 Diabetic neuropathy (DN) is a widespread complication of diabetes, affecting nearly 50% of individuals with the condition. It commonly begins with the gradual loss of sensation in the lower extremities, particularly in the feet. If left undetected and untreated, this loss of sensation can lead to serious consequences, such as foot ulcers and eventual amputations. Early detection is critical to preventing irreversible nerve damage and minimizing the risk of such severe outcomes. However, current diagnostic methods often fail to identify neuropathy at an early stage, when intervention could still halt or reverse nerve degeneration.
Diabetic neuropathy (DN) is a widespread complication of diabetes, affecting nearly 50% of individuals with the condition. It commonly begins with the gradual loss of sensation in the lower extremities, particularly in the feet. If left undetected and untreated, this loss of sensation can lead to serious consequences, such as foot ulcers and eventual amputations. Early detection is critical to preventing irreversible nerve damage and minimizing the risk of such severe outcomes. However, current diagnostic methods often fail to identify neuropathy at an early stage, when intervention could still halt or reverse nerve degeneration.
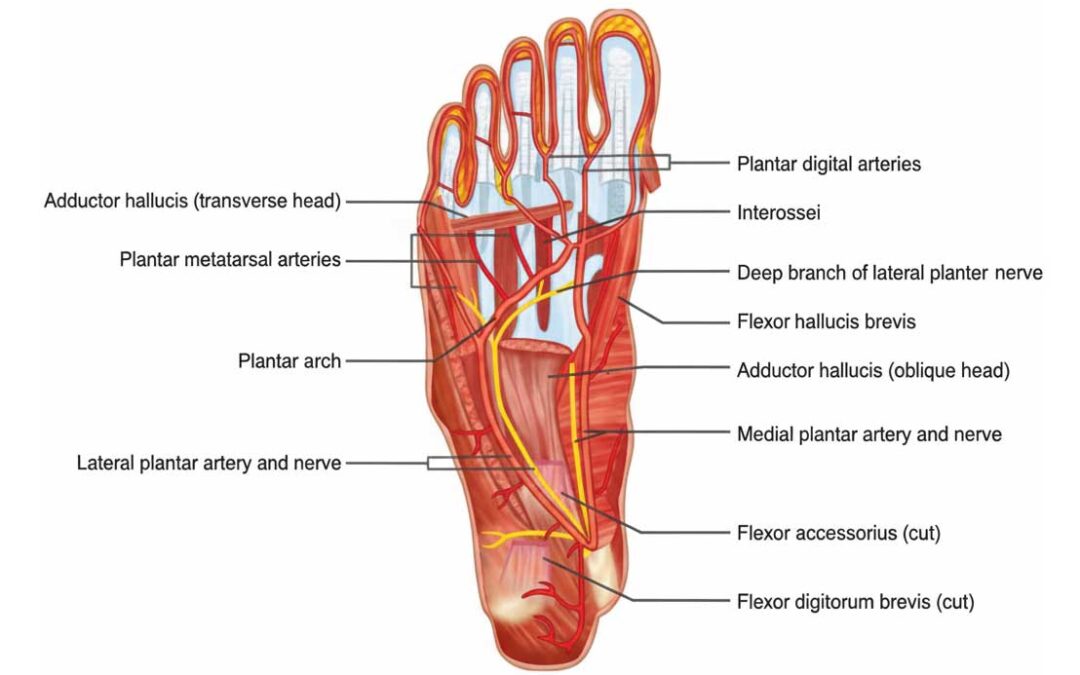
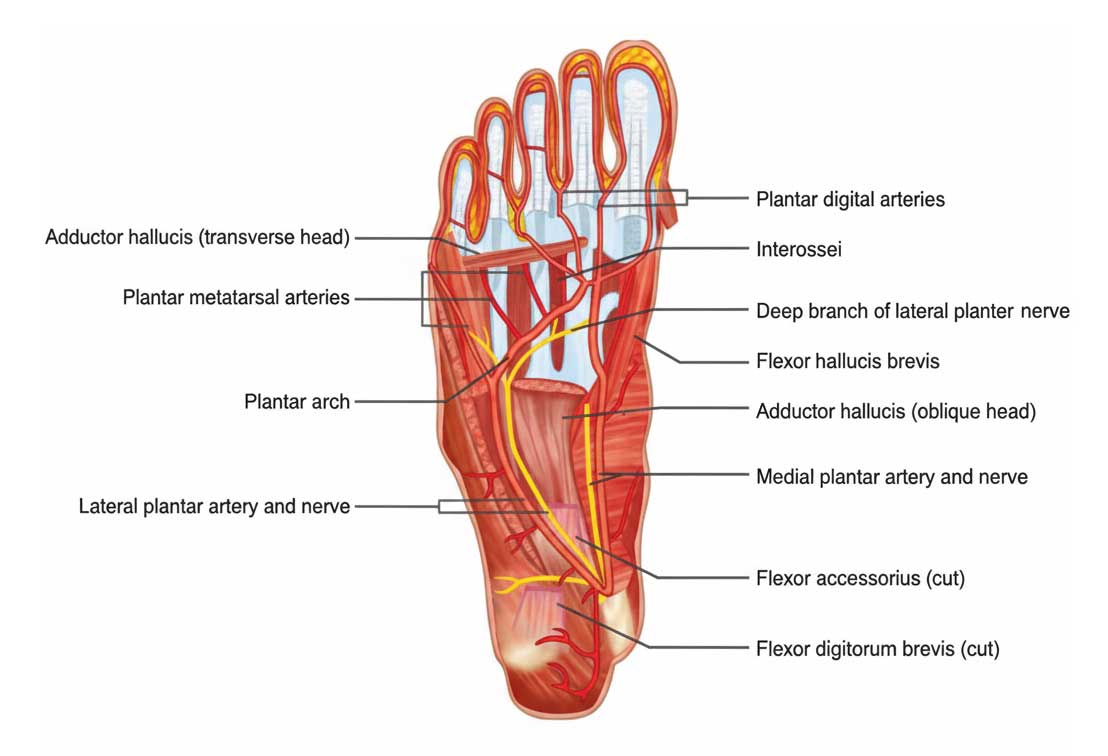
The medial and lateral plantar nerves, responsible for sensory innervation in the foot, are among the first to show signs of damage in DN. Monitoring these nerves offers a potential avenue for early diagnosis. Techniques such as nerve conduction studies (NCS) and quantitative sensory testing (QST) allow for the assessment of nerve function in the distal extremities, where neuropathy typically begins. Early identification of nerve dysfunction through these methods can lead to timely intervention, significantly improving patient outcomes and reducing the risk of severe complications. Addressing the early signs of neuropathy is essential in managing the growing prevalence of diabetes-related complications.
Source: Ahmed GU, Ahmed A, Raza AA, et al. Diagnostic advancements in early detection of diabetic neuropathy: comparative analysis of medial and lateral plantar nerve degeneration. Ann Med Surg (Lond). 2025 30;87(7):4325-4335. doi: 10.1097/MS9.0000000000003441.