assessment for FAI should include an anteroposterior (AP) pelvis, and AP and lateral views of the affected hip, including a Dunn view. The AP pelvis radiograph is used to assess for pincer-type FAI. The Dunn view, which evaluates the anterolateral aspect of the femoral head-neck junction, should be performed for cam-type FAI (Figure 1). The alpha angle is a measure of the prominence of the cam-type FAI lesion, and is abnormal if it is greater than 50º to 55º.8,9 This can be measured using the Dunn view radiograph or oblique sagittal magnetic resonance (MR) images. Clinicians should order an MR arthrogram of the hip for most patients who present with hip and groin pain, have positive impingement signs, and are positive on radiograph. An MR arthrogram, in which gadolinium contrast is injected into the joint, will allow for the diagnosis of labral tears and may indicate the presence of chondral pathology within the hip.10 The alpha angle for cam-type FAI can also be measured from this MRI. A CT scan with 3D reconstructions may be used by surgeons to preoperatively evaluate cam and pincer lesions to assist with surgical planning (Figure 2). This technique provides great imaging of the impinging lesions prior to surgical intervention, but does subject the patient to a higher radiation dose compared with x-ray.
Surgical treatment
Patients who do not respond to conservative treatment and have ongoing pain and symptoms associated with FAI are candidates for surgical intervention. Surgery for this condition has been described using either an open or an arthroscopic technique. Successful surgical correction relies on the correction of the bony abnormality that caused the labral and chondral pathology.
The arthroscopic technique avoids the need to make such a large surgical incision and approach, but relies on adequate arthroscopic visualization. The surgical technique involves an acetabular osteoplasty, or rim trimming for pincer-type FAI.11,12 The labrum is then refixed to the anterior acetabular rim using sutures and anchors.13 The cam-type FAI is managed by performing a femoral osteochondroplasty,11 which involves burring and removal of the femoral impinging bone (Figure 3).12
Physical impairments associated with FAI
Range of motion. In an impinged hip, the contact between a widened femoral neck, an abnormally shaped or oriented acetabulum, or both typically results in decreased range of motion (ROM) of the joint. Specifically, motions requiring hip flexion in combination with adduction and internal rotation, such as getting into a low vehicle, are most frequently affected in those with FAI and result in the most consistent reports of pain.5
A recent study comparing individuals with FAI to asymptomatic cases and controls showed significant differences related to ROM. In particular, those with FAI showed 10% less passive hip flexion, 40% less passive internal rotation, and 25% less passive external rotation than age-matched healthy controls.14 Additionally, our laboratory collected ROM for 60 people with and without FAI (30 per group) and found that those with FAI demonstrated significantly less active ROM for active hip flexion, extension, abduction, adduction, and internal and external rotation when compared with healthy age-matched controls (unpublished data).
Currently, surgery is the only treatment shown to improve hip ROM associated with FAI. Specifically, researchers have found that surgery to remove the bony conflict between the femoral neck and the acetabulum significantly increases active hip flexion by 7% to 11%15,16 and internal rotation by 48% to 56%15,16 in people with FAI at a mean follow up of 30 months. It is important to restore the hip ROM by reducing or removing painful symptoms, especially near the end of terminus range, for people with FAI to return fully to sporting activities.
Muscle weakness. The muscles of the hip have a multitude of functions. In particular, they provide stability for the hip joint, and initiate movement for dynamic weight-bearing activities including walking, running, and squatting. As a ball and socket joint, the hip joint experiences movements in all three planes of motion, with sagittal plane movements (flexion and extension) undergoing the largest range. Hip muscle weakness is prevalent in people with FAI, and is associated with pain and impaired muscle activation as shown using electromyography, specifically during hip flexion.17

Figure 3. Intraoperative picture (left) and fluoroscopic image (right) of patient with treatment of cam-type FAI.
There are very few published data comparing hip muscle strength in people with and without FAI. The limited number of studies in the area, however, support the notion of widespread muscle weakness in people with FAI. Casartelli and colleagues assessed hip muscle strength in 22 individuals with FAI and 22 controls matched for gender, age, and body mass and showed those with FAI exhibited significantly lower maximal voluntary contraction (MVC) strength than controls during hip flexion (26%), abduction (11%), adduction (28%), and external rotation (18%).17 A more recent study confirmed these findings and showed additional weakness of the hip extensors and internal rotators. Specifically, in our cohort of 30 people with FAI and an equal number of people without the condition, we showed those with FAI had significantly lower MVC strength than controls during hip flexion (25%), abduction (18%), adduction (13%), extension (18%), internal rotation (26%), and external rotation (14%).18
Researchers believe that weak hip muscles lead to reduced hip motion and instability within the hip joint,19 which can cause hip pain. More importantly, as indicated above, instability and altered joint contact forces in a hip with FAI may play a role in the early development of hip osteoarthritis.5 As a result, treatment approaches that can effectively restore muscle function and biomechanics to near-normal levels in an impinged hip represent an important component of overall clinical management.
There is no published research on the effectiveness of a muscle-strengthening program in people with FAI. However, in a study of patients with a similar pathology,12 63 individuals scheduled for total hip arthroscopy (THA) were randomized to either a preoperative exercise group or an education group. Participants in the experimental group exercised three times a week over a six-week period prior to surgery, and the intervention was delivered in two phases. In the first phase, participants performed one or two sets of eight to 12 repetitions of single joint movements in a pool, which then progressed at four weeks into the second phase. The second phase incorporated two sets of eight to 12 repetitions of land-based exercises that included a leg press, chest press, and seated row, along with three more upper body exercises and one core exercise.
Those who were enrolled in the preoperative muscle strengthening intervention reported an 18% improvement in lower body muscle strength, improved or stabilized WOMAC (Western Ontario and McMaster Universities Osteoarthritis Index) function and pain scores, and improved SF (Short Form)-36 physical function scores.20 These positive results provide support for the use of muscle strengthening in an FAI population. Research in area as part of a preoperative or standalone treatment for FAI is urgently needed.
Altered biomechanics. Given the known strength and range of motion impairments associated with FAI, it is not surprising that alterations in normal movement patterns are commonly observed in this patient group. Indeed, analysis of functional movement patterns is an integral component of the initial clinical assessment, and findings usually dictate the course of clinical management. However, despite the importance of movement analysis, very little has been published in this area.
Kennedy et al published the first report of differences in gait characteristics between those with (n = 17) and without (n = 14) FAI, and showed that those with FAI exhibited reduced frontal plane range of motion at the hip joint and the pelvis.21 A more recent study showed that, compared with healthy individuals (n = 30), those with FAI (n = 30) walked significantly more slowly and exhibited less peak hip extension, adduction, and internal rotation (effect sizes ranging from .48 to 1).22
This study also reported for the first time that those with FAI experience different hip joint loading patterns than those without painful FAI, as evidenced by 17% lower external hip flexion moments and 25% lower external rotation moments. These differences suggest that those with FAI likely compensate at either distal or proximal segments in an attempt to reduce the magnitude of the internal forces applied to the hip joint. The effects of these potential compensations on the distribution of loads, however, are unclear.
Two studies have compared joint kinematics and kinetics during walking before and after arthroscopic debridement surgery for FAI. Rylander et al tested 11 individuals one month preoperatively and one year postoperatively and showed a significant increase in sagittal plane hip joint range of motion, which was driven by a 3° increase in peak hip flexion following surgery.23 This increase approaches normal ROM reported in other studies,22,24 but, unfortunately, the study had no control group. In contrast, Brisson and colleagues tested 10 patients with unilateral cam impingement and showed that overall gait biomechanics did not return to normal an average of 21 months following surgery.24 Specifically, among the kinematic and kinetic outcomes at each of the lower limb joints, only knee joint sagittal range of motion values were similar to a healthy comparison group following surgery.
These findings suggest that surgical resection and postoperative rehabilitation alone do not significantly normalize gait biomechanics and provide a rationale for targeted gait modification as part of the rehabilitative process.
Future directions
The recent increase in attention paid to FAI both clinically and in research has driven new findings related to the pathology and treatment of this disorder. However, much is still unknown. Though the studies summarized above provide a solid overview of the physical impairments expected during single plane range of motion or strength tests as well as during walking, there is still little known about the biomechanics of more functional movements (such as stair climbing, squatting, or lunging) that people with FAI typically have difficulty performing (see Lamontagne et al25 for a description of hip and pelvis biomechanics during a maximum squat).
Additionally, the pattern and extent of changes in hip muscle activation in people with FAI during these functional activities remains largely unknown. Furthermore, due to the cross-sectional nature of studies on FAI, it is currently unknown whether strength deficits precede the onset of FAI or rather, are a result of FAI.
Finally, though surgery remains the predominant choice for treatment for people with FAI, there is still sparse literature detailing the effects of other treatments. Given the high prevalence, wide range of clinical and biomechanical effects of FAI, and the suggested link to early development of hip OA, more research is urgently needed to help guide effective clinical management of this pathology.
Jerrad R. Guenther, BSc, is a graduate student in the Department of Physical Therapy at the University of British Columbia (UBC) in Vancouver, Canada. Michael K. Gilbart MD, FRCS(C), MEd, is an orthopedic surgeon at the UBC Vancouver Hospital and an assistant professor at the University of British Columbia. Michael A. Hunt, PT, PhD, is an assistant professor in the Department of Physical Therapy at the University of British Columbia.
1. Leunig M, Beaulé PE, Ganz R. The concept of femoroacetabular impingement: current status and future perspectives. Clin Orthop Relat Res 2009;467(3):616-622.
2. Hack K, Di Primio G, Rakhra K, Beaulé PE. Prevalence of cam-type femoroacetabular impingement morphology in asymptomatic volunteers. J Bone Joint Surg Am 2010;92(14):2436-2444.
3. Gosvig KK, Jacobsen S, Sonne-Holm S, et al. Prevalence of malformations of the hip joint and their relationship to sex, groin pain, and risk of osteoarthritis: a population-based survey. J Bone Joint Surg Am 2010;92(5):1162-1169.
4. Leunig M, Jüni P, Werlen S, et al. Prevalence of cam and pincer-type deformities on hip MRI in an asymptomatic young Swiss female population: a cross-sectional study. Osteoarthritis Cartilage 2013;21(4):544-550.
5. Ganz R, Parvizi J, Beck M, et al. Femoroacetabular impingement: a cause for osteoarthritis of the hip. Clin Orthop Relat Res 2003;(417):112-120.
6. Beck M, Kalhor M, Leunig M, Ganz R. Hip morphology influences the pattern of damage to the acetabular cartilage: femoroacetabular impingement as a cause of early osteoarthritis of the hip. J Bone Joint Surg Br 2005;87(7):1012-1018.
7. Clohisy JC, Baca G, Beaulé PE, et al. Descriptive epidemiology of femoroacetabular impingement: a North American cohort of patients undergoing surgery. Am J Sports Med 2013;41(6):1348-1356.
8. Nötzli HP, Wyss TF, Stoecklin CH, et al. The contour of the femoral head-neck junction as a predictor for the risk of anterior impingement. J Bone Joint Surg Br 2002;84(4):556-560.
9. Beaulé PE, Zaragoza E, Motamedi K, et al. Three-dimensional computed tomography of the hip in the assessment of femoroacetabular impingement. J Orthop Res 2005;23(6):1286-1292.
10. Kennedy AA, Rosenfeld SB. Orthopedic perspectives on femoroacetabular impingement. Pediatr Radiol 2013;43 Suppl 1:S83-S89.
11. Philippon MJ, Schenker ML. A new method for acetabular rim trimming and labral repair. Clin Sports Med 2006;25(2):293-297.
12. Philippon MJ, Stubbs AJ, Schenker ML, et al. Arthroscopic management of femoroacetabular impingement: osteoplasty technique and literature review. Am J Sports Med 2007;35(9):1571-1580.
13. Kelly BT, Weiland DE, Schenker ML, Philippon MJ. Arthroscopic labral repair in the hip: surgical technique and review of the literature. Arthroscopy 2005;21(12):1496-1504.
14. Audenaert E, Van Houcke J, Maes B, et al. Range of motion in femoroacetabular impingement. Acta Orthop Belg 2012;78(3):327-332.
15. Siebenrock KA, Schoeniger R, Ganz R. Anterior femoro-acetabular impingement due to acetabular retroversion. Treatment with periacetabular osteotomy. J Bone Joint Surg Am 2003;85-A(2):278-286.
16. Eijer H, Myers SR, Ganz R. Anterior femoroacetabular impingement after femoral neck fractures. J Orthop Trauma 2001;15(7):475-481.
17. Casartelli NC, Maffiuletti NA, Item-Glatthorn JF, et al. Hip muscle weakness in patients with symptomatic femoroacetabular impingement. Osteoarthritis Cartilage 2011;19(7):816-821.
18. Guenther JR, Gilbart MK, Hunt MA. People with femoroacetabular impingement exhibit altered frontal and transverse plane strength, movement, and gait characteristics compared to those without impingement. Osteoarthritis Cartilage 2012;20(Suppl 1):S103-S104.
19. Retchford TH, Crossley KM, Grimaldi A, et al. Can local muscles augment stability in the hip? A narrative literature review. J Musculoskelet Neuronal Interact 2013;13(1):1-12.
20. Rooks DS, Huang J, Bierbaum BE, et al. Effect of preoperative exercise on measures of functional status in men and women undergoing total hip and knee arthroplasty. Arthritis Rheum 2006;55(5):700-708.
21. Kennedy MJ, Lamontagne M, Beaulé PE. Femoroacetabular impingement alters hip and pelvic biomechanics during gait: Walking biomechanics of FAI. Gait Posture 2009;30(1):41-44.
22. Hunt MA, Guenther JR, Gilbart MK. Kinematic and kinetic differences during walking in patients with and without symptomatic femoroacetabular impingement. Clin Biomech 2013;28(5):519-523.
23. Rylander JH, Shu B, Andriacchi TP, Safran MR. Preoperative and postoperative sagittal plane hip kinematics in patients with femoroacetabular impingement during level walking. Am J Sports Med 2011;(39 Suppl):36S-42S.
24. Brisson N, Lamontagne M, Kennedy MJ, Beaulé PE. The effects of cam femoroacetabular impingement corrective surgery on lower-extremity gait biomechanics. Gait Posture 2013;37(2):258-263.
25. Lamontagne M, Kennedy MJ, Beaulé PE. The effect of cam FAI on hip and pelvic motion during maximum squat. Clin Orthop Relat Res 2009;467(3):645-650.








Great Article. Very well written and informative. I didn’t know much about this subject so it was nice to be educated about a very important area of the body.