 By Munira M. Al Mahrouqi, PT, PhD; Bill Vicenzino, PT, PhD; David A. MacDonald, PT, PhD; and Michelle D. Smith, PT, PhD
By Munira M. Al Mahrouqi, PT, PhD; Bill Vicenzino, PT, PhD; David A. MacDonald, PT, PhD; and Michelle D. Smith, PT, PhD
Falls and falls-related injuries are a problem in individuals with chronic ankle symptoms.
Falls are a significant health concern especially among older adults. While falls are associated with osteoarthritis (OA) and persistent pain at the hip and knee, falls have not been investigated in people with chronic ankle symptoms. According to qualitative research on individuals with ankle OA, this population has concerns about falling and reports instability as a key symptom of their condition. Thus, this study aimed to compare self-reported history of falls between adults with and without chronic ankle symptoms. Secondary aims were to compare concern about falling and balance confidence between groups, and to identify factors associated with falling.
Methods
A total of 226 individuals (134 with chronic ankle pain and/or stiffness and 92 controls) participated in this cross-sectional case-control study. Inclusion criteria included ankle joint pain rated as ≥ 2 out of 10 on an 11-point numerical rating scale (NRS) anchored with the ‘No pain’ at 0 and ‘Worst pain imaginable’ at 10, and/or stiffness or reduced movement of ankle in the morning on most days for > 3 months.
Using an online questionnaire, participants provided information on their age, sex, function, comorbid health conditions, ankle pain severity, and pain in bodily locations. Falls in the last 12 months was determined by the question: “In the last 12 months, have you had any falls?” The Falls Efficacy Scale-International (FES-I) was used to measure concern about the possibility of falling when performing 16 different physical and social activities. The Activities-Specific Balance Confidence (ABC) scale was used to measure balance confidence during activities of daily living. The 21-item Activities of Daily Living subscale of the Foot and Ankle Ability Measure (FAAM-ADL) was used to assess function. Severity of ankle pain was measured using an 11-point NRS with 0 anchored with “no pain” and 10 anchored with “worst pain imaginable”. A modified version of the Self-Administered Comorbidity Questionnaire was used to collect data on multimorbidity.
Results
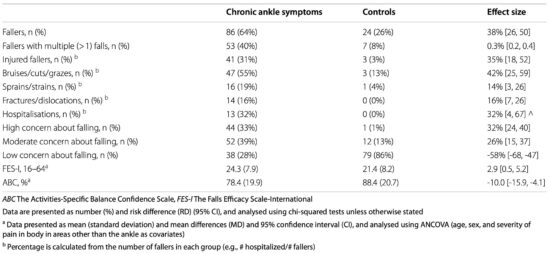
There were 186 falls reported among the chronic ankle symptoms group and 34 falls reported by controls. In the chronic ankle symptoms group, there were significantly more fallers (64%; n = 86) (individuals with 1 or more falls; p < 0.001), more participants who reported multiple (> 1) falls (p = 0.005), and more participants who sustained an injury from falling (p = 0.002) than the control group (26%; n = 24) (Table 1). Twenty-seven percent of participants (n = 60) reported more than 1 fall. The most reported injury type was bruises, cuts, and grazes (46%). All injury types, including serious injuries (eg, fractures/dislocations) and hospitalizations, were more common in fallers with ankle symptoms than fallers in the control group.
Participants with chronic ankle symptoms were 32% more likely to report high concern about falling, and 26% more likely to report moderate concern, than the control group. There were small effect sizes for higher concern about falling (FES-I; SMD (95% CI) = 0.4 (0.1, 0.6; p = 0.017) and lower balance confidence (ABC scale; SMD (95% CI) = 0.5 (0.8, 0.2); p = 0.001) in participants with ankle symptoms compared to controls (Table 1). Fallers had greater concern about falling and were more likely to have chronic ankle symptoms than non-fallers.
 Discussion
Discussion
The data indicate that falls, and becoming injured or hospitalized because of a fall, are more prevalent in individuals with chronic ankle symptoms than those without. Individuals with chronic ankle symptoms had a greater concern about falling and lower balance confidence than controls. Among the participants, falls status was related to concern about falling and whether an individual had chronic ankle symptoms.
Impairments in muscle strength, ankle range of motion, balance, and ambulatory function have been identified in individuals with chronic ankle symptoms. As these characteristics have been linked to falls in other populations, it is possible that they may contribute to an increased risk of falling in individuals with chronic ankle symptoms. Many health conditions reported by the participants with ankle symptoms, such as back pain and depression, are associated with an increased risk of falls. Research has identified a relationship between the number of falls risk factors an individual possesses and increased risk of falling.
Exercise management may address risk factors such as impaired balance and ankle muscle weakness, that are common in people with chronic ankle problems. Implementation of cognitive-behavioral therapies to reduce concern about falling and improve self-efficacy has been shown to be effective in reducing falls in other populations and may be beneficial for individuals with chronic ankle symptoms.
Conclusion
Falls and sustaining an injury from a fall are more prevalent in individuals with chronic ankle symptoms compared to individuals with no ankle symptoms. Findings from this study suggest that healthcare professionals should ask patients presenting with chronic ankle symptoms and ankle OA about their falls history and any concerns they have about falling. Clinicians may want to assess falls risk factors in these patients to identify impairments that can be targeted in management.
The authors are from the Division of Physiotherapy, School of Health and Rehabilitation Sciences at the University of Queensland in St. Lucia, Australia.







